![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
23 Cards in this Set
- Front
- Back
- 3rd side (hint)
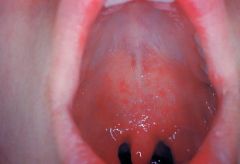
Prodromal symptoms: fever, malaise, dry (croupy) cough, coryza, and conjunctivitis with clear discharge and marked photophobia
Pathognomonic enanthem |
(Koplik spots)
FIRST Rubeola, Measles |
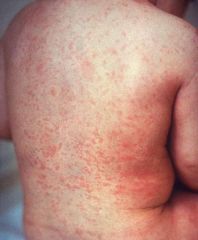
Exanthem is seen first on day 3 or 4, as the prodromal symptoms and fever peak in severity
Blotchy, erythematous, blanching, maculopapular eruption that appears at the hairline and spreads cephalocaudally over 3 days, ultimately involving the palms and soles Once generalized, the rash becomes confluent over proximal areas but remains discrete distally |
|
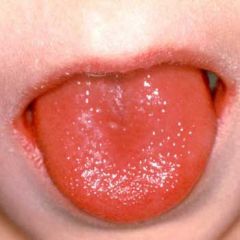
White/ red strawberry tongue
Flushed face, perioral pallor, and a diffuse, blanching, erythematous rash that has a sandpapery consistency on palpation. Palatal petequiae. Pastia lines (accentuation of the rash in the skin flexures/ creases) Desquamation occurs in fine, thin flakes as the acute phase of the illness resolves and is proportional to the intensity of the exanthem. |
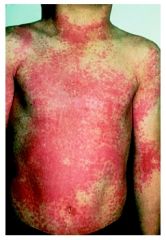
SECOND
Scarlet Fever, Scarlatina |
Tx within 7 days to prevent rheumatic fever
Streptococcus pyogenes |
|
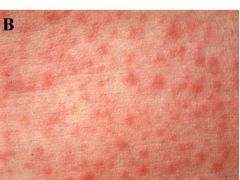
The exanthem is a discrete, pinkish red, fine maculopapular eruption, which, like measles, typically begins on the face and spreads cephalocaudally. The rash becomes generalized within 24 hours, then begins to fade, clearing completely by 72 hours.
The occipital, posterior cervical, and postauricular LAD Arthritis and arthralgias are frequent in young girls |
THIRD: Rubella, German measles
|
Forchheimer spots are seen in some patients on day 1 of the rash
Little or no prodrome Encephalitis is the most serious complication |
|
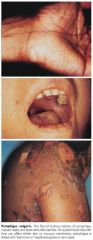
Onset is heralded by fever and irritability, often accompanied by vomiting followed by the development of diffuse erythroderma that spreads rapidly from head to toe and simulates the appearance of a sunburn
In contrast to streptococcal scarlet fever, the involved skin is tender, even to light touch. Within 1 to 3 days, thin-walled, flaccid, bullous lesions appear and rupture soon after formation followed by epidermal separation |
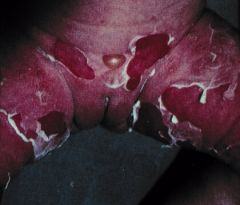
Staphylococcal Scalded Skin Syndrome (SSSS), Ritter's disease
|
Nikolsky sign (separation of the skin in response to stroking)
The primary infection is usually mild, with purulent nasopharyngitis, conjunctivitis, impetigo, and infections of the umbilicus and circumcision sites seen most commonly. Staphylococcus aureus’ phage group II coagulase-positive’s epidermolytic exotoxin |
|
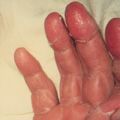
PRODROME: low-grade fever, malaise, myalgias, and vomiting.
DISEASE: abrupt increase in fever with chills, worsening myalgias, repetitive vomiting, abdominal pain, severe watery diarrhea, orthostatic dizziness, and weakness RASH: diffuse erythroderma, mimicking sunburn. SHOCK: Hypotension and oliguria may become prominent, accompanied by alterations in level of consciousness. |

FOURTH: Toxic Shock Syndrome
|
Menstruating women (tampon) or skin lesion, an abscess, or purulent conjunctivitis as the primary focus of infection.
Desquamation usually beginning a week after onset of the rash. It is most prominent over the palms and soles and in the periungual areas, and the skin is shed in thick casts. coag-positive staphylococci of phage group I or III |
|
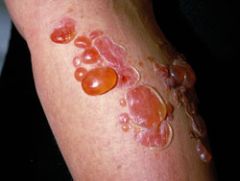
Thin walled large flaccid bullae.
|
Bullous impetigo
|
S. aureus
|
|
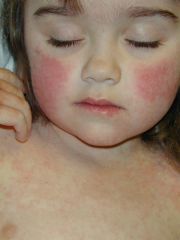
Slapped check
Lacy, reticulated erythema on the extremities or trunk. Papular purpuric “gloves and socks” syndrome |
FIFTH: Erythema Infectiosum
|
Parvo B 19
After 3 to 5 days, the eruption fades, although it may return for up to 4 months following exercise, overheating, or sun exposure. |
|
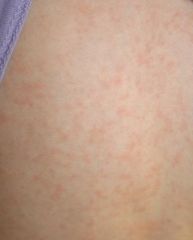
Exanthem of this disorder usually appears abruptly after 3 days of high fever and irritability. Fever stops.
|
SIXTH: Exanthem subitum, Roseola infantum
|
6 and 36 months with high fever (>39C) without a source
Human Herpes Virus 6 |
|
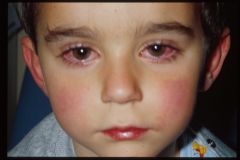
Non-purulent conjunctivitis, rhinitis, pharyngitis with or without exudate, and a discrete, blanching, maculopapular rash
|
Adenovirus
|
|
|
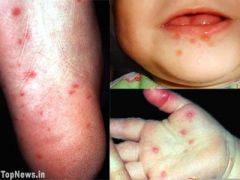
Enanthem: mildly painful, shallow, yellow ulcers surrounded by red halos in the oral mucosa (it is called herpangina when the rash is not present)
Exanthem: thick-walled, gray vesicles on an erythematous base involves the palmar, plantar, and interdigital surfaces of the hands and feet and sometimes the buttocks. |
Hand-foot-mouth
|
Coxsackievirus
A16 |
|
|
- Non specific maculopapular rash
- Eyelid edema is found in 50% - Severe pharyngotonsillitis - Generalized lymphadenopathy epitrochlear - Gianotti-Crosti syndrome |
Infectious mononucleosis
EBV |
Up to 80% of patients with infectious mononucleosis experience "ampicillin rash" if treated with ampicillin or amoxicillin
|
|
|
Multistage (papules, vesicles, and umbilicated and scabbed lesions)
|
Varicella: chickenpox
varicella-zoster virus |
GAS super infection
VZIG within 96 hours of exposure for immunocompromised children who have not had varicella previously (including those on short-course, high-dose steroids) |
|
|
Rash and fever.
Waterhouse-Friderichsen syndrome (shock and purpura) = adrenal hemorrhage and secondary adrenal insufficiency. 50% have NL WBC (overwhelmed immune system) Only about 20% of these patients have meningitis. Deaths within 24 hours circulatory collapse and CHF caused by endotoxic shock and myocarditis |
Meningococcemia
Neisseria meningitides gram-negative diplococci. |
Antimicrobial prophylaxis with RIFAMPIN, Ceftriaxone or cipro for members of the same household or persons in "closed communities" like military barracks, dormitories, or day-care centers.
|
|
|
Transmission occurs when a person is bitten by an infected Ixodes species tick (deer tick).
Ixodes scapularis (formerly Ixodes dammini) is the most common vector. RASH: erythema migrans (50% of cases) begins as a red papule or macule at the site of the tick bite and often goes unrecognized. The lesion gradually enlarges (to a median size of 15 cm), forming a large plaque, which tends to clear centrally, giving it an annular configuration. Systemic symptoms: CNS: aseptic meningitis, VII paralysis, optic neuritis. HEART: A-V block or myopericarditis. The arthritis of Lyme disease is a late manifestation, seen in up to 50% of untreated patients: pauciarticular, involving large joints (knee). Late neurologic manifestations include encephalitis, encephalopathy, ataxia, radiculoneuritis, and myelitis. |
Lyme disease
tick-borne infection caused by the spirochete Borrelia burgdorferi |
TREATMENT
> 8 DOXYCYCLINE for 14-21d. < 8 AMOX or CEFUROXIME DISSEMINATED OR LATE DISEASE 21-28 days. NE of the USA (Connecticut) |
|
|
Usually transmitted to humans by the bite of an infected tick.
Mortality is as high as 5% to 7%. Splenomegaly (30% to 50%). The rash begins distally on the wrists, ankles, palms, and soles, usually appearing as an erythematous, blanching, fine, macular or maculopapular eruption. It then spreads centripetally and becomes petechial. |
Rocky Mountain Spotted Fever
Rickettsia rickettsii obligate intracellular parasites |
Thrombocytopenia and NL/ low WBC and hyponatremia.
TREATMENT Doxycycline (regardless of age) |
|
|
1. A vascular malformation or port-wine stain over the face that involves the cutaneous distribution of the ophthalmic division of the V nerve
2. Ipsilateral leptomeningeal angiomatosis with associated intracranial calcifications 3. A high incidence of MR and ipsilateral ocular complications like buphthalmos (corneal enlargement), glaucoma or a coloboma Seizures and a facial port-wine stain = ______ - _____ syndrome, which can be confirmed by CT scan. CT buzz words: progressive ipsilateral cerebral atrophy, serpiginous calcifications of brain parenchyma and intracranial calcifications |
Sturge-Weber
|
Only patients with lesions involving the forehead and upper eyelid are at risk for associated neuro-ocular complications
Repeated ophthalmologic and CT examinations are indicated only in this high-risk group, which has a 10% to 20% incidence of associated intracranial angiomas. |
|
|
The characteristic skin lesion of tuberous sclerosis are
Ash-leaf spots: congenital, well demarcated, 1- to 3-cm macular hypopigmented lesions on the trunk. Angiofibroma (adenoma sebaceum): erythematous papules over the nose and malar region of the face. ~40% of children with TS demonstrate these lesions by 3 years of age. Shagreen patch, a plaque of thickened skin with a cobblestone or orange-peel texture often seen on the dorsal aspect of the trunk. Periungual fibromas Oral examination may reveal pitting of dental enamel |
Tuberous sclerosis
A.D. Wood's light exam: any child, with a fair complexion + idiopathic seizures in infancy. Up to 0.5% of normal newborns an isolated hypopigmented macule is a NL variant (nevus depigmentosus) |
Seizures (96%)
Mental retardation (60%) Intracranial calcification (49%) Tumors of various organs (cardiac rhabdomyoma (66%), renal angiomyolipomas (75%), pulmonary lymphangiomyomatosis (<2%), and hepatic hamartoma) |
|
|
Port-wine stain that is usually located over the lateral aspect of one leg
Hypertrophy (usually hemihypertrophy) and lymphedema |
Klippel-Trénaunay syndrome
|
|
|
|
Germ line mutations in the VHL tumor suppressor gene (3p25-26).
Multiorgans, including the cerebellum(hemangioblastomas), spinal cord, medulla, retina (angiomata), kidney, pancreas, and epididymis. |
von Hippel-Lindau disease
AD |
Renal carcinoma is the most common cause of death
|
|
|
Multisystem, degenerative disorder characterized by ataxia, oculocutaneous telangiectasia, immunodeficiency, and a high incidence of neoplasia (ALL or lymphoma).
Recurrent sinus and pulmonary infections due to cellular and humoral (IgA and IgM deficiency). |
Ataxia-Telangiesctasia
AR |
Tremors of the head may be seen before 1 yr, and ataxia is evident when the child first walks.
Ocular telangiectasia at 6yo. |
|
|
Present at birth, manifest as a yellowish-tan, waxy linear lesion
Nevus may be found on the scalp, face, neck, trunk, or extremities 15% to 20% risk of malignant degeneration Association with seizures and mental retardation has been reported. |
Linear nevus sebaceus of Jadassohn
|
The risk of neurologic abnormalities is greatest when the cutaneous lesion is located in the midfacial area.
|
|
|
Congenital neurocutaneous disorder in which an epidermal nevus (raised, often warty hyperpigmented lesions typically in a linear pattern) is seen in association with neurologic dysfunction (seizure, MR, DD).
|
Epidermal nevus syndrome
|
Unilateral hemimegalencephaly with intractable seizures is the commonest CNS abnormality
|
|
|
Cutaneous, neurologic, ophthalmologic, and dental manifestations
1st stage: Linearly distributed vesicles on an erythematous base 2nd stage: lesions evolve into warty papules, which can have thick overlying crusts 3rd stage: swirled hyperpigmented patches replaced the warty lesions by 8 months of age |
Incontinentia pigmenti
X-linked dominant syndrome |
Neurologic and ophthalmologic occur in about 30% of patients: seizures, CVA, developmental delay, mental retardation, and microcephaly.
DDX: neonatal herpes |

