![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
12 Cards in this Set
- Front
- Back
|
How does PCO2 drive breathing? |
Through production of H+ ion, which acts on chemoreceptors |
|
|
Draw the effect of increased arterial PCO2 on breathing. |
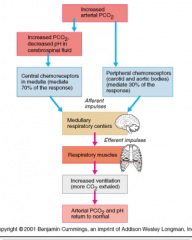
|
|
|
Where is diaphragm breathing controlled from? |
Medulla |
|
|
Difference between respiratory and ventilatory failure? |

|
|
|
What are the mechanisms of respiratory failure? |
Hypoxemic failure V/Q mismatch Shunt (perfusion but no ventilation) Exacerbated by low mixed venous O2 (SvO2) Hypercapnic failure Decreased minute ventilation (MV) relative to demand Increased dead space ventilation (opposite of shunt) |
|
|
Know the five causes of hypoxemia: |
1. Decreased PiO2 2. Hypoventilation 3. V/Q inequality 4. Shunt 5. Diffusion limition
1,2 = normal A-a (no intrinsic lung disease) |
|
|
Causes of hypercapnic resp failure: |
1. Central hypoventilation 2. Neuropathies 3. Muscle (pump) failure: muscular dystrophy, myopathies, myasthenia gravis 4. Airway obstruction |
|
|
How to evaluate for resp failure? |
1. H & P 2. Vital signs including pulse oximetry 3. CXR 4. EKG 5. ABG (air blood gas) 6. CBC 7. Electrolytes 8. Sputum and blood cultures, UA 9. Helical CT Vs. V/Q scan (inhale Xe133 and see where the air went for ventilation) 10. PFT (pulmonary function test on outpatient basis) |
|
|
Hypoxic respiratory failure: How to treat? |
1. Supplemental O2 2. Most common mech = V/Q mismatch |
|
|
How to treat bronchospasm? |
Bronchodilators Beta2 agonists Anticholinergic agents Albuterol Ipratropium Formoterol
|
|
|
How long does it take BDs to work? Is this enough to relieve all bronchospams? |
Albuterol = 5-10 min Iprotropium = similar Formoterol = rapid onset of action
No, may not be able to devilry to all areas of lung |
|
|
What conditions for acute bronchospasm? |
Bee sting Asthma Anaphylaxis |

