![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
53 Cards in this Set
- Front
- Back
|
Two basic principle of autoimmune disorders. |
(1) Characterized by immune-mediated damage of tissues.
(2) Involves loss of self-tolerance |
|
|
What is the prevalence of autoimmune disorders?
|
1% in the USA. More common in women; classically affects women of childbearing age.
|
|
|
What is the etiology of autoimmune disorders?
|
Etiology is likely an environmental trigger in genetically susceptible individuals (increased incidence in twins and associated with certain HLA subtypes).
|
|
|
What mediates the damage in SLE?
|
Autoantibodies against the host damage multiple tissues via type II HST (cytotoxic) and type III (Ag-Ab complexes) HST.
|
|
|
SLE is more common in ________ (men/women), especially ___________.
|
women; african-american women.
|
|
|
What are clinical features of SLE?
|
• Fever, weight loss (chronic inflammation)
• Malar 'butterfly' rash, especially upon sun exposure • Arthritis • Serositis (pleura, pericardium) • Inflammation of brain; CNS psychosis |
|
|
The most common cause of death in lupus patients is _________. Most commonly due to what pattern of injury? Aside from this, a common cause of death is ________.
|
renal damage; diffuse proliferative glomerulonephritis; infection.
|
|
|
True or false: SLE can involve the heart.
|
True. All three layers. Can produce a characteristic Libman-Sacks endocarditi. One of the key findings is the presence of vegetations on BOTH sides of the heart valve involved.
|
|
|
True or false: In SLE there may be autoantibodies to formed blood elements.
|
True. There may be formed antibodies against RBCs, PLTs, WBCs.
|
|
|
This autoantibody is seen in CREST syndrome.
|
C is for Calcinosis and anti-Centromere antibody
|
|
|
This autoantibody is seen in celiac disease.
|
(1) Antiendomysial IgA
(2) Antigliadin IgA (3) Anti-tissue transglutaminase IgA |
|
|
This autoantibody is seen in drug-induced lupus.
|
Anti-histone
|
|
|
This antibody is seen in DM type I.
|
Anti-insulin
|
|
|
This autoantibody is seen in Hashimoto's.
|
Antimicrosomal antibody
Antithyroglobulin |
|
|
This autoantibody is seen in SLE.
|
(1) Anti-Smith (Sm)
(2) ANA (3) Anti-dsDNA |
|
|
This autoantibody is seen in primary biliary cirrhosis.
|
Antimitochondrial antibody
|
|
|
This autoantibody is seen in Sjögrens.
|
Anti-SS-A (Ro)
Anti-SS-B (La) |
|
|
This antibody is seen in microscopic polyangiitis.
|
Antimyeloperoxidase antibody.
|
|
|
This autoantibody is seen in mixed connective tissue disease.
|
Anti-ribonucleoprotein.
|
|
|
This autoantibody is seen in Wegener's granulomatosis.
|
(1) C-ANCA
(2) Antiproteinase 3 antibody |
|
|
This autoantibody is seen in systemic sclerosis.
|
(1) Anti-topoisomerase
(2) ANA |
|
|
This autoantibody is seen in dermatomyositis.
|
ANA
|
|
|
Anti-dsDNA is highly ______ (sensitive/specific) for SLE.
|
specific
|
|
|
ANA is ________ (sensitive/specific) for SLE.
|
sensitive
|
|
|
These drugs are common causes of drug-induced SLE.
|
(1) Hydralazine
(2) Procainamide (3) Isoniazid |
|
|
What is the treatment of drug-induced SLE?
|
Remove drug. It usually results in remission.
|
|
|
This syndrome is associated with SLE in _____% of cases.
|
antiphospholipid syndrome; 30%
|
|
|
Antiphospholipid syndrome is associated with what?
|
Autoantibody against proteins bound to phospholipids.
|
|
|
In antiphospholipid syndrome the MC antibodies are [...]
|
Anticardiolipin and lupus anticoagulant
|
|
|
The presence of autoantibodies in antiphospholipid syndrome could interfere with what? |
Lead to false-positive syphilis test and falsely-elevated PTT lab studies, respectively
|
|
|
Why is lupus anticoagulant called an anticoagulant.
|
It produces a falsely elevated PTT.
|
|
|
Lupus anticoagulant results in _______________. Treatment is?
|
Results in arterial and venous thrombosis including deep venous thrombosis, hepatic vein thrombosis, placental thrombosis (recurrent pregnancy loss), and
stroke. Lifelong anticoagulation. |
|
|
What is Sjögren syndrome? What type of damage is it?
|
Autoimmune destruction of lacrimal and salivary glands. Lymphocyte-mediated damage (type IV hypersensitivity) with fibrosis.
|
|
|
Sjögren clinically presents as?
|
Classically presents as dry eyes (keratoconjunctivitis), dry mouth (xerostomia), and recurrent dental carries in an older woman (50-60 years)—"Can't chew a cracker, dirt in my eyes".
|
|
|
A woman has bilaterally enlarged parotid glands with dry eyes. Treatment is begun and parotid glands shrink back to normal. A few years later, the left parotid gland has again swelled up. What is going on?
|
Sjögrens syndrome has an increased risk for B-cell (marginal zone) lymphoma.
|
|
|
Autoimmune disorders are often associated with _________________.
|
other autoimmune disorders
|
|
|
A woman with dry eyes and mouth develops nodules on her forearm close to her elbow. What is going on?
|
Sjögren is associated with other autoimmune diseases, especially Rheumatoid arthritis.
|
|
|
Another word for scleroderma is ___________.
|
systemic sclerosis
|
|
|
What is scleroderma?
|
Autoimmune tissue damage with activation of fibroblasts and deposition of collagen (fibrosis) . Primarily targets the skin (scleroderma), gastrointestinal tract, lungs, and kidneys.
|
|
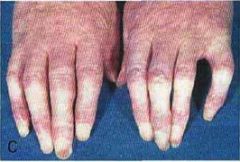
A woman has the following sign. This is the MC initial sign of what?
|
Raynaud's phenomenon, MC initial sign of systemic sclerosis.
Sequential color changes (white to blue to red) caused by digital vessel vasculitis and fibrosis |
|
|
Describe the two types of systemic sclerosis.
|
(1) Diffuse type (skin and early visceral involvement). Almost any organ can be involved; esophagus is commonly affected, resulting in disordered motility (dysphagia for solids and liquids).
(2) Localized type (local skin and late visceral involvement). Prototype is CREST syndrome: Calcinosis/anti-Centromere antibodies, Raynaud phenomenon. Esophageal dysmotility, Sclerodactyly, and Telangiectasias of the skin. |
|
|
What is MCTD?
|
Mixed connective tissue disease.
Autoimmune-mediated tissue damage with mixed features of SLE, systemic sclerosis, and polymyositis. Characterized by serum antibodies against U1 ribonucleoprotein |
|
|
In systemic sclerosis, the MCC of death is ____________.
|
respiratory failure
|
|
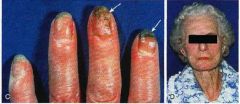
What is your first clinical suspicion?
|
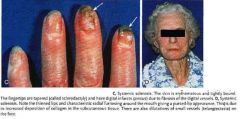
|
|
|
The MC cardiac finding in SLE is ___________________.
|
fibrinous pericarditis with effusion
|
|
|
A woman with SLE delivers a newborn. What complications in the newborn could you expect to see?
|
Complete heart block in newborns
• Caused by IgG anti-SS-A (Ro) antiboilies crossing the placenta |
|
|
A woman with SLE has recurrent spontaneous abortions. The doctor states that this is unrelated to her condition. Is he right?
|
He is wrong. Recurrent spontaneous abortions can be caused by antiphospholipid antibodies.
|
|
|
Would serum complement be high or low in SLE?
|
Low due to complement activation due to immune complexes.
|
|
|
In the pathogenesis of SLE, genetic links appear to be located on chromosome __.
|
6
|
|
|
Provide five examples of environmental factors that may be important in exacerbating or triggering SLE.
|
(1) Infections (virus/bacteria)
(2) UV (3) Estrogen (4) Medications (5) Extreme stress They destroy cells, leading to Abs directed against various nuclear antigens. |
|
|
A serum __________ is the most useful screening test for autoimmune diseases.
|
ANA
|
|
|
This type of transplant has the best allograft survival rate. It is associated with what? |
cornea; danger of transmission of Creutzfeldt-Jakob
|
|
|
The fetus is an ___________ that is not rejected by the mother. What tissue may prevent maternal T cells from entering the fetus?
|
allograft
trophoblastic tissue |

