![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
93 Cards in this Set
- Front
- Back
|
What type of virus is HSV? |
- herpes simplex virus
- DNA virus - herpesvirus family |
|
|
What are the two forms of HSV? |
HSV 1 - spread predominantly through oral (above waist) |
|
|
How does spread of HSV to an uninfected host occur?
|
- during periods of asymptomatic viral shedding |
|
|
What is the usual incubation period of HSV?
|
3 - 9 days
|
|
|
Define PRIMARY INFECTION of HSV? |
- initial exposure of an individual who has not been previously exposed to the disease |
|
|
Most primary infections of HSV occur when?
|
childhood - subclinical - few result in clinical disease |
|
|
What is the most common form of symptomatic primary HSV? |
acute herpetic gingivostomatitis |
|
|
acute herpetic gingivostomatitis - Most common pattern of ________HSV infection; most cases occur between ages of ________; _____ onset with anterior ____________, fever (103 to 105°F), anorexia, irritability, and sore mouth lesions; mild to severely debilitating and may last from _____ up to _____. |
1. symptomatic Primary 2. 6 mos and 5 years 3. abrupt 4.cervical lymphadenopathy 5. 5-7 days up to 2 WEEKS
|
|
|
Most cases of acute herpetic gingivostomatitis arise when?
|
6 months to 5 years |
|
|
Explain why HSV is "neurotropic"?
|
it is transported via nerves to sensory ganglia, the TRIGEMINAL GANGLION to reside in a latent form |
|
|
How is diagnosis of HSV usually made?
|
clinical. |
|
|
Which treatment mode is good for HSV and in which time frame? |
If identified within 2-3 days then ACYCLOVIR is helpful.
|
|
|
What is SECONDARY INFECTION of HSV?
|
reactivation of the latent virus, causing vesiculo-ulcerative eruption on infected epithelial surface |
|
|
WHat are PRODROMAL symptoms of HSV? |
- tingling |
|
|
Where do most secondary lesions of HSV appear? |
vermillion border and surrounding skin
|
|
|
What is the name for the most common form of secondary infection of HSV? |
- recurrent herpes labialis
|
|
|
Intraoral recurrence of HSV are almost always restricted to what types of surfaces? |
keratinized mucosa that is bound to bone |
|
|
Acute herpetic gingivostomatitis Oral lesions: Affected mucosa initially has __________ -----> rapidly collapse to numerous, ______ ------> enlarge slightly with central _______ covered by _____ -------> adjacent ulcerations _______ ------> larger, shallow, irregular ulcerations. Occurs on ______mucosa. number of lesions variable. In all cases gingiva is enlarged, painful, and extremely erythematous and often has distinctive _______ along mid-facial _______. Involvement of the labial mucosa may spread beyond the wet line to include adjacent vermilion border of the lips. May also have ________ of the perioral skin. |
1. pinhead vesicles 2. small red lesions 3. central ulceration 4. Yellow Fibrin 5. Coalesce 6.both movable and nonmovable (attached) mucosa 7. punched-out erosions 8. free gingival margins 9. satellite vesicles |
|
|
What is HERPETIC WHITLOW?
|
primary or secondary HSV infection involving the finger.
|
|
|
What is the more common layman's term for VARICELLA?
|
Chickenpox |
|
|
How is VZV spread?
|
- direct contact
- airborne droplets |
|
|
Describe the skin lesions of VZV?
|
intensely pruritic vesicles
- "dew-drops on rose petals" |
|
|
Describe the oral lesions of VZV: |
- few 1-2 mm shallow oral ulcers, generally not as symptomatic as cutaneous lesions |
|
|
How is diagnosis of VZV made?
|
- history of exposure in past 3 weeks |
|
|
What is the treatment for VZV?
|
- supportive care |
|
|
Define Herpes zoster?
|
- herpes zoster is the recurrent form of varicella infection. |
|
|
What is the laymans term for Herpes Zoster?
|
- shingles
|
|
|
What is the reason that VZV can recur?
|
after initial infection with VZV the virus is transported up the sensory nerves where it resides in a latent form in the DORSAL SPINAL GANGLIA. |
|
|
Describe oral lesions of herpes zoster?
|
Oral lesions occur with trigeminal nerve involvement and are sharply and distinctively unilateral along nerve distribution - STOP AT MIDLINE |
|
|
What can be a cause of significant morbidity with herpes zoster?
|
ocular involvement may lead to permanent blindness
|
|
|
Infectious mononucleosis is caused by what virus?
|
Epstein-Barr Virus |
|
|
How is EBV transmitted?
|
Through Saliva - sharing straws or kissing in adults
|
|
|
What is the difference between getting EBV in childhood vs adolescent / adult?
|
Childhood - usually asymptomatic |
|
|
What are some signs of Mono?
|
- lymphadenopathy
- oropharyngeal tonsillar enlargement - oral lesions: lymphoid enlargement, NUG, petechiae on palate |
|
|
What is the treatment for MONO?
|
- IM resolves within 4-6 weeks. No specific treatment other than bed rest.
|
|
|
What are the most prominent members of the PARAMYXOVIRUS FAMILY?
|
Measles
Mumps |
|
|
How is MEASLES spread?
|
- airborne droplets
|
|
|
Define "Kopliks spots"
|
in Measles, small erythematous macules with white necrotic centers appearing on buccal mucosa
|
|
|
Koplik's spots in Measles generally precede skin rash by how long?
|
1-2 days
|
|
|
During what period is the MEASLES patient contagious?
|
- 2 days prior to becoming symptomatic
- 4 days after rash develops |
|
|
What are some possible complications of MEASLES?
|
- encephalitis
- viral pneumonia |
|
|
When is the MMR vaccine recommended?
|
- 12-15 months first dose
- 1 months second dosse |
|
|
What is HAND FOOT AND MOUTH disease?
|
Highly contagious systemic infection usually caused by coxsackievirus A.
|
|
|
How is HFM disease transmitted?
|
inhalation of airborne droplets or by contact with saliva containing virus
|
|
|
HFM disease most commonly occurs in what demographic>?
|
children 1-5 years old |
|
|
Describe the oral lesions of hand foot mouth disease:
|
shallow ulcers 2-7 mm in diameter (1-30) on buccal mucosa, labial mucosa and tongue
|
|
|
Describe the skin lesions of hand foot mouth:
|
1-3 mm erythematous macules that may develop a central vesicle |
|
|
What is the treatment for hand foot mouth:
|
self-limiting. Resolves within 7-10 days
|
|
|
Define HERPANGINA:
|
enterovirus infection caused by any one of several strains of coxsackievirus A or B or echovirus
|
|
|
Describe the lesions of Herpangina:
|
acute onset of sore throat, fever, 1-2mm shallow oral ulcers (2-6) localized to posterior soft palate/tonsillar pillar region
|
|
|
What is ACUTE LYMPHONODULAR PHARYNGITIS?
|
localized infection of coxsackievirus A |
|
|
What is ACUTE LYMPHONODULAR PHARYNGITIS characterized by?
|
sore throat, fever, and mild headache
|
|
|
What is the clinical features of acute lymphonodular pharyngitis? |
low numbers (1-5 ) of yellow to dark pink papules develop on soft palate or tonsillar pillars
|
|
|
What diseases are related to HERPES SIMPLEX VIRUS?
|
- primary herpes gingivostomatitis
- secondary herpes infections (recurrent herpes labialis) - genital herpes |
|
|
What diseases are related to VARICELLA ZOSTER VIRUS?
|
- chickenpox
- shingles |
|
|
What disease are related to EPSTEIN BARR VIRUS? |
- mononucleosis (mono)
- Burkitt's lymphoma - Nasopharyngeal carcinoma - hairy leukoplakia |
|
|
What disease are related to HUMAN PAPILLOMAVIRUSES?
|
- oral papilloma / warts
- condyloma acuminatum - focal epithelial hyperplasia |
|
|
What diseases are related to COXSACKIEVIRUSES?
|
- herpangina
- hand foot mouth disease - acute lymphonodular pharyngitis |
|
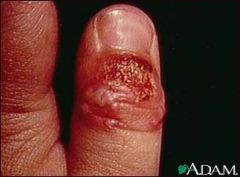
This patient has a history of cold sores appearing often on the lips. They present to your office with this condition. What is your diagnosis?
|
Herpetic whitlow |
|
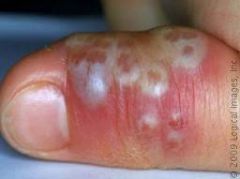
This patient has a history of cold sores appearing often on the lips. They present to your office with this condition. What is your diagnosis?
|
Herpetic whitlow
|
|
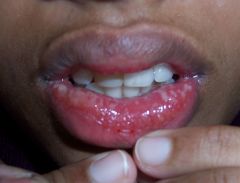
This child present to you with ulcerations on the oral mucosa and surrounding areas. They are very painful and some of the blisters have already ruptured. What is your diagnosis?
|
Acute herpetic gingivostomatitis (Primary Herpes Simplex Infection)
|
|
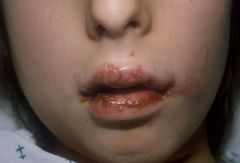
This child present to you with ulcerations on the oral mucosa and surrounding areas. They are very painful and some of the blisters have already ruptured. What is your diagnosis?
|
Acute herpetic gingivostomatitis (Primary Herpes Simplex Infection)
|
|
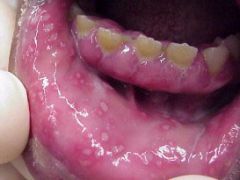
This child present to you with ulcerations on the oral mucosa and surrounding areas. They are very painful and some of the blisters have already ruptured. What is your diagnosis?
|
Acute herpetic gingivostomatitis (Primary Herpes Simplex Infection)
|
|
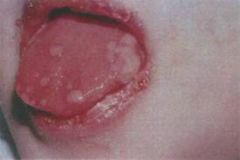
This child present to you with ulcerations on the oral mucosa and surrounding areas. They are very painful and some of the blisters have already ruptured. What is your diagnosis?
|
Acute herpetic gingivostomatitis (Primary Herpes Simplex Infection)
|
|
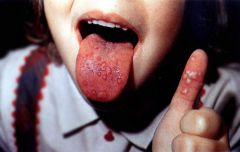
This child present to you with ulcerations on the oral mucosa and surrounding areas. They are very painful and some of the blisters have already ruptured. What is your diagnosis?
|
Acute herpetic gingivostomatitis (Primary Herpes Simplex Infection)
|
|
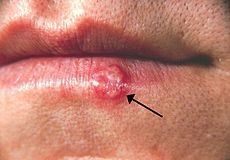
This adult presents with a "cold sore" on the lip. They say that this happens once or twice a year. What is your diagnosis?
|
Recurrent Herpes Labialis
|
|
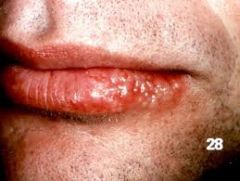
This adult presents with a "cold sore" on the lip. They say that this happens once or twice a year. What do you tell the patient?
|
That the lesion should go away within 7-10 days. Can prescribe analgesics for the pain. Acyclovir if the lesion has only been for 2-3 days active.
|
|
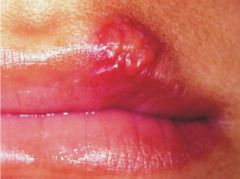
What is this lesion?
|
Recurrent Herpes Labialis
|
|
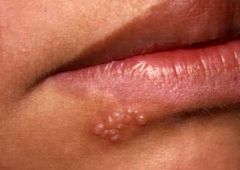
What is this lesion?
|
Recurrent Herpes Labialis
|
|

What virus is this child infected with?
|
Varicella zoster (Chicken pox)
|
|
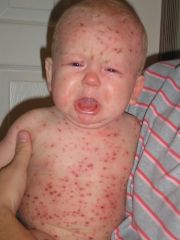
What virus is this child infected with?
|
Varicella zoster (Chicken pox)
|
|
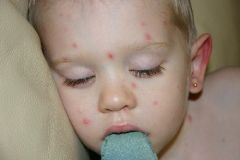
What virus is this child infected with?
|
Varicella zoster (Chicken pox)
|
|
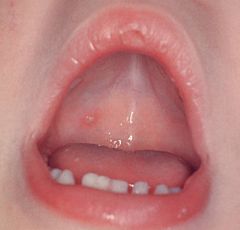
What virus is this child infected with?
|
Varicella zoster (Chicken pox)
|
|
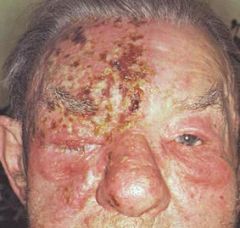
This elderly man has a positive history for chickenpox in his childhood. He presents with this severe condition strangely following unilateral trigeminal distribution. What is your diagnosis? |
Herpes Zoster (Shingles) |
|
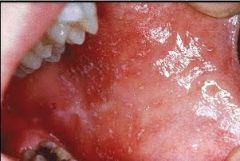
These are known as "Koplik's Spots". Which condition are they associated with? Why are they significant? |
MEASLES
They precede the rash by 2 days. |
|
|
What is the percentage of patients sustaining a needle stick from a documented HIV-positive person become infected with HIV?
|
0.3% |
|
|
Which ONE of the following is the most appropriate test for diagnosing acute HIV infection during acute retroviral syndrome? |
HIV PCR
|
|
|
Diagnosis of ORAL CANDIDIASIS is most appropriately made by visual appearance plus which ONE of the following confirmatory lab tests? |
Gram stain
|
|
|
A 27 year old male IDU (Injection Drug USer) presents with multiple smooth, papular, facial lesions, 2-4mm in diameter with a central umbilicus. What is the diagnosis?
|
Molluscum contagiosum
|
|
|
AZT and 3YC are antiretroviral drugs which work by which ONE of the following mechanisms?
|
Inhibition of REVERSE TRANSCRIPTASE and DNA CHAIN TERMINATION |
|
|
Efavirenz and Nevirapine are antiretroviral drugs which work by which mechanism?
|
Inhibition of reverse transcriptase alone |
|
|
Nelfinavir and Lopinavir are antiretroviral drugs which work by which mechanism?
|
Inhibiton of protease
|
|
|
Saquinavir and Atazanavir are antiretroviral drugs which work by which mechanism?
|
Inhibition of protease |
|
|
Enfuvirtide is an antiretroviral drug which works by which mechanism? |
Inhibition of HIV/target cell fusion |
|
|
Raltegravir is an antiretroviral drug which works by what mechanism?
|
Inhibition of integrase
|
|
|
Maraviroc is an antiretroviral drug which works by what mechanism?
|
Inhibition of chemokine receptor CCR5
|
|
|
When should POST EXPOSURE PROPHYLAXIS begin? |
Within 2 hours of exposure
|
|
|
List the AIDS-defining illnesses: |
- esophageal candidiasis |
|
|
regarding HSV infections Children with initial exposure tend to exhibit ________while adults demonstrate more often a ______. HSV-2 exposure correlates directly with ______. |
1. acute herpetic gingivostomatitis 2. Pharyngotonsillitis 3. sexual activity |
|
|
pharyngotonsillitis - sore throat, fever, malaise, and headache with numerous _______ on tonsils, posterior pharynx. Vesicle rupture ----------> numerous shallow coalescing ulcerations with an overlying diffuse _______. Ninety percent of this type of adult primary infection remains________ to ________ |
1. small vesicles 2. gray-yellow exudate 3. posterior 4. Waldeyer’s ring. |
|
|
Most common site of recurrence for HSV-1 is ______ of the adjacent skin of the lips and is called________ ("cold sore”, "fever blister”) - _____ of U.S. population believed to have a history of herpes labialis. Most common triggering factors: _______ & ______ |
1. vermilion border 2. herpes labialis 3. 15-45% 4. ultraviolet light and trauma |
|
|
Herpes Labialis Recurrences also seen less often on skin of nose, chin, or cheek. Recurrences also affect oral mucosa almost always limited to the ________mucosa ; lesions more _____; 1-3 mm vesicles ------> collapse, cluster of erythematous macules, enlarge or coalesce -----> _______ ulceration -------> healing within ________ |
1. keratanized (bound to bone - attached gingiva, hard palate) 2. subtle 3. central yellow 4. 7-10 days |
|
|
HSV recurrence in _______ significant and different - persist and spread on the skin until antiviral therapy, immune status improves, or die; oral mucosa also can be involved and may spread to ________; involved sites begin as _______ epithelium ------> spread_______ -------> zone of superficial _____ with circinate, raised, _____ border. |
1. immunocompromised hosts 2. unbound mucosa 3. brown, raised necrotic 4. laterally 5. erosion 6. yellow |

