![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
57 Cards in this Set
- Front
- Back
|
causes of intracellular edema
|
Metabolic
anaerobic metabolism inflammation |
|
|
causes of extracellular edema
|
increased capillary pressure – CHF, RF
increased capillary permeability - burns decreased plasma proteins (COP) – liver failure blockage of lymph return - malignancy |
|
|
what is SIADH? How is it treated ?
|
Syndrome of inappropriate antidiuretic hormone (SIADH)
Failure of feedback mechanism that regulates ADH release and inhibition Continued secretion of ADH Retention of water Dilutional hyponatrmia Causes – brain tumor SIADH – too much ADH released, too much volume. Acute treatment: hypertonic sodium sol., chronic: fluid restriction. |
|
|
What are the 2 types of Diabetes Insipidus? Symptoms? How are they treated?
|
Abbreviation: DI.
Excessive urination caused either by inadequate amounts of circulating vasopressin (antidiuretic hormone) in the body (hypothalamic DI) or by failure of the kidney to respond to antidiuretic hormone (nephrogenic DI). Urinary output is often massive (e.g., 5 to 15 L/day), which may result in dehydration in patients who cannot drink enough liquid to replace urinary losses (e.g., those with impaired consciousness). The urine is dilute (specific gravity is often below 1.005), and typically the patient's serum sodium level and osmolality rise as free water is eliminated as urine. If water deficits are not matched or the urinary losses are not prevented, death will result from dehydration. SYMPTOMS The primary symptoms are urinary frequency, thirst, and dehydration. TREATMENT When DI is a side effect of drug therapy, the offending drug is withheld. DI caused by failure of the posterior pituitary to secrete antidiuretic hormone is treated with synthetic vasopressin. |
|
|
major function of sodium
how is sodium regulated? |
Functions
Body compartment fluid regulation* (reg. volume) Cell membrane permeability and transport Neuromuscular impulse conduction Acid-base regulation Regulation of sodium: GFR, Sympathetic NS RAAS, aldosterone (secreted by adrenal cortex and promotes Na retention, K excretion) ANP: produced by stretch receptors in atrium of heart |
|
|
major functions of potassium
potassium is regulated by... |
Functions
Regulates ICF osmolality*** Transmembrane electrical potential potassium is regulated by aldosterone and H+ |
|
|
major functions of calcium
calcium is regulated by |
Functions
Nerve impulse transmission Myocardial contractility Bone metabolism: 99% of Ca is in bones & teeth Coagulation Regulation: Parathyroid hormone – secreted when Ca low Vitamin D Calcitonin (thyroid) – inhibits calcium release from bone. secreted when calcium high |
|
|
_____ and calcium increase and decrease together.
|
magnesium
|
|
|
major functions of magnesium
regulation of magnesium |
Functions
Activates ATP* Mediator at myoneural junctions* Carbohydrate, protein metabolism Cell membrane transport of Na and K Regulation: GI absorption Renal tubule excretion |
|
|
6 functions of the kidney
|
1. Excretion / elimination of waste products
-Glomerular filtration 2. Regulation of water and electrolyte balance -Tubular re-absorption / Tubular secretion 3. Regulation of acid-base balance 4. Control of BP, ECF volume - RAAS 5. Production of erythropoietin, prostaglandin 6. Synthesis of active form of vitamin D |
|
|
what's the hydrostatic pressure in the glomerulus?
|
Hydrostatic pressure in glomerulus – equal to MAP - 60-80mmHg
|
|
|
what's a normal GFR?
|
GFR 125 mL / minute
|
|
|
what is the creatinine clearance?
how is it measured? |
Close to accurate estimate of GFR
Calculated from concentration of creatinine in (24 hour) urine and blood |
|
|
what is ANP?
|
atrial natriuretic peptide. released in atrium in response to stretch receptors.
travels through the system and causes an increase in GFR and a decrease in secretion of angiotensin II, renin, alosterone, with the result of DECREASING blood volume and consequently arterial pressure. |
|
|
what is aldosterone?
|
secreted by adrenal cortex
promotes renal re-absorption of Na excretion of K |
|
|
talk through the renin angiotensin system's response to low blood pressure
|
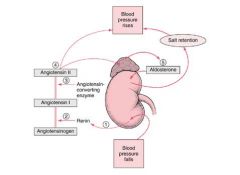
|
|
|
what is ADH?
|
Antidiuretic hormone ADH - re-absorbs water
secreted by anterior pituitary |
|
|
where is renin released from?
|
the juxtaglomerular apparatus
|
|
|
what is the normal specific gravity of urine?
|
Urine specific gravity – 1.010-1.025
|
|
|
what can a specific gravity of 1.001 -1.008 indicate?
|
Dilute – 1.001-1.018
Kidney infection, renal damage |
|
|
give a brief description of BUN, blood urea nitrogen, and give its normal level in mg/ dL
|
Blood urea nitrogen (BUN) – 7-18 mg/dl
Nitrogen portion of urea which is a byproduct of protein metabolism, excreted through kidney. Elevated with impaired kidney function Index of glomerular filtration |
|
|
what is the "third space"
|
the transcellular compartment located in strategic body areas where there is continual movement of body structures (pericardial sac, peritoneal cavity, pleural cavity).
|
|
|
4 (book) causes of edema
IDIO |
1. increased capillary pressure (A. Increased vascular volume - HF, kidney disease, etc. B. Venous Obstruction C. Decreased arteriolar resistance (calcium channel blocking meds)
2. decreased colloidal osmotic pressure (loss of plasma proteins, decreased production of plasma proteins, such as in liver disease) 3. Increased capillary permeability (allergy, infammation, malignancy, tissue injury and burns) 4. Obstruction of lymphatic flow (malignant obstruction, removal of lymph nodes) |
|
|
cellular changes that occur with glomerular disease
|
1. increases in glomerular or inflammatory cell number
2. basement membrane thickening (membranous) 3. changes in noncellular glomerular components (sclerosis and fibrosis) |
|
|
what is sclerosis in glomerulonephritis?
|
sclerosis refers to an increase in the amount of extracellular material in the mesangial, subendothelial, or subepithelial tissue of the glomerulus
|
|
|
what is fibrosis in glomerulonephritis?
|
fibrosis refers to the deposition of collagen fibers.
|
|
|
glomerular changes:focal vs. diffuse vs. segmental vs. mesangial
|
focal: only some glomeruli are affected
diffuse: involving all glomeruli and all parts of glomeruli segmental: only a certain segment of each glomerulus is affectetd mesangial: affecting only mesangial cells. |
|
|
what is azotemia?
|
a build-up of nitrogenous products in blood.
|
|
|
chain of events in glomerulonephritis
|
1. Inflammation of glomerular structures
- Immune complexes become trapped in glomerular capillary membrane causing inflammatory response 2. Disruption of capillary membrane - Capillary permeability increases to plasma proteins and blood cells – proteinuria, hematuria, pyruria, azotemia 3. Glomerular filtrate decreases - oliguria 4. Sodium and water retention produce edema |
|
|
acute nephritic syndrome
|
recent onset of hematuria and proteinuria, impairment of kidney function (azotemia), and salt and water retention causing edema and hypertension.
|
|
|
Rapidly progressive glomerulonephritis
|
progression of renal failure over days to weeks, in most cases in the context of nephritic presentation, typically assoicated with pathologic finding of extensive glomerular crescent formation on renal biopsy
|
|
|
Nephrotic syndrome
|
nephrotic-range proteinuria (>3.5 g in 24 h), hypoalbuminemia, hyperlipidemia, lipiduria.
|
|
|
describe renal tubular acidosis (+2 types)
|
Defects in re-absorption of bicarbonate or excretion of hydrogen which results in metabolic acidosis
Proximal renal tubular acidosis – milder form (sometimes called type II) Defect in re-absorption of bicarbonate (loss of bicarb) Sodium loss, hypovolemia, aldosterone secretion & decreased serum potassium Distal renal tubular acidosis Failure to secrete hydrogen Sodium loss, hypokalemia as above |
|
|
most common type of renal cancer?
|
Renal cell carcinoma – 80-85%
Risk factors Chronic renal calculi Cystic disease, chronic renal insufficiency Smoking, obesity Occupational exposures – asbestos Rare hereditary form Asymptomatic in early stages, then hematuria, pain, palpable mass in flank area |
|
|
phases of acute renal failure
|
1. Initiation period – initial insult or injury
2. Oliguric period - < 400 ml of urine produced in 24 hours, elevated creatinine, BUN, K, Mg, S/S appear 3. Diuretic period – increase U/O, labs normal Recovery period – improved renal function, normovolemia. 3-12 months. 1-3% permanent reduction in GFR |
|
|
stage I-V description of chronic kidney disease
|
Stage 1 – GFR - 90% (kidney damage)
Stage 2 – GFR 60-89% Stage 3 – GFR 30-59% Stage 4 – GFR 15-29% Stage 5 – GFR < 15% (kidney failure) |
|
|
causes of acute renal failure
|
1. Prerenal
- hypovolemia - decreased vascular filling - HF and cardiogenic shock - deacreased renal perfusion (sepsis, vasoactive mediators,etc.) 2. Intrinsic or Intrarenal - Acute tubular necrosis (prolonged ischemia, exposure to nephrotoxic drugs, heavy metals, etc. 3. Postrenal - Bilateral ureteral obstruction - Bladder outlet obstruction |
|
|
causes of chronic renal failure
|
1. Systemic disease
Diabetes / Hypertension Chronic kidney infections, inflammation, obstruction Vascular disease 2. Medications, toxins 3. Environmental / occupational agents – lead, mercury, arsenic |
|
|
clinical manifestations of acute renal failure
|
Changes in urine
Increased creatinine, BUN Azotemia (uremia) – uremic frost Hyperkalemia Metabolic acidosis Abnormalities in calcium, phosphorus Anemia |
|
|
right coronary artery
|
Inferior wall L ventricle
R atrium, ventricle SA node, AV node Becomes the right posterior descending coronary artery Posterior surface R&L ventricle |
|
|
left coronary artery
|
Left anterior descending (LAD)
1-4 diagonals Anterior wall L ventricle Portion of the R ventricle Circumflex L atrium, lateral, posterior wall L ventricle SA node |
|
|
ischemia, injury, and infarction. How do these differ?
|
ischemia - A temporary deficiency of blood flow to an organ or tissue.
The deficiency may be caused by diminished blood flow either through a regional artery or throughout the circulation. infarction - Death of tissue that results from deprivation of its blood supply. injury - trauma or damage to the tissue |
|
|
Reynaud's disease
|
A primary vasospastic disease of small arteries and arterioles; the cause is unknown. There is an exaggerated response of vasomotor controls to cold or emotion.
|
|
|
mitral stenosis
|
Incomplete opening of mitral valve
Left atrial distention Pulmonary congestion Incomplete left ventricle filling Decreased cardiac output |
|
|
aortic stenosis
|
blood is unable to flow freely from the left ventricle to the aorta.
|
|
|
2 disorders of the pericardium
|
1. Pericardial effusion – accumulation of fluid in the pericardial cavity
Injury, inflammation, altered capillary dynamics Compression on heart, limits venous return Pericardial tamponade – blood, fluid, pus 2. Pericarditis – inflammation of pericardium Secondary to other systemic diseases, infections |
|
|
conduction system of the heart
|
SA node
Internodal tracts AV node Bundle of His right and left bundle branches Perkinje fibers |
|
|
causes of HF
|
Hypertension
AMI Congenital heart disease Diseases of the myocardium Cardiomyopathies Myocarditis Pericarditis / cardiac tamponade Cardiac dysrhythmias |
|
|
symptoms of HF
|
Dyspnea, orthopnea
Rales, pleural effusions Cyanosis Frothy sputum Fatigue Decreased urinary output Edema Hypo/hypertension S3 gallop |
|
|
5 complications of AMI
|
Ventricular Dysrhythmias (esp. dangerous)
Hypotension Cardiogenic shock – decreased cardiac output, decreased tissue perfusion Myocardial rupture Ventricular aneurysms – hypertrophy, thinning |
|
|
treatment of AMI
|
Medical management
Oxygen, aspirin, morphine, nitroglycerin Antiplatelet, antithombin medications – aspirin, plavix, heparin, integrilin Thombolytics (fibrinolytics) – clot dissolver (e.g., TPA, retivase) Percutaneous coronary intervention (PCI) Angioplasty, stent Coronary artery bypass graft (CABG) |
|
|
hypertonic
isotonic is.... hypotonic is... |
350 mOsm
280 mOsm / L 200 |
|
|
sodium level
|
135-145 mEq/L
|
|
|
potassium level
|
3.5-5.3 mEq/L
|
|
|
choloride level
|
97-110 mEq/L
|
|
|
phosophate level
|
3.0-4.5 mg/dl
|
|
|
magnesium level
|
1.3-2.2 mEq/L
|

