![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
57 Cards in this Set
- Front
- Back
|
Generally what you're looking for on CXR for interstitial lung disease
|
bilateral interstial opacities
|
|
|
alveorlar disease looks like what on CXR?
|
Fluffy, cotten-y,
|
|
|
ILD Clinical Features (4)
|
Insidious onset of DOE and/or cough is most common.
Spontaneous pneumothorax (especially eosinophillic granuloma) Manifestations of extrathoracic disease (sarcoidosis, collagen vascular) Can present with systemic symptoms (fever, weight loss, arthralgias) |
|
|
ILD Physical Exam (4)
|
1) Bibasilar crackles
2) Clubbing 3) Signs of pulmonary hypertension 4) Signs of systematic involvement |
|
|
Chest X-Ray: General Features
|
Bilateral interstitial changes, usually symmetric
Volume loss |
|
|
Types of interstitial pattern (5)
|
A. Ground glass
Diffuse clouding: discrete lesions cannot be detected Seen with early stages of most ILD B. Nodular Often reflects blood stream dissemination (miliary Tb, talcosis) C. Reticular – networks of linear densities D. Reticulonodular – combination of b and c E. Honeycomb Air-containing, cystic spaces 5-10 mm in diameter in vicinity of overt interstitial disease Represents end-stage fibrotic lung of any etiology |
|
|
classic ild
|
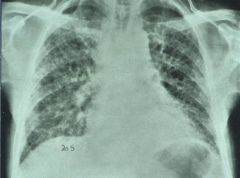
?
|
|
|
ild
|
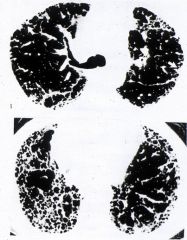
?
|
|
|
What do Pulmonary function tests show in ILD?
|
A. Restrictive lung disease
B. Low diffusing capacity (DLCO); striking drop in oxygenation during exercise C. Usually normal air flows (FEV1%) D. May have obstructive component; small airways disease, superimposed bronchiectasis |
|
|
What do Arterial blood gases show in ILD (early) ?
|
Early: Rest: near normal PO2 (generally low PCO2)
- Exercise: sharp drop in O2 sat |
|
|
What do Arterial blood gases show in ILD (late) ?
|
Late: Rest: Hypoxemia worsened by exercise (PCO2 may rise to normal or elevated values as respiratory status worsens)
|
|
|
Interstitial pneumonitis (alveolitis):
A. Usually mixed population of cells (mononuclear cell/polys) with _________ cell predominance B. May have eosinophilic component C. Granulomas may be present |
mononuclear
|
|
|
Pathology assoc with ILD
|
1) Interstitial pneumonitis (alveolitis)
2) Fibrosis 3) Bronchiectasis 4) As disease progresses, may see sequence of: interstitial pneumonitis→ pneumonitis plus fibrosis → severe fibrosis → honeycombing + bronchiectasis |
|
|
This is sarcoidosis. What's in the middle?
|
Granuloma
|
|
|
What can cause granulomatis inflammation?
|
look it up (Crohn's disease, tuberculosis, Leprosy, sarcoidosis, berylliosis and syphilis. It is also a feature of Wegener's granulomatosis and Churg-Strauss syndrome, two related autoimmune disorders-per wikipedia)
|
|
|
Causes of Pneumoconiosis
|
silica, asbestos, beryllium, coal
|
|
|
Causes of Hypersensitivity pneumonitis
|
thermophillic actinomyces, bacteria, amoebae, fungi
(farmer's lung) |
|
|
Drugs/Poisons assoc with ILD
|
1. Chemotherapeutic agents (bleomycin, busulfan, methotrexate, chlorambucil, melphalan, etc.)
2. Antibiotics (nitrofurantoin) 3. Gold 4. Methylsergide 5. Paraquat 6. Hexamethonium, mecamylamine, pentolinium, etc. 7. Talc 8. Hydrochlorothiazide 9. Cromolyn 10. Amiodarone 11. Cooking oil contaminated with rapseed oil |
|
|
Connective Tissue diseases Associated with ILD
|
1. Rheumatoid arthritis
2. Progressive systemic sclerosis 3. Mixed connective tissue disease 4. Polymyositis / dermatomyositis 5. Systemic lupus erythematosus 6. Ankylosing spondylitis 7. Sjogrens |
|
|
Idiopathic association with ILD
|
1. Sarcoidosis
2. Vasculitis (interstitial disease usually is minor component) 3. Histiocytosis X – Eosinophilic granuloma 4. Idiopathic pulmonary fibrosis 5. Idiopathic pulmonary hemosiderosis 6. Chronic pulmonary alveolar proteinosis 7. Tuberous sclerosis 8. Familial pulmonary fibrosis |
|
|
Vasculitides having the Lung Primarily involved:
|
Wegener’s granulomatosis
Lymphomatoid granulomatosis Churg-Strauss vasculitis |
|
|
Vasculitides having the Lung secondarily involved
|
Systemic leukocytoclastic vasculitis
|
|
|
Infectious associationws with ILD
|
Usually residue from widespread active
inflammation: mycobacterial, fungal, parasitic, Pneumocystis, viral |
|
|
General Approach to the Patient With Interstitial Lung Disease
|
A. Establish diagnosis
B. Evaluate extent / severity of pulmonary and nonpulmonary involvement C. Evaluate inflammatory activity (controversial) D. Treatment |
|
|
Diagnostic Evaluation of Interstitial Lung Disease
|
1. History and Physical
2. Chest x- ray 3. CT chest (high resolution) 4. Pulmonary Function Tests 5. Arterial blood gas, exercise oximetry 6. Various Serology 7. Gallium Scan 8. Bronchoscopy with Bronchoalveolar Lavage and Transbronchial Biopsy 9. Open Lung Biopsy |
|
|
Classic ILD with lymphadenopathy - hilar adenopathy = sarcoidosis
|
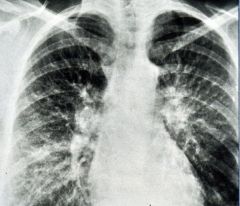
?
|
|
|
Chest X-ray
Upper Lobe involvement Predominant: |
A Ankylosing spondylitis
S Sarcoidosis S Silicosis E Eosinophilic granuloma T Tuberculosis |
|
|
Lower Lobe Predominant
|
B Bronchiectasis
A Asbestosis D DIP / UIP / IPF B Breast A Aspiration S Sarcoidosis S Scleroderma |
|
|
Mid-Lung Predominant
|
Sarcoidosis
Uremia Congestive heart failure Goodpasture’s Pulmonary alveolar proteinosis |
|
|
Pulmonary histology not needed for what disorders?
|
A. Collagen vascular
B. Asbestosis |
|
|
When lung tissue is needed, it can be obtained via:
|
A. Transbronchial bx
B. Open bx / Video Assisted Thoracoscopy (VATS)– the gold standard |
|
|
Transbronchial bx – useful if positive, especially in sarcoidosis, infections, tumor; not interpretable if normal or if shows "______"
|
“interstitial pneumonitis”
|
|
|
Open bx / Video Assisted Thoracoscopy (VATS)– the gold standard; however, still is often only compatible with a diagnosis and most helpful in __________.
Tissue should be obtained from several areas within lung, including obviously involved regions, and areas that appear relatively normal |
ruling out other diagnoses.
|
|
|
Interstitial Lung Diseases That can be Diagnosed by Transbronchial Biopsy (10)
|
1. Sarcoidosis
2. Inorganic Dust Diseases 3. Hypersensitivity Pneumonitis 4. Histiocytosis X 5. Pulmonary Hemorrhage Syndromes 6. Eosinophilic Pneumonia 7. Drug – induced Interstitial Disease 8. Lymphangioleiomyomatosis 9. Infections 10. Tumors |
|
|
Interstitial Lung Diseases that can be Diagnosed by Bronchoalveolar Lavage (4)
|
1. Pulmonary Alveolar Proteinosis
2. Pulmonary Hemorrhage Syndromes 3. Histiocytosis X 4. Infections |
|
|
Interstitial Lung Diseases with Increased Polymorphonuclear Leukocytes on Bronchoalveolar Lavage (6)
|
1. Idiopathic Pulmonary Fibrosis
2. Collagen Vascular Disorders 3. Asbestosis 4. ARDS 5. BOOP 6. Infection |
|
|
Interstitial Lung Diseases with Increased Lymphocytes on Bronchoalveolar Lavage (4)
|
1. Sarcoidosis
2. Hypersensitivity Pneumonitis 3. BOOP 4. Idiopathic Pulmonary Fibrosis |
|
|
Esophageal manometrics is associated with what disease
|
(Scleroderma)
|
|
|
Collagen vascular serologies show what?
|
A. sed rate, ANA, rheumatoid factor
B. anti Scl – 70 , anti centromere antibody C. ANCA (anti neutrophil cytoplasmic antibody) D. anti Jo, anti PM 1 E. antiglomerular basement membrane antibody (Goodpasteurs) |
|
|
IgG precipitating antibodies – positive in 90% of patients with acute ______ _______
|
hypersensitivity pneumonitis
|
|
|
ACE – abnormally high levels suggestive but not diagnostic of ______
|
sarcoidosis
|
|
|
Evaluation of Extent / Severity of Organ Involvement:
Pulmonary tests: |
A. PFT with DL CO
B. Exercise ABG or O2 sat (oximetry) |
|
|
The concept of alveolitis
A. Inflammation of the lower respiratory tract precedes and causes subsequent fibrosis B. The symptoms and physiologic derangements of ILD can result from inflammation or fibrosis. Are those due to fibrosis are reversible? |
no
|
|
|
Quantification of inflammatory activity may provide an index of:
(1) Amount of reversibility in a patient’s defect (2) Risk of a patient subsequently developing pulmonary _________ |
fibrosis
|
|
|
Indices of Sarcoidosis
(5) |
(1) ACE
(2) Lavage (% T lymphs, % OKT4 (+) lymphs) (3) SPEP (4) Gallium scan (5) Lysozyme |
|
|
Indices of Idiopathic pulmonary fibrosis (2)
|
(1) Gallium scan
(2) Lavage (% polys, % eos) |
|
|
Treatment for asbestosis
|
none
|
|
|
Treatment for Eosinophillic granuloma
|
not effective
|
|
|
Treatment for Idiopathic pulmonary fibrosis, sarcoidosis, hypersensitivity pneumonitis
|
steroids still controversial as to who to treat and with how much;
cytotoxic agents even more controversial; gamma interferon |
|
|
Treatment of Wegener’s
|
cytotoxin + steroids;
imuran, bactrim in selected patients |
|
|
Treatment of Goodpasture’s
|
cytoxan + plasmapheresis
|
|
|
O2 for patients with:
A. Polycythemia B. PaO2 < _?_ (resting, exercise, or sleep) |
55
|
|
|
most likely findings in moderate ILD
|
lung capacity decr
FEV1 percent normal diff capac decr |
|
|
most common blood gas finding in early mild ILD
|
mild resp alkalosis
no resting hypoxemia oxy dest with exercise no metabolic acidosis (distractor) |
|
|
there are 2 type of granuloma
|
necrotizing (necrosis involved)
non-necrotizin |
|
|
necrotizing disease?
|
TB
|
|
|
non-necrotizing granulomas diseases
|
sarcoid and autoimmune dis
|

