![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
50 Cards in this Set
- Front
- Back
|
Eye: what questions should be asked in the history? |
Change in vision Pain (Dull & deep orSharp/Foreign-body Itching /irritation Lacrimation (tears) Discharge Photosensitivity Halos Contact lenses Hx of Trauma/chemical injury Hx of ocular procedure/surgery Hx of dermatologic/autoimmune/rheumatologic |
|
|
What should be inspected during an eye exam? |
-Inspection of all anatomy (lid,conjunctiva, sclera, iris, pupil, lens, anterior/posterior aqueous humour -Visual acuity -Ocular movement -Pupillary size, equity in shape,round (r/o glaucoma and iritis) -Pupillary light reflexes -Gross exam of the anterior segmentwith a penlight or slit lamp -Ophthalmoscopy exam -Fluorescein dye and cobalt bluelight (green highlights corneal lesion and white highlights corneal opacity) -Portable tonometer measures intraocular pressure(r/o glaucoma) |
|
|
What are the red flags of the eye assessment? (Require ER referral) |
1. Vision loss 2. Pt respots flashes of light 3. Severe pain 4. Severe photophobia 5. Blurry vision – if it is associated with any of the above symptoms 6. Abnormal assessment of the pupils – abnormal shape, fixed or nonreactive to light 7. Diplopia or nystagmus – if associated with any of the above symptoms 8. Evidence of occular hemorrhage 9. Conjunctivitis in newborns |
|
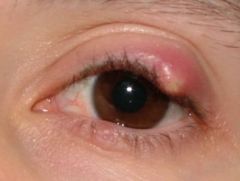
Identify this condition. |
Hordeolum |
|
|
What is a hordeolum? |
External hordeolum: infection of the sebaceous glands of the eyelid Internal hordeolum: infection of the eyelid margin; rare Usually caused by a staphylococcus infection |
|
|
What are the clinical manifestations of hordeolum? |
Redness, swelling and tenderness May have tearing, photophobia and a foreign-body sensation Small, yellowish pustule at the base of the eyelash (often ruptures and discharges pus to relieve pain and resolve lesion) Specific to internal hordeolum: Inflammation may be severe, sometimes with fever or chills. |
|
|
What is the treatment for a hordeolum? |
1. hot compress 2. oral antibitotics (if not responsive to compress) 3. incision and drainage (if needed) 4. topical antibiotics are usually ineffective Usually resolves in 2-4 days |
|
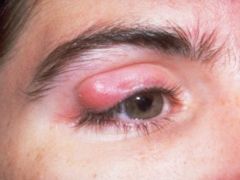
Identify this condition. |
Chalazion |
|
|
What is a chalazion? |
Obstruction of the meibomian (oil-secreting) gland. Non-infectious. |
|
|
What are the clinical manifestations of a chalazion? |
Redness, swelling, early tenderness. With time is becomes small, non-tender nodule or lump |
|
|
How do you diagnosis a hordeolum and chalazion? |
Clinical presentation, conditions may be indistinguishable for first two days. Internal hordeolum is rare so should only be investigated if chills and fever present. |
|
|
What is the treatment for chalazion? |
Hot compress Incision and curettage Intrachalazion corticosteroid therapy Resolves in 2-8 weeks |
|
|
What is blepharitis? |
-Inflammation of the eyelid -Acute or chronic -Anterior: eyelid skin and lashes -Posterior: meibomian glands -Can be caused by infection (s. aureus) |
|
|
What are the signs and symptoms of blepharitis? |
-Burning -Pruritis -Crusting/drainage -Erythema -Thickening of lid (chronic) -NO acute pain, NO changes in visual acuity |
|
|
What is the treatment for blepharitis? |
-Compress -Clean lids with baby shampoo -Avoid use of contacts or cosmetics -Topical erythromycin or polysporin |
|
|
What are the four types of conjunctivitis? |
1. Bacterial 2. Viral 3. Gonococcal and chlamydial 4. Allergic |
|
|
What are the most common organisms of bacterial conjunctivitis? |
s. aureus, s. pneumoniae, h. influenzae, m. catarrhalis |
|
|
What are the clinical manifestations of bacterial conjunctivitis? |
-rapid onset of redness -gluey/sticky eyelids, crusts in morning -copious, thick mucopurulent discharge -more discharge = more severe -pain, foreign body sensation -photophobia is a sign of corneal infiltration |
|
|
What is the non-pharm treatment for bacterial conjunctivitis? What is the OTC treatment for bacterial? What is the Rx treatment for bacterial? (Adults and children > 1yr) |
Self limiting, delay abx, hand and eye hygiene OTC: polysporin eyedrops/ointment Rx: erythromycin ointment, fucidin drops |
|
|
What are the clinical manifestations of viral conjunctivitis? |
-thin, clear, watery discharge; minimal lash crust -rapid onset of diffuse redness -itchy eyes; history of conjunctivitis -foreign body sensation -tearing |
|
|
What conjunctivitis is most common in children? Adults? |
Children - bacterial Adults - viral |
|
|
What are the clinical manifestations of allergic conjunctivitis? |
-Itchy; worse with rubbing -watery, thin discharge; white rope like discharge may be present -bilateral diffuse redness -eyelids red or edematous -other allergic symptoms present |
|
|
What type of conjunctivitis needs an urgent referral? What are the clinical manifestations of this type? |
Gonococcal and chlamydial -tender pre-auricular lymphadenopathy -rapid onset of unilateral redness -lid edema *Corneal perforation can occur |
|
|
In what population do you need an urgent referral for peri-orbital/orbital cellulitis? |
Paediatric population |
|
|
What is periorbital cellulitis? What is orbital cellulitis? |
1. infection of the eyelid and surrounding skin anterior to the orbital septum; usually begins superficial to the orbital septum (lid only) 2. infection of the orbital tissues posterior to the orbital septum; usually begins deep to the orbital septum (affects eye structures) |
|
|
What are the clinical manifestations of periorbital cellulitis? orbital cellulitis? |
Both disorders can cause tenderness, swelling, warmth, redness or discolouration of the eyelid, and fever Orbital cellulitis is likely if there is: decreased ocular motility, pain with eye movements, proptosis, or decreased visual acuity |
|
|
What diagnostic studies can you use to diagnosis periorbital cellulitis/orbital cellulitis? |
-Swab for C&S -CBC + differential -ESR -BC |
|
|
What is the treatment for periorbital cellulitis? What is the treatment for orbital cellulitis? |
Peri: Oral antibitotics gm + coverage (cephalexin, clindamycin) Orbital: Hospitalization, IV abx, surgical drainage if abscess, optho referral |
|
|
What is glaucoma? |
Increased intraocular pressure Intraocular pressure is controlled by the aqueous humour in the anterior chambers of the eye. Can be suspected when the intraocular pressure is > than 22 mmHg. |
|
|
What are the two types of glaucoma? Which type is a medical emergency? |
1. Primary open angle glaucoma 2. Angle closure glaucoma - Medical emergency |
|
|
What are the clinical manifestations of primary open angle glaucoma? |
Peripheral vision loss which eventually may lead to central vision loss. May lead to blindness. These symptoms are usually insidious, and patients may be asymptomatic for a significant period of time. |
|
|
What are the clinical manifestations of angle closure glaucoma? |
Sudden vision loss, blurred vision, pain, halo appearance around lights |
|
|
What is the treatment for glaucoma? |
Beta-adrenergic blockers (Timolol) - receptor blocker in ciliary epithelium, thus lowering pressure because there is less aqueous humor production Prostaglandin analongs (latanoprost, travoprost) - lower pressure by increased outflow of aqueous humor |
|
|
What is a cataract? |
Progressive, painless clouding of the (normally clear) lens -Results in localized or generalized vision loss and eventual blindness (assess visual acuity) |
|
|
What is the most common cause of cataracts? |
-Aging -Occurs in 92% of those 75 and older (females>males) -Can be congenital |
|
|
What are the signs and symptoms of cataracts? |
-May be asymptomatic -Cloudy vision -Difficulty driving at night -Halos around lights |
|
|
What is the treatment for cataracts? |
-May not always be advised if not affecting vision axis -Surgery |
|
|
Briefly describe amblyopia |
Lazy eye; reduction or dimness of vision forunknown reasons -Associated with strabismus, anisometropia,diabetes, renal failure, malaria, alcohol, tobacco -Most common cause of vision loss in children -Treated by patching unaffected eye or extended timeperiods to ensure use of affected eye |
|
|
Briefly describe scotoma |
-Circumscribeddefect of the central field of vision; has serious impact on visual acuity |
|
|
Breifly describe nystagmus |
Involuntary eye movement that is rapid and repetitive -Can be vertical, horizontal, circular -Congenital vs acquired |
|
|
Briefly describe strabismus |
Deviation of one eye from the other when looking at an object. It results in the failure for the affected individual to focus both eyes on the same object and loss of binocular vision. -Primary symptom is diplopia |
|
|
What is macular degeneration? |
Central scotoma (loss of vision), blurred or distorted central vision, difficulty with reading and night vision |
|
|
What are the two types of macular degeneration |
Atrophic (dry) -Most common -Gradual vision loss -Caused by aging Exudative (wet) -Faster and more pronounced vision loss -Abnormal growth of vessels behind retina = hemorrhage and swelling |
|
|
What is retinal detachment? What is the treatment? |
-Retina is detached or pulled from normal position -Requires immediate medical attention to prevent permanent vision loss -Laser eye surgery or freeze treatment |
|
|
What is the most common type of retinal detachment? |
Rhegmatogenous - tear of break in the retina, allowing fluid to get between retina and retinal pigment epithelium (RPE), causing outer retina to be deprived of oxygen and nutrients |
|
|
What is hyphemia? |
Blood floating within the anterior chamber of the eye -Most commonly occurs after trauma -Eye pressure should be monitored for signs of glaucoma |
|
|
What is corneal abrasion? |
Superficial trauma to the thin epithelial layer of the cornea -Pts present with photophobia and moderate to severe pain -May Rx erythromycin prophylactically |
|
|
What is keratitis? |
-Inflammation of the cornea -Bacterial -S/S: pain, photophobia, tearing, FB sensation, diplopia, conjunctival hyperemia -May do C/S and stain of ulcer -Tx: d/c/ contact lens use, lubricate eye, abx Refer to opthalmology |
|
|
What is uveitis? |
-Inflammation of the uveal tract -Immunologic origin HLA-B27 -S/S: unilateral, pain, photophobia, vision loss, small pupil, ciliary flush, corneal opacities -Refer to opthalmology |
|
|
What conditions require referral to an optho? |
Scleritis, uveitis, acute angle closure glaucoma, keratitis |

