![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
61 Cards in this Set
- Front
- Back
|
What are the functions of blood vessels? |
O2/nutrient delivery CO2/waste removal Delivery of hormonal signals Regulate blood flow |
|
|
What is macrovasculature? What diameter is the cutoff for a macro vessel? |
Vessels greater than 0.1 mm diameter - arteries and veins |
|
|
What radius defines micro vasculature? |
Vessels smaller than 0.1mm in diameter - arterioles, capillaries, venules |
|
|
What is a portal system? |
Where blood is carried from one site to another without direct involvement of the heart |
|
|
Give two examples of a portal system |
- Hepatic portal system, from the GI tract to the liver - hypothalamic-pituitary portal system |
|
|
What types of tissue are vessel walls made of? |
Endothelium Muscle/elastic tissue Connective tissue |
|
|
Which is larger, an artery or a vein? |
Vein |
|
|
What are the three layers of blood vessel walls? |
Tunica intima - endothelium Tunica media - muscle/elastic Tunica adventitia - connective |
|
|
What is the tunica intima composed of? |
- A single layer of squamous epithelial cells and the associated basal lamina - Sub-endothelial connective tissue - internal elastic lamina |
|
|
What is the tunica media composed of? |
- Either smooth muscle cells, oriented concentrically, or elastic fibres - external elastic lamina |
|
|
What is the tunica adventitia made of? |
- Fibro elastic connective tissue arranged longitudinally - some Adipose tissue |
|
|
What are the elastic laminae? |
Thin bands of elastic tissue on the outermost layers of the intima and media |
|
|
Which of the blood vessels contain more developed tunica intima/media? |
Arteries |
|
|
What is the function of the tunica intima? |
- To regulate blood clotting, vascular tone and blood flow - to secrete collagen, lamin, endothelin, nitric oxide and von Willebrand factor - also contains ACE1 and ACE2 to regulate blood pressure |
|
|
What does endothelin do? |
A vasoconstrictor |
|
|
What effect does nitric oxide have on arterial diameter? |
It is a vasodilator, so it increases it |
|
|
What is von Willebrand factor? What does it associate with? |
A clotting protein which binds to factor VIII |
|
|
What is ACE? What do they do? |
Angiotensin Converting Enzyme. There are two types, ACE1 and ACE2. ACE1 converts angiotensin-1 into angiotensin-2, which causes vasoconstriction. ACE2 has the opposite effect, converting angiotensin-2 into angiotensin (1-7), a vasodilator |
|
|
Why are ACE inhibitors useful drugs? |
They block the action of ACE1, reducing the production of the vasoconstrictor angiotensin-2, therefore lowering arterial resistance and BP |
|
|
What is the function of the tunica media? What cells/molecules does it contain? |
To provide tension and protection. It contains concentric smooth muscle cells, as well as elastic fibres, type III collagen and proteoglycans |
|
|
Which blood vessels don't have a tunica media? |
Capillaries and venules |
|
|
EDS IV is a defect in? |
Ehlers-Danlos Syndrome type IV, where a defect in type III collagen can lead to aneurysms |
|
|
What is the vasa vasorum? |
The 'vessels of vessels' that provide blood supply to the large arteries and, more often, veins |
|
|
Which layers do the vasa vasorum supply? |
Tunica media/adventitia |
|
|
What are the three types of arteries and what are their relative sizes? |
Elastic (conducting) - these are the largest, eg aorta and pulmonary arteries
Muscular (distributing) Arterioles - smallest |
|
|
Why do elastic arteries need to contain lots of elastic fibres? |
Because they have to withstand high and fluctuating pressures |
|
|
How does the elastin/muscle ratio change as distance from the heart increases? |
Less elastin, more muscle |
|
|
What is atherosclerosis? |
Chronic disease where arteries thicken, harden, lose their elasticity and eventually occlude |
|
|
What are the risk factors for atherosclerosis? |
Age Hypertension Diabetes Smoking High LDL levels |
|
|
What is the difference between LDL and HDL? |
LDL transport cholesterol to tissues and cells, and is relatively higher in lipoprotein. HDL Transports it to the liver, and is relatively lower in lipoprotein. LDL is associated with disease |
|
|
Describe the development of atherosclerosis? |
- Endothelial damage causes leukocytes to migrate to the site of damage and cause local inflammation - macrophages invade and take up LDL cholesterol, becoming foam cells - accumulation of foam cells causes a fibrous plaque to develop and potentially rupture |
|
|
What is coronary heart disease? Describe its symptoms |
- Narrowing or blockage of coronary arteries - angina, dyspnoea, sweating, left arm pain, irregular heart beat |
|
|
What are the risk factors for CHD? |
smoking, hypertension, obesity, high alcohol consumption, lack of exercise, stress |
|
|
What are the two kinds of stroke? |
Ischaemic stroke - Blood vessel becomes blocked Haemorrhagic stroke - blood vessel bursts |
|
|
What are the two classes of ischaemic stroke? |
Thrombosis - locally formed clot Embolism - migration of embolus from elsewhere |
|
|
By how long after a Stroke does a patient need to undergo thrombolysis? |
4.5 hours |
|
|
What is a thrombectomy? |
Passing a thin tube up the femoral artery and passing it up to the blood clot, trapping it in a wire mesh and pulling it out |
|
|
What is an AAA? |
Abdominal aortic aneurysm |
|
|
What is gangrene? |
Necrotic tissue as a result of ischaemia in peripheral tissues |
|
|
Which types of cell surround arterioles and venules? |
Smooth discontinuous muscle cells and pericytes |
|
|
What are pericytes? What can they do? |
Accompanying cells in the micro vasculature that can promote vessel stabilisation, regulate vascular tone and tissue perfusion, and can also differentiate into macrophages |
|
|
What can pericytes differentiate into? |
Fibroblasts Smooth muscle cells Macrophage Among other things |
|
|
What is angiogenesis? |
Formation of new blood vessels |
|
|
Why are arterioles called resistance vessels? |
Because they have the highest resistance of all the systemic circuit, meaning they set the entire peripheral resistance |
|
|
What are pre-capillary sphincters? |
A ring of smooth muscle surrounding the junction between an arteriole and a capillary, which can constrict to prevent flow down those capillaries |
|
|
What are the 3 types of capillary? |
Continuous Fenestrated Sinusoidal |
|
|
Describe continuous capillaries. Where do you find them? |
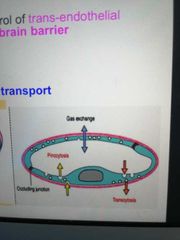
- They have no pores or fenestra in their walls - Present in muscle, nervous and connective tissue where protein passage isn't needed |
|
|
Describe Fenestrated capillaries |
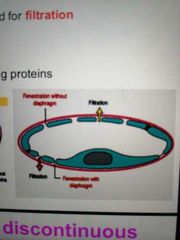
They have 60-80 nm pores in their walls Found in vessels where protein passage is needed, eg kidney The pores have diaphragms |
|
|
Describe Sinusoidal capillaries? |
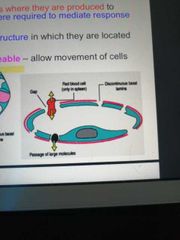
Discontinuous epithelial cells, with large fenestrae Promote enhanced protein and cell passage Found where leukocytes need to migrate in order to promote immune response |
|
|
What are arteriovenous shunts? |
Channels in the vascular system that allow capillary beds to be bypassed. Common in the skin to allow thermoregulation |
|
|
Where would you find an arterio-arterial anastamosis? |
Circle of Willis in the brain |
|
|
Where would you find a veno-venous anastamosis? |
Portacaval anastamosis - hepatic portal system |
|
|
Where would you find an arterio-venous anastamosis? |
Finger tips or skin |
|
|
What is diapedesis and where does it typically take place? |
Migration of cells such as neutrophils and monocytes through the blood vessel walls. Typically in small veins or venules |
|
|
What are varicose veins? |
Where the valves in the veins no longer work properly, allowing blood to flow backwards, causing distension of the veins. Especially prominent in the legs |
|
|
What is DVT? |
Deep vein thrombosis, a blood clot in one of the deep veins in the body. Could break off and travel to the lungs, causing a pulmonary embolism |
|
|
What is vasculitis? Two types, symptoms, potential cause? |
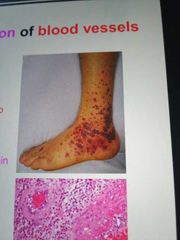
Inflammation of veins (phlebitis) or arteries (arteritis) Causes purpura of the skin, thought to be autoimmune |
|
|
Give three important blood barriers |
Blood brain barrier Blood air barrier Kidney filtration barrier |
|
|
What is the blood brain barrier composed of and what is its function? Draw a diagram |
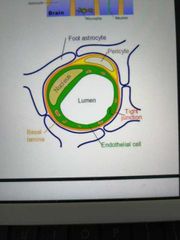
Specialised endothelial cells containing tight junctions Astrocytes Pericytes Microglia
It prevents paracellular and transcellular diffusion between the blood and the brain |
|
|
What is the blood-air barrier composed of? |
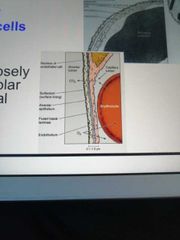
Cytoplasm of alveolar cells Cytoplasm of endothelial cells Fused basal laminae of these two layers |
|
|
What is the kidney filtration barrier composed of? |
Thin Fenestrated endothelium of capillaries Basal lamina, fused with podocytes |

