![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
32 Cards in this Set
- Front
- Back
|
Preferred Bone Marrow Bx Site |
Iliac crest |
|
|
Bence-Jones Test |
Measures the level of abnormal proteins (called Bence-Jones proteins) in the urine
Used to Dx multiple myeloma
Normal test is (-) |
|
|
Schillings Test |
24h urine collection assesses the excretion of B12 in urine
Oral B12 given followed by IM B12 1 - 2 hours later
Must be NPO until IM B12 is given
Used to Dx pernicious anemia |
|
|
Risk Factors for Blood Disorders |
EtOH
Smoking |
|
|
Assessment: Cognitive/Perceptual Changes |
Pain- esp. joint pain, bone pain
Note any strange sensations - changes in taste, vision, hearing; numbness/tingling/paresthesias
|
|
|
Assessment: Physical Exam |
General condition and appearance; fever
Skin
Lymph nodes
Abdomen - spleen/liver enlargement, abd girth |
|
|
Nursing Assessment of Lymph Nodes |
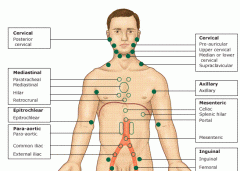
Systemic assessment
Cervical, axillary, mediastinal, epitrochlear, mesenteric, para-aortic, inguinal
Symmetry, size, consistency (hard/soft), tender/non-tender |
|
|
Anemia |
reduction in either the number of RBCs, the amount of hemoglobin, or the hematocrit (percentage of packed RBCs per deciliter of blood) |
|
|
Polycythemia |
excess of RBCs |
|
|
Types of Anemia (Chart) |
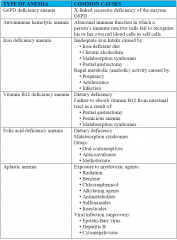
|
|
|
Glucose-6-phosphate dehydrogenase (G6PD) deficiency anemia |
X-linked recessive deficiency of the enzyme G6PD
10 - 14% black male US population and may also affect ]middle-eastern population
Usually not affected until stressor - infection or drugs (antimalarials, sulfa, nireofurantoin, NSAIDS); fava beans also associated with hemolytic response (favism)
Causes hemolytic crisis - |
|
|
Autoimmune hemolytic anemia |
Abnormal immune function in which a person’s immune reactive cells fail to recognize his or her own red blood cells as self cells
|
|
|
Iron deficiency anemia |
Inadequate iron intake caused by: • Chronic alcoholism • Malabsorption syndromes • Partial gastrectomy Rapid metabolic (anabolic) activity caused by: • Adolescence • Infection |
|
|
Vitamin B12 deficiency anemia |
Due to dietary deficiency
Can be caused by failure to absorb vitamin B12 from intestinal tract as a result of: • Pernicious anemia • Malabsorption syndromes
Can be caused by prolonged therapy with PPI, anti-epiletics, antihistamines, and metformin
B12 deficiency causes anemia by inhibiting folic acid transport and reducing DNA synthesis in precursor cells. These precursor cells then undergo improper DNA synthesis and increase in size.
Vit B12 deficiency anemia is not the same as pernicious anemia, but rather can be caused by pernicious anemia
Pernicious anemia is anemia resulting from a failure to absorb B12 and is caused by a deficiency of intrinsic factor (a substance normally secreted by the gastric mucosa) |
|
|
Folic acid deficiency anemia |
Dietary deficiency - a diet lacking green leafy vegetables, liver, yeast, dried beans, and nuts, is the most common cause
Malabsorption syndromes, such as Crohn’s disease, are the second most common cause
Chronic alcohol abuse with malnutrition is another cause
Drugs (oral contraceptives, anticonvulsants, methotrexate) can slow or prevent the absorption and conversion of folic acid to its active form, leading to folic acid deficiency and anemia |
|
|
Aplastic anemia |
Deficiency of circulating red blood cells (RBCs) because of failure of the bone marrow to produce these cells
Usually occurs with leukopenia and thrombocytopenia
Usualls occurs with pancytopenia (deficiency in RBC, WBC, and PLT)
Exposure to myelotoxic agents (radiation, sulfonamides, insecticides) |
|
|
S/S of Anemia |
Signs and symptoms are fatigue, palpitations, tachycardia, tachypnea, dyspnea, pallor, possibly CP, heart murmur, HA
Assess diet
Assess for potential causes of bleeding |
|
|
Chronic S/S of Anemia |
Chronic signs may include skin, hair and nail changes- glossitis, brittle hair (signs of nutritional deficiency) pica
May be asymptomatic |
|
|
Classification of Anemia: Normocytic |
RBC look normal
Blood loss - decreased H/H & low RBC
Aplastic |
|
|
Classification of Anemia: Microcytic |
Depletion of iron and Hgb stores resulting in small RBC
Iron deficiency
Also may be due to toxicities such as lead poisoning, neoplasm, chronic infection
Thalassemia - less hemoglobin and fewer red blood cells in your body than normal |
|
|
Classification of Anemia: Macrocytic (Megaloblastic) |
Enlarged, abnormal RBC as a result of improper DNA synthesis
B12 and Folic Acid Deficiency
Some drugs- phenytoin (Dilantin), sulfas
EtOH related - usually also has nutritional deficiency |
|
|
Classification of Anemia: Hemolytic |
Lysis of RBC
Inherited or acquired
Trauma- mechanical heart valves (can catch RBC when closes), hemodialysis etc. |
|
|
S/S of Aplastic Anemia |
Bone marrow failure and poor oxygenation • weakness, pallor, and petechiae/ecchymosis
CBC shows severe macrocytic anemia, leukopenia and thrombocytopenia
bone marrow biopsy may show replacement of cell-forming marrow with fat
Infection is common with leukopenia, especially neutropenia
Increased r/f bleeding d/t decreased PLT |
|
|
S/S of Folic Acid Deficiency Anemia |
Manifestations are similar to those of vitamin B12 deficiency, but nervous system functions remain normal because folic acid deficiency does not affect nerve function
The absence of neurologic problems helps distinguish folic acid deficiency from vitamin B12 deficiency
|
|
|
Pancytopenia |
A deficiency of RBC, WBC and PLT |
|
|
S/S of Vitamin B12 Deficiency Anemia |
Pallor, jaundice, glossitis (a smooth, beefy-red tongue), sore tongue, fatigue, and weight loss, abd pain, AMS/dimentia, N/V
Because vitamin B12 is needed for normal nerve function, patients with pernicious anemia may also have paresthesias (abnormal sensations) in the feet and hands, decreased vibratory sense, weakness, and poor balance
Neurologic/neuromuscular deficits may not be reversible |
|
|
S/S of Iron Deficiency Anemia |
weakness, pallor, fatigue, reduced exercise tolerance, fissures at the corners of the mouth
Nails become brittle, thin, coarsely ridged, or spoon-shaped and concave
Low H/H
Serum Fe values are less than 10 ng/mL; serum transferrin and IBC are increased |
|
|
Tx for Iron Deficiency Anemia |
Treat malnutrition or other conditions causing malnutrition (i.e. EtOH)
If acute blood loss, may need transfusion
Replace Fe - foods high in iron and good nutrition
Fe supplementation - oral is most common; enteric coated 150 - 200 mg 3 to 4 times daily given with OJ or vit C one hour before meals
Fe should be taken for 2 - 3 months after normalization of serum Fe
Liquid Fe stains teeth (and uniform!); have pt use straw
Can give with food if GI upset occurs
Always use Z-track with IM Fe (will tattoo skin)
Causes constipation and black tarry stools
KEEP AWAY FROM CHILDREN |
|
|
Foods High in Iron |
Lean meats - red meat
Organ meat (high in fat/cholesterol)
Fortified cereal
Beans and peas
Green leafy veggies
Eating with vit C enhances absorption |
|
|
Tx for Aplastic Anemia |
Remove causative agent (i.e. toxin)
Immunosuppressive therapy
Bone marrow transplant if severe (previous transplant increases r/f rejection)
Prevent/monitor for infection/bleeding |
|
|
Tx for B12 Deficiency Anemia |
Pernicious anemia - B12 IM therapy for life (oral B12 does not work because stomach cannot absorb it)
Oral B12 if not pernicious anemia
Dietary sources of B12 include animal products such as meat, eggs and dairy
Reserves are stored in liver
Vegetatians/vegans are at high r/f B12 deficiency anemia
Screen for gastric ca if pt has B12 deficiency |
|
|
Tx for Hemolytic Anemia |
Remove/limit cause
Corticosteroids (autoimmune)
Splenectomy (specifically autoimmune)
Blood transfusion if severe
|

