![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
35 Cards in this Set
- Front
- Back
|
What is mosaicism
|
the presence of two or more genetically distinct cell populations in a single individual
|
|
|
Types of mosaicisms
|
Chromosomal
- generalized - tissue specific or Single gene |
|
|
What is generalized mosaicism
|
occurs in postzygotic divisions (may begin as a normal or abnormal karyotype if is chormosomal
- X-inactivation - mosaic down syndrome |
|
|
What is X inactivation
|
- soon after fertilization, somewhere bw 8 and 32 cell there is an irrevical decision so that in the indiv with 2 X chromosomes, one of the Xs shuts down for dosage compensation
- all the descendant of that cell will now have the same X chr shut down - mosicism is then represented in all tissues - may express recessive condition - 50/50 shut down of mat or pat X - ex calico cat |
|
|
Mosaic down syndrome
|
- conceptus could begin as a trisomy, then lose one 21 chromosome in a cell in the first several division (meiotic event)
- or could begin as normal conceptus but have nondysjunction during a subsequent mitotic division |
|
|
How common is mosaic down syndrome in those kids with down syndrome?
|
2%
|
|
|
What is tissue specific mosaicism?
|
- one particular area, tissue or organ has confined mosaicism
|
|
|
3 types of tissue specific mosaicism
|
- somatic
- germline (subtype of somatic) - confined placental mosaicism (CPM) |
|
|
germline mosaicism
|
a type of tissue specific (somatic) mosaisim
- ex osteogenesis imperfecta (almost always lethal) |
|
|
If a germline mosaicism leads to baby born with osteogenesis imperfecta, what can you tell the mom about the likelihood of this recurring?
|
observed recurrence is 6%
- more than baseline population risk for mutation (<1%) ( if it have been a recessive trait, the recurrence would be 25%) |
|
|
What is confined placental mosaicism
|
- occurs at or after the third post-zygotic division (after conception)
- more likely to be seen in the placenta; with no mosaisism at the level of the embryo - can arise from normal diploid or abnormal zygote |
|
|
In development of placenta, blastocyst wall, inner cell mall give rise to?
|
- blastocyst wall give rise to chorion
- inner cell mass give rise to: >the embryo (three cells only), >yolk sac, >allantois and >parts of amnion |
|
|
How common is confined placental mosaicism in cases of mosaicism?
|
2%
|
|
|
What are some symptoms of CPM?
|
- normal
- intrauterine growth retardation - occasional overgrowth - fetal death |
|
|
Describe trisomic rescue
|
- conception begins as a trisomy
- in some cells the extra chromosome gets lost - the 3 cells that form the fetus carry on with the right # of chromosomes |
|
|
Why would there be poor fetal outcome in CPM?
|
- suboptimal placental function
- particular chromosome involved matters - proportion of normal:abnomal cells - ofter normal cells have better growth and tend to outgrow the abnormal cell - |
|
|
What % of CPM preg have prenatal or perinatal complications?
|
16-21%
|
|
|
What is the most common aneuploidy for conception?
|
trisomy 16
- BUT not seen amoung live born fetuses (letal in a non-mosaic state) |
|
|
What is uniparental disomy ?
|
inherting all or part of a pair of chromosomes from one parent
|
|
|
3 causes of UPD?
|
- trisomic rescue
- monosomic rescue (goes back to 46 chr) - gametic complementation |
|
|
UPD trisomic rescue
|
- start out with trisomic conceptus
- then have post-zygotic loss of the extra chromosome - if corrected in embyroblast lineage (3 cells), you can have a euploid fetus with trisomic placenta - depends which chr gets lost during time of correction - may end up with one mat and one pat chr OR 2 from one parent (UPD) |
|
|
What is genetic imprinting important in relation to UPD?
|
- severity of symptoms will depend on how much imprinting is involved
- some genes are only active if they pass through the mother/father |
|
|
Possible outcomes of trisomic rescue?
|
- 1/3 : one pat on mat (bi-parental inheritance)
- 2/3 : 2 pat or mat (UPD) |
|
|
Chr 15 and trisomic rescue
|
- it really matters which chormosome is rescued for chr 15 because it has blocks where genes are either maternally or paternally imprinted
|
|
|
Where would nondysjunction need to occur for fetus to end up with one homolgue of each? What is this called?
|
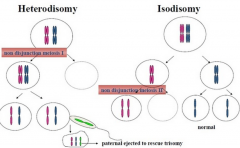
meiosis 1 ( chr dont separate and therefore what goes to cell is both chromosomes and so at time of meiosis 2, you will have both mat/pat present)
= heterodysomy ( most common) |
|
|
Where would the nondysjuction need to occur to end up with two homologues from one parent? What is this called?
|
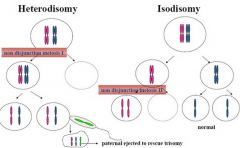
- Meiosis 2
- called isodisomy - chromatids (two copies of original chromosome) don't separate properly |
|
|
If a CF gene is present on the isodisomic chromatid, will the child have CF?
|
Yes. Isodisomy can uncover autosomal recessive disorders where the mutatins only came from one parent.
|
|
|
Gametic complementation
|
UPD - ex maternal nondysjuction + paternal nullisomy
|
|
|
Clinical features of CPM and UPD
|
- not yet well defined
- often difficult to differentiate the effects of CPM (ex trisomy 16) from the effects of UPD16 - IUGR displayed in both |
|
|
Clinical feature of UPD
|
- recessive disorder
- effects ay depend on the presence of imprinted genes - |
|
|
What is imprinting?
|
differential allelic expression depending on parent of origin
- need complete maternal and paternal sets of chromosomes from fetal development in mice - triploid gynogenic embryos - small placental tissue - triploid androgenic embryos - large placental with little or no embryo |
|
|
What is prader-willi syndrom?
|
15q11-13
- either paternal chr deleted or maternal UPD - presentation: massively obese - when born are skinny and hypotonic, but around at year they have a huge increase in appetite --> morbid obesity |
|
|
What is angelman syndrome
|
15q11-13
maternal chromosome deleted or paternal UPD - aka happy puppet - skinny appearance - do not thrive, many can't walk, minimal development |
|
|
Somatic gene mosaicism
|
- autosomal dominant
- individual is heterozygous for the mutation - cause cyst to develop in kidneys - individual is heterozygous but homozygous in terms of cysts - cysts cell are clonal ( from one cell or event) - mosaic for cells with only germline mutation and cells with both that and inactivation mutation - commonest genetic cause for chronic renal failure - another example is hereditary breast cancer (2 hit theory) |
|
|
What to do with CVS result?
|
- offer amniocentesis
- detailed US - may want to do UPD studies, depending on chr involved (eg chr 15) - careful follow up of preg |

