![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
62 Cards in this Set
- Front
- Back
|
What is Multiple Sclerosis (MS)
|
a disease of the central nervous system in which neurons become demylinated resulting in motor, sensory, and other problems.
|
|
|
General disease characteristics of MS
|
Multiple areas of CNS are affected leading to multiple deficits (many symptoms)
Sclerosis refers to plaque (scar) formation leading to disability Chronic: life-long disease Progressive: usually increases in severity over time |
|
|
What are the different types of MS?
|
Benign
Relapsing-remitting: fluctuating course of exacerbations (attacks) and remissions Secondary progressive Primary progressive |
|
|
What is important for nl nerve transmission?
|
myelin
myelin is lost autoimmune |
|
|
In what age group does MS occur commonly?
|
people in 20s and 30s
|
|
|
MS Picture
|
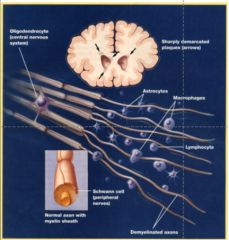
Plaques at many sites – the diagnostic hallmark of multiple sclerosis – are illustrated here in paraventricular regions of the frontal lobe and in the central nervous system. The protective myelin sheath, produced by oliqodendrocytes and schwann cells, is destroyed and plaque forms, in part as a result of abnormal immune system activity. An inflammatory response causes edema and decreased nerve conduction. Astrocytes, lymphocytes, and macrophages may further disrupt demyelinated axons.
|
|
|
What cells make Myelin?
|
Schwann cells and oligodendrocytes
|
|
|
What are the causes of MS?
|
Cause of MS:
Autoimmune disease – there is a cell mediated autoimmune attack against myelin Viral agent Genetic predisposition |
|
|
What are the MOTOR symptoms of MS?
|
Motor (movement) symptoms
Ataxia: trouble moving and loss of coordination, i.e., walking Loss of balance: increased risk of falling Paralysis: inability to move spasticity: muscle cramps or spasms Tremor: shaking of extremities, especially upper limb |
|
|
What nerves are affected with MS:
central or peripheral? |
ONLY CENTRAL
|
|
|
What are Sensory Symptoms of MS?
|
Sensory symptoms
Visual deficits (blurred, reduced, or double vision): usually first symptom to occur Loss of sensation in limbs Parethesias: tingling in extremities Pain Vertigo |
|
|
What is most common symptom of MS?
|
Fatigue or weakness: most common symptoms
|
|
|
What is the Tx of MS?
|
Specific and Nonspecific
Tx Specific target pathogenesis of Dz Nonspecific - attack only symptoms |
|
|
Drug Treatment of MS
Specific treatment of disease process |
Interferons – Two versions of interferon beta-1b (Betaseron & Extavia) and two versions of interferon beta-1a (Avonex & Rebif)
|
|
|
What was the MOA for Interferons?
|
uncertain but beneficial effects may be due to immunomodulatory actions. One thought is that INFs decrease antigen presentation in the CNS, which appears to limit immune attack on myelin
|
|
|
What interferons work in MS?
|
Beta 1b
and Beta 1a EXAM names |
|
|
What is the the major difference between the two interferons are pharmacokinetic (due to slight structural differences).
|
Betaseron (beta-1b) and Rebif (beta-1a) are given by alternate day sc. injections
Avonex (beta-1a) is given by weekly im. injection. |
|
|
how do the interferons have to be given?
|
By injection they are proteins and can be degraded
|
|
|
What are adverse Rxn of Interferons?
|
Adverse reactions:
flu-like symptoms (muscle ache, fever, chills, asthenia) Injection site reactions Antibody formation (can limit effectiveness of drug) Depression |
|
|
What is the Clinical use of Interferons?
|
Used to decrease the frequency and severity of exacerbations in patients with relapsing forms of MS. Uncertain whether they actually slow the progression of the disease
used in chronic forms of MS also |
|
|
Another specific Tx for MS
|
Glatiramer
|
|
|
What is Glatiramer
|
a synthetic compound which resembles a component of myelin
|
|
|
What is the MOA of Glatiramer?
|
Since drug resembles a component of myelin, it’s thought that it may protect myelin by acting as a “decoy” attracting immune cells away from myelin
|
|
|
How must Glatiramer be given?
|
Must be given by sc. Injection, once daily
|
|
|
What are adverse rxns of Glatiramer
|
Generally well tolerated. The most common side effects are:
Injection site reactions Flushing, chest tightness or pain, shortness of breath (within 15 min) Joint pain Muscle stiffness |
|
|
What is the clinical use of Glatiramer
|
Approved for the treatment of relapsing-remitting MS. Has been shown to decrease the rate of relapse
|
|
|
Next specific tx drug for MS
|
Mitoxantrone
|
|
|
What does Mitoxantrone do?
|
a cancer chemotherapeutic agent recently approved to treat advanced MS
Acts by suppressing immune attack on myelin |
|
|
What are side effects of Mitoxantrone
|
Common side effects include nausea, bladder infections, mouth sores, and loss of menstrual cycle.
Patients should only receive the drug for 2-3 years due to a cumulative effect on cardiac conduction***** |
|
|
What is the another specific tx for MS?
|
Natalizumab
|
|
|
What is Natalizumab
|
A recombinant humanized MAB
Binds to a specific site on an adhesion molecule on activated lymphocytes and monocytes. This blocks adhesion and prevents leukocyte entry into CNS, therby decreasing immune attack on myelin. |
|
|
What are adverse effects of Natalizumab?
|
Minor – headache, fatigue etc.
Allergic reactions and antibody formation may limit usefulness Progressive multifocal leukoencephalopathy****EXAM |
|
|
What is the clinical use of Natalizumab?
|
Monotherapy in pts who don’t respond to other drugs. Due to risk of PML, only available in special centers to registered pts.
|
|
|
What is the last Specific MS drug?
|
Fingolimod
|
|
|
What is Fingolimod?
|
The first oral specific therapy for MS
Mechanism – inhibits migration of T cells out of lymph nodes via action on sphingosine-1-phosphatase receptor. Pharmacokinetics – slow but complete absorption; highly bound; halflife 4-9 days. Adverse effects – bradycardia and increased infections Use – prevent relapse and progression |
|
|
What are the specific tx?
|
1. Interferons beta-1b and beta-1a
2. Glatiramer 3. Mitoxantrone 4. Natalizumab 5. Fingolimod |
|
|
Non-specific Drug Treatment:
Symptomatic treatment |
Anti-inflammatory steroids – used for management of acute symptoms because they close damaged blood brain barrier and reduce inflammation in the CNS
|
|
|
What are your anti-inflammatory steroids?
|
methylprednisolone,
dexamthasone, prednisone, betamethasone, prednisolone |
|
|
Symptomatic treatment (cont.)
for MS |
Anti-depressants – both SSRIs (e.g., fluoxetine [Prozac]) and tricyclics (e.g., amitriptyline [Elavil]) are used to treat depression associated with MS.
Amitriptyline (and carbamazepine [Tegretol]) are used to treat neuralgia associated with damaged nerves. Imipramine used to treat urinary incontinence. |
|
|
Symptomatic treatment (cont.)
for MS |
Anti-spasmodics – a variety of drugs are used to relieve spasms, cramping, and muscle tightness caused by spasticity in MS, including benzodiazepines such as clonazepam (Klonopin) and dizaepam (Valium), baclofen (Lioresal; central GABAB agonist), tizanidine (Zanaflex; central α2 agonist) and dantrolene (Dantrium).
|
|
|
Symptomatic treatment (cont.)
for tremors and fatigue |
Amantadine
|
|
|
Symptomatic treatment (cont.)
for vertigo |
Meclizine
|
|
|
Symptomatic treatment (cont.)
for urinary incontinence |
Oxybutanin
|
|
|
Symptomatic treatment (cont.)
for neuralgia |
Carbamazepine and phenytoin
|
|
|
What is Amyotrophic Lateral Sclerosis (ALS)
|
A progressive degenerative disease of motor neurons. Glutamate “excitotoxicity” may be responsible for the disease
|
|
|
Drug treatment of ALS
Riluzole |
is the first (and, so far, only) drug approved for the specific treatment of ALS
|
|
|
What is the MOA of Riluzole?
|
Pharmacology
Riluzole is a voltage-gated sodium channel blocker which is thought to act by inhibiting glutamate release |
|
|
Riluzole
Pharmacokinetics |
Orally effective
Half-life ~ 12 hours Highly bound to plasma proteins Hepatic metabolism (some metabolites active) and renal excretion |
|
|
Riluzole
Adverse reactions |
Asthenia, dizziness, vertigo
Nausea, diarrhea, vomiting Circumoral parethesias SGPT elevation (monitor liver chemistry – may require DC) |
|
|
Riluzole
Therapeutic use |
Has been shown to increase survival in ALS patients but not increase strength or neurological function
|
|
|
Drug treatment of ALS
NON-specific Tx |
consist of baclofen** for spasticity and gabapentin** to slow decline in muscle strength
|
|
|
What is Alzheimer’s Disease
|
A progressive, neurodegenerative disease, occurring later in life. It is the most common type of senile dementia, characterized by cognitive deficits, behavioral disorders, and mood changes
|
|
|
What is the Drug treatment Alzheimer’s Disease
|
Acetylcholinesterase inhibitors
|
|
|
What are the Acetylcholinesterase inhibitors
|
Donepezil
Galantamine Tacrine Rivastigmine |
|
|
Acetylcholinesterase inhibitors
MOA |
the cognitive deficits of the disease are thought to be related, in part, to degeneration of cholinergic neurons in the cortex and hippocampus resulting in deficient cholinergic neurotransmission.
Acetylcholinesterase inhibitors increase cholinergic activity by decreasing metabolism of Ach. Benefit is modest (< 10% improve) and short-lived. |
|
|
Drug treatment Alzheimer’s Disease
Memantine |
MOA – memantine is a “use-dependent” NMDA receptor antagonist. The theory behind its action in Alzheimer’s is that it blocks glutaminergic overstimulation of NMDA receptors, which can be toxic to neurons which are important in learning and memory, but allows low levels of receptor activation.
|
|
|
Memantine
Adverse effects |
Dizziness, headache, constipation, and confusion. Is generally well tolerated.
|
|
|
Memantine
Therapeutic use |
Provides modest benefit by appearing to slow progression of the disease. Can be used with cholinesterase inhibitors to improve their effectiveness. May also be useful in the treatment of neurodegeneration associated with ALS, Parkinson’s disease, and epilepsy.
|
|
|
Drug treatment of Alzheimer’s Disease
SSRI’s and atypical antipsychotics |
useful for depression and agitation.
|
|
|
Drug treatment of Alzheimer’s Disease
Gingko |
shown to modestly improve memory in some Alzheimer’s patients.
|
|
|
Drug treatment of Alzheimer’s Disease
Estrogen |
Estrogen may increase risk
not good! |
|
|
Drug treatment of Alzheimer’s Disease
Caprylidene |
a “medical food” metabolized to ketones to provide energy to brain (may be decreased glucose uptake)
|

