![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
81 Cards in this Set
- Front
- Back
|
What is direct pathway?
|
Striatum stimulates GPi and SNr which disinhibit thalamus --> increased initiation and maintenance of movement
|
|
|
What is indirect pathway?
|
Striatum stimulates GPe and STN which inhibit thalamus --> less movement.
|
|
|
What does substantia nigra pars compacta do?
|
Stimulates direct pathway (D1 receptors) and inhibits indirect pathway (D2 receptors).
|
|
|
Name 3 alpha-synuclein disorders
|
(1) Parkinson's
(2) Diffuse Lewy Body Dementia (3) MSA |
|
|
What is abnormal protein in Parkinson's?
|
Alpha-synuclein
|
|
|
What is abnormal protein in Diffuse Lewy Body Dementia?
|
Alpha-synuclein
|
|
|
What is direct pathway?
|
Striatum stimulates GPi and SNr which disinhibit thalamus --> increased initiation and maintenance of movement
|
|
|
What is abnormal protein in multiple system atrophy?
|
Alpha-synuclein
|
|
|
What is indirect pathway?
|
Striatum stimulates GPe and STN which inhibit thalamus --> less movement.
|
|
|
Name 3 poly-glutamine (CAG repeat) disorders
|
(1) Huntingdon's
(2) DRPLA (3) SCA |
|
|
What does substantia nigra pars compacta do?
|
Stimulates direct pathway (D1 receptors) and inhibits indirect pathway (D2 receptors).
|
|
|
What is genetic anomaly in Huntingdon's?
|
CAG repeat on 4p16.3. < 28 reps normal, > 40 reps disease. Huntingtin is abnormal protein.
|
|
|
Name 3 alpha-synuclein disorders
|
(1) Parkinson's
(2) Diffuse Lewy Body Dementia (3) MSA |
|
|
What is abnormal protein in corticobasal degeneration?
|
4 repeat tau
|
|
|
What is abnormal protein in Parkinson's?
|
Alpha-synuclein
|
|
|
What is abnormal protein in Diffuse Lewy Body Dementia?
|
Alpha-synuclein
|
|
|
What is abnormal protein in multiple system atrophy?
|
Alpha-synuclein
|
|
|
Name 3 poly-glutamine (CAG repeat) disorders
|
(1) Huntingdon's
(2) DRPLA (3) SCA |
|
|
What is genetic anomaly in Huntingdon's?
|
CAG repeat on 4p16.3. < 28 reps normal, > 40 reps disease. Huntingtin is abnormal protein.
|
|
|
What is abnormal protein in corticobasal degeneration?
|
4 repeat tau
|
|
|
What is toxic protein in Progressive Supranuclear Palsy?
|
4 repeat tau
|
|
|
What is toxic protein in frontotemporal dementia w/ parkinsonism?
|
4 repeat tau
|
|
|
3 classes of drugs that can cause parkinsonism.
|
(1) Anti-psychotics (eg Haldol)
(2) Anti-emetics (Metoclopramide) (3) Dopamine depleters (eg Tetrabenazine) |
|
|
3 toxins that can cause parkinsonism
|
(1) Acute CO poisoning
(2) Acute MPTP (3) Manganese |
|
|
What is toxic protein in Progressive Supranuclear Palsy?
|
4 repeat tau
|
|
|
2 viral illnesses that can present w/ parkinsonism
|
(1) West Nile
(2) Japanese encephalitis |
|
|
What is toxic protein in frontotemporal dementia w/ parkinsonism?
|
4 repeat tau
|
|
|
Presentation of manganese toxicity.
|
Symmetric parkinsonism not responsive to dopa. Often have dystonic features and oculogyric crisis.
|
|
|
3 classes of drugs that can cause parkinsonism.
|
(1) Anti-psychotics (eg Haldol)
(2) Anti-emetics (Metoclopramide) (3) Dopamine depleters (eg Tetrabenazine) |
|
|
Epidemiology of essential tremor
|
6 in 100 000. Multimodal age onset -- adolescence, early adulthood, > 60s
|
|
|
3 toxins that can cause parkinsonism
|
(1) Acute CO poisoning
(2) Acute MPTP (3) Manganese |
|
|
Clinical features of essential tremor
|
5-12 Hz freq. Absent at rest, elicited w/ movement or postures. Mostly upper limbs, can affect writing. Voice or head can be affected.
|
|
|
2 viral illnesses that can present w/ parkinsonism
|
(1) West Nile
(2) Japanese encephalitis |
|
|
What is frequency of essential tremor?
|
5-12 Hz
|
|
|
Presentation of manganese toxicity.
|
Symmetric parkinsonism not responsive to dopa. Often have dystonic features and oculogyric crisis.
|
|
|
Treatment options for essential tremor (3)
|
(1) Alcohol (2/3 respond)
(2) Beta-blockers (propanolol) (3) Anti-convulsants (primidone, topiramate, gabapentin) |
|
|
Epidemiology of essential tremor
|
6 in 100 000. Multimodal age onset -- adolescence, early adulthood, > 60s
|
|
|
Clinical features of essential tremor
|
5-12 Hz freq. Absent at rest, elicited w/ movement or postures. Mostly upper limbs, can affect writing. Voice or head can be affected.
|
|
|
What is frequency of essential tremor?
|
5-12 Hz
|
|
|
Treatment options for essential tremor (3)
|
(1) Alcohol (2/3 respond)
(2) Beta-blockers (propanolol) (3) Anti-convulsants (primidone, topiramate, gabapentin) |
|
|
3 syndromes that can have acanthocytes
|
(1) Neuroacanthocytosis
(2) Abetalipoproteinemia (3) McLeod syndrome |
|
|
Presentation of neuroacanthocytosis
|
- Onset 8-62 yrs
- Stereotyped orofacial dyskinesias, chorea, parkinsonism, seizures (50%) - Often autosomal recessive inheritance |
|
|
Genetic abnormality in McLeod syndrome
|
X-linked recessive mutation in XK gene (Kell antigen)
|
|
|
Onset of McLeod syndrome
|
Age 50
|
|
|
What is an acanthocyte?
|
Contracted erythrocyte with thorny projections
|
|
|
3 syndromes that can have acanthocytes
|
(1) Neuroacanthocytosis
(2) Abetalipoproteinemia (3) McLeod syndrome |
|
|
Presentation of McLeod syndrome
|
- CK increased
- Axonal peripheral neuropathy - Limb chorea |
|
|
Presentation of neuroacanthocytosis
|
- Onset 8-62 yrs
- Stereotyped orofacial dyskinesias, chorea, parkinsonism, seizures (50%) - Often autosomal recessive inheritance |
|
|
What is genetic anomaly in PKAN?
|
Mutation in PANK2 gene on chr 20.
|
|
|
Genetic abnormality in McLeod syndrome
|
X-linked recessive mutation in XK gene (Kell antigen)
|
|
|
What is characteristic neuroimaging finding in PKAN?
|
"Eye of the tiger" sign -- hypointensity in globus pallidus w/ surrounding hyperintensity on T2.
|
|
|
Onset of McLeod syndrome
|
Age 50
|
|
|
Pathophysiology of PKAN
|
Neurodegeneration w/ brain iron accumulation. Pantothenate kinase is a regulatory enzyme involved in coenzyme A synthesis.
|
|
|
What is an acanthocyte?
|
Contracted erythrocyte with thorny projections
|
|
|
4 subtypes of neurodegeneration w/ brain iron accumulation
|
"PAIN"
PKAN Aceruloplasminemia Infantile neuroaxonal dystrophy Neuroferritinopathy |
|
|
Presentation of McLeod syndrome
|
- CK increased
- Axonal peripheral neuropathy - Limb chorea |
|
|
What is genetic anomaly in PKAN?
|
Mutation in PANK2 gene on chr 20.
|
|
|
What is characteristic neuroimaging finding in PKAN?
|
"Eye of the tiger" sign -- hypointensity in globus pallidus w/ surrounding hyperintensity on T2.
|
|
|
Pathophysiology of PKAN
|
Neurodegeneration w/ brain iron accumulation. Pantothenate kinase is a regulatory enzyme involved in coenzyme A synthesis.
|
|
|
4 subtypes of neurodegeneration w/ brain iron accumulation
|
"PAIN"
PKAN Aceruloplasminemia Infantile neuroaxonal dystrophy Neuroferritinopathy |
|
|
Clinical presentation of PKAN
|
Childhood onset w/ insidious onset of gait disorder and dystonia. Rigidity, dysarthria, spasticity, dementia, retinitis pigmentosa, optic atrophy may all be present
|
|
|
Clinical presentation of PKAN
|
Childhood onset w/ insidious onset of gait disorder and dystonia. Rigidity, dysarthria, spasticity, dementia, retinitis pigmentosa, optic atrophy may all be present
|
|
|
Genetic anomaly in Wilson's disease
|
13q14.3 mutation in ATP7B gene. Autosomal recessive.
|
|
|
Genetic anomaly in Wilson's disease
|
13q14.3 mutation in ATP7B gene. Autosomal recessive.
|
|
|
Epidemiology of Tourette's
|
- Age of onset 5-15 yrs (peak 7)
- 3-4x higher in males |
|
|
Epidemiology of Tourette's
|
- Age of onset 5-15 yrs (peak 7)
- 3-4x higher in males |
|
|
Diagnostic Criteria For Tourette's (5)
|
(1) Onset before 18 yrs
(2) Both motor and vocal tics present at some point (3) Variation in pattern of tics (4) Tics at least daily (5) Tics present for > 1 yr |
|
|
Diagnostic Criteria For Tourette's (5)
|
(1) Onset before 18 yrs
(2) Both motor and vocal tics present at some point (3) Variation in pattern of tics (4) Tics at least daily (5) Tics present for > 1 yr |
|
|
Mechanism of action of clonidine
|
Alpha-2 adrenergic agonist (increases NE release)
|
|
|
Mechanism of action of clonidine
|
Alpha-2 adrenergic agonist (increases NE release)
|
|
|
Work up for Sydenham's chorea
|
ASOT, ECG, echo, cardiology consult
|
|
|
Work up for Sydenham's chorea
|
ASOT, ECG, echo, cardiology consult
|
|
|
Jones criteria for rheumatic fever
|
(1) Joints - Polyarthritis
(2) Heart - Carditis (3) Nodules (4) Erythroderma nodosum (5) Sydenham's chorea * 2 major or 1 major and 2 minor * Minor: Fever, arthralgia (if no arthritis), ESR/CRP increased, leukocytosis, heart block on ECG, previous rheumatic fever or inactive heart dx |
|
|
Jones criteria for rheumatic fever
|
(1) Joints - Polyarthritis
(2) Heart - Carditis (3) Nodules (4) Erythroderma nodosum (5) Sydenham's chorea * 2 major or 1 major and 2 minor * Minor: Fever, arthralgia (if no arthritis), ESR/CRP increased, leukocytosis, heart block on ECG, previous rheumatic fever or inactive heart dx |
|
|
Treatment for Sydenham's chorea
|
(1) Valproic acid
(2) Clonidine ** Need longterm Pen G prophylaxis |
|
|
Treatment for Sydenham's chorea
|
(1) Valproic acid
(2) Clonidine ** Need longterm Pen G prophylaxis |
|
|
How long after strep pharyngitis do symptoms of rheumatic fever present?
|
3 weeks
|
|
|
How long after strep pharyngitis do symptoms of rheumatic fever present?
|
3 weeks
|
|
|
Mechanism of action for Artane (Trihexiphenidyl)
|
Anti-cholinergic (anti-muscarinic)
|
|
|
Mechanism of action for Artane (Trihexiphenidyl)
|
Anti-cholinergic (anti-muscarinic)
|
|
|
Sketch the basal ganglia pathways.
|
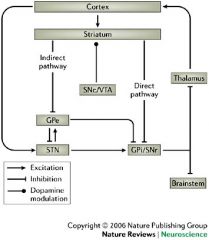
|

