![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
172 Cards in this Set
- Front
- Back
|
1. What kind of onset does appendicitis have?
2. Where is the pain referred with appendicitis? 3. Where does the pain localize in appendicitis? |
1. Abrupt Onset
2. Pain is referred to epigastric or periumbilical area 3. Right lower quadrant |
|
|
What is the classic presentation of appendicitis?
|
right lower quadrant abdominal pain, anorexia, nausea, and vomiting
|
|
|
What might be seen on rectal exam with appendicitis?
|
Right sided rectal tenderness
|
|
|
What are the four physical exam signs associated with appendicitis?
|
1. McBurney’s point
2. Rovsing’s sign 3. Psoas sign (more common with retrocecal appendix) 4. Obturator sign (more common with pelvic appendix) |
|
|
What is the TX for appendicitis?
|
open or laparoscopic appendectomy
|
|
|
What is diverticulosis?
|
Presence of multiple divertucula (outpouchings) in the colon - mucosal layer of the colon herniates through the muscularis layer
|
|
|
Diverticulitis is mostly where?
|
In the sigmoid colon
|
|
|
What are the two main things associated with the etiology of diverticulitis?
|
1. Increased intraluminal pressure causes diverticula
2. Thought to be related to low fiber diet |
|
|
What is the gold standard for diagnosis diverticulitis?
|
Colonoscopy
|
|
|
This is Inflammation and gross or microscopic perforation of the diverticulum.
|
Diverticulitis
|
|
|
What is a major symptom of diverticulitis?
|
Left lower quadrant pain
|
|
|
How can diverticulitis present?
|
Perforation can present as generalized abdominal pain with peritoneal signs, high fever, and leukocytosis
|
|
|
How do you diagnose diverticulitis?
|
Diagnosis:
KUB and upright: Free air Ileus Bowel obstruction CT scan |
|
|
How do you TX mild diverticulitis?
|
Antibiotics: broad spectrum with anaerobic coverage for 7-10 days
Cipro and metronidazole Treat as outpatient if no peritoneal signs and no co-morbidities Symptoms should markedly improve within 3 days; if not re-evaluate diagnosis |
|
|
How do you TX severe diverticulitis?
|
Hospitalization
NPO & IVF Broad spectrum IV antibiotics with anaerobic and gram-negative coverage |
|
|
This is a Life-threatening vascular emergency
Incidence: 1/1000 hospital admissions Cause of 1% of ED visits for acute abdomen High mortality rate (50-90%), varying with cause and extent of ischemic bowel Higher mortality rate than colon cancer Occurs most frequently in elderly patients, known cardiac disease, known atherosclerotic disease |
Ischemic Bowel Disease
|
|
|
90% patients over 60 years
Patients do not appear severely ill Mild abdominal pain, tenderness present Rectal bleeding, bloody diarrhea common Colonoscopy is procedure of choice |
Colonic Ischemia
|
|
|
Age varies with etiology of ischemia
Patients appear ill Pain is severe, tenderness not prominent Bleeding uncommon Angiography indicated |
Mesenteric Ischemia
|
|
|
Most common vascular disorder of intestines
Most common cause of colitis after 50 years Usually self-limiting condition Transient reduction in blood flow to the colon |
Ischemic Colitis
|
|
|
What are the two major causes of Ischemic colitis?
|
Arterial occlusion (60-70%)
Hypoperfusion syndromes (20-30%) |
|
|
What is a major sign of ischemic colitis?
|
Left lower quadrant pain followed by rectal bleeding
|
|
|
How do you diagnose ischemic colitis?
|
Diagnosis is made by colonoscopy
Angiography or magnetic resonance angiography not indicated |
|
|
What is the TX for ischemic colitis?
|
Treatment is supportive with IV fluids, bowel rest, and antibiotics
|
|
|
Reduction in intestinal blood flow
Commonly arises from occlusion, vasospasm, and/or hypoperfusion of the mesenteric vasculature Abdominal pain is out of proportion to physical findings Can be acute and chronic based on rapidity and degree to which blood flow is compromised |
Mesenteric Ischemia
|
|
|
Sudden onset of intestinal hypoperfusion
Occlusive or non-occlusive obstruction of arterial or venous blood flow Most common arterial is emboli or thrombosis of mesenteric arteries Most common venous is thrombosis or segmental strangulation |
Acute Mesenteric Ischemia
|
|
|
This has Episodic or constant intestinal hypoperfusion
Mesenteric atherosclerotic disease |
Chronic Mesenteric Ischemia
|
|
|
What are the four causes of mesenteric ischemia?
|
Aterial embolus >50%
Nonocclusive ischemia 25% Venous thrombosis 5-15% Arterial thrombosis 10% |
|
|
What are the physical findings with mesenteric ischemia?
|
Rapid onset of severe periumbilical abdominal pain
Minimal physical findings: abdomen remains soft, with little or no tenderness on palpation nausea, vomiting, and mild tachycardia may be present |
|
|
As necrosis develops/progresses in mesenteric ischemia what can be seen?
|
signs of peritonitis appear, no bowel sounds, stool may be heme-positive
signs of shock, frequently followed by death |
|
|
A sudden onset of pain with mesenteric ischemia suggests?
|
arterial embolism
|
|
|
A more gradual onset of pain with mesenteric ischemia suggests?
|
venous thrombosis
|
|
|
Mesenteric Ischemia: Patients with a history of postprandial abdominal discomfort (which suggests intestinal angina) may have?
|
Arterial Thrombosis
|
|
|
How do you diagnose mesenteric ischemia?
|
Mesenteric angiography (gold standard) if diagnosis unclear
Early diagnosis important because mortality increases significantly with intestinal infarction Laboratory studies are nonspecific Marked leukocytosis with immature WBCs, elevated HCT consistent with hemoconcentration, metabolic acidosis, LDH Abdominal plain films CT scan |
|
|
What is the initial management of mesenteric ischemia?
|
aggressive hemodynamic monitoring and support
correction of metabolic acidosis broad spectrum antibiotics nasogastric tube for gastric decompression |
|
|
What TX must be given long term for patients with mesenteric ischemia?
|
Long-term anticoagulation or antiplatelet therapy
|
|
|
In mesenteric ischemia mortality approaches 70-90% if ?
|
Intestinal infarction occurs
|
|
|
Functional disorder
Chronic or recurrent GI symptoms not explained by structural or biochemical abnormalities Idiopathic |
Irritable Bowel Disease (IBS)
|
|
|
What are three main things with IBS presentation?
|
Intermittent, crampy lower abdominal pain
Onset associated with change in form/appearance of stool and frequency Abdominal pain relieved by defecation |
|
|
How do you diagnose IBS?
|
Diagnosis established once organic disease is excluded
AVOID over testing CBC, ESR, TFTs, albumin, guaiac stool If diarrhea Stool O&P, stool cultures Anti-gliadin, IgA endomysial antibodies to rule out celiac |
|
|
How do you TX severe IBS?
|
Medications reserved for severe refractory symptoms
Antispasmodics (anticholinergics) Dicyclomine (Bentyl) Hyoscaymine (Levsin) Watch for side effects: urinary retention, constipation, tachycardia, dry mouth Antidiarrheals Loperamide (Lomotil) Anticonstipation Fiber Osmotic laxatives (milk of magnesia) Lactulose Sorbitol Psychotropic medications TCAs Serotonin receptor agonists and antagonists Tegaserod (Zelnorm) Alosetron (Lotronex) |
|
|
What two disease make up inflammatory bowel disease?
|
Ulcerative colitis
Crohn’s dz |
|
|
How does the underlying pathology of Ulcerative colitis and Crohn's differentiate themselves from each other?
|
UC effects mucosa and submucosa of the colon
Crohn’s affects all 4 layers of the colon and/or small bowel |
|
|
More common in Jewish population and in industrialized countries
Genetic predisposition Age 10 - 40 M = F More common in nonsmokers or former smokers (severity lower in active smokers) |
Ulcerative Colitis
|
|
|
This is the pathophysiology of what?
Inner lining of colon dies and sloughs off Only mucosa and submucosa are affected Rare ileum involvement |
Ulcerative Colitis
|
|
|
What are the symptoms of ulcerative colitis?
|
Bloody and/or mucous containing diarrhea (mild dz: < 4 BMs/day, severe dz > 6 BMs/day)
Abdominal pain (usually LLQ, but may be generalized) Fever Fatigue Weight loss Anorexia Tenesmus and rectal bleeding in 25% Acute onset, fulminant within 24-48h < 10% develop pancolitis |
|
|
What are four common systemic symptoms seen with ulcerative colitis?
|
Cirrhosis
Pericholangitis Pyoderma gangrenosum 20% of patients develop arthritis |
|
|
These are all signs of what?
Appear quite ill Pale appearance Tachycardia, hypotension Fevers (> 103ºF) Abd: distension, slow /absent bowel sounds, firm, tender to light & deep palpation in LLQ w/ or without rebound Rectal tenderness Guaiac positive |
Ulcerative colitis
|
|
|
When you perform a barium enema in ulcerative colitis, what are three things that would be most likely seen?
|
“Cobble stone” appearance 2/2 ragged mucosal ulcerations and luminal narrowing
Loss of haustral markings Thumb printing |
|
|
How do you treat distal colitis?
1. Proctitis? 2. Proctosigmoiditis? |
1. Proctitis
Mesalamine supp 100mg pr qd or Hydrocortisone supp 100 mg pr qd 2. Proctosigmoiditis Mesalamine enema 4 g pr qd or Hydrocortisone enema 100mg pr qd |
|
|
How do you treat mild to moderate ulcerative colitis?
|
Sulfasalazine 1-1.5 g po bid or
Mesalamine 2-4.8 g po qd or Balsalazide 2.25g po tid (add mesalamine enema qd or prednisone 40-60mg qd if no improvement after 2-4 weeks) |
|
|
How do you treat severe ulcerative colitis?
|
(10-15% of pts, need hospitalization)
Methylprednisolone 48-60 mg IV qd |
|
|
These are used in ulcerative colitis if medical Tx fails and to avoid surgery
Risk of chronic immunosuppression Azathioprine (Infliximab), is a drug in this class, used In mod to severe dz Clinical response in 65%, clinical remission in 33% |
Immunomodulating agents
|
|
|
The following are reasons for what?
Persistent bleeding Perforation Cancer risk or cancer Dx Toxic megacolon (< 2% of pts) Debilitating refractory illness |
The use of surgical intervention in ulcerative colitis
|
|
|
What is something that should be done every 1-2 years in patients with ulcerative colitis?
|
Colonoscopy because 30% of patients develop cancer.
|
|
|
Seen in all countries
Presents at any age Peaks at age 10-40 and again at age 60-80 Can affect any GI mucosa (Mouth to anus) |
Crohn's Disease
|
|
|
Effects all 4 layers of intestinal mucosa (transmural) w/ ulcerations and distinct noncaseating granulomas filling the crypts
Causes bowel wall thickening, inflexibility and stenosis Since transmural, fistulas and perirectal fissures are common Can invade bladder or ureters “Skip” lesions |
Crohn's Disease
|
|
|
What are three types of symptoms seen with Crohn's disease?
|
Insidious onset
Vague c/o of fatigue, malaise, wt loss, low-grade fever Crampy RLQ pain w/ watery diarrhea, relieved by defecation |
|
|
What are four common systemic signs seen with Crohn's disease?
|
Erythema nodosum
Aphthous ulcers Renal stones Gallstones |
|
|
The following are all signs for what?
Thin, undernourished pt w/ low-grade fever Tender RLQ mass (misDx’ed for appendicitis) Perianal scarring, skin tags, fissures and abscesses + Systemic signs such as Erythema nodosum, nail clubbing or joint inflammation |
Crohn's Disease
|
|
|
What are four diagnostic studies for Crohn's disease?
|
Since the lesions can be anywhere you need -
barium swallow, upper GI series, small bowel follow through and barium enema to evaluate entire GI tract |
|
|
What is specific drug TX for Crohn's disease?
|
5-Aminosalcylic acid agents (mesalamine: asacol or pentasa) – beneficial in colonic dz, unclear if beneficial in small bowel dz or in preventing recurrence.
Abx (cipro or flagyl) – little or no effect per meta-analysis Corticosteroids – suppress acute clinical Sx Budosemide effective in mild - mod ileal dz – less side effects than other systemic corticosteroids Prednisone or methylprednisolone in severe Crohn’s; 20% of pts cannot be tapered off of steroids; 75% of pt with initial improvement on steroids experience relapse within 1 yr Ca and Vitamin D supplements Immunomodulating drugs: (Azathioprine, mercaptprine or methotrexate) Permits elimination of steroids in 75% of pts and Fistula closure in 30% of pt Remission and maintenance of remission is 3 x more likely Immunomodulating drugs: Anti-TNF therapies (Infliximab) Used in severe dz or fistula-forming dz |
|
|
What is something that must be done in the long term TX of patient's with Crohn's Disease?
|
Colonoscopy q 1-2 yrs, starting 8 yrs after Dx
due to high rate of cancer development. |
|
|
These complications are usually associated with what?
Colon cancer, Toxic megacolon, Hemorrhage |
Ulcerative colitis
|
|
|
These complications are usually associated with what?
Perforation, Fistulas and Fissures, Growth retardation, Malabsorption syndrome |
Crohn's Disease
|
|
|
Usually sporadic mass lesions that protrude into the intestinal lumen
|
Colon polyps
|
|
|
What are the three major pathology groups associated with colon polyps?
|
Mucosal neoplastic (adenomatous) polyps - 70%
Mucosal non-neoplastic polyps Submucosal lesion |
|
|
95 % of cases of adenoCA arise from ?
|
Adenomas
|
|
|
>1cm in size, contain villous features or high-grade dysplasia
|
Advanced adenoma
|
|
|
What are the specific rules for postpolypectomy surveillance in patients with 1-2 adenomas, 3-10 adenomas, >10 adenomas?
|
Repeat colonoscopy in 5-10 yrs if 1-2 small tubular adenomas found
Repeat colonoscopy in 3 yrs if 3-10 adenomas found, with 1 adenoma > 1cm, or villous features or high-grade dysplasia Repeat colonoscopy in 1-2 yrs if > 10 adenomas found (consider familial polyposis syndrome) |
|
|
approximately 50% of colon cancer is found?
|
Distal to the splenic flexure
|
|
|
What are the signs and symptoms of colon cancer?
|
AdenoCA grows slowly
Sx depend on location Fe deficiency anemia w/ fatigue and weakness Change in bowel habits and crampy abdominal pain 2/2 obstruction (most likely if CA in the descending colon) Tenesmus Urgency Recurrent hematochezia Hepatomegaly in metastatic spread |
|
|
What is involved with screening for colon cancer in patients over 50?
|
Annual fecal occult blood testing
Barium enema or Flex Sig every 5 yrs Colonoscopy every 10 yrs |
|
|
What are the two different rules for patients who have family members that had colon cancer?
|
1. If fam member > 60yrs at Dx: start at age 40 w/ colonoscopy every 10 yrs
2. If fam member < 60 yrs at Dx, or more than 1 first degree fam member: start at age 40, or 10 yrs younger than dx of youngest affected fam member w/ colonoscopy every 5 yrs |
|
|
In rectal cancer - low anterior resection w/colorectal anestomosis (sphincter preservation) - the minimal requirement is what?
|
2cm of healthy tissue
|
|
|
In stage II and III of colorectal cancer, what is an adjuvent therapy given?
|
Fluorouracil (XRT sensatizing agent) + XRT
|
|
|
60 % of mechanical small bowel obstructions
post appendectomy, colorectal surgery, and gynecologic and upper GI procedures Acute within 4 weeks of surgery or decades later in chronic obstruction |
Post surgical adhesions - scarring after surgery
|
|
|
a mechanical SBO - surgical emergency (vascular compromise leads to bowel ischemia & further morbidity & mortality)
|
Strangulated SBO
|
|
|
The following are signs of what?
Crampy intermittent abd pain Pain may become constant & severe w/ development of strangulation Nausea Vomiting (in proximal obstruction) Diarrhea (early in dz process) Absence of flatus or BM Fever & tachycardia (late in dz process) |
Mechanical SBO
|
|
|
The following are physical signs of what?
Abdominal distention Hyperactive bowel sounds hypoactive bowel sounds (later) Fever, tachycardia, rebound tenderness and guarding R/o strangulated hernia Rectal exam, if guaiac + = Cancer or late strangulation |
Mechanical SBO
|
|
|
What imaging is ordered with a mechanical SBO?
|
Plain x-ray/ KUB: flat and upright
Air-fluid levels Loop width > 2.5 cm Can’t different strangulation from simple obstruction Enteroclysis Good for differentiating partial from complete obstruction Contraindicated in perforation |
|
|
~ 90% sensitive & specific in detecting SBO
capable of revealing abscess, inflammatory process, extraluminal pathology resulting in obstruction, & mesenteric ischemia distinguish between ileus & mechanical small bowel in post-op pts No oral contrast required for Dx of SBO because the retained intraluminal fluid serves as a natural contrast agent small-bowel loop > 2.5 cm in diameter dilated proximal to a distinct transition zone of collapsed bowel < 1 cm in diameter |
Abdominal CT
|
|
|
What are the six things used to treat mechanical SBO?
|
1. NG-tube w/ suction for bowel decompression
2. IVF 3. Analgesics and antiemetics 4. Abx to cover gram-negative & anaerobic organisms-cefazolin, cefoxetin, cefotetan, cefuroxime – Levo&Flagyl 5. Early surgical consultation 6. Observation (up to 3 days) |
|
|
Usually temporary condition in which there is neurogenic failure or loss of peristalsis in the intestine in the absence of mechanical obstruction
|
Acute paralytic ileus
|
|
|
Usually temporary condition in which there is neurogenic failure or loss of peristalsis in the intestine in the absence of mechanical obstruction
|
Acute paralytic ileus
|
|
|
What are the signs and symptoms of an acute paralytic ileus?
|
Mild diffuse, continuous abd discomfort
Nausea and vomiting Abd distention ↓ or absent bowel sounds No BM and/or flatulence |
|
|
What labs do you run in diagnosing acute paralytic ileus?
|
check for electrolyte abnormalities : ↓K, ↑Ca, ↓Mg, ↓Phos
|
|
|
How do you treat acute paralytic ileus?
|
Treat underlying medical or surgical condition
Bowel rest w/ NPO, gradual advancement of diet NG tube w/ suction and IVF Alvimopan (minimizes many of the undesirable side-effects of opioids such as constipation without affecting analgesia or precipitating withdrawal) |
|
|
Bacillus
anaerobic gram-positive spore-forming opportunistic pathogen incidence & severity of infection have increased alarmingly since 2000 ! |
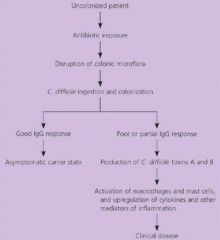
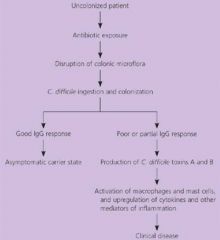
Clostridium difficile
|
|
|
|
|
|
The NAP-1 strain of clostridium difficile is highly resistant to?
|
Fluoroquinolones
|
|
|
What are the ABX most commonly associated with C. Diff?
|
Clindamycin
Penicillin derivatives (esp. amoxicillin-clavulanate) Cephalosporins (esp. 3rd generation) |
|
|
What is the presentation of C. diff?
|
Diarrhea during or after Abx use
May be bloody None during late dz Abdominal discomfort Fever Leukocytosis suddenly, doubled 30-50K |
|
|
How do you treat C. diff?
|
Depends on clinical presentation
D/c Abx if possible, diarrhea resolves in ~20% of pts If pt has risk factors or Abx cannot be d/c’ed Metronidazole 500mg PO TID or QID x 10-14 days (> 90% response rate) OR in severe dz Vancomycin 125-500mg PO QID x 10-14 days (also > 90% response rate, but $$$) |
|
|
How do you treat a recurrence of C. diff?
|
Tx: Repeat course of Metronidazole or Vanco
|
|
|
How do you treat multiple recurrence of C. diff?
|
Tapering and pulse-dosing regimen of Vancomycin - regimen not proven, can use e.g. :
125mg PO Q 6h x 14 days Then 125mg PO q12h x 7 days Then 125mg PO qd x 7 days Then 125 mg PO QOD x 4 doses Then 125mg PO every 3 days x 5 doses No prolonged metronidazole 2/2 adverse effects including peripheral neuropathy! |
|
|
These are CONTRAINDICATED in C. diff TX because they ↓ intestinal motility which exacerbates toxin-mediated dz!
|
Opiates and Antidiarrheal
|
|
|
What complication, and what tx for it, is involved with C. diff?
|
Severe Cdiff diarrhea in 3% of pts
30-85% mortality rate in these pts Tx: Metronidazole IV + Vancomycin po (via NG Tube if necessary) |
|
|
Acute dilation of the colon, seen in ulcerative colitis and Clostridium difficile colitis, that may result in perforation of the colon, septicemia, and death.
|
Toxic megacolon
|
|
|
The outlet for the GI tract
Lined with squamous epithelium Contains sensory nerve endings |
Anus
|
|
|
Lower 10-15cm of the large intestine
Lined by mucosal & columnar epithelium Contains stretch nerve fibers but not pain |
Rectum
|
|
|
Separates the anus and rectum
Delineates sensory and pain nerve fibers |
Dentate line
|
|
|
An area at the Dentate Line that the anal glands drain into
Common site for anal abscesses and fistulas |
Anal Crypts (Crypts of Morgagni)
|
|
|
Lower muscle edge of the rectum
Controlled by the Autonomic Nervous System |
Internal Sphincter
|
|
|
Controlled by the Spinal Nerve
Under voluntary control |
External Sphincter
|
|
|
Blood vessels around the anus
Hemorrhoids are made up of this. |
Venous Plexus
|
|
|
Acute onset with a palpable mass after straining
Acute pain usually lasts up to 72 hours and then subsides |
External Hemorrhoids
|
|
|
Aching after a bowel movement
|
Internal Hemorrhoids
|
|
|
Tearing-like pain during a bowel movement
Pain may persist until tear heals |
Anal Fissures
|
|
|
Pain of gradual onset, localized, constant but increased with bowel movements
|
Anal Abscesses
|
|
|
Usually cause pain after invasion of the sphincter muscle
|
Anal Cancer
|
|
|
When evaluating anal problems what are the six things associated with the physical exam?
|
Abdominal Examination
Visual Inspection of the Anal & Perineal Areas Digital Anal/Rectal Palpation Prostate Exam Anoscope Visualization Sigmoidoscopy and Colonoscopy in selected individuals |
|
|
An acute longitudinal tear or a chronic ovoid ulcer in the anoderm (squamous epithelium)
Most commonly located anterior and posterior to the anus (12 and 6 o’clock) When found laterally considered other diagnoses: Inflammatory Bowel Disease, Syphilis, Abscesses, Herpes Usually associated with constipation, straining or explosive diarrhea Acute pain or stinging occurring with or shortly after a bowel movement May be associated with bright red blood |
Anal fissure
|
|
|
What type of surgery is done for persistent anal fissures?
|
Lateral Internal Sphincterotomy is most commonly performed
A cut is made into the internal anal sphincter to alleviate spasm Main concern with surgery is anal incontinence |
|
|
Localized collections of pus
Usually due to infections in the anal crypts which tracks through the planes in the anorectal region Most common organisms: E. coli, Proteus, Bacteroides, streptococci & staphylococci |
Anal Abscesses
|
|
|
Located at the anal verge, superficial and points to the skin
|
Perianal Abscesses:
|
|
|
Tracks across the sphincter and is located under the Levator muscle, visible on the buttock but deeper
|
Ischiorectal Abscess:
|
|
|
Between the inner circular and outer longitudinal muscle layers; typically associated with an anal bulge palpated within the rectum
|
Intersphincteric Abscess:
|
|
|
Above the Levator muscle; may extend into the peritoneum or abdominal organs
|
Supralevator Abscess:
|
|
|
The following are clinical manifestations of what?
Perianal Swelling, Pain, Erythema, Tenderness Swelling, Pain & Tenderness on Digital Exam Painful Defecation Fever, Chills, Malaise Lower Abdominal Pain |
Anal Abscesses
|
|
|
How do you TX anal abscess?
|
Incision and Drainage for Superficial Abscesses
Deeper abscesses may require drainage under anesthesia in OR IV antibiotics for patients with systemic manifestations, neutropenia or diabetes Ciprofloxacin (Cipro) and Metronidazole (Flagyl) Ampicillin/Sulbactam (Unasyn) Sitz baths, Stool Softeners, Bulking Agents as needed |
|
|
Tubelike tract with one opening in the anal canal and the other opening in the perianal skin
The most common cause of this is a cryptoglandular infection Usually a history of recurrent abscesses followed by intermittent or constant discharge May occur spontaneously Crohn’s Disease, TB |
Anal Fistulas
|
|
|
How do you TX anal fistulas?
|
Treatment is predominately surgical
Pain management after surgery may be required Sitz baths, stool softeners and/or bulking agents may be recommended Recurrence is rare after surgical extraction of the tract Sigmoidoscopy may be performed to rule out Crohn’s Disease |
|
|
This is a chronic infection of the skin in the gluteal cleft
Most common between the ages of 15-30; it occurs after the onset of puberty Males are more commonly affected than females Whites are more commonly affected than African Americans or Asians Other risk factors include increased sweating, poor hygiene, obesity and local trauma |
Pilonidal Infections - AKA Sacrococcygeal Pilonidal Sinus
|
|
|
Dilated veins of the hemorrhoidal plexus
Majority develop after the age of 30 Increase pressure of supporting tissue stretches, the vessels dilate, vessel walls become thin and bleed, with continued pressure the vessels protrude Risk Factors Aging, Chronic Constipation or Diarrhea, Pregnancy, Hereditary, Laxative or Enema Abuse |
Hemorrhoids
|
|
|
Originate above the Dentate Line
Graded on a I-IV Scale Grade I: Bulge with Defecation Grade II: Prolapse occurs with Defecation but recedes spontaneously Grade III: Require digital manipulation after prolapsing Grade IV: Can not be replaced after prolapse |
Internal Hemorrhoids
|
|
|
Originate below the Dentate Line
Usually present as a bulge with defecation |
External Hemorrhoids
|
|
|
What is the symptomatic TX for mild hemorrhoids?
|
Stool Softeners, Increase Fiber & Fluids
Sitz Bath Anesthetic Ointments and/or Suppository NSAIDs for pain |
|
|
What are four medical/surgical TX options for hemorrhoids?
|
Injection Sclerotherapy
Option for bleeding hemorrhoids Rubber Band Ligation Option for large, prolapsed internal hemorrhoids Infrared Photocoagulation Used for small internal hemorrhoids Surgical Hemorrhoidectomy Surgical excision under anesthesia Most complete method of removal for both internal and external hemorrhoids |
|
|
This is required to distinguish hyperplastic polyps from precancerous lesions
|
Biopsy
|
|
|
Adenomatous polyps (tubular, tubulovillous, and villous) are precursors to ?
|
Cancer
|
|
|
What is the most common type of anal cancer?
|
Squamous cell
|
|
|
What are two major risk factors for anal cancer?
|
HPV, Anal Squamous Intraepithelial Lesions (ASIL),
|
|
|
What is a normal pH?
|
7.4
|
|
|
What is a normal PaCO2?
|
40mmHg
|
|
|
What is a normal HCO3?
|
24
|
|
|
What is the Henderson Hesselbalch equation for pH?
|
pH = 6.1 + log(HCO3/0.03PaCo2)
|
|
|
If you see PaCO2 elevate, and the pH lowers, and HCO3 compensates what does this mean?
|
Respiratory acidosis
|
|
|
If you see PaCO2 decrease, pH rise, HCO3 compensates what does this mean?
|
Respiratory alkalosis
|
|
|
If you see an HCO3 decrease, a pH lowers, PaCO2 compensates, what does this most likely mean?
|
Metabolic acidosis
|
|
|
If you see an increase in HC03, a rise in pH, and a PaCO2 compensates.
|
Metabolic Alkalosis
|
|
|
What is an easily reversible cause for respiratory acidosis due to hypercapnea resulting from hyperventilation?
|
Narcotic overdose
|
|
|
A patient can also be too weak to breath and this can cause respiratory acidosis. What is a disorder/disease that could cause this?
|
Myasthenia gravis
|
|
|
When someone is suffering from acidosis what does it do to their overall appearance?
|
It acts as a depressant
|
|
|
When someone is suffering from alkalosis what does it do to their overall appearance?
|
It acts as a stimulant
|
|
|
How do you tx respiratory acidosis?
|
Tx is directed to the underlying cause.
|
|
|
Because opioid drug overdose is an important reversible cause of acute respiratory acidosis, what is the primary way of TX this form of acidosis?
|
Naloxone 0.04-2mg IV if no obvious cause for respiratory depression is present.
|
|
|
Hyperventilation causes?
|
Hypocapnea leading to respiratory alkalosis
|
|
|
In acute cases of this, there is lightheadedness, anxiety, parasthesias, perioral numbness, and tingling sensation in the hands and feet.
|
Respiratory alkalosis
|
|
|
In acute hyperventilation syndrome what is the TX?
|
Rebreathing into a paper bag will increase the PaCO2. Sedation may be necessary if the process persists.
|
|
|
This can present with high anion gap and hyperchloremic (GI loss of bicarb or RTA)
|
Metabolic acidosis
|
|
|
This is either usually saline responsive (volume contraction, low K), or saline unresponsive (hyperaldosteronism)
|
Metabolic alkalosis
|
|
|
What is a normal anion gap?
|
12 +/-4
|
|
|
Anion gap = ?
|
measured anions - measured cations
|
|
|
These are causes of what?
Lactic acidosis Ketoacidosis - diabetic, alcoholic, starvation Renal Failure Toxins - ethylene glycol, methanol, salicylates, propylene glycol, proglutamic acid |
High Anion Gap Metabolic Acidosis (HAGMA)
|
|
|
This may help identify the cause of HAGMA?
|
Plasma Osmolal gap in HAGMA
|
|
|
What is the most common cause of plastma osmolal gap?
|
Alcohol intoxication (as from methanol or ethylene glycol)
|
|
|
What are the main causes of hyperchloremic metabolic acidosis?
|
GI bicarbonate loss and Renal Tubular Acidosis
|
|
|
With this you will see a negative urinary anion gap.
|
GI bicarbonate loss
|
|
|
With this inability to excrete H+, generate HCO3-, or reabsorb HCO3- occurs
There are three major types, 1, 2 and 4 The urinary anion gap varies |
Renal Tubular Acidosis
|
|
|
When this is severe, Kussmaul respirations (deep, regular, sighing respirations) are seen.
|
Metabolic acidosis
|
|
|
In general, severe acidosis (pH<7.20) warrants the IV administration of?
|
NaHCO3 50-100 meq over 30-45min, during the initial 1-2 hours of therapy.
|
|
|
What is it essential to do when administering therapy for metabolic acidosis?
|
Monitor plasma electrolytes during the course of therapy since the K may decline as pH rises.
|
|
|
What is the goal in TX metabolic acidosis?
|
The goal is to increase the HCO3- to 10meq/L and the pH to 7.15, not to increase these values to normal.
|
|
|
This occurs as a result of net gain of HCO3 or loss of nonvolatile acid (usually HCl by vomiting) from the extracellular fluid.
Involves a generative stage (in which the loss of acid usualloy causes alkalosis) and a maintenance stage (in which the kidneys fail to compensate by excreting HCO3) |
Metabolic alkalosis
|
|
|
This is characterized by extracellular volume contraction and hypokalemia
Urine chloride low (unless caused by diuretics) Urine HCO3 reabsorption is increased proximally accounting for paradoxic aciduria |
Saline responsive metabolic alkalosis
|
|
|
This is characterized by:
Hyperaldosteronism Extracellular volume expanded Urine chloride high |
Saline unresponsive metabolic alkalosis
|
|
|
Mild alkalosis is generally well tolerated, but severe or symptomatic alkalosis pH > ___? requires urgent treatment.
|
pH > 7.6
|
|
|
This is when you can have the presence of over 1 simple disorder.
Can have double or triple disorders but not quadruple (because can not have a simultaneous respiratory acidosis and respiratory alkalosis) |
Mixed disorders
|
|
|
What are the six steps in acid base diagnosis?
|
1. Obtain ABG and Lytes at same time.
2. Compare HCO3 values to verify accuracy 3. Calculate the anion gap 4. Determine primary abnormality 5. Assess compensatory response 6. Assess the delta ratio for high anion gap |
|
|
True or False:
If pH is normal, then by definition no acid base disorder is present? |
False
|
|
|
How do you calculate anion gap from labs?
|
Na - HCO3 + Cl = Anion Gap
|
|
|
How do you calculate delta ratio?
What does it mean if the delta ratio is over 2? |
Delta AG = calculated anion gap - normal anion gap
Delta HCO3 = Patient HCO3 lab value - normal HCO3 Delta ratio = Delta Anion Gap/Delta HCO3 |

