![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
40 Cards in this Set
- Front
- Back
|
what organs are in the foregut
|
oesophagus --> miduodenum
|
|
|
midgut
|
mid-duodenum--> 2/3 transverse colon
|
|
|
hindgut organs
|
1/3 transverse colon--> 1/2 anal canal
|
|
|
purpose of mucosal layers at:
- oesophagus & anus - stomach - small int - large int (colon) |
OES & ANUS: protective
STOM: secretory SMALL: absorp (nutrients) COLON: absorp (water, secretion (mucus)q |
|
|
what the enteric nervous system
where does it innervate how is it influenced by ANS |
independent NS within WALLS of GI organs
- control contraction smooth muscle ANS: par ↑speed, symp ↓speed |
|
|
which 3 sphincters control flow of GI content
- what type of muscle - loc |
PYLORIC- stomach exit, smooth m.
INTERNAL anal- sup anal canal, smooth m. EXTERNAL anal- infer anal canal, skeletal m. |
|
|
what lines internal wall of stomach
|
rugae
|
|
|
where does the abdominal aorta bifurcate
|
level of the umbilicus- T4
|
|
|
what cells make up the peritoneum
|
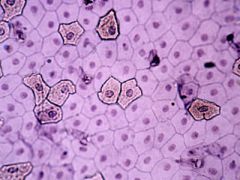
simple squamous epethelium - MESOTHELIUM
|
|
|
what't the omental foramen
where is it what lies anterior to it |
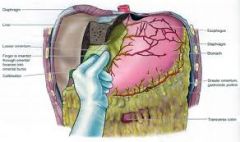
communication between the greater & lesser sacs
posterior free edge of lesser omentum ANT: hepatoduodenal liagment (containing PORTAL TRIAD) |
|
|
structure and attachments of greater omentum
|
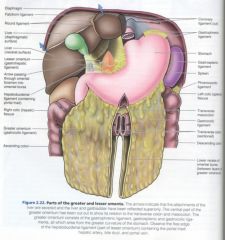
greater curve of stomach --> apron --> folds back on itself --> attaches back onto anterior transverse colon
double layerd mesothelium --> 4 layered omentum |
|
|
what's contained within the mesentery
|
blood vessels
nerves lymphatics |
|
|
which intraperitoneal pouches are present in the male
|
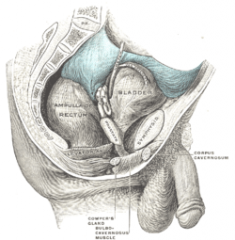
RECTOVESICAL: between rectum/ bladder
|
|
|
which intraperitoneal pouches are present in the female
|
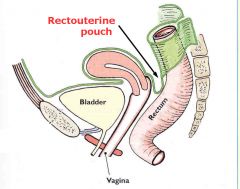
UTEROVESICAL: uteruus/ bladder
RECTOUTERINE: rectum/ uterus |
|
|
where does fluid collect in peritoneal infection
|
male or female pouches
rectovesical (M) rectouterine or uterovesical (F) |
|
|
name some retroperitoneal organs
|
oesophagus
duodenum (part 2-4) ascending & descending colon kidneys, IVC & aorta anal canal & rectum |
|
|
name some intraperitoneal oragns
|
stomach
1st part duodenum liver spleen pancreas small int transverse colon sigmoid |
|
|
role of the gallbladder
what is it stimulated by |
stores and concentrates bile (synthesised in liver)
contractions stimulated b y FAT & PROTEIN (mediated by hormone CCK) |
|
|
what sensory nerve supply is to the body wall (abdo muscles) and PARIETAL pleura
what can it sense characteristic pain |
SOMATIC sensory
-pressure, PAIN, heat, laceration PAIN: localised, sharp, stabbing no referred pain (except inferior surface diaphragm) |
|
|
irritation of the inferior surface of the diaphragm causes what particular pain feature
|
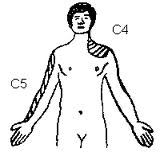
REFERRED pain
C3,4,5 --> shoulder tip pain dermatomes supplied by those cervical spinal nerves |
|
|
visceral nerve supply (sensory & motor) to smooth muscle of GI tract and VISCERAL peritoneum supplied by which nerve
sensitive to what characteristic pain |
CN X VAGUS
- insensitive to touch, heat, laceration - senses: stretch, ischaemia, inflammation, chemical irritation PAIN: poorly localised, dull, ache, nausea |
|
|
visceral pain sensation from GI organs or visceral peritoneum can be referred where
|
foregut --> epigastrium
midgut--> umbilius hindgut --> suprapubic |
|
|
route a somatic pain signal would take
|
1) somatic sensory nerve stimulation - AFFERENTS
2) POSTerior route spinal nerve (crossing over in spinal cord) 3) CNS (thalamus --> cerebral cortex) 4) somatic motor EFFERENTS 5) spinal cord crossing over 6) skeletal muscle effector |
|
|
route visceral pain signal
|
1) sensory visceral afferents
2) vagus sacral spinal ganglia (parasymp carnio-sacral outflow) 3) referred to dermatome |
|
|
describe the pain of appendicitis and how it changes
|
initial STRETCH irritation of VISCERAL peritoneum --> VISCERAL pain referred to umbilical region...
later irritation of PARIETAL peritoneum --> localised SOMATIC pain in RIF |
|
|
at which part does bile from the liver enter the duodenum
|
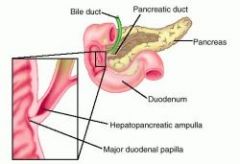
2nd part of duodenum via major duodenal papilla
|
|
|
where can teh fundus of the gallbladder be located
|
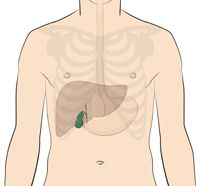
costal margin of 9th rib
|
|
|
what's in the portal triad
|
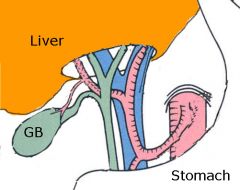
hepatic artery
hepatic portal vein CBD ANS nerves & lymphatics |
|
|
3 main initial branches off the celiac trunk
|
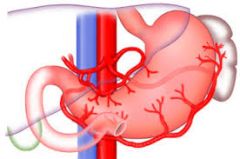
left gastric------splenic----------hepatic
|
|
|
what branch does the splenic artery give
|
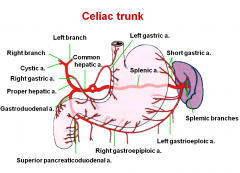
left gastro-omental
|
|
|
what branches does the hepatic artery give
|
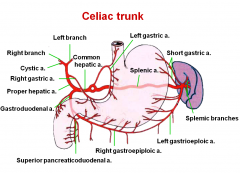
right gastric----gastroduodenal
|
|
|
gastroduodenal arises from the hepatic artery of the celiac trunk.
what does this divide to give |
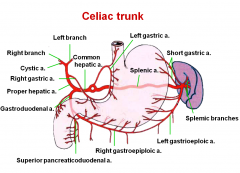
pancreaticoduodenal ----right gastro-omental
|
|
|
coeliac trunk --> hepatic artery
- what does teh hepatic artery divide into |
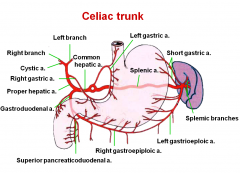
cyctic artery ----- R & L hepatic branches
|
|
|
how does the hepatic portal vein form
|
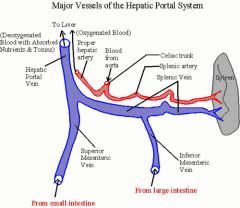
IMA drains into splenic
SMA merges with splenic |
|
|
CBD flow into duodenum controlled by what
|
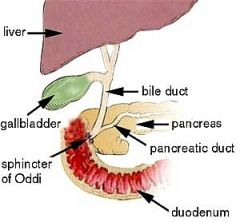
sphincter of oddi
|
|
|
lobes of liver and loc
|
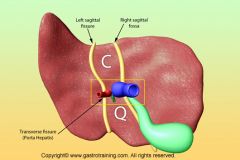
R,L, caudate, quadrate
|
|
|
what structure divides the L & R liver lobes anteriorly
|
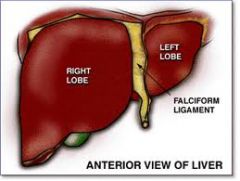
falciform lig --> round lig (embryological remnent)
|
|
|
all nutreints except what is conveyed to liver by portanl system for METABOLISM
- what does liver store - what does it secrete in GI tract |
except FAT
- stored GLYCOGEN - synthesises BILE |
|
|
acinar cells of pancreas - role and secretion
langerhans cells of pancreas- role & secretions |
ACINAR: EXOcrine- pancreatic juices via DUCTS
ISLETS: ENDOcrine- hormones into BLOOD (end-no ducts!) |
|
|
what's a cholecystectomy
|
removal of gallbladder (dissect portal triad)
|

