![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
30 Cards in this Set
- Front
- Back
|
What is the normal range of serum bilirubin and above what level do you see jaundice? |
Normal = 3-20 umol/L Above 35 umol/L = visible jaundice |
|
|
Majority of bilirubin is secreted by what and as what? |
Majority of bilirubin (99%) secreted as urobilin in stool. |
|
|
List steps in bilirubin processing incl. where things happen |
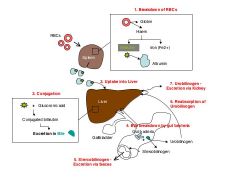
1. Spleen - RBC broken into Haem + globin - Haem broken into bilirubin + Iron 2. Circulation - Bilirubin + albumin = unconjugated bilirubin forms 3. Liver - Glucoronic acid conjugates bilirubin - Bile formed and stored in gallbladder 4. Gut - Bile broken down into urobilinogen and stercobilinogen 5. Stercobilinogen excreted in feces, Urobilinogen excreted in urine. Some urobilinogen reabsorbed by liver. |
|
|
What is bile made of? |
Bile = Bilirubin + cholesterol + bile salts |
|
|
Most common hereditary cause of increased bilirubin |
Gilbert's syndrome - mild decrease in glucuronyltransferase activity |
|
|
Enzyme that conjugates bilirubin |
glucuronyltransferase |
|
|
What is hereditary spherocytosis |
Hereditary spherocytosis is an auto-hemolytic anemia characterized by the production of red blood cells (RBCs) that are sphere-shaped (spherocytosis) rather than the normal biconcave disk shaped (donut-shaped) RBCs. This shape is more prone to rupture. One cause of prehepatic jaundice. |
|
|
List 8 causes of prehepatic jaundice |
- hemotlytic anaemia - hereditary spherocytosis - thalassaemias - G6PD deficiency - sickle cell anaemia - drugs - large hematoma being degraded (transient) - neonatal jaundice |
|
|
List 9 causes of intrahepatic jaundice |
Hepatocellular disease Viral infections (hepatitis A, B, and C) Chronic alcohol use Autoimmune disorders Intrahepatic malignancy Other Drugs (e.g. paracetamol o/d) Pregnancy Parenteral nutrition Sarcoidosis Primary biliary cirrhosis Primary sclerosing cholangitis |
|
|
List causes of post-hepatic jaundice |
- Gall stones / cholelithiasis |
|
|
Urine and stools in cholestasis |
Dark urine as most bilirubin is being secreted via urine (since bile/chole flow into gut is blocked/stasis) Pale stools because bile flow into gut is blocked. Bile gives stool the characteristic brown color. Without it, stools are pale. |
|
|
One examination sign in patients with increased hemolysis |
Splenomegaly |
|
|
What could scratch marks be due to in a patient presenting with jaundice |
Pruritis due to bile salts deposition in the skin |
|
|
What is the yellowing of sclera and skin in Jaundice called? |
Icterus |
|
|
Investigations in jaundice |
LUV SCUBA * LFTs * Urine urobilinogen + urine bilirubin * Virology (Hep viruses + EBV + CMV) * Serum bilirubin * Coagulation studies * Ultrasound (?bile ducts obstruction) * Blood screen (?anemia) * Amylase (?pancreatitis) |
|
|
What type of jaundice? Conj br - raised Unconj br - normal |
Post-hepatic |
|
|
What type of jaundice? Conj br - normal Unconj br - raised |
Pre-hepatic |
|
|
Urine bilirubin in pre-hepatic jaundice? |
Absent (i.e. normal) |
|
|
Urine bilirubin in post-hepatic jaundice? |
Increased |
|
|
Presence of bilirubin in urine indicates what? |
High levels of conjugated bilirubin in the blood |
|
|
Liver disease in which copper accumulates. What is it called and what is one sign of it? |
Wilson's disease and the signs in brown rings near the inside edge of the iris (copper deposition). The sign is called Kayser-Fleischer Rings. |
|
|
Observable signs of liver disease. (13 - FLASH PADLOCKS) |
FLASH PADLOCKS * Clubbing * Leukonychia * Palmar erythema * Spider naevi (upto 5 are normal) * Fetor hepaticus * Asterixis * Ascites * Lymphadenopathy * Kayser-Fleischer rings (Wilson's disease) * Bronze discolorisation (Iron) * Dupuytren's contracture * Caput medusae (portal htn) * Hemorrhoids * Oesophageal varices * Oedema * Scratch marks (pruritis) |
|
|
Two hepatomegalic diseases, and one hepatoatrophic disease. |
Hepatomegaly - hepatitis (inflammation), and fatty liver Atrophic - cirrhosis |
|
|
Two types of hepatotoxicity |
Type A - intrinsic - predictable Type B - idiosyncratic - unpredictable |
|
|
4 presentation types of hepatotoxicity |
1. Hepatitis-like 2. Cholestasis 3. Steatosis 4. Zonal necrosis |
|
|
Common causative agents of:
hepatitis-like injury |
Isoniazid
Phenytoin |
|
|
Common causative agents of:
cholestatic injury |
Rifampicin
Augmentin
Carbamazepine |
|
|
Common causative agents of:
steatotic injury |
Amiodarone,
Tetracycline (abxs),
Protease inhibitors (antivirals),
Methotrexate |
|
|
Investigations in suspected hepatotoxicity |
- FBC - LFTs - INR - U&C - Ultrasound of liver and gallbladder - Abdo CT - Liver biopsy if needed |
|
|
Management in patient w hepatotoxicity |
1. ABC 2. Stop offending drug if known 3. Antidote if available 4. Correct electrolyte imbalances 5. Analgesia 6. Liver transplant if damage to liver is too severe and widespread |

