![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
102 Cards in this Set
- Front
- Back
|
*What radiographic views are critical to diagnose fractures?
|
Orthogonal views (at least 2)
|
|
|
When can oblique radiographs be useful in detecting a fracture?
|
X-rays parallel to fracture
Minimally displaced fractures |
|
|
When might you want to take a radiograph of the opposite limb as well?
|
Young animals (physes)
Implant size selection |
|
|
Why should you always take a radiograph of the joint above and below a fracture?
|
To assess the displacement of the limb
|
|
|
What are the 5 factors of fracture detection?
|
1. Quality of radiograph
2. Direction of X-ray beam 3. Degree of displacement 4. Summation of overlying structures 5. Knowledge of normal anatomy |
|
|
How does the x-ray beam need to hit a bone relative to the fracture in order to detect the fracture?
|
X-ray beam has to be parallel to the fracture for detection
|
|
|
What are the 8 features used to describe a fracture?
|
1. Complete/incomplete
2. Direction of fracture 3. Location-which bone 4. Location-within bone 5. Degree of comminution 6. Displacement 7. Open/closed 8. Special types |
|
|
What is a complete fracture? Incomplete?
|
Complete=through both cortices
Incomplete=one cortex or a fissure |
|
|
When describing the direction of a fracture what axis are you using?
|
The long axis of bone
|
|
|
What do you call a break that is straight across the bone (90 degrees)?
|
Transverse
|
|
|
*What is a short and long oblique fracture?
|
Long oblique=0-45 degrees
Short oblique=45-89 degrees |
|
|
What causes a spiral fracture?
|
Torsional trauma, then fracture goes in a spiral
|
|
|
What do you need to include when stating which bone has the fracture detected in a radiograph?
|
Whether its left or right
|
|
|
What are some examples of bone location (within bone) of a fracture?
|
Diaphyseal
-proximal, mid or distal Metaphyseal -Metaphyseal in immature -Metaphyseal region of diaphysis if mature Physeal -Immature |
|
|
What determines if a fracture is comminuted or simple?
|
Number of fracture lines
|
|
|
What is a simple fracture?
|
One fracture line
|
|
|
What is a comminuted fracture?
|
Bone divided into 3 or more fragments
-Mild, moderate or severe |
|
|
*How do you describe the displacement of a fracture?
|
Describe the displacement of the part that is no longer connected to the body w/ respect to the body.
-Cranial/caudal -Medial/lateral -+/- overriding (2 pieces overlap) |
|
|
What is an open fracture?
|
Has external communication
|
|
|
How can you identify an open fracture? (3)
|
1. Gas in soft tissues
-immediate=open -Many days post injury=open or infected 2. Bone extending beyond soft tissues 3. Physical exam diagnosis |
|
|
True or false. If you see gas in the soft tissue near a fracture then it means it is an open fracture.
|
False, could be infection too if it's been several days after the injury
|
|
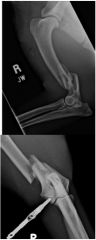
Describe the fracture.
|
-Complete
-Likely open -Short oblique fracture -Of the distal diaphysis -Of the right humerus -With mild comminution -and caudal, lateral and mild overriding displacement |
|
|
What are the 6 specific fracture types?
|
1. Salter Harris
2. Avulsion 3. Compression 4. Condylar 5. Chip 6. Slab |
|
|
*What is an avulsion fracture?
|
Fracture occurs at the site of soft tissue attachment on the bone
-Piece of bone is ripped off bc the soft tissue ripped it off |
|
|
Where are avulsion fractures especially common?
|
At apophyses (has nubbins and ridges)
-Occurs at medial and lateral collateral ligaments too |
|
|
What type of view can be really helpful in diagnosing avulsion fractures?
|
Stressed views
-may see what looks like sand that is avulsion fragments -Joint shouldn't really open hardly at all |
|
|
What is a compression fracture?
|
Bone is crushed
-Bone is shorted -+/- increased opacity |
|
|
Where do compression fractures typically occur?
|
Vertebrae or epiphyses
|
|
|
What is a condylar fracture?
|
Where the condyle is separated from the parent bone
|
|
|
What is a bi-condylar fracture?
|
Between the condyles
|
|
|
What is a supracondylar fracture?
|
Proximal to the condyle
|
|
|
*What is a chip fracture?
|
Involves one articular surface
|
|
|
What animals typically get chip fractures?
|
Horses
-And greyhounds that run in circles |
|
|
Are chip fractures a small or large bone fragment?
|
Small fragment
|
|
|
What 2 injuries generally result in chip fractures?
|
Direct bone trauma
Hyperextension injury |
|
|
*What is a slab fracture?
|
Involves 2 articular surfaces
|
|
|
What animals typically get slab fractures?
|
Horses
|
|
|
Do slab fractures have a small or large bone fragment?
|
Large bone fragment
|
|
|
What 2 types of injury can cause slab fractures?
|
Hyperextension injury
Repetitive stress |
|
|
*How many condyles does the humerus have? Femur?
|
Humerus= 1 condyle
Femur=2 condyles |
|
|
What breed of dog is predisposed to fracturing the humeral condyle? Why?
|
Spaniels-have incomplete ossification of humeral condyle so it never completely mineralizes so relies on soft tissues
|
|
|
What do you need to do while you have a spaniel with a condylar fracture still anesthetized?
|
Check the other leg because probably incompletely mineralized on that leg too so can take preventive measures
|
|
|
What does it mean when you say the condyle was "ununited"?
|
Means the condyle wasn't completely fused and completely came off
|
|
|
Why does repetitive stress result in chip or slab fractures?
|
Repetitive stress causes damage then add more bone and more bone which becomes brittle and fractures
|
|
|
What happens any time a fracture happens on the articular surface of a bone?
|
Arthritis will develop
|
|
|
What are 3 causes of secondary fractures?
|
1. Fatigue/stress (typically performance
2. *Pathologic 3. Folding |
|
|
*What are 3 underlying processes that can result in pathologic fractures?
|
Neoplasia
Osteomyelitis Osteopenia |
|
|
What animals get osteopenia?
|
Young animals that are not fed properly, animals lacking calcium and vitamin D can get secondary hyperparathyroidism--> osteopenia
|
|
|
What can happen to the bones of adult animals in renal failure?
|
Can get secondary renal hyperparathyroidism and rubber jaw
|
|
|
What is a secondary fracture due to bone folding usually due to?
|
Osteopenia/hyperparathyroidism
|
|
|
What are stress fractures?
|
Microfractures in the bone cortex
|
|
|
What causes stress fractures?
|
Repetitive stress/cyclical loading
|
|
|
What animals are predisposed to stress fractures?
|
Performance horses
-Bucked shins Racing greyhounds |
|
|
**What is a pathologic fracture?
|
Pre-existing disease causes bone to fracture spontaneously
-Mild or no trauma in history |
|
|
True or false. Pathologic fractures due to hyperparathyroidism is usually secondary not primary hyperparathyroidism.
|
True
|
|
|
*What are pathologic fractures most commonly due to?
|
Neoplasia
-Osteosarcoma |
|
|
You take a radiograph and see an aggressive lesion right near where the fracture is, what should you do while the animal is still asleep?
|
It's a pathologic fracture- take a chest film!
|
|
|
*If a fracture seems to have occurred for no reason, what should you do?
|
Biopsy the fracture site
Take thoracic radiographs |
|
|
What is the difference b/w how normal bone looks compared to abnormal bone when fractured (pathologic fracture VS non-pathologic fracture)?
|
Normal bone breaks in sharp margins, but pathologic fractures tend to have round fractures (if old could be bone remodeling)
|
|
|
If you were asked the opacity of metastasis in the chest, what would you say?
|
Soft tissue
|
|
|
What region of bone lesions make you think metastasis? Primary lesion?
|
Metastasis=diaphyseal region
primary= metaphyseal region |
|
|
How do folding fractures due to osteopenia appear on radiographs?
|
-Bone is less opaque with thin cortices
-Cortex is bent -Fracture lines overlap=appear sclerotic |
|
|
*What are 2 types of secondary hyperparathyroidism that result in folding fractures?
|
-Nutritional secondary hyperparathyroidism
-Renal secondary hyperparathyroidism |
|
|
*What bones will be most affected by the nutritional secondary hyperparathyroidism?
|
Long bones
|
|
|
*What bones will be most affected by an adult animal with renal secondary hyperparathyroidism?
|
Skull (rubber jaw)
|
|
|
What has to be present in order to have any type of a Salter Harris fracture?
|
A physis
-All types are physeal fractures |
|
|
What does a higher number mean when talking about Salter Harris fractures?
|
Higher number=more likely to cause altered physeal growth
-goes from bad to worse |
|
|
What is a type I-V Salter Harris fracture?
|
1=physis only
2=physis/metaphysis 3=physis/epiphysis 4=physis/metaphysis/epiphysis 5=Physeal crushing |
|
|
How can physeal crushing appear on a radiograph? What should you do if you suspect physeal crushing?
|
Like a closed physis, if suspect then take a radiograph of the other leg
|
|
|
What are the 2 types of fracture healing?
|
1. Primary bone healing
2. Secondary bone healing |
|
|
*What type of fracture healing is the most common?
|
Secondary bone healing
|
|
|
What is primary bone healing?
|
-Direct healing by osseous tissue (extension of Haversian osteons across gap)
-Very small fracture gap (0.15-0.3 mm)=direct contact -Extremely rigid fixation |
|
|
What is secondary bone healing?
|
-Most common
-Callus formation |
|
|
How is primary bone healing characterized radiographically?
|
-Lack of periosteal callus
-Gradual loss of fracture line |
|
|
*What are the steps of callus maturation? (steps of secondary bone healing)
|
1. Hematoma
2. Granulation tissue 3. Fibrocartilage 4. Mineralized cartilage 5. Bone |
|
|
*What are the opacities related to the stages of secondary bone healing?
|
-Hematoma, granulation tissue, fibrous & cartilaginous callus=soft tissue opaque
-Endochondral ossification and bony callus, remodeling= mineral opaque |
|
|
What are you actually seeing when you see a fracture on a radiograph?
|
Soft tissue silhouetting with soft tissue in the gap
|
|
|
True or false. A fracture gap does not normally get wider as healing happens.
|
False, fibrous tissue grows into bone on either side of the fracture so the fracture gap gets wider-a good sign that healing is happening
|
|
|
**What happens during week 1 of secondary bone healing?
|
Resorption of fracture margins and vascular ingrowth
Widening of fracture gap, rounding of fracture margins |
|
|
What happens during week 3 of secondary bone healing?
|
Periosteal, endosteal and intercortical callus
|
|
|
What happens during week 4 of secondary bone healing?
|
Callus becomes well-defined and begins to bridge the fracture gap
|
|
|
What happens after week 4 of secondary bone healing?
|
Fracture line slowly disappears and callus becomes like parent bone.
|
|
|
**What are the 4 A's of fracture implant assessment?
|
1. Alignment
2. Apposition 3. Apparatus 4. Activity |
|
|
To assess the alignment of a fracture implant, what should you be looking at?
|
The joints above and below the fracture
|
|
|
What is the apposition when assessing fracture implants?
|
How much the pieces touch
|
|
|
What is the apparatus when assessing fracture implants?
|
The implants-the plates and screws
|
|
|
What is the activity when assessing fracture implants?
|
Healing
|
|
|
Can you assess the activity of a fracture implant immediately post op?
|
No, shouldn't be any activity immediately after, that's something you assess w/ time
|
|
|
*What does it mean if you see lucency around implant pins?
|
Motion OR osteomyelitis
-Loosening and infection both manifest as lucency |
|
|
Other than detecting lucency around implants, what are 7 other implant complications?
|
1. Implant migration
2. Bending/breaking of implants 3. Implant associated neoplasia -Sarcomas, femur, 5.8 yrs post fracture 4. Delayed union 5. Mal-union 6. Non-union 7. Sequestrum |
|
|
What is delayed union?
|
Not healed in expected time for bone/patient age etc
|
|
|
*What does it mean when there's non-union during fracture healing?
|
All signs of repair have ceased and further healing will not occur without surgical intervention.
|
|
|
What is mal-union?
|
Healed or healing in a non-anatomic position
|
|
|
True or false. Mal-union requires surgical intervention to finish healing.
|
False, that's non-union
|
|
|
What is a sequestrum?
|
Dead bone fragment
|
|
|
**How do sequestrums appear on radiographs?
|
Sclerotic fragment outlined by decreased opacity
|
|
|
What does it mean when a non-union fracture healing is atrophic?
|
Bone is dissolving-very bad
|
|
|
*What are the 3 components of a sequestrum?
|
1. Sequestrum
2. Involucrum 3. Cloaca -+/-draining tract |
|
|
*What is an involucrum?
|
Reactive bone that encloses a bone sequestrum
-Outer rim of sclerotic bone |
|
|
How often should you recheck a fracture?
|
Every 4-6 weeks
|
|
|
*If an animal has a fracture and an aggressive lesion is suspected, what should you do?
|
Repeat radiographs in 7-10 days
|
|
|
*If a bone breaks for no reason, what should you do?
|
Thoracic radiographs
Bone biopsy |

