![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
100 Cards in this Set
- Front
- Back
|
Name 6 cell types found in the walls of the respiratory mucosa
|
1. Ciliated columnar epithelium (respiratory epithelium)
2. Simple columnar epithelium (secretory epithelium) 3. Mucous goblet cells 4. Brush cells 5. Diffuse endocrine cells 6. Basal cells |
|
|
What is the structure and function of respiratory epithelium?
|
pseudostratified columnar epithelium with cilia that beat distal to proximal.
Most predominant epithelium cell Continues until respiratory bronchioles |
|
|
What is the structure and function of secretory epithelium?
|
Simple columnar epithelium
Responsible for serous secretions |
|
|
What is the structure and function of mucous goblet cells?
|
Synthesis of mucinogen, which becomes mucous when hydrated.
Present until terminal bronchioles. |
|
|
What is the structure and function of Brush cells?
|
They have no cilia, many microvilli.
Are responsible for the sneeze reflex |
|
|
What is the structure and function of diffuse endocrine cells?
|
Control mucous and seromucous secretion
Control vessel diameter |
|
|
What is the structure an function of basal cells?
|
Rest on the basement membrane.
Do not reach the lumen--pseudostratified. Stem cells. |
|
|
Which cell is thought to be responsible for the sneeze reflex?
|
Brush cells
|
|
|
What is metaplasia?
|
Abnormal transformation of adult cells in a tissue to a form which in not normal for that tissue. Can be a response to disease, physical, or chemical event.
|
|
|
What cell type will be increased in a smokers epithelium? Which is decreased?
|
Goblet cells are increased. Decrease in cilia due to carbon monoxide.
|
|
|
The respiratory system has two parts. Name them.
|
1. Conducting system
2. Respiratory system |
|
|
What is the function of the conduction system?
|
1. Provides conduit to transfer air
2. Cleans, moistens, and warms air |
|
|
What are four main tissue types present in the conduction system?
|
1. Cartilage
2. Elastic fibers 3. Collagen fibers 4. Smooth muscle |
|
|
How does the concentration on elastic fibers change from proximal to distal?
|
Increases
|
|
|
How does the concentration of collagen change from proximal to distal?
|
Decreases
|
|
|
What is the relationship between the elastic fiber concentration and the diameter of the respiratory system?
|
Inverse relationship. As diameter gets smaller, the [elastic] increases
|
|
|
What is the orientation of the elastic fibers in the lamina propria?
|
Longitudinal
|
|
|
What is the smooth muscle orientation in the conduction portion?
|
Mostly circular
|
|
|
What is the function of the nasal cavity?
|
To filter, warm, and humidify air
|
|
|
What unique cell type is found in the nasal cavity?
|
Olfactory mucosa
|
|
|
Where is the vestibule?
|
The anterior portion of the nasal cavity.
|
|
|
What is vibrissae?
|
Nose hair, generally whiskers on animals.
|
|
|
What structures can be found in the nasal fossa?
|
Concha (inferior, middle, superior)
|
|
|
What antibodies do plasma cells in the lamina propria release?
|
IgA and IgE
|
|
|
IgE will bind basophils and mast cells. What reaction will this cause?
|
Binding of allergen or antigen to this bound IgE/mast cell complex causes the release of inflammation mediators of the mast cell and basophil. Causes symptoms of hay fever and colds.
|
|
|
Many medications are delivered via the nasal cavity. Why?
|
Easy access to the venous plexus beneath the nasal mucosa.
|
|
|
Where can drainage from an infected maxillary sinus be seen?
|
Below the middle concha (due to the opening to the sinus in that location)
|
|
|
The nasal cavity is separated into two parts. Name them.
|
1. Olfactory area
2. Respiratory area |
|
|
Where is the olfactory area?
|
Roof of the nasal cavity and on the superior nasal concha.
|
|
|
The olfactory epithelium consists of 3 cell types. Name them.
|
1. Olfactory cell
2. Sustentacular cell 3. Basal cell |
|
|
Describe the structure of olfactory cells.
|
1. Bipolar neurons whose apical surfaces are modified to form the olfactory vesicle and olfactory cilia
2. Dendrites terminate in bulbous olfactory vesicle with 6-20 nonmotile cilia 3. form an odor receptor on ciliated surface. |
|
|
How is something smelled?
|
Odor molecule, dissolved in serous fluid, binds protein receptor (which is made in Bowman's glands). Once threshold is meet, triggers olfactory bulb.
|
|
|
What is the function and description of sustentacular cells?
|
supporting cells with apically located ovoid nuclei.
|
|
|
What is the function of the basal cell in the olfactory epithelium?
|
They are stem cells for all the olfactory epithelium.
|
|
|
What is spatio-temporal patterning?
|
Olfactory linked to memory.
|
|
|
Describe the structure and function of the Bowman's glands?
|
1. Located in the lamina propria
2. Synthesis of an odorant binding protein 3. Seromucous secretion important in dissolving odors and cleans the surface |
|
|
What are swell bodies and why do they occur?
|
venous plexus in lamina propria that enlarge alternately on two sides of nasal cavity (every 30 minutes) giving mucosa on occluded side time to recover from desiccation and help to direct air to the olfactory epithelium
|
|
|
Where does the IgA secrete by plasma cells in the nasal cavity lamina propria go?
|
Into the olfactory gland (Bowman's gland).
|
|
|
Where are the nuclei of the olfactory cells located?
|
Centrally in the olfactory epithelium.
|
|
|
What are paranasal sinuses?
|
air spaces within bone lined with respiratory epithelium.
|
|
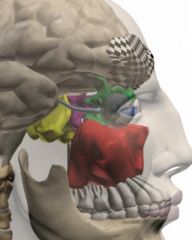
Name the sinuses
|
Frontal sinus is black check
Maxillary sinus is red Anterior ethmoid sinuses are green Posterior ethmoid sinuses are purple Sphenoid sinus is yellow |
|
|
The larynx connects what two structures?
|
The pharynx to the trachea
|
|
|
The larynx is made of what two tissues?
|
Large hyaline plates and small elastic cartilage plates
|
|
|
The larynx is responsible for phonation. Why?
|
Houses the vocal cords.
|
|
|
What structure in the larynx prevents food and fluid from entering the respiratory system?
|
Epiglottis
|
|
|
Epiglottis has two sides. Name them.
|
Tracheal and lingual
|
|
|
The epiglottis has two types of epithelium. Name them and the surface on which they appear.
|
1. Lingual surface is stratified squamous epithelium
2. Tracheal surface is pseudostratified ciliated columnar epithelium (respiratory epithelium). |
|
|
What makes up the core of the epiglottis?
|
Elastic cartilage
|
|
|
During swallowing, what describe the movement of the tongue and the epiglottis.
|
backward motion of tongue forces epiglottis over the laryngeal opening, closing the larynx and directing food into the esophagus
|
|
|
The larynx houses vocal cords. Name them.
|
True and False vocal cords.
|
|
|
Describe the structure of the false vocal cords.
|
They are the upper folds in the larynx.
They are covered by respiratory epithelium, have glands, and not muscle. Forms the anterior border of the laryngeal ventricle. |
|
|
What muscle lines the laryngeal ventricle?
|
Ventricularis muscle
|
|
|
What kind of epithelium lines the true vocal cords?
|
Stratified squamous epithelium (nonkeratinized)
|
|
|
What structures are housed in the true vocal cords?
|
Vocalis muscle (skeletal)
Vocal ligament (elastic fiber) |
|
|
Name the main differences between the false and true vocal cords.
|
1. False is covered by respiratory epithelium. True is covered by stratified squamous epithelium.
2. False has no muscle. True has the vocalis muscle. 3. False has glands. True has no glands. |
|
|
True vocal cords started out being covered by respiratory epithelium, then changed to stratified squamous. What is this process called?
|
Metaplasia
|
|
|
What structure in the larynx is prone to infection?
|
Laryngeal ventricle. Causing laryngitis. Very difficult to treat because is it not a very vascular region and connect be reached with mouth washes.
|
|
|
What four layers of tissue make up the trachea?
|
1. Epithelium (with all 6 cell types present)
2. Lamina propria 3. Submucosa 4. Adventitia |
|
|
What can be found in the lamina propria of the trachea?
|
1. Seromucous glands that can extend into the submucosa
2. Collagen and elastic fibers with well defined elastic lamina |
|
|
What structure is found in the adventitia of the trachea?
|
1. C-shaped hyaline cartilage rings, which are closed off by the trachealis muscle
|
|
|
How is the c-rings of the trachea attached?
|
The perichondrium hyaline cartilage are fused to the submucosa and adventitia.
|
|
|
Describe the main bronchi structure.
|
Very similar to the trachea. Right is straighter and trifurates. The left bifurcates.
Cartilaginous rings become irregular. Smooth muscle spirals between submucosa and cartilage. |
|
|
Describe intrapulmonary division of the bronchi.
|
Secondary (lobar) goes to the lobes.
Tertiary (segmental) goes to the bronchopulmonary segments. |
|
|
Name the epithelium that lines the intrapulmonary bronchi.
|
Respiratory epithelium
|
|
|
Name the two divisions of bronchi.
|
Extra and Intrapulmonary
|
|
|
What glands can be found between the cartilage plates and spiral muscles in the intrapulmonary bronchi.
|
Seromucous glands.
|
|
|
Describe the transition from large bronchi branches to bronchioles.
|
1. No more seromucous glands
2. No cartilage 3. By definition 1mm in diameter 4. Shorter epithelium. From respiratory to shorter simple cuboidal epithelium. 5. No more goblet cells, appearance of clara cells. 6. Predominantly smooth muscle and elastic fibers in the lamina propria. |
|
|
As goblet cells decrease, clara cells increase. Describe the function and location of clara cells.
|
Found in the bronchiole. Have dome-hat shaped appearance.
1. No cilia, only short microvilli 2. Secrete glycoproteins to protect mucosa. 3. Degrade airborne toxins (p450 cytochrome) 4. Can regenerate the bronchiole epithelium. |
|
|
Describe parasympathetic innervation of a bronchiole.
|
Bronchiole constriction
|
|
|
Describe sympathetic innervation of a bronchiole.
|
Bronchiole dilation
|
|
|
What is asthma?
|
Widespread constriction of the bronchioles. Difficulty in expelling air from the lung. Associated with an allergic reaction.
|
|
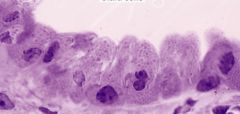
Identify the cell type.
|
Clara cells.
|
|
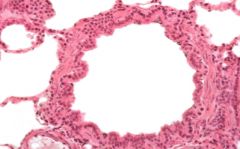
Identify this vessel.
|
Bronchiole
|
|
|
Respiratory portion is made up of four structures. Name them.
|
1. Respiratory bronchiole
2. Alveolar duct 3. Alveolar sac 4. Alveoli |
|
|
Describe the epithelium of the alveolar duct.
|
Simple squamous epithelium-- Type I pneumocyte
|
|
|
What kind of epithelium line the alveoli wall and septum?
|
Type I and Type II pneumocytes
|
|
|
When do most of the alveoli form?
|
85% after birth--by the age of 10.
|
|
|
What is a pore of Kohn and what is its function?
|
Small pores that connect adjacent alveoli. When blockage occurs in the bronchiole, collateral respiration can occur through the pores of Kohn.
|
|
|
Describe the structure and function of a Type I pneumocyte.
|
Simple sqaumous
Attenuated (stretched) for gas exchange Forms 95% of the alveolar surface Cannot regenerate |
|
|
Describe the structure and function of a Type II pneumocyte.
|
Cubiodal
Forms 5% of the alveolar surface Can regenerate the entire alveolar surface Produces surfactant |
|
|
Describe the role and appearance of surfactant in the lungs.
|
Reduces tension in alveoli
Stored in lamellar bodies of Type II pneumocytes. Starts at 23 weeks. Present at 26-28 weeks in amniotic fluid |
|
|
What is Hyaline Membrane Disease and how do you treat it?
|
Premature infants lack sufficient surfactant causing alveoli to collapse
Give mom glucocorticoids to induce synthesis of surfactant by baby |
|
|
What cells form the interalveolar septum?
|
Type I and Type II pneumocytes
|
|
|
What kind of capillaries are found in alveoli?
|
Continuous
|
|
|
What are the 2 portions of the interalveolar septum and what are their functions?
|
1. Thin--gas exchange
2. Thick--wicking of fluid |
|
|
Describe the 4 layers of the blood-gas barrier.
|
1. surfactant
2. cytoplasm of Type I pneumocyte 3. fused basal lamina of Type I pneumocyte and endothelium of capillary 4. Cytoplasm of the endothelium |
|
|
Describe the cells and fibers found in thick portion of the interalveolar septum.
|
1. elastic, collagen, reticular fibers
2. fibroblasts, macrophages and mast cells |
|
|
What is the terminal location of the lymphatics (moving distally).
|
Alveolar sac. No lymphatics in the alveoli.
|
|
|
How is lymph removed from the alveoli?
|
1. Wicking action of thick interalveolar septum.
2. fluid diffuses proximally in the interstitium until it enters small lymphatics at about the level of the respiratory bronchioles. Lymphatics then follow the bronchial tree. |
|
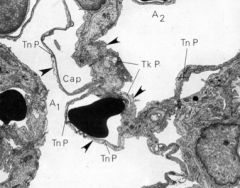
Identify the area between the arrows.
|
Interalveolar septum. Thin and thick.
|
|
|
Name macrophages present in the alveoli and the two types present.
|
Called Dust cells.
1. Free 2. Fixed |
|
|
What do Dust cells produce and why?
|
Elastase to break down debris and fibrosis.
|
|
|
What structure allows the dust cells to roam freely from on alveoli to alveoli?
|
Pores of Kohn
|
|
|
What are heart failure cells?
|
Alveolar macrophages that have phaged an RBC and stain positive for Fe.
|
|
|
The lungs have a dual blood supply and drainage. Name the systems.
|
1. Pulmonary arteries and veins
2. Bronchial arteries and veins |
|
|
What is the function of the pulmonary capillary system?
|
Gas exchange.
Pressure is 25 mmHg |
|
|
What is the function of the bronchial capillary system?
|
Supply the lung.
Pressure is 110-135 mmHg |
|
|
What artery supplies the bronchial arteries?
|
Thoracic aorta
|
|
|
What vessels do bronchial arteries anastomize with?
|
pulmonary arteries
|
|
|
Describe emphysema.
|
Breakdown of the interalveolar septum and wall.
Decreased elasticity "Pink puffer"--enough air, just can't move it Caused by an inhibition of alpha-1 antitrysin, which protects against elastase |

