![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
139 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
functions of bone tissue (2)
|
-bear heavy loads and stresses
-calcium reservoir |
|
|
|
hydroxyapatite
|
calcium phosphate crystal in bone matrix
|
|
|
|
consequences of mineralized matrix (4)
|
-gains hardness
-loses flexibility -reduced diffusion of nutrients -no internal (interstitial) growth |
|
|
|
macroscopic appearance of immature bone
|
cancellous (spongy)
network of bony trabeculae |
|
|
|
microscopic appearance of immature bone
|
woven, disorganized
|
|
|
|
immature bone tissue (when does it develop, characteristics)
|
-primary bone or woven bone
-initially develops in embryo (replaced by mature bone) -not strong |
|
|
|
mature bone tissue (characteristics)
|
-secondary bone or lamellar bone
-replaces immature bone quickly -stronger |
|
|
|
mature bone matrix (compared with immature)
|
-more mineralized
-has lamellar (layered) structure |
|
|
|
two varieties of mature bone
|
-compact (dense)
-cancellous (honey-comb) |
|
|
|
diaphysis
|
shaft of a long bone
|
|
|
|
epiphysis
|
ends of long bone
|
|
|
|
diaphysis (inside)
|
marrow cavity
-contains yellow or red bone marrow |
|
|
|
epiphysis (inside)
|
filled with cancellous bone
|
|
|
|
mature bone walls are made of..
|
compact bone
|
|
|
|
mature bone inside made of..
|
cancellous bone/spongy
|
|
|
|
histological preparations of bone (2)
|
-dried prep
-decalcified prep |
|
|
|
dried preparation of bone
|
-dry, white, unstained
-water and organic material NOT present -only mineral present |
|
|
|
decalcified preparation of bone
|
-purple (collagen still present), acidophillic
-mineral is removed -organic material remains |
|
|
|
extracellular matrix of mature bone (components, abundance)
|
-most abundant
-consists of ground substance and fibers |
|
|
|
cells of mature bone
|
osteocytes
|
|
|
|
EC matrix of mature bone: organic component (ground substance)
|
-similar to cartilage
-has proteoglycan aggregates |
|
|
|
EC matrix of mature bone: organic component (fibers)
|
-collagen type 1
-they are encrusted with minerals (why bone is "mineralized") -makes up 90% of organic component |
|
|
|
EC matrix of mature bone: organic component (proteins)
|
-osteocalcin
-osteonectin --mediate binding of minerals to collagen type 1 |
|
|
|
EC matrix of mature bone: inorganic component (components)
|
hydroxyapatite
-deposited on surface of collagen type 1 fibers; makes them hard |
|
|
|
EC matrix of mature bone: inorganic component (weight)
|
65% of dry weight
|
|
|
|
EC matrix of mature bone: organic component (weight)
|
35% of dry weight
|
|
|
|
3 types of lamellae
|
-concentric
-interstitial -circumferential |
|
|
|
concentric lamellae
|
-most important
-form haversian systems -where stresses are felt -"structural unit" of compact bone |
|
|
|
Haversian Systems
|
-cylinders of compact bone
-formed by concentric lamellae |
|
|
|
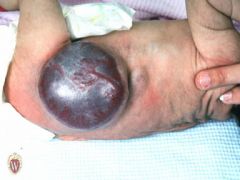
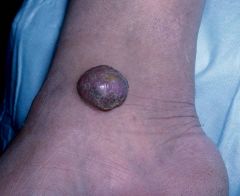
elevated and solid, may or may not be clearly demarcated; deeper in dermis, > 2 cm
|
tumor
a big nodule 2nd pict result of a av malformation |
|
|
interstitial lamellae
|
-whatever is left between osteons-remnants of old osteons
|
|
|
|
haversian canal
|
-center of haversian system
-where blood vessels are found |
|
|
|
volkmann's canal
|
-interconnects haversian canals
|
|
|
|
mature cancellous bone
|
-also lamellar
-not thick enough for osteons-only have interstitial lamellae |
|
|
|
osteocytes (where)
|
-mature bone cells embedded in mineralized matrix
-occupy lacunae |
|
|
|
osteocytes (function)
|
-maintain the extracellular matrix of bone tissue
-secrete the components of matrix for bone maintenance -cannot proliferate |
|
|
|
osteocytes (structure)
|
-elongated
-cytoplasm has filipodia -no basement membrane |
|
|
|
filipodia
|
-extend from osteocytes
-connect with other filipodia=allows communication with surrounding osteocytes |
|
|
|
lacunae
|
spaces in matrix where osteocytes are embedded
|
|
|
|
canaliculi
|
spaces in matrix where filipodia are embedded
|
|
|
|
gap junction (function and location)
|
-located between filipodia, connects cytoplasm
-communication junction |
|
|
|
gap junction (structure)
|
-made up of many connexons
|
|
|
|
connexon pore
|
-transmembrane pore constructed from 6 subunits of the protein connexin
-makes up a gap junction -is permeable |
|
|
|
periosteum (location and function)
|
-connective tissue covering mature bone tissue
-performs appositional growth |
|
|
|
periosteum (2 layers)
|
-fibrous layer
-osteogenic (cellular) layer |
|
|
|
fibrous layer of periosteum
|
-outer layer
-relatively thick -acidophillic-pink -collagen type 1 fibers -fibroblasts |
|
|
|
osteogenic layer of periosteum
|
-inner layer
-thick -contains lots of active osteoprogenitor cells -very few if any collagen type 1 |
|
|
|
osteoprogenitor cells
|
-in osteogenic layer of periosteum
-fusiform shape -no basement membrane -rapidly divide -differentiate into osteoblasts |
|
|
|
osteoblasts
|
-young bone cells
-secrete all organic components of matrix -mineralize the matrix -round/cuboidal -cannot divide |
|
|
|
appositional growth
|
-bone grows in thickness at the periosteum
-new matrix put on old one -single row of osteoblasts |
|
|
|
osteoblasts produce new bone matrix in two steps
|
1. secretion of osteoid
2. mineralization |
|
|
|
Osteoid (components)
|
all organic components of the matrix
-ground substance -collagen type 1 fibers -osteocalcin -osteonectin matrix vesicles |
|
|
|
osteoid matrix vesicles
|
-calcium and phosphate ions
enzymes: -alkaline phosphatase -pyrophosphatase |
|
|
|
osteoid mineralization
|
-begins several days after osteoid production
-hydroxyapatite crystals begin to form in matrix vesicles -crystalization spreads to collagen type 1 fibers -mineralized bone is very acidophillic |
|
|
|
osteocalcin and osteonectin
|
mediate crystalization of collagen type 1 fibers
|
|
|
|
osteocyte
|
-once osteoblast is embedded in immature bone
-replaces immature bone with mature bone tissue |
|
|
|
osteoblasts (lay down)
|
immature bone tissue in two steps
1. secrete osteoid 2. mineralization |
|
|
|
types of ossification (2)
|
1. intramembranous ossification
2. endochondral ossification |
|
|
|
endochondral ossification center
|
-places where cartilage is replaced by bone tissue
|
|
|
|
hypertrophy
|
enlargement of cell
|
|
|
|
2 places where cartilage remains
|
1. articular cartilage
2. epiphyseal plate |
|
|
|
articular cartliage
|
-thin band of cartilage that covers the surface of the epiphysis
-provides smooth surface between bones -always remains as long as bone is healthy |
|
|
|
epiphyseal plate
|
-thick plate of cartilage that remains between the diaphysis and the epiphysis
|
|
|
|
periosteal bone collar (where)
|
established around the diaphyseal portion of a long bone
|
|
|
|
growth of endochondral bone begins..
|
during 2nd trimester (12 weeks) of fetal life and into early adulthood
|
|
|
|
lengthwise growth of bone
|
-through the internal growth of epiphyseal plate cartilage
-begins near the center of the plate and proceeds outward toward the primary ossification center |
|
|
|
lengthwise bone growth (5 distinct layers)
|
1. zone of reserve cartilage
2. zone of proliferation 3. zone of hypertrophy 4. zone of calcified cartilage 5. zone of resorption |
|
|
|
zone of reserve cartilage
|
-population of chondrocytes
-NOT dividing |
|
|
|
zone of proliferation
|
-isogenous groups (division occuring)
-cells actively produce collagen II and XI |
|
|
|
zone of hypertrophy
|
-contains hypertrophic cartilage cells
chondrocytes: -remain active -secrete type I and X collagen -secrete VEGF |
|
|
|
zone of calcified cartilage
|
-hypertrophied cells begin to degenerate
-cartilage matrix becomes calcified -scaffold for new bone -chondrocytes (in more proximal part) undergo apoptosis |
|
|
|
zone of resorption
|
-calcified cartilage in direct contact with connective tissue of marrow cavity
-small blood vessels invade (source of osteoprogenitor cells), then differentiate into osteoblasts -new bone formed -has mixed spicules |
|
|
|
epiphyseal line
|
-remnant of epiphyseal plate
|
|
|
|
bone resorption (what is it)
|
-cellular breakdown of the bone matrix
-important part of bone remodeling |
|
|
|
bone resorption (by who)
|
-done by osteoclasts
|
|
|
|
osteoclasts
|
-members of mononuclear phagocytic system
-very large -multinucleated -rich in lysosomes -developed from bone marrow cells |
|
|
|
resorption bays
|
-Howships lacunae
-depressions of bone matrix -where active osteoclasts lie |
|
|
|
ruffled border
|
-resorbing surface of active cell
-highly folded surface (microvillus structures) -surrounded by cytoplasmic ring |
|
|
|
clear zone
|
-cytoplasmic ring that surrounds the ruffled border of osteoclasts
-contains band of actin filaments that seal the resorption bay |
|
|
|
parathyroid hormone
|
-secreted by parathyroid gland
-secretion stimulated by decline in blood calcium -increases osteoclast activity |
|
|
|
calcitonin
|
-secreted by thyroid gland
-secretion stimulated by increase in blood calcium -decreases osteoclast activity (inhibits bone resorption) |
|
|
|
Rickets
|
-children
-inadequate mineralization of osteoid (soft bone) -lack of Ca/P, vitamin D |
|
|
|
osteomalacia
|
adult rickets
|
|
|
|
osteoporosis
|
-decrease in bone density
-brittle bone -prevalent in post menopausal women (decrease in estrogen-inhibits osteoclasts differentiation) |
|
|
|
muscle cells also known as
|
muscle fibers or myofibers
|
|
|
|
sarcoplasm
|
cytoplasm of muscle cells
|
|
|
|
sarcolemma
|
plasma membrane of muscle cells
|
|
|
|
external lamina
|
basal lamina of the basement membrane of muscle cells
|
|
|
|
endomycium
|
loose connective tissue that supports the basement membrane
|
|
|
|
striated muscle (2 classes)
|
-skeletal
-cardiac |
|
|
|
nonstriated muscle (1 class)
|
smooth muscle
|
|
|
|
skeletal muscle classified as 3 types of muscle
|
1. striated
2. somatic (outer body wall) 3. voluntary |
|
|
|
characteristics of skeletal muscle fibers
|
-cylindrical, linear cells
-unbranched -extend from origin to insertion -each cell is multinucleated -nuclei on periphery of cell -each cell separated from other cells by endomycium -cells do not communicate with each other -each cell has own innervation |
|
|
|
myoblasts
|
-can divide
-fuse and form muscle fiber |
|
|
|
true syncytium
|
each muscle fiber has a "true fusion"
|
|
|
|
fascicles
|
bundles of muscle fibers
|
|
|
|
perimycium
|
loose and dense connective tissue that wraps each fascicle
|
|
|
|
epimycium
|
dense connective tissue that wraps around all of the fascicles
|
|
|
|
organ
|
bundles of parallel muscle fascicles
|
|
|
|
fascicle
|
bundles of parallel muscle fibers
|
|
|
|
Type I skeletal muscle fiber
|
SLOW OXIDATIVE
-small fibers -rich in mitochondria and myoglobin -slow-twitch, fatigue resistant -repetitive contraction |
|
|
|
Type IIa skeletal muscle fiber
|
FAST OXIDATIVE GLYCOLYTIC
-medium fibers -intermediate mitochondria and myoglobin -lots of glycogen storage -fast-twitch, fatigue resistant |
|
|
|
Type IIb skeletal muscle fiber
|
FAST GLYCOLYTIC
-large fibers -poor in mitochondria and myoglobin -fast-twitch, fatigue prone |
|
|
|
satellite cells
|
-stem cell population of skeletal muscle
-found under basement membrane |
|
|
|
actin and myosin
|
contractile proteins
|
|
|
|
A band
|
dark striations
|
|
|
|
I band
|
light striations
|
|
|
|
sarcomere
|
unit of muscle contraction
z line to z line |
|
|
|
thick filaments
|
stacked down the center of each sarcomere
create each A band |
|
|
|
thin filaments
|
interdigitate with the thick filaments
6 thin: 1 thick -only on I band |
|
|
|
H zone
|
region down the center of the A band where there is no overlap of thin and thick filaments
|
|
|
|
thick filament component
|
consists of many myosin molecules
|
|
|
|
thin filament components (3)
|
-actin
-tropomyosin -troponin |
|
|
|
actin
|
-contractile protein
-has binding sites for myosin heads |
|
|
|
tropomyosin
|
-actin-binding protein
|
|
|
|
troponin
|
-tropomyosin regulatory protein
-binding sites for Ca |
|
|
|
titin
|
protein that links thick filaments to Z line
|
|
|
|
alpha-actin
|
protein that links thin filaments to Z line
|
|
|
|
myomesin
|
protein that holds thick filaments in register
-creates M line |
|
|
|
sarcolemma function
|
-excitable membrane
-conducts action potential along surface of the cell |
|
|
|
Transverse tubules (T tubules)-where
|
-invaginations of the sarcolemma
-one at each A band/I band junction |
|
|
|
Transverse tubules (T tubules)-function
|
-excitable membrane
-conducts action potential into the interior of the cell |
|
|
|
sarcoplasmic reticulum (where)
|
-extends from t-tubule to t-tubule
-completely covers each myofibril |
|
|
|
sarcoplasmic reticulum (function)
|
-Ca storage (used for contraction)
-stored in the terminal cisternae |
|
|
|
terminal cisternae
|
-end "sacs"
-located at each end of the reticulum |
|
|
|
neuromuscular junction
|
point of innervation of each muscle fiber
|
|
|
|
motor end plate
|
neural side of the neuromuscular junction
|
|
|
|
terminal bouton
|
-presynaptic membrane
-neurotransmitter vesicles containing acetylcholine -covered by scwhann cell |
|
|
|
postsynaptic membrane
|
-at sarcolemma
-folded |
|
|
|
primary cleft
|
main cleft that runs along the presynaptic membrane
|
|
|
|
secondary synaptic cleft
|
spaces within the junctional folds
|
|
|
|
external lamina of neuromuscular junction
|
-runs along primary cleft and folds into each secondary cleft
-rich in acetylcholinesterase |
|
|
|
acetylcholine receptors
|
embedded within postsynaptic membrane
|
|
|
|
cardiac muscle cell characteristics
|
-NOT true synctia
-single nucleus, centrally located -fibers are cylindrical and short -branched - |
|
|
|
cardiac muscle regarded as...
|
"functional syncytium"
-cells are branched -specialized intercellular junctions -all contracts at the same time (heart beat) |
|
|
|
intercalated disks (functions-2)
|
1. adhere cells together
2. allows chemical and electrical communication |
|
|
|
intercalated disks (components-2)
|
1. transverse component
2. lateral component |
|
|
|
transverse component of intercalated disks
|
-designed for adhesion
-adherens junctions (zonula and macula adherens) |
|
|
|
lateral component of intercalated disks
|
-gap junctions-permits action potential to jump cells (electrical synapse)
|
|

