![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
87 Cards in this Set
- Front
- Back
|
What percentage of students had burnout mid-final year
|
28%
|
|
|
What percentage of interns had burnout 8 months in?
|
75%
|
|
|
What is the criteria for burnout?
|
Emotional exhaustion
Depersonalisation Lack of personal accomplishment |
|
|
What does stress management in medical education help with?
|
Reduced anxiety, distress and depression
Increased sensitivity to self and others Reduced perceptions of isolation ^use of positive coping skills ^ immune function ^knowledge of stress |
|
|
What is Primary Prevention?
|
Targeted at healthy individuals, aiming to stop disease progress before it has established
-Management of risk factors -Lifestyle modifications |
|
|
Why might primary prevention be difficult to initiate?
|
Because there is nothing wrong with a person and they feel it is unecessary to make a change when nothing is wrong
|
|
|
What is primordial prevention?
|
Inhibition of the emergence of a risk factor
-vaccines |
|
|
What is secondary prevention?
|
Aimed at slowing the process of a disease in order to avoid complications when its progression is well underway, but symptoms are yet to manifest.
-Lifestyle modification -Treatment of early stages |
|
|
What is tertiary prevention?
|
When a chronic disease is established and complications have emerged, prevention methods include rehab and avoidance of more complication
-Invasive and $$ |
|
|
What does essence stand for?
|
Education
Stress Management Spirituality Exercise Nutrition Connectedness Environment |
|
|
What is the Ornish program?
|
A program where patients followed a program consisting of this stuff as well as normal treatment
-group support -stress management programs -Low-fat, vegetarian diet (max 10% fat) -Moderate exercise -No Smoking |
|
|
What was the major factor of the ornish program which was central to improving health?
|
Stress management
|
|
|
how was the ornish program advantageous?
|
Less death, Less symptoms, greater fitness, more autonomy, better relationships
Better life quality |
|
|
What are enabling strategies?
|
Those which enable people to act on health advice and knowledge
-Goal setting, improving motivation |
|
|
What is motivational interviewing?
|
Motivational interviewing is a directive,
client-centered counseling style for eliciting behaviour change by helping clients to explore and resolve ambivalence.” |
|
|
What style of counselling is motivational interviewing?
|
Quiet and eliciting with a relationship more like a partner/companion one.
|
|
|
How does readiness to change come about? How consistent is it?
|
It is fluctuating and is a product of interpersonal interactions
|
|
|
What does BASK stand for
|
Behaviour
Attributes Skills Knowledge |
|
|
What is the BASK model used for?
|
Educational intervention and targets for behavioural change
|
|
|
Why is giving factual information potentially useless in eliciting change?
|
Because if the motivation isn't there and attitude is the main problem, facts aren't going to change the mind
|
|
|
What is the SMART goals framework?
|
A framework which helps to successfully set a goal
|
|
|
When might a goal in the SMART framework not be achieved?
|
When one or more steps are missed out
|
|
|
What does SMART stand for?
|
Specific
Measurable Attractive Realistic Timely |
|
|
What are the 6 stages of the prochaska-diclemente cycle of behavioural change?
|
1)Relapse
2)pre-contemplation 3)contemplation 4)preparation 5)Action 6) Maintainance |
|
|
Describe the 6 stages of the Prochaska-Diclemente cycle
|
1)RELAPSE-Don't view as failure but as an experience
2)PRE-CONTEMPLATION- before thoughts of change 3) CONTEMPLATION-start to think about behavioural change 4)PREPARATION- Preparing for change 5)ACTION-implementing change 6)MAINTENANCE- change becomes long-term and relatively effortless |
|
|
Why is it important to note which stage of the PDcycle a patient is in?
|
Inappropriate discussions meant for another phase can be off putting
|
|
|
Why is stress in modern life increasing and which gender shows the greatest increase?
|
Because of busy lives and less resilience
Males |
|
|
Why can chronic stress create mood problems
|
Because it reduces the levels of seratonin.
|
|
|
What will be the largest burden of disease in the next decade or so?
|
Mental Health
|
|
|
What are the health effects of chronic stress?
|
Symptoms-pain etc
Behaviour-bad lifestyle Resistance-immunity Disease-genetic expression |
|
|
When is the fight/flight response good and when is it bad?
|
Good- appropriately regulated and ellicited, not prolonged
Bad- prolonged and inappropriately activated |
|
|
How do men and women differ in their response to stress?
|
Men-fight/flight
Women- tend/befriend |
|
|
What is allostatic load?
|
The wear and tear on the body due to prolonged exposure to stress
|
|
|
What are some issues associated with allostatic load?
|
DNA degradation
neyrodegredation metabolic syndrome |
|
|
What is the theory behind the Psychoneuroimmunology?
|
That the mind and nervous system communicates with the immune system, effecting how efficient it is
|
|
|
What types of stress will activate and supress immunity?
|
Chronic Stress- Supress
Acute stress- activates |
|
|
How does stress and the perception of stress contribute to immune response
|
The way which a stressful event is perceived directly effects how prolonged the effects are
Increased rates of relapse of chronic conditions are related to increased stress |
|
|
How does Stress affect DNA?
|
^ DNA mutations
Decreased DNA repair rates Alters genetic expression ^ Genetic ageing ^ rate of telomere shortening and therefore ^ genetic age |
|
|
What is psychology?
|
The study of the mind, brain and behaviour
|
|
|
What is Health Psychology?
|
The relationship between psychological factors and health/illness
|
|
|
What is the biopsychosocial model
|
a conceptual model that assumes that psychological and social factors must also be included along with the biologic in understanding a person's medical illness or disorder.
|
|
|
What is the WHO definition of health?
|
Health is a state of complete medical, physical and social well-being and is not merely the absence of disease.
|
|
|
What are some factors which can influence how someone perceives their health?
|
Age,
Presence/absence of illness Energy Behaviour Psychosocial wellbeings Functionability |
|
|
Why is important in the medical profession
|
-Contributes to an understanding of how behaviour,emotion and cognition influence health
-Understand the development of people throughout life -Understand emotional disorders |
|
|
What is behaviour?
|
The manner in which something acts or reacts to a situation
|
|
|
Why is an understanding of behaviour relative to health?
|
We understand how it impacts on our health and on illnesses related to behaviour
|
|
|
What are common factors of the 5 leading causes of Australian deaths?
|
Behavioural risk factors
|
|
|
What is learning?
|
A relatively permanent change in behaviour which us a result of prior experience
|
|
|
What are the 4 elements of classical conditioning?
|
Unconditioned Stimulus
Unconditioned response Conditioned stimulus Conditioned response |
|
|
What are the unconditioned stimuli and responses in classical conditioning
|
-Stimulus which innately produces a response
-Response produced by the UCS |
|
|
What are the conditioned stimuli and responses in classical conditioning?
|
-Stimulus produces the conditioned response after repeated coupling with the unconditioned stimulus
|
|
|
What is operant conditioning?
|
When the consequences immediately following a behaviour will determining whether or not it is repeated
STIMULUS>>>RESPONSE>>>CONSEQUENCE |
|
|
What is reinforcement in terms of operant conditioning?
|
A consequence that increases chances of a behaviour being repeated
|
|
|
What is punishment in terms of operant conditioning?
|
A consequence that decreases the chances of behaviour being repeated
|
|
|
Describe the influences of +ve/-ve punishment/reinforcement in operant conditioning
|

|
|
|
What effects the strength of reinforcement/punishment of a behaviour after it has been elicited?
|
-How soon after the behaviour it occurred
-The size and strength of the reaction |
|
|
What are the differences between Classical conditioning and Operant conditioning?
|
Types of behaviour- CC response elicited and OC response emitted
Associations-CC associates with stimulus, OC associates with consequence Order of event. CC- learning association comes before response. OC comes after |
|
|
What are superstitious behaviours and when do they occur
|
Behaviours unrelated to a response which are used to repeat/avoid outcomes. Occurs when an event occurs in close proximity to an independant behaviour
|
|
|
Describe elements of the Social Cognitive Theory
|
We think about experiences and try to understand them
Not all learning occurs via conditioning and can be initiated by observed behaviours |
|
|
Which behaviours are most likely to be imitated?
|
Those of a competent model
|
|
|
What is illness behaviour?
|
The process of a person going from well to sick
|
|
|
What are the 4 elements of the 'sick role'
|
-Excused from responsibilities
-Not held responsible -Wants to get better -Co-operates with advice |
|
|
Other than biological influences, why are there variations in the health of those with the same illnesses?
|
The different ways people cope with illness influence how healthy they are
|
|
|
What is cognition?
|
All of the mental process we use.
|
|
|
What is a rational choice?
|
One that is based on the perceived probability of the occurrence of options
|
|
|
What is the formula of behaviour relating to expectancy-value theories?
|
Behaviour= Value x Expectancy
|
|
|
In regards to the expectancy/value model, when is behavioural change most likely?
|
When the combination of expectancy and value numbers are high
|
|
|
What are heuristics? Give an example
|
Problem solving strategies that are based on general rules that usually work
-symmetry rule: symptom= illness, no symptoms =no illness -Reasoning by analysis: Decisions based on what worked in the past |
|
|
What are some heuristics used in a clinical setting?
|
Representativeness- Decisions based on the assumption that an event is representative of an entire category of events.
Availability- Decisions based on the availability of information |
|
|
Why are heuristics not always effective
|
N'ASSUMEZ RIEN
There is always something else to a person outside of a model |
|
|
What is an algorithm?
|
A mechanical routine/formula/rules that can be used to solve all problems of a specific type
|
|
|
What is an example of an algorithm in medicine?
|
Differential diagnosis: Identify disease possbilities
Biomedical theories: Cause =symptom |
|
|
What is a major influence on health behaviour?
|
Thoughts on health.
Those people who's behaviours change have a different set of thoughts than those who do not |
|
|
What is the common sense model?
|
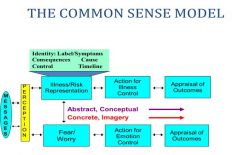
A model which is used in identifying the content of health threat representations and for understanding how thoughts and associated emotions motivate protective behaviour
|
|
|
What are 5 attributes of health threat representations?
|
IDENTITY: lable, symptoms
CAUSE TIMELINE: onset, duration CONSEQUENCES: Outcomes CONTROL/CURE: Meds, preventions |
|
|
Why do health threat representations influence how people cope with illness?
|
They elicit emotion
Can be concrete or abstract elements making things confusing |
|
|
How is imagery advantageous in influencing health behaviour?
|
-It's processed faster
-Its remembered better -Has a greater affect -Shows a more concrete future (cause/effect) |
|
|
What are expectations?
|
A set of cognitions about what is likely to happen given a particular situation
|
|
|
What is the balance theory?
|
Suggestions that balance is when all of our cognitions are in accordance with the other
|
|
|
Why is balance important in expectations?
|
Moderate and realistic expectations, that have more balanced sets of cognitions show better outcomes
|
|
|
What is a placebo?
|
The non-specific effects produced by a treatment
|
|
|
What is a placebo effect?
|
When people respond to inert treatments. Often elicited by expectations
|
|
|
What is the wonder drug effect?
|
The tendency for treatments to work best while they're new to the market
|
|
|
What are the psychologicaland pysiological explanations of placebo effects during treatment
|
PSYCHOLOGICAL.
Conditioning- prior good experience Perceptions Validation- HCW gives warranted treatment PHYSIOLOGICAL Reduced stress Endorphin release- pain reduced psychoneuroimmunology- changed perception influences immunity |
|
|
How can health professionals act as a placebo?
|
-Validate the sense that something is wrong
-Mobilise patient resources Both reduce stress and give clear thinking |
|
|
What are some criticisms of the prochaska-diclemente model of change
|
There are fuzzy borders between stages of change
|
|
|
In reference to the P-D model of change, when is there a higher level of change following treatment?
|
When the stage of change is further into the cycle
|

