![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
35 Cards in this Set
- Front
- Back
|
Which two species of bacteria can form endospores? |
Bacillus and Clostridium |
|
|
Endospores |
A heat resistant cell wall structure that can allow the organisms to lay dormant for long periods of time |
|
|
Vegi Cell |
Normally growing cell that forms the endospore |
|
|
Why heat the malachite green stain? |
Heat is needed for the malachite green stain to force the dye into the endospore |
|
|
What color is an endospores former? |
Green with some red vegi cells |
|
|
List endospore stain procedure |
-Smear bacteria (heat fix etc) -Place oval piece of paper towel over slide -Flood slide with malachite green -Heat/steam slide for 5mins (with applicator stick -Let cool -Remove paper towel and rinse well with water -Safranin counter stain (1min) -Rinse and blot |
|
|
How is clinical different from classical? |
Clinical performs multiple tests with one media while classical IDs unknowns with specific biochemical tests |
|
|
Classical microbiology method steps |
-Achieve pure culture -Gram stain -Biochemical characterization tests -Compare results |
|
|
Clinical microbiology method steps |
-Create list of suspects based on symptoms and location of infection -Streak for isolation using differential/selective media -Identify suspicious colony -Conduct gram stain and additional test |
|
|
Selective media |
Media that contains ingredients that inhibit the growth of a certain group of bacteria ex: gram positive bacterium does not grow on MacConky due to bile salts |
|
|
Differential media |
Media that contains ingredients that provide biochemical information ex: pH indicator |
|
|
What type of bacteria is MacConky used for? (in clinic setting?) |
Isolates Salmonella and Shigella (Stool samples) |
|
|
What type of bacteria is EMB used for? (Clinical setting) |
Fecal coliform bacteria |
|
|
MacConky interpretation (When IDing) |
pH indicator: Ferments lactose - Red/pink (less than 6.8 pH)
pH indicator: Does not ferment lactose: yellow (above pH 8)
Inhibitor: Growth - Gram negative (not Staph)
Inhibitor: No growth - Gram positive (Staph) |
|
|
EMB characteristics when IDing |
pH indicator: (Strong fermenters) Ferments Lactose - Metallic green or black pH indicator: (Weak fermenters) Does not ferment lactose - Pink/purple Inhibitor: Growth - Not gram positive Inhibitor: No growth - (probably) gram positive |
|
|
MacConky ingredients |
- Lactose and neutral red (pH indicator) - Crystal Violet and bile salts (inhibitor) |
|
|
Eosin Methylene Blue (EMB) ingredients |
- Sucrose and Lactose - Eosin and Methylene blue (pH indicator and inhibitor) |
|
|
Mannitol salt agar (MSA) ingredients |
- High salt 7.5% (inhibitor) - Mannitol (carb/sugar) with pH indicator phenol red |
|
|
MSA characteristics |
Growth: Haloduric (high salt tolerant organisms) No growth: Does not tolerate salt Pink/yellow color: Ferments mannitol Red color: Does not ferment mannitol |
|
|
Blood agar ingredients |
- 5% Sheep red blood cells - TSA |
|
|
Blood agar characteristics (when IDing) |
- Clearing around colonies: Produces betahemolysins Greenish halo around colonies: Produces AlphaHemolysins |
|
|
Evidence of S. aureus after tests? (The results) |
-Gram positive (Purple cocci) -Catalase positive (Bubbles) -Ferments mannitol (Yellow/pink) -Salt tolerate (Grows on MSA) -Beta hemolytic (Clearing around colonies) -Congulase positive -Meduim sized gold (On MSA) |
|
|
Describe beta hemolysis on BA (Blood agar) |
Clearing around colonies |
|
|
Describe alpha hemolysis on BA (blood agar) |
A greenish halo around the colony (It is not completely dissolving the RBC membranes) |
|
|
What does a staph suspicious colony look on MacConky and EMB? |
No growth, MacConky and EMB inhibits growth of gram positive organisms |
|
|
What does a staph suspicious colony look like on MSA? |
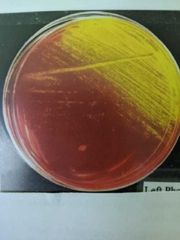
Yellow/Pink because it ferments mannitol and is salt tolerant |
|
|
What does a staph suspicious colony looked like on BA? (Blood agar) |
There will be a clearing around the colonies |
|
|
What does staph look like after coagulase test? |
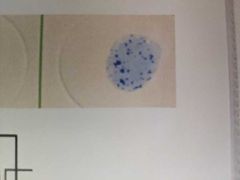
Small blue clots in reagent |
|
|
Four mechanisms by which bacteria become resistant to antibiotics |
1) Chromosomal mutation that causes a change in the structure of the drug binding site. (Drug can't bind) 2) Chromosomal mutation that causes a change in membrane permeability. (Drug can't enter the cell) 3) Acquisition of a gene that enables the bacterium to produce an enzyme that destroys the drug. (Drug is destroyed or inactivated) 4) Acquisition of a gene that enables the bacterium to produce an MDR (multiple drug resistance) pump. (The drug is pumped out of the cell before it can have an effect) |
|
|
Five different modes of action of antibiotics |
1) inhibition of cell wall synthesis 2) inhibition of protein synthesis 3) inhibition of enzyme activity 4) injury to cell membrane 5) inhibition of DNA synthesis |
|
|
Name one example antibiotic for inhibition of cell wall synthesis |
1) Penicillin, methicillin, amoxicillin, cephalosporins, cephamycins (beta-lactam antibiotics) 2) Bacitracin 3) Vancomycin 4) Carbapenmes |
|
|
Name one example of an antibiotic that inhibits protein synthesis |
1) tetracycline 2) streptomycin 3) Gentamicin 4) Kanamycin 5) Erythromycin 6) Chloramphenicol 7) Ketolides/Macrolides = Azithromycin |
|
|
Name one example for an antibiotic that inhibits enzyme activity |
1) Sulfonamides 2) Trimethoprim |
|
|
Name one antibiotic example that injures cell membrane |
1) Polymyxins 2) Nystatin |
|
|
In one example of an antibiotic that inhibits DNA synthesis |
1) Ciprofloxacin (Fluoroquinolones) 2) Norfloxacin (Quinolones) |

