![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
41 Cards in this Set
- Front
- Back
|
What are the 3 basic functions of the liver in glucose metabolism?
|
1. Store glucose
2. Breakdown glucose 3. Make glucose from other organic molecules |
|
|
What is the name of the biochemical process the liver utilizes when storing glucose?
|
Glycogen synthesis
|
|
|
Name the enzyme responsible for “trapping” glucose within hepatocyts:
|
glucose-6-phosphatase
|
|
|
What chemical reaction does glucose-6-phosphatase catalyze?
|
Glucose → glucose-6-phosphate
|
|
|
What structural arrangement is glucose stored as glycogen?
|
Glycogen is arranged in a tree-like branching structure
|
|
|
Name the glucose linkages that give glycogen it’s branching structure:
|
a-1,4 linkage and a-1,6 linkage
|
|
|
What tissues/ organs rely on the liver storage of glucose?
|
RBC, retina, renal medulla and brain
|
|
|
Why do RBCs, the retina, the renal medulla and the brain rely on liver stores of glucose?
|
These tissues do not have the capacity to store their own metabolic fuel
|
|
|
What is the name of the biochemical process the liver utilizes to produce chemical energy in the form of ATP from glucose?
|
Glycolysis
|
|
|
What are the chemical products of glycolysis?
|
Glucose → 2 ATP + pyruvate
|
|
|
Describe the branching pattern of glycogen:
|
Glucose monomers are linked together by -1,4 glycosicic bonds, with β-1,6-glycosidic branching occurring approximately every 10 units.
|
|
|
What is the significance of glycogen’s branched structure?
|
Branching increases the solubility of glycogen, and it also increases the rate at which glucose can be stored and mobilized from glycogen.
|
|
|
What organs are dependent on glucose as their fuel source; where is this store located and in which form?
|
The erythrocytes, retina, renal medulla, and brain are dependent on glucose for fuel, the liver and muscle both store glycogen as a reserve for these organs.
|
|
|
True or false: the breakdown of glucose into pyruvate requires energy derived from ATP?
|
True.
The catabolic enzyme hexokinase requires ATP to create one G6P from each glucose molecule. |
|
|
What is the starting point for glycolysis, what is the end product and what will happen to it next.
|
Glucose
Pyruvate Citric Acid Cycle |
|
|
What is the Cori Cycle?
|
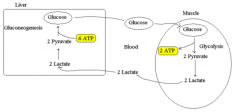
|
|
|
What is the name of the biochemical process the liver utilizes to produce glucose from of the organic substrates?
|
Gluconeogenesis
|
|
|
What organic substrates can be used in gluconeogenesis?
|
Pyruvate, amino acids, lactate
|
|
|
Describe the Cori cycle:
|
muscle lactate produced by anaerobic metabolism → transported to liver hepatocytes via blood → lactate is converted to glucose via gluconeogenesis → glucose is transported to muscles → repeat
|
|
|
What is ammonia?
|
Metabolic waste product from amino acid metabolism
|
|
|
How is ammonia produced?
|
When an amino group is released from an amino acid
|
|
|
What is the chemical formula for ammonia?
|
NH3
|
|
|
What organ removes ammonia in the body?
|
The liver
|
|
|
How is ammonia removed from the body?
|
Ammonia is combined with CO2 to produce urea (NOTE: there are several steps, substrates and enzymes involved in this process)
|
|
|
What are the advantages of converting ammonia into urea?
|
Urea is non-toxic and water-soluble
|
|
|
What is the advantage of urea being water-soluble?
|
Urea can be excreted via the kidneys
|
|
|
Describe the production of unconjugated billirubin:
|
1. With in phagocytes RBC are digested
2. Heme is released from RBC 3. Heme → Biliverdin (releasing iron and CO) via Heme oxygenase 4. Biliverdin → Bilirubin (water insoluble) via biliveriden reductase 5. Bilirubin binds to albumin and transported in the blood |
|
|
Describe the production of conjugated bilirubin:
|
1. Unconjugated bilirubin → travel to sinusoid capillaries of liver → free bilirubin enter hepatocyte
2. Free bilirubin → bind to ligandin (prevent diffusing out of cell) 3. Bilirubin → conjucation with glucuronic acid via glucuronyl transferase 4. Conjugated bilirubin → bile via energy dependent excretion |
|
|
Describe the production and fate of urobilinogen:
|
1. Conjugated bilirubin in bile → urobilinogen via intestinal bacteria
2. Urobilinogen absorbed into portal circulation or excreted as feces 3. Urobiligen → liver (excreted as bile again) or kidney (excreted in urine) |
|
|
Describe the fate of urobilinogen excreted as feces:
|
1. Urobiligen → stereobilinogens via bacteria
2. Stereobilinogen → stercobilins via oxidation |
|
|
What process in the body generates ammonia?
|
Amino acid catabolism releases amino groups which form ammonia.
|
|
|
How does the body deal with the ammonia it creates?
|
The primary mechanism for converting neuro-toxic ammonia into urea is through the hepatic urea cycle.
|
|
|
How might you treat acute hyperammonemia?
|
Hemodialysis or exchange trasfusions to lower the blood ammonia level.
|
|
|
What lifestyle management schemes might you recommend to your patient who suffers from hyperammonia?
|
Decrease dietary protein intake.
|
|
|
You are a CC-3 on your pediatric rotation when you see a neonate presenting with mental retardation and convulsions. Your are a ken reviewer and had recetly looked over your GI-4 notes, what from GI-4 would you include in you DDx?
|
A genetic deficiency in the urea cycle enzymes, inducing an ammonia toxicity, this X-linked trait are known to occur at a rate of 1/25000 live births.
|
|
|
Define Bilirubin.
|
Bilirubin is the yellow breakdown product of heme produced by the reticuloendothelial system.
|
|
|
What are the components of the reticuloendothelial system?
|
Spleen
Kupffer Cells Bone Marrow Connective Tissue Lymph Nodes |
|
|
What is the function of the reticuloendothelial system?
|
To recognize aging erythrocytes and to break them down into heme and globin.
|
|
|
What is the result of a UDP-glucuronyl transferase deficiency?
|
Bilirubin would remain uncongugated and which would present as intrahepatic induced jaundice.
|
|
|
What is Gilbert’s Syndrome?
|
Gilbert's syndrome is caused by approximately 30%-50% reduced glucuronidation activity of the enzyme UDP-glucuronyl transferase and presents as jaundice with elevated serum unconjugated bilirubin
|
|
|
What is enterohepatic circulation of bilirubin?
|
Conjugated bilirubin is converted by intestinal flora to urobinogen which is mostly absorbed in the terminal ileum and re-excreted by the liver, some is eliminated I the feces.
|

