![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
5 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Pathogenesis of subcutaneous mycoses |
1.Fungi is introduced to skin via trauma 2.development of local lesion (pastule,abscess,ulcer ) 3.moves to the lymphatic system 4.lymphatic system becomes thickened and cord like 5.multiple abscess occurs along the lymphatic |

|
|
|
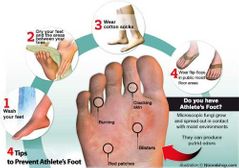
How to avoid tinea infection |
1.Expose the skin to air as much as possible 2.Wear cotton sock instead of synthetics 3.Clean shower 4.Wear thogs 5.Don't share towels 6.Don't walk bare foot of if you have tinea pedis
|
|
|
|
Mention tinea management pitfalls |
Don't use nystatin since dermatophyte are resistant to it Don't use oral ketoconazole due to hepatotoxicity(cyp450 inhibitor) Don't use combination of methadisone and clotrimazole it increase infection Don't treat unconfirmed tinea capitis Don't use griseofulvin |

Refer to microbiology notes slide 28 |
|
|
Coccidiodes immitis |
Coccidiodes immitis is the soil fungi They form cotton colony in saboaurad agar Most common in southern USA and Latin america Pathogenesis Is due to two antigens 1.spherulin 2.coccidiodin These antigen are also used in test The disease in airborne First it invade the 🫁 followed by asymptomatic phase 1%of infection may disseminate and cause lesion like TB CLINICAL FEATURES 1.fever 2.ache 3.malaise 4.cough 5.valley fever LABORATORY FINDINGS 1.microscopy presence of spherulin 2.culture subauraud agar is used 3.innoculation to animal such as mice 4.serology 5.skin test |
|
|
|
Wewe ni nani |
Mimi ni awena masoud nassoro |
|

