![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
166 Cards in this Set
- Front
- Back
|
How do you diagnose infection with HSV?
|
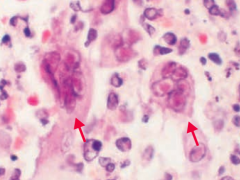
- Viral culture for skin / genitalia |
|
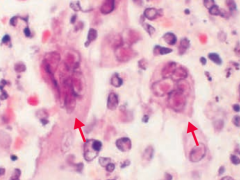
What does this image show? Sign of?
|
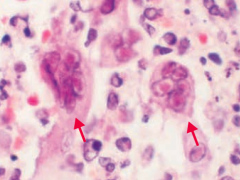
Positive Tzanck smear in genital herpes (HSV-2)
|
|
|
What are the types of RNA viruses?
|

- Reovirus
- Picornavirus - Hepevirus - Calicivirus - Flavivirus - Togavirus - Retrovirus - Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which RNA viruses are enveloped?
|

*Enveloped |
|
|
Which RNA viruses are not enveloped?
|

* Not enveloped
* Reovirus * Picornavirus * Hepevirus * Calicivirus - Flavivirus - Togavirus - Retrovirus - Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which RNA viruses are DS?
|

DS = *
* Reovirus - linear (10-12 segments) - Picornavirus - Hepevirus - Calicivirus - Flavivirus - Togavirus - Retrovirus - Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which viruses are (+) linear ssRNA?
|

+ssRNA = *
- Reovirus * Picornavirus * Hepevirus * Calicivirus * Flavivirus * Togavirus * Retrovirus * Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which viruses are (-) linear ssRNA?
|

(-) ssRNA, linear = *
- Reovirus - Picornavirus - Hepevirus - Calicivirus - Flavivirus - Togavirus - Retrovirus - Coronavirus * Orthomyxovirus * Paramyxovirus * Rhabdovirus * Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which viruses are (-) circular ssRNA?
|

(-) ssRNA, circular
- Reovirus - Picornavirus - Hepevirus - Calicivirus - Flavivirus - Togavirus - Retrovirus - Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus * Arenavirus * Bunyavirus * Delta virus |
|
|
Which RNA viruses are icosahedral?
|

* Reovirus
* Picornavirus * Hepevirus * Calicivirus * Flavivirus * Togavirus * Retrovirus - Coronavirus - Orthomyxovirus - Paramyxovirus - Rhabdovirus - Filovirus - Arenavirus - Bunyavirus - Delta virus |
|
|
Which RNA viruses are helical?
|

- Reovirus
- Picornavirus - Hepevirus - Calicivirus - Flavivirus - Togavirus - Retrovirus * Coronavirus * Orthomyxovirus * Paramyxovirus * Rhabdovirus * Filovirus * Arenavirus * Bunyavirus * Delta virus |
|
|
What are the types of Reoviruses?
|
- Coltivirus
- Rotavirus |
|
|
What is the #1 cause of fatal diarrhea in children?
|
Rotavirus (Reovirus - no envelope, DS linear, icosahedral (double))
|
|
|
What is the medical importance of the Coltivirus?
|
- Causes Colorado Tick Fever
- Type of arbovirus - transmitted by arthropods (ticks) - Reovirus - no envelope, DS linear (10-12 segments), icosahedral (double) |
|
|
What is the medical importance of the Rotavirus?
|
- #1 cause of fatal diarrhea in children
- Reovirus - no envelope, DS linear (10-12 segments), icosahedral (double) |
|
|
What are the types of Picornaviruses?
|
PERCH:
- Poliovirus - Echovirus - Rhinovirus - Coxsackievirus - HAV |
|
|
What is the medical importance of the Poliovirus?
|
Causes Polio
- Salk (killed / injected) and Sabin (live attenuated / oral) vaccines - Picornavirus (no envelope, SS (+) linear, icosahedral) |
|
|
What is the medical importance of the Echovirus?
|
Causes aseptic meningitis
- Picornavirus (no envelope, SS (+) linear, icosahedral) |
|
|
What is the medical importance of Rhinovirus?
|
"Common cold"
- Picornavirus (no envelope, SS (+) linear, icosahedral) |
|
|
What is the medical importance of the Coxsackievirus?
|
- Aseptic meningitis
- Herpangina (mouth blisters, fever) - Hand, foot, and mouth disease - Myocarditis and pericarditis - Picornavirus (no envelope, SS (+) linear, icosahedral) |
|
|
What is the medical importance of the HAV?
|
Causes Acute Viral Hepatitis
- Picornavirus (no envelope, SS (+) linear, icosahedral) |
|
|
What is the medical importance of the Hepevirus family?
|
- Hepatitis E Virus (HEV)
- No envelope, SS (+) linear, icosahedral |
|
|
What is the medical importance of the Calicivirus family?
|
Norovirus - viral gastroenteritis
- No envelope, SS (+) linear, icosahedral |
|
|
What are the types of Flaviviruses?
|
- HCV
- Yellow Fever - Dengue Fever - St. Louis Encephalitis - West Nile Virus |
|
|
What are the characteristics of Flaviviruses?
|

- Envelope
- SS (+) linear - Icosahedral |
|
|
What is the medical importance of Togaviruses? Characteristics?
|

- Rubella
- Eastern equine encephalitis - Western equine encephalitis - Envelope, SS(+) linear, Icosahedral |
|
|
What is the medical importance of Retroviruses? Types? Characteristics?
|

- Have reverse transcriptase
- HIV: AIDS (complex and conical) - HTLV: T-Cell Leukemia (icosahedral) - Enveloped, SS (+) Linear |
|
|
What is the medical importance of Coronaviruses? Characteristics?
|

- Common cold
- SARS - Envelope, SS (+) linear, Helical |
|
|
What is the medical importance of Orthomyxoviruses? Characteristics?
|

Influenza Virus
- Envelope - SS (-) Linear (8 segments) - Helical |
|
|
What is the medical importance of Paramyxoviruses? Characteristics?
|

PaRaMyxovirus:
- Parainfluenza = Croup - RSV = bronchiolitis in babies, rx = ribavirin - Measles - Mumps - Envelope, SS (-) linear (non-segmented), helical |
|
|
What does RSV cause? Treatment? Characteristics?
|

- Causes bronchiolitis in babies
- Treat with Ribavirin - Paramyxovirus: enveloped, SS (-) linear (non-segmented), helical |
|
|
What is the medical importance of Rhabdoviruses? Characteristics?
|

Rabies
- Envelope - SS (-) linear - Helical |
|
|
What is the medical importance of Filoviruses? Characteristics?
|

Ebola / Marburg hemorrhagic fever (often fatal)
- Envelope - SS (-) linear - Helical |
|
|
What is the medical importance of Arenaviruses? Characteristics?
|

- LCMV: Lymphocytic Choriomeningitis Virus
- Lassa Fever Encephalitis (spread by mice) - Enveloped, SS (-) Circular (2 segments), Helical |
|
|
What is the medical importance of Bunyaviruses? Characteristics?
|

- California encephalitis
- Sandfly / Rift Valley fevers - Crimean-Congo hemorrhagic fever - Hantavirus - hemorrhagic fever, pneumonia - Enveloped, SS (-) circular (3 segments), helical |
|
|
What is the medical importance of Delta Virus? Characteristics?
|

- HDV: defective virus that requires HBV co-infection
- Enveloped, SS (-) circular, uncertain capsid symmetry |
|
|
What are the negative stranded viruses? What do they require?
|
Always Bring Polymerase Or Fail Replication
- Arenaviruses - Bunyaviruses - Paramyxoviruses - Orthomyxoviruses - Filoviruses - Rhabdoviruses Must transcribe (-) strand to (+) - Virion brings its own RNA-dependent RNA polymerase |
|
|
What are the segmented viruses? How many segments?
|
All are RNA viruses: BOAR
- Bunyaviruses: 3 segments - Orthomyxoviruses (influenza): 8 segments - Arenaviruses: 2 segments - Reoviruses: 10-12 segments |
|
|
What are the Picornaviruses?
|
PERCH on a "Peak" (PICO)
- Poliovirus - Echovirus - Rhinovirus - Coxsackievirus - HAV |
|
|
What is unique about Picornaviruses?
|
- Small RNA virus
- RNA is translated into 1 large polypeptide that is cleaved by proteases into functional viral proteins - Can cause aseptic (viral) meningitis (except Rhinovirus and HAV) - All are enteroviruses (fecal-oral spread) except rhinovirus |
|
|
What are the characteristics of Rhinovirus? What does it cause?
|
Picornavirus - non-enveloped RNA virus
- Cause of common cold - > 100 serologic types - Acid labile (destroyed by stomach acid) therefore does not infect the GI tract (unlike other picornaviruses) |
|
|
What family of virus is Yellow Fever Virus? How is it transmitted? Symptoms?
|
Flavivirus (also an arbovirus - transmitted by Aedes mosquitos)
- Virus has a monkey or human reservoir - Symptoms: high fever, black vomitus, and jaundice |
|
|
Which virus causes high fever, black vomitus, and jaundice?
|
Yellow Fever Virus (type of flavivirus)
|
|
|
What is the most important global cause of infantile gastroenteritis? Characteristics?
|
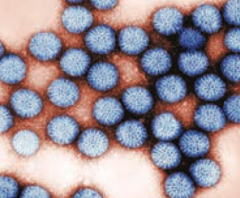
Rotavirus = Right Out The Anus
- Type of Reovirus - Segmented dsRNA virus - Major cause of acute diarrhea in US during winter, especially at day-care centers, kindergartens |
|
|
What is the mechanism of action of Rotavirus? Implications?
|
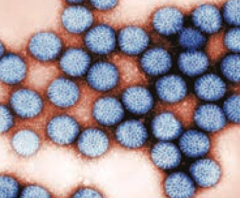
- Villous destruction with atrophy leads to decreased absorption of Na+ and loss of K+
- Major cause of acute diarrhea in Us during winter, especially in day-care centers and kindergartens - CDC recommends routine vaccination of all infants |
|
|
What type of virus is Influenza Virus? Characteristics?
|
Orthomyxovirus
- Enveloped - (-) ssRNA w/ 8-segment genome - Rapid genetic gchanges |
|
|
What antigens are on influenza viruses? Actions?
|
- Hemagglutinin - promotes viral entry
- Neuraminidase - promotes progeny virion release |
|
|
Which protein on influenza virus promotes viral entry?
|
Hemagglutinin
|
|
|
Which protein on influenza virus promotes progeny virion release?
|
Neuraminidase
|
|
|
Patients infected with the influenza virus are at risk for what?
|
Fatal bacterial superinfection
|
|
|
What are the types and characteristics of the influenza vaccines?
|
- Reformulated vaccine ("the flu shot" contains the viral strains most likely to appear during the flu season
- Killed viral vaccine (injected) most commonly used - Live attenuated (temperature sensitive) vaccine that replicates in the nose but not in the lung is administered intranasally |
|
|
What are the types of genetic changes to the influenza vaccine? Which is more serious?
|
- Genetic shift / antigenic shift
- Genetic drift Sudden Shift is more deadly than graDual Drift |
|
|
What does genetic SHIFT of influenza viruses cause?
|
Pandemics
- Reassortment of viral genome - Segments undergo high-frequency recombination, such as when human flu A virus combines with swine flu A virus |
|
|
What does genetic DRIFT of influenza viruses cause?
|
Epidemics
- Minor (antigenic drift) changes are based on random mutation |
|
|
What kind of virus is Rubella? What disease does it cause?
|
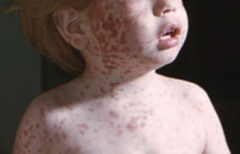
Togavirus
- Causes rubella, aka German (3-day) Measles - Fever, postauricular and other lymphadenopathy, arthralgias and fine rash - Mild disease in children, but severe congenitally |
|
|
What are the impacts of Rubella (togavirus) if acquired congenitally?
|
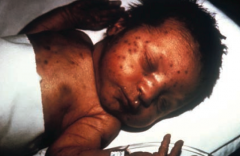
Serious congenital disease (a ToRCHeS infection):
- Blueberry muffin appearance indicates extramedullary hematopoiesis |
|
|
What are the types of Paramyxoviruses?
|
- Parainfluenzae
- Mumps - Measles - RSV |
|
|
Which virus causes croup - seal-like barking cough?
|
Parainfluenza (type of paramyxovirus)
|
|
|
Which virus causes respiratory tract infections (bronchiolitis, pnuemonia) in infants?
|
RSV (type of paramyxovirus)
|
|
|
What are the characteristics of all paramyxoviruses?
|
- Contain surface F (fusion) proteins
- F protein causes respiratory epithelial cells to fuse and form multinucleated cells |
|
|
Which drug can prevent pneumonia caused by RSV infection in premature infants? Mechanism?
|
Palivizumab - monoclonal antibody against F protein
|
|
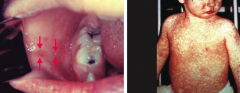
Which virus causes Koplik spots (left) and a descending maculopapular rash (right)
|
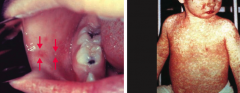
Measles virus (a paramyxovirus)
|
|
|
What are the characteristic symptoms of Measles infection?
|
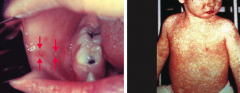
- Koplik spots - bright red spots with blue-white center on buccal mucosa that precedes measles rash by 1-2 days (left)
- Descending maculopapular, erythematous rash that includes limbs (right) 3 "C's" of measles: - Cough - Coryza (inflammation of nose) - Conjunctivitis |
|
|
What are the possible sequelae of Measles infection?
|
- SSPE: Subacute Sclerosing Panencephalitis (occurs years later)
- Encephalitis (1:2000) - Giant cell pneumonia (rarely, in immunosuppressed) |
|
|
What can be used to prevent severe exfoliative dermatitis in malnourished children with Measles?
|
Vitamin A
|
|
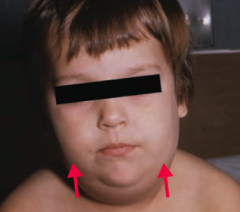
Which virus causes Parotitis (picture), Orchitis (inflammation of testes), and aseptic Meningitis?
|
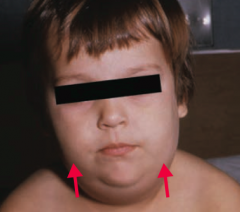
Mumps virus (a type of paramyxovirus)
|
|
|
What are the symptoms of Mumps?
|
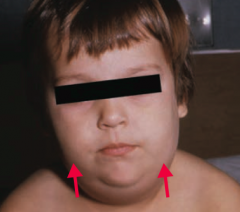
Mumps makes your parotid glands and testes as big as POM-poms
- Parotitis (picture) - Orchitis (inflammation of testes) - Aseptic Meningitis - Can cause sterility (especially after puberty) |
|
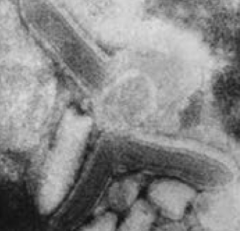
Which virus is bullet-shaped?
|
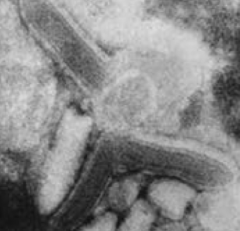
Rabies virus
|
|
|
What cells are affected by the Rabies virus?
|
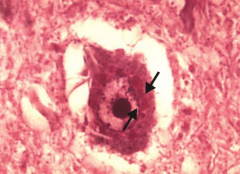
Rabies virus characteristically infects Purkinje cells of the cerebellum and neurons in the hippocampus
- Cytoplasmic inclusions = Negri body (arrows) |
|
|
What are the symptoms of Rabies Virus?
|
- Long incubation period (weeks to months) before onset of symptoms
- Progression of disease: fever, malaise → agitation, photophobia, hydrophobia → paralysis, coma → death |
|
|
From which animals is it more common to acquire Rabies virus?
|
Bat, raccoon, and skunk bites more common than dog bites in US
|
|
|
What is the pathophysiology of Rabies virus?
|
Virus travels to the CNS (Purkinje cells of cerebellum and hippocampal neurons) by migrating in a retrograde fashion up nerve axons
|
|
|
How should you treat a patient you think may be exposed to Rabies virus?
|
- Wound cleansing
- Vaccination +/- rabies immune globulin |
|
|
What are the types of Hepatitis viruses? Virus family? DNA/RNA?
|
- HAV: RNA picornavirus
- HBV: DNA hepadnavirus - HCV: RNA flavivirus - HDV: RNA delta virus - HEV: RNA hepevirus |
|
|
How are the Hepatitis viruses transmitted?
|
- HAV: fecal-oral
- HBV: parenteral, sexual, maternal-fetal - HCV: primarily blood (IVDU, post-transfusion) - HDV: parenteral, sexual, maternal-fetal - HEV: fecal-oral, especially with waterborne epidemics * HAV and HEV: the vowels hit your bowels |
|
|
What are the signs and symptoms of ALL hepatitis viruses?
|
- Episodes of fever
- Jaundice - ↑ ALT and AST |
|
|
Which Hepatitis viruses require a carrier?
|
HBV, HCV, HDV
|
|
|
What is the relative incubation time for the Hepatitis viruses?
|
- HAV: short (weeks)
- HBV: long (months) - HCV: long - HDV: superinfection (HDV after HBV) is short - HDV: co-infection (HDV with HBV) is long - HEV: short |
|
|
Which Hepatitis viruses have risk for progressing to hepatocellular carcinoma? How?
|
- HBV (integrates into host genome, acts as oncogene
- HCV (from chronic inflammation) - HDV |
|
|
What are the characteristics of HAV?
|
- RNA picornavirus
- Fecal-oral transmission - No carrier - Short incubation time (weeks) - No risk for HCC - Usually "A"symptomatic, "A"cute, "A"lone (no carrier) |
|
|
What are the characteristics of HBV?
|
- DNA hepadnavirus
- Parenteral, sexual, or maternal-fetal transmission - Carrier - Long incubation time (months) - Risk for HCC (integrates into host genome and acts as oncogene) - DNA polymerase has both DNA- and RNA-dependent activities; upon entry into nucleus the polymerase functions to complete the partial dsDNA - The host RNA polymerase transcribes mRNA from viral DNA to make proteins - DNA polymerase then reverse transcribes viral RNA to DNA which helps form new viral particles |
|
|
What are the characteristics of HCV?
|
- RNA flavivirus
- Primarily transmitted via blood (IVDU, post-transfusion) - Carrier - Long incubation time - Risk of HCC (from chronic inflammation) - "C"hronic, "C"irrhosis, "C"arcinoma, "C"arrier |
|
|
What are the characteristics of HDV?
|
- RNA delta virus
- Parenteral, sexual, or maternal-fetal transmission - Carrier - Superinfection (HDV after HBV) has short incubation time - Co-infection (HDV with HBV) has long incubation time - Risk for HCC - "D"efective virus "d"ependent on HBV superinfection → ↓ prognosis |
|
|
What are the characteristics of HEV?
|
- RNA hepevirus
- Fecal-oral transmission, especially with waterborne epidemics - No carrier - Short incubation time - No risk for HCC - High mortality in pregnant women - "E"nteric, "E"xpectant mothers, "E"pidemic |
|
|
What does it mean if your patient has anti-HAV (IgM)?
|
Best test to detect active Hepatitis A infection
|
|
|
What does it mean if your patient has anti-HAV (IgG)?
|
Indicates prior HAV infection and/or prior vaccination; protects against re-infection
|
|
|
What does it mean if your patient has HBsAg?
|
Indicates hepatitis B infection (antigen found on surface of HBV)
|
|
|
What does it mean if your patient has anti-HBs?
|
Indicates immunity to Hepatitis B (antibody to HBsAg)
|
|
|
What does it mean if your patient has anti-HBc (IgM)?
|
Acute / recent infection with HCV (antibody to HBcAg)
|
|
|
What does it mean if your patient has anti-HBc (IgG)?
|
Prior exposure to HCV or chronic infection
|
|
|
What does it mean if your patient has HBeAg?
|
Active viral replication and therefore high transmissibility
|
|
|
What does it mean if your patient has anti-HBe?
|
Low transmissibility
|
|
|
What is the best serologic marker to detect active Hepatitis A infection?
|
Anti-HAV (IgM)
|
|
|
What is the serologic marker that indicates prior HAV infection and/or prior vaccination?
|
Anti-HAV (IgG)
|
|
|
Which serologic marker protects against reinfection of HAV?
|
Anti-HAV IgG
|
|
|
Which serologic marker indicates hepatitis B infection?
|
HBsAg
|
|
|
Which serologic marker indicates immunity to Hepatitis B infection?
|
Anti-HBs
|
|
|
Which serologic marker is associated with the core of HBV?
|
HBcAg
|
|
|
Which serologic marker indicates acute / recent infection with HBV?
|
Anti-HBc IgM
|
|
|
Which serologic marker indicates prior exposure or chronic infection with HBV?
|
Anti-HBc IgG
|
|
|
Which serologic marker is positive during the window period of HBV infection?
|
- Anti-HBc (IgG and IgM)
- Anti-HBe |
|
|
Which serologic marker indicates active viral replication and high transmissibility of HBV?
|
HBeAg
|
|
|
Which serologic marker indicates low transmissibility of HBV?
|
Anti-HBe
|
|
|
When is the ratio of ALT > AST?
|
Viral hepatitis
|
|
|
When is the ratio of AST > ALT?
|
Alcoholic hepatitis
|
|
|
Which serologic markers are present during Acute HBV? What do these markers mean?
|
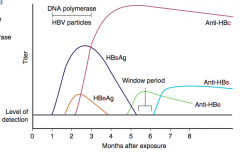
- HBsAg: hepatitis B infection
- HBeAg: high transmissibility and active viral replication - Anti-HBc IgM: acute / recent HBV infection |
|
|
Which serologic markers are present during the window period of HBV infection? What do these markers mean?
|
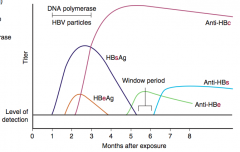
- Anti-HBe: low transmissibility
- Anti-HBc IgM: acute / recent HBV infection |
|
|
Which serologic markers are present during Chronic HBV (high infectivity)? What do these markers mean?
|
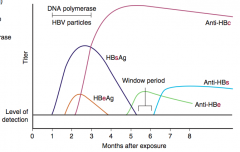
- HBsAg: hepatitis B infection
- HBeAg: high transmissibility and active viral replication - Anti-HBc IgG: prior exposure or chronic infection |
|
|
Which serologic markers are present during Chronic HBV (low infectivity)? What do these markers mean?
|
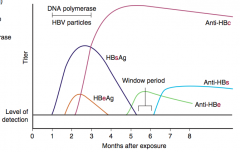
- HBsAg: hepatitis B infection
- Anti-HBe: low transmissibility - Anti-HBc IgG: prior exposure or chronic infection |
|
|
Which serologic markers are present during Recovery from HBV? What do these markers mean?
|
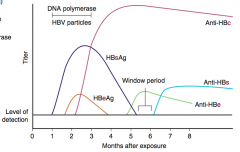
- Anti-HBs: immunity to HBV
- Anti-HBe: low transmissibility - Anti-HBc IgG: prior exposure or chronic infection |
|
|
Which serologic markers are present if immunized to HBV? What do these markers mean?
|
Anti-HBs: indicates immunity to HBV
|
|
|
What kind of virus is HIV?
|
Retrovirus
- Enveloped - SS (+) linear RNA - Diploid genome: 2 molecules of RNA - Complex and conical |
|
|
What are the structural genes (proteins coded for) by HIV?
|
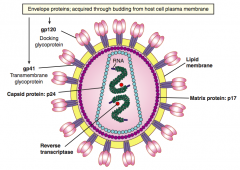
- env (gp120 and gp41)
- gag (p24) - pol |
|
|
What does the "env" gene by HIV code for?
|
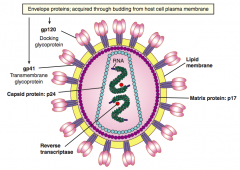
gp120 and gp41
- Formed from cleavage of gp160 to form envelope glycoproteins - gp120: attachment to host CD4+ T cell - gp41: fusion and entry |
|
|
What does the "gag" gene by HIV code for?
|
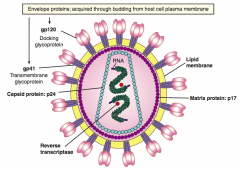
p24
- Capsid protein |
|
|
What does the "pol" gene by HIV code for?
|
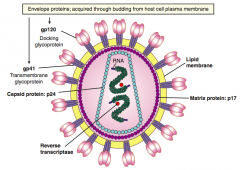
- Reverse transcriptase
- Aspartate protease - Integrase |
|
|
Which HIV gene/protein is responsible for attachment to host CD4+ T cell?
|
gp120 glycoprotein
- Formed from cleavage of gp160 which is encoded by "env" gene - One of the "env"elope proteins |
|
|
Which HIV gene/protein is responsible for fusion and entry?
|
gp41 glycoprotein
- Formed from cleavage of gp160 which is encoded by "env" gene - One of the "env"elope proteins |
|
|
Which HIV gene/protein is the capsid protein?
|
p24 protein
- "gag" gene |
|
|
Which HIV gene encodes reverse transcriptase, aspartate protease, and integrase?
|
"pol" gene
|
|
|
What is the function of Reverse Transcriptase in HIV?
|
- Synthesizes dsDNA from RNA
- dsDNA then integrates into host genome |
|
|
What does HIV bind on T cells?
|
- CCR5 co-receptor (early) OR CXCR4 co-receptor (late)
- CD4 |
|
|
What does HIV bind on macrophages?
|
- CCR5 co-receptor
- CD4 |
|
|
What can give someone immunity to HIV? How?
|
Homozygous CCR5 mutation (usually the virus will bind this co-receptor on T cells and macrophages)
|
|
|
What can give someone a slower course of HIV? How?
|
Heterozygous CCR5 mutation (usually the virus will bind this co-receptor on T cells and macrophages)
|
|
|
How do you make an initial diagnosis of HIV infection?
|
ELISA - sensitive, so it rules out (SNOUT) but has a high false-positive rate and low threshold
|
|
|
How do you make a confirmatory diagnosis of HIV infection?
|
Western Blot assay confirms positive ELISA results
- Specific so rules in (SPIN) - High false-negative rate and high threshold |
|
|
How can you determine the amount of HIV RNA in the plasma? Implications of this test?
|
HIV PCR / viral load test
- High viral load associated with poor prognosis - Also can be used to monitor effects of drug therapy |
|
|
How do you diagnose AIDS?
|
≤ 200 CD4+ cells / mm3
(normal 500-1500 cells/mm3) OR HIV positive with AIDS defining condition (eg, Pneumocystis pneumonia) OR CD4 percentage < 14% |
|
|
What is the use of ELISA and Western Blot tests for HIV?
|
Looks for antibodies to viral proteins
- Both often falsely negative in the first 1-2 months of HIV infection - Both often falsely positive initially in babies born to infected mothers (anti-gp120 crosses placenta) - ELISA used first to rule out (sensitive) - Western blot used second to rule in (specific) |
|
|
What are the four stages of untreated HIV infection?
|
Four F's:
1. Flu-like (acute) 2. Feeling fine (latent) 3. Falling count 4. Final criss |
|
|
What happens during the latent phase of HIV infection?
|
Virus replicates in the lymph nodes
|
|
|
What happens to the CD4+ T-cell count during an HIV infection?
|
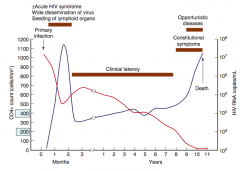
Red line
- Primary infection: drops from normal to ~500 over ~1 month - Latency: increases initially within a couple of months but eventually drops over a number of years - Late in disease: count drops more significantly first to moderate immunocompromise (<400) and eventually into AIDS diagnosis (<200) |
|
|
What happens to the HIV RNA copies / mL plasma during an HIV infection?
|
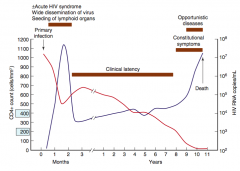
Blue line
- Primary infection: spikes within 2 months - Drops back down during clinical latency - Increases when latent period ends / immunocompromise |
|
|
What pathogen(s) cause a systemic presentation in HIV-positive adults?
|
Histoplasma capsulatum
|
|
|
What pathogen(s) cause a dermatologic presentation in HIV-positive adults?
|
- Candida albicans
- EBV - Bartonella henselae |
|
|
What pathogen(s) cause a gastrointestinal presentation in HIV-positive adults?
|
Cryptosporidium species
|
|
|
What pathogen(s) cause a neurologic presentation in HIV-positive adults?
|
- Toxoplasma gondii
- HIV itself - JC virus reactivation (cause of PML) - Cryptococcus neoformans - CMV |
|
|
What pathogen(s) cause an oncologic presentation in HIV-positive adults?
|
- EBV
- HPV - HHV-8 |
|
|
What pathogen(s) cause a respiratory presentation in HIV-positive adults?
|
- CMV
- Aspergillus fumigatus - Pneumocystis jirovecii - S. pneumoniae - Mycobacterium avium-intracellulare (aka Mycobacterium Avium Complex - MAC) |
|
|
Which pathogen causes low-grade fevers, cough, hepatosplenomegaly, and tongue ulcers in HIV-positive adults? Lab findings? Other?
|
Histoplasma capsulatum
- Oval yeast cells within macrophages - CD4+ < 100 cells / mm3 - Usually H. capsulatum only causes pulmonary symptoms in immunocompetent hosts |
|
|
Which pathogen causes fluffy white cottage-cheese lesions in HIV-positive adults? Lab findings? Other?
|
Candida albicans
- Pseudohyphae - Commonly oral if CD4+ < 400 cells/mm3 - Esophageal if CD4+ < 100 cells/mm3 - C. albicans causes oral thrush and esophagitis |
|
|
Which pathogen causes hairy leukoplakia in HIV-positive adults? Findings? Other?
|
Ebstein Barr Virus (EBV)
- Often on lateral tongue |
|
|
Which pathogen causes superficial vascular proliferation in HIV-positive adults? Lab findings? Other?
|
Bartonella henselae
- Biopsy reveals neutrophilic inflammation - B. henselae causes bacillary angiomatosis |
|
|
Which pathogen causes chronic, watery diarrhea in HIV-positive adults? Lab findings? Other?
|
Cryptosporidium species
- Acid-fast cysts seen in stool - Especially when CD4+ < 200 cells / mm3 |
|
|
Which pathogen causes abscesses in HIV-positive adults? Lab findings? Other?
|
Toxoplasma gondii
- Many ring-enhancing lesions on imaging - CD4+ < 100 cells/mm3 |
|
|
Which pathogen causes dementia in HIV-positive adults? Other?
|
Directly associated with HIV
- Must differentiate from other causes |
|
|
Which pathogen causes encephalopathy in HIV-positive adults? Lab findings? Other?
|
JC virus reactivation
- Cause of PML (progressive multifocal leukoencephalopathy) - Due to reactivation of a latent virus - Results in demyelination - CD4+ < 200 cells/mm3 |
|
|
Which pathogen causes meningitis in HIV-positive adults? Lab findings? Other?
|
Cryptococcus neoformans
- India ink stain reveals yeast with narrow-based budding and large capsules - CD4+ < 50 cells/mm3 |
|
|
Which pathogen causes retinitis in HIV-positive adults? Lab findings? Other?
|
Cytomegalovirus (CMV)
- Cotton-wool spots on fundoscopic exam - May also occur with esophagitis - CD4+ < 50 cells/mm3 |
|
|
Which pathogen causes non-Hodgkin Lymphoma (large cell type) in HIV-positive adults? Findings? Other?
|
May be associated with EBV
- Often on oropharynx (Waldeyer ring) |
|
|
Which pathogen causes primary CNS lymphoma in HIV-positive adults? Findings? Other?
|
Often associated with EBV
- Focal or multiple - Differentiate from toxoplasmosis |
|
|
Which pathogen causes squamous cell carcinoma in HIV-positive adults? Findings? Other?
|
HPV
- Often in anus (men who have sex with men) - Or in cervix |
|
|
Which pathogen causes Superficial Neoplastic Proliferations of Vasculature in HIV-positive adults? Findings? Other?
|
HHV-8 (Kaposi Sarcoma)
- Do not confuse with Bacillary Angiomatosis caused by B. henselae - Biopsy reveals lymphocytic inflammation |
|
|
Which pathogen causes interstitial pneumonia in HIV-positive adults? Findings? Other?
|
Cytomegalovirus (CMV)
- Biopsy reveals cells with intranuclear (owl eye) inclusion bodies |
|
|
Which pathogen causes pleuritic pain and hemoptysis in HIV-positive adults? Findings? Other?
|
Aspergillus fumigatus
- Invasive aspergillosis - Infiltrates seen on imaging |
|
|
Which pathogen causes pneumonia with a ground-glass appearance on imaging of lungs in HIV-positive adults? Lab findings? Other?
|
Pneumocystis jirovecii
- Especially with CD4+ < 200 cells/mm3 |
|
|
Which pathogens cause pneumonia in HIV-positive adults? Findings? Other?
|
- CMV: interstitial pneumonia, biopsy shows intranuclear (owl eye) inclusion bodies
- Pneumocystis jirovecii: pneumocystis pneumonia, ground glass appearance on imaging - S. pneumoniae: generally with CD4+ >200 cells/mm3 |
|
|
Which pathogen causes tuberculosis like disease in HIV-positive adults? Lab findings? Other?
|
Mycobacterium avium-intracellulare (aka Mycobacterium Avium Complex (MAC))
- Especially with CD4+ < 50 cells/mm3 |
|
|
What are the types of prion diseases?
|
- Creutzfeldt-Jakob disease (sporadic form)
- Gerstmann-Sträussler-Scheinker syndrome (inherited form) - Kuru (acquired form) |
|
|
What is the cause of prion diseases?
|
Conversion of normal (predominantly α-helical) protein termed prion protein (PrP-c) to a β-pleated form (PrP-sc) which is transmissible
|
|
|
What accumulates in patients with prion diseases? Characteristics?
|
PrP-sc (β-pleated form of proteins)
- Resists protease degradation - Facilitates conversion of still more PrP-c → PrP-sc |
|
|
What are the results of accumulation of PrP-sc in patient with prion diseases?
|
- Spongiform encephalopathy
- Dementia - Ataxia - Death |
|
|
Which form of prion disease is sporadic?
|
Creutzfeldt-Jakob disease (rapidly progressive dementia)
|
|
|
Which form of prion disease is inherited?
|
Gerstmann-Sträussler-Scheinker Syndrome
|
|
|
Which form of prion disease is acquired?
|
Kuru
|

