![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
141 Cards in this Set
- Front
- Back
|
Which protozoa cause GI infections? |
- Giardia lamblia
- Entamoeba histolytica - Cryptosporidium |
|
|
Which protozoa cause CNS infections?
|
- Toxoplasma gondii
- Naegleria fowleri - Trypanosoma brucei |
|
|
Which protozoa cause hematologic infections?
|
- Plasmodium (P. vivax/ovale, P. falciparum, P. malariae)
- Babesia |
|
|
Which protozoa cause visceral infections?
|
- Trypanosoma cruzi
- Leishmania donovani |
|
|
Which protozoa cause STDs?
|
Trichomonas vaginalis
|
|
|
Which parasite causes bloating, flatulence, foul-smelling fatty diarrhea (often seen in campers / hikers)? How is it transmitted? Diagnosed? Treated?
|
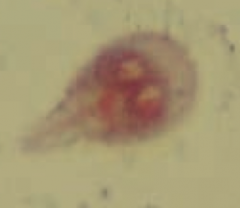
Giardia lamblia (GI protozoa)
- Transmitted via cysts in water - Diagnose by presence of trophozoites or cysts in stool - Treat with Metronidazole |
|
|
What disease is caused by Giardia lamblia? Symptoms?
|
Giardiasis
- Bloating - Flatulence - Foul-smelling, fatty diarrhea - Often seen in campers / hikers (Think fat rich Ghiradelli chocolates for fatty stools of Giardia) |
|
|
How is Giardia lamblia transmitted? Diagnosed?
|
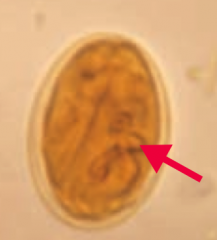
- Transmitted via cysts in water
- Diagnose by presence of trophozoites or cysts in stool |
|
|
How is Giardia lamblia treated?
|
Metronidazole
|
|
|
Which parasite causes bloody diarrhea (dysentery), liver abscesses (anchovy paste exudate), RUQ pain (d/t flask-shaped ulcer if submucosal abscess of colon ruptures)? How is it transmitted? Diagnosed? Treated?
|
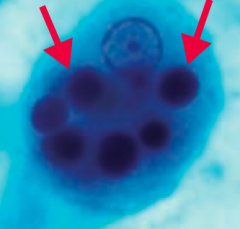
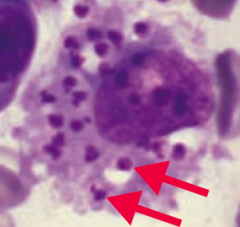
Entamoeba histolytica (GI protozoa)
- Transmitted via cysts in water - Diagnosed w/ serology and/or trophozoites with RBCs in the cytoplasm (picture) or cysts (with up to 4 nuclei) in the stool - Treat with Metronidazole; iodoquinol for asymptomatic cyst passers |
|
|
What disease is caused by Entamoeba histolytica? Symptoms?
|
Amebiasis
- Bloody diarrhea (dysentery) - Liver abscess ("anchovy paste" exudate) - RUQ pain (histology shows flask-shaped ulcer if submucosal abscess of colon ruptures) |
|
|
How is Entamoeba histolytica transmitted? Diagnosed?
|
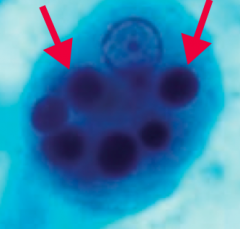
- Transmitted via cysts in water
- Diagnosed w/ serology and/or trophozoites with RBCs in the cytoplasm (arrows) or cysts (with up to 4 nuclei) in the stool (circle between arrows) |
|
|
How is Entamoeba histolytica treated?
|
- Metronidazole
- Iodoquinol for asymptomatic cyst passers |
|
|
Which parasite causes severe diarrhea in AIDS or mild disease (watery diarrhea) in non-immunocompromised patients? Transmission? Diagnosis? Treatment?
|
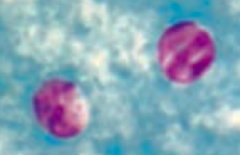
Cryptosporidium (GI protozoa)
- Transmitted via oocysts in water - Diagnose via oocysts on acid-fast stain - Treated with nitazoxanide in immunocompetent hosts - Primarily focus on prevention by filtering city water supplies |
|
|
What disease is caused by Cryptosporidium? Symptoms?
|
- Severe diarrhea in AIDS
- Mild disease (watery diarrhea) in non-immunocompromised |
|
|
How is Cryptosporidium transmitted? Diagnosed?
|
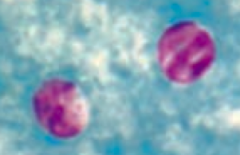
- Transmitted via oocysts in water
- Diagnose via oocysts on acid-fast stain |
|
|
How is Cryptosporidium treated?
|
- Treated with nitazoxanide in immunocompetent hosts
- Primarily focus on prevention by filtering city water supplies |
|
|
How do the protozoa that cause GI infections present?
|
- Giardia lamblia: fatty diarrhea, bloating, flatulence
- Entamoeba histolytica: bloody diarrhea, liver abscesses, RUQ pain - Cryptosporidium: severe diarrhea in AIDS or mild watery diarrhea in healthy |
|
|
How are the protozoa that cause GI infections transmitted?
|
- Giardia lamblia: cysts in water
- Entamoeba histolytica: cysts in water - Cryptosporidium: oocysts in water |
|
|
How are the protozoa that cause GI infections diagnosed?
|
- Giardia lamblia: trophozoites or cysts in stool
- Entamoeba histolytica: serology and/or trophozoites (w/ RBCs in cytoplasm) or cysts (with up to 4 nuclei) in stool - Cryptosporidium: oocysts on acid-fast stain |
|
|
How are the protozoa that cause GI infections treated?
|
- Giardia lamblia: Metronidazole
- Entamoeba histolytica: Metronidazole; iodoquinol for asymptomatic cyst passers - Cryptosporidium: prevention (filtering city water) and nitazoxanide in immunocompetent |
|
|
Which protozoa cause CNS infections?
|
- Toxoplasma gondii
- Naegleria fowleri - Trypanosoma brucei |
|
|
Which parasite causes brain abscesses in HIV patients (ring enhancing brain lesions on CT/MRI)? Transmission? Diagnosis? Treatment?
|
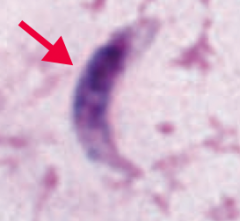
Toxoplasma gondii (protozoa)
- Transmitted via cysts in meat or oocysts in cat feces; crosses placenta (pregnant women should avoid cats) - Diagnosed via serology and biopsy (tachyzoite - picture) - Treat with Sulfadiazine + Pyrimethamine |
|
|
What is the classic presentation of congenital Toxoplasma gondii infection?
|
Classic Triad
- Chorioretinitis - Hydrocephalus - Intracranial calcifications |
|
|
What is caused by Toxoplasma gondii infection?
|
Brain abscess in HIV
- Seen as a ring-enhancing brain lesion on CT/MRI |
|
|
How is Toxoplasma gondii transmitted and diagnosed?
|
- Transmitted via cysts in meat or oocysts in cat feces; crosses placenta (pregnant women should avoid cats)
- Diagnosed via serology and biopsy (tachyzoite - picture) |
|
|
How is Toxoplasma gondii treated?
|
Sulfadiazine + Pyrimethamine
|
|
|
Which parasite presents as rapidly fatal meningoencephalitis? Transmission? Diagnosis? Treatment?
|
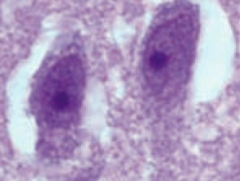
Naegleria fowleri (protozoa)
- Transmitted via swimming in freshwater lakes (think Nalgene bottle filled with fresh water containing Naegleria); enters via cribriform plate - Diagnosed via amoebas in spinal fluid (picture) - Treat with Amphotericin B (effective for a few survivors) |
|
|
What kind of disease is caused by Naegleria fowleri infection?
|
Rapidly fatal meningoencephalitis
|
|
|
How is Naegleria fowleri transmitted and diagnosed?
|
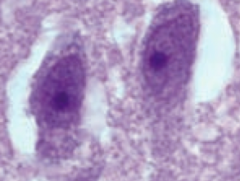
- Transmitted via swimming in freshwater lakes (think Nalgene bottle filled with fresh water containing Naegleria); enters via cribriform plate
- Diagnosed via amoebas in spinal fluid (picture) |
|
|
How is Naegleria fowleri treated?
|
Amphotericin B (effective for a few survivors)
|
|
|
Which parasite causes African sleeping sickness - enlarged lymph nodes, recurring fever, somonlence, and coma? Transmission? Diagnosis? Treatment?
|
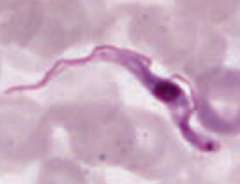
Trypanosoma brucei (protozoa)
- Transmitted via Tsetse fly, a painful bite - Diagnose via blood smear (picture) - Treat with SURamin for blood borne disease or MELAsoprol for CNS penetration ("it SURe is nice to go to sleep" - MELAtonin helps with sleep) |
|
|
What are the subspecies of Trypanosoma brucei?
|
- Trypanosoma brucei rhodesiense
- Trypanosoma brucei gambiense |
|
|
What does infection with Trypanosoma brucei cause?
|
African sleeping sickness
- Enlarged lymph nodes - Recurring fever (d/t antigenic variation) - Somnolence - Coma |
|
|
How is Trypanosoma brucei transmitted and diagnosed?
|
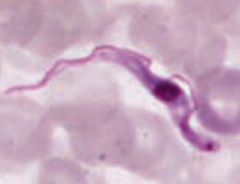
- Transmitted via Tsetse fly, a painful bite
- Diagnose via blood smear (picture) |
|
|
How is Trypanosoma brucei treated?
|
Treat with SURamin for blood borne disease or MELAsoprol for CNS penetration
("it SURe is nice to go to sleep" - MELAtonin helps with sleep) |
|
|
How do the protozoa that cause CNS infections present?
|
- Toxoplasma gondii: brain abscess in HIV and congenital disease (chorioretinitis, hydrocephalus, intracranial calcifications)
- Naegleria fowleri: rapidly fatal meningoencephalitis - Trypanosoma brucei: African sleeping sickness |
|
|
How are the protozoa that cause CNS infections transmitted?
|
- Toxoplasma gondii: cysts in meat or oocysts in cat feces (crosses placenta)
- Naegleria fowleri: swimming in freshwater lakes; enters via cribriform plate - Trypanosoma brucei: Tsetse fly, painful bite |
|
|
How are the protozoa that cause CNS infections diagnose?
|
- Toxoplasma gondii: serology, biopsy (tachyzoite)
- Naegleria fowleri: amoebas in spinal fluid - Trypanosoma brucei: blood smear |
|
|
How are the protozoa that cause CNS infections treated?
|
- Toxoplasma gondii: Sulfadiazine + Pyrimethamin
- Naegleria fowleri: Amphotericin B (effective for a few survivors) - Trypanosoma brucei: Suramin (blood-borne disease) or Melarsoprol (CNS penetration) |
|
|
Which protozoa cause hematologic infections?
|
- Plasmodium (P. vivax/ovale, P. falciparum, P. malariae)
- Babesia |
|
|
Which parasite causes malaria: fever, headache, anemia, splenomegaly? Transmission? Diagnosis? Treatment?
|
Plasmodium (protozoa)
- Transmitted via mosquitos (Anopheles) - Diagnosed with blood smear, trophozoite ring form within RBC, schizont containing merozoites - Treat with Chloroquine (if resistant use Mefloquine or Atovaquone / Proguanil); if life-threatening use IV quinidine (check for G6PD deficiency); for P. vivax / ovale add Primaquine (check for G6PD deficiency) |
|
|
What are the species of Plasmodium?
|
- P. vivax / ovale
- P. falciparum - P. malariae |
|
|
What are the characteristics of P. vivax / ovale?
|
- 48 hour cycle (tertian - includes fever on first day and third day)
- Dormant form (hypnozoite) in LIVER (liver has 5 letters and so do vivax and ovale) |
|
|
What are the characteristics of P. falciparum?
|
- Severe
- Irregular fever patterns - Parasitized RBCs occlude capillaries in brain (cerebral malaria), kidneys, and lungs |
|
|
What are the characteristics of P. malariae?
|
72 hour cycle (quartan)
|
|
|
How is Plasmodium transmitted?
|
Mosquito (Anopheles)
|
|
|
How do you diagnose Plasmodium infection?
|
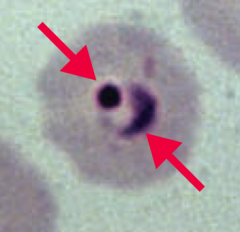
- Blood smear
- Trophozoite ring form within RBC (picture) - Schizont containing merozoites |
|
|
How do you treat Plasmodium infection?
|
- Begin with Chloroquine - blocks Plasmodium heme polymerase
- If resistant to Chloroquine, use Mefloquine or Atovaquone / Proguanil - If life-threatening, use IV Quinidine (test for G6PD deficiency) - If P. vivax / ovale - add Primquine for Hypnozoite (in liver) and test for G6PD deficiency) |
|
|
For what drugs for Plasmodium / Malaria infection should you check for G6PD deficiency? When are these drugs used?
|
- IV Quinidine - for life-threatening cases
- Primaquine - for P. vivax / ovale strains |
|
|
Which parasite presents with fever and hemolytic anemia, predominantly in NE US? Transmission? Diagnosis? Treatment?
|
Babesia
- Transmitted via Ixodes tick - Diagnosed with blood smear (ring form or Maltese cross) or PCR - Treat with Atovaquone + Azithromycin |
|
|
What does Babesia infection cause?
|
Babesiosis
- Fever - Hemolytic anemia - Asplenia increases risk of severe disease |
|
|
How is Babesia transmitted?
|
Ixodes tick (same as Borrelia burdorferi of Lyme disease)
- May co-infect humans with both Babesia and Lyme disease |
|
|
How is Babesia diagnosed?
|
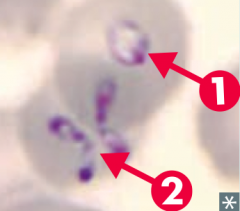
- Blood smear: ring form (1) and "Maltese cross" (2)
- PCR |
|
|
How do you treat Babesia infection?
|
Atovaquone + Azithromycin
|
|
|
How do the hematologic protozoa differ in their disease presentation?
|
- Plasmodium: malaria - fever, headache, anemia, splenomegaly
- Babesia: fever and hemolytic anemia, more severe if asplenic |
|
|
How do the hematologic protozoa differ in their disease transmission?
|
- Plasmodium: mosquito (Anopheles)
- Babesia: Ixodes tick (same as Borrelia burgdorferi of Lyme disease, may co-infect) |
|
|
How do the hematologic protozoa differ in their diagnosis?
|
- Plasmodium: blood smear, trophozoite ring form within RBC, schizont containing merozoites
- Babesia: blood smear (presence of ring form or Maltese cross) or PCR |
|
|
How do the hematologic protozoa differ in their treatment
|
- Plasmodium: Chloroquine (or if resistant: Mefloquine or Atovaquone / Proguanil), +/- Quinidine if life-threatening, +/- Primaquine if Vivax or Ovale
- Babesia: Atovaquone + Azithromycin |
|
|
Which protozoa cause visceral infections?
|
- Trypanosoma cruzi
- Leishmania donovani |
|
|
Which protozoa causes Chagas disease - dilated cardiomyopathy, megacolon, megaesophagus? Transmission? Diagnosis? Treatment?
|
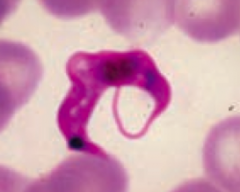
Trypanosoma cruzi (protozoa)
- Transmitted via Reduviid bug ("kissing bug") feces, deposited in a painless bite (much like a kiss) - Diagnosed via blood smear (picture) - Treat with Benznidazole or Nifurtimox |
|
|
What disease does Trypanosoma cruzi cause? Symptoms?
|
Chagas disease
- Dilated Cardiomyopathy - Megacolon - Megaesophagus - Predominantly in S. America |
|
|
How is Trypanosoma cruzi transmitted and diagnosed?
|
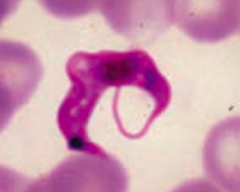
- Transmitted via Reduviid bug ("kissing bug") feces, deposited in a painless bite (much like a kiss)
- Diagnosed via blood smear (picture) |
|
|
How is Trypanosoma cruzi treated
|
Benznidazole or Nifurtimox
|
|
|
Which parasite causes visceral leishmaniasis (kala-azar) - spiking fevers, hepatosplenomegaly, and pancytopenia? Transmission? Diagnosis? Treatment?
|
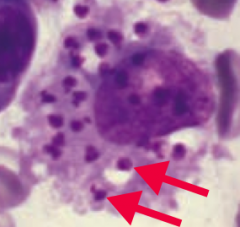
Leishmania donovani (protozoa)
- Transmitted via sandfly - Diagnose via presence of macrophages containing amastigotes (picture) - Treat with Amphotericin B and Sodium Stibogluconate |
|
|
What disease is caused by Leishmania donovani? Symptoms?
|
Visceral Leishmaniasis (Kala-Azar)
- Spiking fevers - Hepatosplenomegaly - Pancytopenia |
|
|
How is Leishmania donovani transmitted and diagnosed?
|
- Transmitted via sandfly
- Diagnose via presence of macrophages containing amastigotes (picture) |
|
|
How is Leishmania donovani treated?
|
Amphotericin B and Sodium Stibo
|
|
|
How do the visceral protozoa present?
|
- Trypanosoma cruzi: Chagas disease (dilated CM, megacolon, megaesophagus)
- Leishmania donovani: visceral leishmaniasis (spiking fevers, hepatosplenomegaly, pancytopenia) |
|
|
How are the visceral protozoa transmitted?
|
- Trypanosoma cruzi: Reduviid bug (kissing bug) feces, deposited in a painless bite (much like a kiss)
- Leishmania donovani: Sandfly |
|
|
How are the visceral protozoa diagnosed?
|
- Trypanosoma cruzi: blood smear
- Leishmania donovani: macrophages containing amastigotes |
|
|
How are the visceral protozoa treated?
|
- Trypanosoma cruzi: Benznidazole or Nifurtimox
- Leishmania donovani: Amphotericin B and Sodium Stibogluconate |
|
|
Which protozoa cause STDs?
|
Trichomonas vaginalis
|
|
|
Which parasite presents as vaginitis with foul-smelling greenish discharge, itching and burning and causes the cervix to look like a strawberry? Transmission? Diagnosis? Treatment?
|

Trichomonas vaginalis
- Transmitted sexually (doesn't exist outside human because it can't form cysts) - Diagnosed via presence of trophozoites (motile - picture) on wet mount; "strawberry cervix" - Treat with Metronidazole for patient and partner (prophylaxis) |
|
|
How do you distinguish Trichomonas vaginalis from Gardnerella vaginalis?
|
- Trichomonas vaginalis: protozoa / parasite
- Gardnerella vaginalis: gram-variable bacterium associated with bacterial vaginosis |
|
|
How does Trichomonas vaginalis present?
|
Vaginitis
- Foul-smelling, greenish discharge - Itching and burning |
|
|
How is Trichomonas vaginalis transmitted and diagnosed?
|

- Transmitted sexually (doesn't exist outside human because it can't form cysts)
- Diagnosed via presence of trophozoites (motile - picture) on wet mount; "strawberry cervix" |
|
|
How is Trichomonas vaginalis treated?
|
Metronidazole for patient and partner (prophylaxis)
|
|
|
What are the types of intestinal nematodes (roundworms)?
|
- Enterobius vermicularis (pinworm)
- Ascaris lumbricoides (giant roundworm) - Strongyloides stercoralis - Ancylostoma duodenale, Necator americanus (hookworms) |
|
|
What are the types of tissue nematodes (roundworms)?
|
- Onchocerca volvulus
- Loa loa - Wuchereria bancrofti - Toxocara canis |
|
|
Which parasite causes intestinal infection causing anal pruritus and is diagnosed by the Scotch Tape test? Transmission? Treatment?
|
Enterobius vermicularis (pinworm / nematode)
- Fecal-oral transmission - Treat with Bendazoles or pyrantel pamoate (because worms are bendy) |
|
|
What kind of parasite is Enterobius vermicularis? How is it transmitted?
|
- Pinworm - nematode / roundworm
- Transmitted via fecal-oral route |
|
|
What symptoms are caused by Enterobius vermicularis? How is it treated?
|
- Intestinal infection causing anal pruritus (diagnosed via Scotch Tape test)
- Treat with Bendazoles or pyrantel pamoate (because worms are bendy) |
|
|
Which parasite causes intestinal infection and the eggs are visible in feces under a microscope? Transmission? Treatment?
|
Ascaris lumbricoides (giant roundworm - nematode)
- Fecal-oral transmission - Treat with Bendazoles or pyrantel pamoate |
|
|
What kind of parasite is Ascaris lumbricoides? How is it transmitted?
|
- Giant roundworm - nematode
- Transmitted via fecal-oral route (eggs are visible in feces under the microscope) |
|
|
What symptoms are caused by Ascaris lumbricoides? How is it treated?
|
- Intestinal infection
- Treat with bendazoles or pyrantel pamoate |
|
|
Which parasite causes an intestinal infection causing vomiting, diarrhea, and epigastric pain that may mimic the feeling of a peptic ulcer)? Transmission? Treatment?
|
Strongyloides stercoralis (nematode)
- Larvae in soil penetrate the skin - Treat with Ivermectin or Albendazole |
|
|
What kind of parasite is Strongyloides stercoralis? How is it transmitted?
|
- Nematode (roundworm)
- Larvae in soil penetrate the skin |
|
|
What symptoms does Strongyloides stercoralis cause? Treatment?
|
- Intestinal infection causing vomiting, diarrhea, epigastric pain (may be peptic-ulcer like)
- Treat with Ivermectin or Albendazole |
|
|
Which parasite causes intestinal infection that leads to anemia by sucking blood from intestinal walls? Transmission? Treatment?
|
Ancylostoma duodenale and Necator americanus (hookworms)
- Larvae penetrate the skin - Treat with Bendazoles or Pyrantel Pamoate |
|
|
How are the different intestinal nematodes (roundworms) transmitted?
|
- Enterobius vermicularis (pinworm): fecal-oral
- Ascaris lumbricoides (giant roundworm): fecal-oral (eggs visible in feces under microscope) - Strongyloides stercoralis: larvae in soil penetrate skin - Ancylostoma duodenale, Necator americanus (hookworms): larvae penetrate skin |
|
|
How do the intestinal nematodes (roundworms) differ in presentation?
|
- Enterobius vermicularis (pinworm): anal pruritus (diagnosed via Scotch Tape test)
- Ascaris lumbricoides (giant roundworm): intestinal infection - Strongyloides stercoralis: vomiting, diarrhea, epigastric pain (may be peptic-ulcer like) - Ancylostoma duodenale, Necator americanus (hookworms): intestinal infection causes anemia by sucking blood from intestinal walls |
|
|
How do the intestinal nematodes (roundworms) differ in treatment?
|
- Enterobius vermicularis (pinworm): Bendazoles or Pyrantel Pamoate
- Ascaris lumbricoides (giant roundworm): Bendazoles or Pyrantel Pamoate - Strongyloides stercoralis: Ivermectin or Albendazole - Ancylostoma duodenale, Necator americanus (hookworms): Bendazoles or Pyrantel Pamoate |
|
|
What are the types of tissue nematodes (roundworms)?
|
- Onchocerca volvulus
- Loa loa - Wuchereria bancrofti - Toxocara canis |
|
|
Which parasite causes hyperpigmented skin and river blindness? Transmission? Treatment
|
Onchocerca volvulus (nematode / roundworm)
- Black flies, black skin nodules, "black sight" - Allergic reaction to microfilaria possible - Transmitted via female blackfly bite - Treat with IVERmectin (for rIVER blindness) |
|
|
What kind of parasite is Onchocerca volvulus? How is it transmitted?
|
- Nematode (roundworm)
- Transmitted via female blackfly bite |
|
|
What symptoms does Onchocerca volvulus cause? How do you treat it?
|
- Hyperpigmented skin and river blindness
- Allergic reaction to microfilaria possible ("black flies, black skin nodules, and black sight") - Treat with Ivermectin (IVERmectin for rIVER blindness) |
|
|
Which parasite causes swelling in the skin and the worm can be visualized in the conjunctiva? Transmission? Treatment?
|
Loa loa (nematode / roundworm)
- Transmitted via deer fly, horse fly, and mango fly - Treat with Diethylcarbamazine |
|
|
What kind of parasite is Loa loa? How is it transmitted?
|
- Nematode / roundworm
- Transmitted via deer fly, horse fly, and mango fly |
|
|
What symptoms does Loa loa cause? Treatment?
|
- Swelling in skin
- Worm can be visualized in the conjunctiva - Treat with Diethylcarbamazine |
|
|
Which parasite blocks lymphatic vessels leading to elephantiasis 9 months to 1 year after bite? Transmission? Treatment?
|
Wuchereria bancrofti (nematode / roundworm)
- Transmitted via female mosquito - Treat with Diethylcarbamazine |
|
|
What type of parasite is Wuchereria bancrofti? How is it transmitted?
|
- Nematode / roundworm
- Transmitted via female mosquito |
|
|
What symptoms does Wuchereria bancrofti cause? Treatment?
|
- Blocks lymphatic vessels → elephantitis
- Takes 9 months to 1 year after bite from female mosquito to become symptomatic - Treat with Diethylcarbamazine |
|
|
Which parasite causes visceral larva migrans? Transmission? Treatment?
|
Toxocara canis (nematode / roundworm)
- Transmitted via fecal-oral route - Treated with Albendazole or Mebendazole |
|
|
What kind of parasite is Toxocara canis? How is it transmitted?
|
- Nematode / roundworm
- Transmitted via fecal-oral route |
|
|
What symptoms does Toxocara canis cause? Treatment?
|
- Visceral larva migrans
- Treat with Albendazole or Mebendazole |
|
|
How are the tissue nematodes / roundworms transmitted?
|
- Onchocerca volvulus: female blackfly bite
- Loa loa: deer fly, horse fly, mango fly - Wuchereria bancrofti: female mosquito - Toxocara canis: fecal-oral |
|
|
What symptoms do the tissue nematodes / roundworms cause?
|
- Onchocerca volvulus: hyperpigmented skin and river blindness, allergic reaction to microfilaria possible
- Loa loa: swelling in skin, worm in conjunctiva - Wuchereria bancrofti: blocks lymphatic vessels - elephantitis (takes 9mo-1yr to become symptomatic) - Toxocara canis: visceral larva migrans |
|
|
How are the tissue nematodes / roundworms treated?
|
- Onchocerca volvulus: Ivermectin (for rIVER blindness)
- Loa loa: Diethylcarbamazine - Wuchereria bancrofti: Diethylcarbamazine - Toxocara canis: Albendazole or Mebendazole |
|
|
Which nematodes are ingested?
|
You'll get sick if you EAT these!
- Enterobius vermicularis (pinworm) - Ascaris lumbricoides (giant roundworm) - Toxocara canis |
|
|
Which nematodes are acquired through a cutaneous route?
|
These get into your feet from the SANd?
- Strongyloides stercoralis - Ancylostoma duodenale (hookworm) - Necator americanus (hookworm) |
|
|
Which nematodes are acquired via a bite?
|
Lay LOW to avoid getting bitten
- Loa loa - Onchocerca volvulus - Wuchereria bancrofti |
|
|
What are the cestodes (tapeworms)?
|
- Taenia solium
- Diphyllobothrium latum - Echinococcus granulosus |
|
|
Which parasite causes cysticercosis (cysts in skin) and neurocysticercosis (cysts in brain) after ingestion of larvae encysted in undercooked pork? Disease? Transmission? Treatment?
|
Taenia solium (cestodes / tapeworms)
- Intestinal infection treated with Praziquantel - Cysticercosis treated with Praziquantel - Neurocysticercosis treated with Albendazole - Ingestion of larvae encysted in undercooked pork or ingestion of eggs |
|
|
What kind of parasite is Taenia solium? How is it transmitted?
|
- Cestode (tapeworm)
- Transmitted via ingestion of larvae encysted in undercooked pork or by ingestion of eggs |
|
|
What diseases are caused by Taenia solium? How are they treated?
|
- Intestinal infection treated with Praziquantel
- Cysticercosis (cysts in skin) treated with Praziquantel - Neurocysticercosis (cysts in brain) treated with Albendazole |
|
|
Which parasite causes a vitamin B12 deficiency by competing for B12 in the intestine, leading to anemia? Transmission? Treatment?
|
Diphyllobothrium latum (cestode / tapeworm)
- Ingestion of larvae from raw freshwater fish - Treated with Praziquantel |
|
|
What kind of parasite is Diphyllobothrium latum? How is it transmitted?
|
- Cestode / tapeworm
- Ingestion of larvae from raw freshwater fish |
|
|
What disease does Diphyllobothrium latum cause? How is it treated?
|
- Vitamin B12 deficiency (tapeworm competes for B12 in intestine), which causes anemia
- Treat with Praziquantel |
|
|
Which parasite causes hydatid cysts in liver, causing anaphylaxis if antigens are release? Transmission? Treatment?
|
Echinococcus granulosus (cestode / tapeworm)
- Ingestion of eggs from dog feces - Surgeons must pre-inject hydatid cysts in liver with ethanol to kill cysts before removal - Or treat with Albendazole |
|
|
How are the Cestodes (Tapeworms) transmitted?
|
- Taenia solium: ingestion of larvae encysted in undercooked pork or ingestion of eggs
- Diphyllobothrium latum: ingestion of larvae from raw freshwater fish - Echinococcus granulosus: ingestion of eggs from dog feces |
|
|
What diseases do the Cestodes (Tapeworms) cause?
|
- Taenia solium: intestinal infection and cysticercosis and/or neurocysticercosis
- Diphyllobothrium latum: vitamin B12 deficiency, causing anemia - Echinococcus granulosus: hydatid cysts in liver, can cause anaphylaxis if antigens released |
|
|
How are the Cestodes (Tapeworms) treated?
|
- Taenia solium: Praziquantel and Albendazole for Neurocysticercosis
- Diphyllobothrium latum: Praziquantel - Echinococcus granulosus: Albendazole |
|
|
What are the Trematodes (flukes)?
|
- Schistosoma
- Clonorchis senensis |
|
|
Which parasite causes liver and spleen granulomas, fibrosis, and inflammation or if chronic, can lead to squamous cell carcinoma of the bladder (painless hematuria)? Transmission? Treatment?
|
Schistosoma (trematode / fluke)
- Snails are hosts, cercariae penetrate skin of humans - Treat with Praziquantel |
|
|
What kind of parasite is Schistosoma? How is it transmitted?
|
- Trematode (fluke)
- Snails are the host, cercariae (free-swimming larval stage) penetrate skin of humans |
|
|
What kind of disease does Schistosoma cause? Treatment?
|
- Liver and spleen granulomas, fibrosis, and inflammation
- Chronic infection with S. haematobium can lead to squamous cell carcinoma of bladder (painless hematuria) - Treat with Praziquantel |
|
|
Which parasite causes biliary tract inflammation and pigmented gallstones and is associated with cholangiocarcinoma? Transmission? Treatment?
|
Clonorchis sinensis (trematode / fluke)
- Transmitted via undercooked fish - Treat with Praziquantel |
|
|
What kind of parasite is Clonorchis sinensis? How is it transmitted?
|
- Trematode / fluke
- Transmitted via undercooked fish |
|
|
What disease does Clonorchis sinensis cause? Treatment?
|
- Biliary tract inflammation, which can lead to pigmented gallstones
- Associated with cholangiocarcinoma - Treat with Praziquantel |
|
|
How are the trematodes / flukes transmitted?
|
- Schistosoma: snails are host, cercariae penetrate skin of humans
- Clonorchis senensis: undercooked fish |
|
|
What diseases do the trematodes / flukes cause?
|
- Schistosoma: liver and spleen granulomas, fibrosis and inflammation; chronic infection associated with squamous cell carcinoma of bladder
- Clonorchis senensis: biliary tract inflammation can lead to pigmented gallstones; associated with cholangiocarcinoma |
|
|
How are the trematodes / flukes treated?
|
- Schistosoma: Praziquantel
- Clonorchis senensis: Praziquantel |
|
|
Which parasite should you associate with biliary tract disease and cholangiocarcinoma?
|
Clonorchis sinensis - trematode / fluke
|
|
|
Which parasite should you associate with brain cysts and seizures?
|
Taenia solium (neurocysticercosis) - cestode / tapeworm
|
|
|
Which parasite should you associate with hematuria and bladder cancer?
|
Schistosoma haematobium - trematode / fluke
|
|
|
Which parasite should you associate with liver (hydatid cysts)?
|
Echinococcus granulosus - cestode / tapeworm
|
|
|
Which parasite should you associate with microcytic anemia?
|
Nematodes / roundworms:
- Ancylostoma duodenale (hookworm) - Necator americanus (hookworm) |
|
|
Which parasite should you associate with perianal pruritus?
|
Enterobius vermicularis (pinworm) - nematode / roundworm
|
|
|
Which parasite should you associate with portal hypertension?
|
Trematodes / flukes (cause liver granulomas, fibrosis, and inflammation)
- Schistosoma mansoni - Schistosoma japonicum |
|
|
Which parasite should you associate with vitamin B12 deficiency?
|
Diphyllobothrium latum - cestode / tapeworm
|

