![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
55 Cards in this Set
- Front
- Back
|
What is the normal value for ipsilateral R1 latency?
|
< 13 msec
|
|
|
What is the normal value for ipsilateral R2 latency?
|
<40 msec
|
|
|
What is the normal value for contralateral R2 latency?
|
<41 msec
|
|
|
What specific nerve innervates taste for anterior 2/3 of tongue with CN 7?
|
chorda tympani?
|
|
|
What is the sensory innervation of facial nerve?
|
sensation to posterior external auditory canal, tympanic and external acoustic membranes
|
|
|
What is the etiology of Bell's palsy?
|
reactivation of latent HSV type 1, often isolated from geniculate ganglion endoneurium (79% of pt.)
|
|
|
What is Ramsay Hunt syndrome?
|
Herpes Zoster infection with vesicle in the external auditory canal or posterior pharynx with 7th nerve palsy and tinnitus and decreased hearing with 8th nerve involvement
|
|
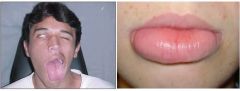
What is the diagnosis?
|
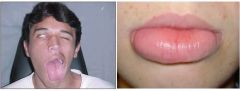
Melkersson-Rosenthal syndrome, tongue abnormalities, 7th N palsy, recurrent orofacial edema
|
|
|
What CMAP amplitude suggests complete recovery after Bell's palsy?
|
More than 30% of normal side indicates likely complete recovery
|
|
|
What is the pattern of multiofcal motor neuropathy?
|
weakness, fasciculations, atrophy, mostly upper ext, asymm, individual nerve territories
|
|
|
What is MAMA?
|
multifocal acquired motor axonopathy without conduction blocks
|
|
|
Which CIDP variant often has fasciculations?
|
MMN
|
|
|
What are the differences in treatment response between MMN and classic CIDP?
|
MMN could be less responsive to steroids, this is also true of MAMA (multifocal acquired motor axonopathy)
|
|
|
What is the classic site of weakness for slow channel syndrome?
|
finger extensors
|
|
|
What is the action of MuSK?
|
Muscle specific knase mediates agrin-induced clustering of Ach receptors and may affect the formation of ACh receptors
|
|
|
What is the mechanism of action of azathioprine?
|
It forms 6-mercaptopurine which inhibits purine synthesis
|
|
|
What is the mechanism of action of mycophenolate mofetil?
|
It inhibitis inosine monophosphate dehydrogenase which acts to decrease purine synthesis
|
|
|
What is CMD 1A (congenital muscular dystrophy type 1A)?
|
Merosin aka Lamin alpha-2 deficiency. This is a protein in extracellular space that binds the extracellular matrix to the membrane (cross structure) expressed in most tissues
|
|
|
What is the clinical phenotype of CMD 1A?
|
30% have seizures, mental retardation in up to 50%, facial and limb muscle weakness, joint contractures, elevated CK (exception to other CMD), 30% have seizures, white matter findings due to decreased expression of laminin in BBB, can have neuropathy
|
|
|
What is CMD (congenital muscular dystrophy 1B)?
|
Unknown protein/gene
|
|
|
What is CMD 1C? (congenital muscular dstrophy 1C)
|
Fukutin related protein, (related to LGMD 2I)
|
|
|
What is CMD 1D?
|
only in 1 patient, LARGE gene
|
|
|
How is the diagnosis of CMD 1A made?
|
merosin staining on muscle biopsy as well as genetic testing for laminin alpha-2
|
|
|
What is the gene abnormality in CMD with early rigid spine?
|
Selenoprotein-N
|
|
|
What is the mechanism of action of methotrexate?
|
inhibits folate metabolism
|
|
|
What is Calciotriol?
|
1,2 dihydroxycholecalciferol
|
|
|
What are some causes of Tarsal tunnel syndrome. Think about structures that occur at that location.
|
Bone- RA, bony tumor
Muscle- AH hypertrophy Trauma- Frx, Hematoma Mass- neuroma, fibroma, abcess, lipoma, cyst Repeated compresssion |
|
|
What are some causes of sciatic neuropathy? Think about the structures that occur in that location
|
Muscle- Pyriformis syndrome, muscle fibrosis
Bone- Frx, bone tumor Mass- Neuroma, fibroma, bone tumor, muscle tumor, abcess, cyst, lipoma, aneurysm Trauma- Frx, Hematoma Iatrogenic- Injxn, Surgery, prolonged standing |
|
|
What type of aneurysm may lead to a sciatic neuropathy?
|
aneurysm or pseudoaneurysm of a persistent sciatic artery
|
|
|
What is ligament of struthers?
|
ligamentous/fibrous band between the medial epicondyl and a bony spur on distal medial humerus (present in 1-2% of populations)
|
|
|
What type of entrapment neuropathy can ligament of struthers cause?
|
proximal median nerve entrapment, involving the pronator teres.
|
|
|
What type of symptoms suggest median neuropathy due to ligament of struthers?
|
pain on elbow extension and forearm supination. Decreased radial artery during the same movement (b/c the brachial artery runs next to the median nerve)
|
|
|
What are the places of entrapment attributed to "pronator syndrome"
|
lacertus fibrosus
pronator teres heads sublimis bridge |
|
|
What is lacertus fibrosus?
|
fibrous band that connects forearm musculature and medial biceps tendon
|
|
|
What are symptoms suggestive of median neuropathy due to lacertus fibrosus?
|
resisted elbow flexion with arm in supination
|
|
|
What are symptoms suggestive of median neuropathy due to entrapment in pronator teres?
|
Tinel's over pronator teres, pronator can feel enlarged or firm. Pronator teres primarily pronates the arm with the elbow in extension, as opposed to pronator quadratus which pronates the arm with the elbow in flexion
|
|
|
What are symptoms suggestive of median neuropathy due to sublimis bridge entrapment?
|
pain or resistance with flexion of the PIP on index finger
|
|
|
Why is it that an AIN may cause weakness of DIP flexion in digit 2 but not digit 3?
|
Digit 3 (middle finger) may be spared in AIN because some people have primary innervation of DIP flexion in digit 3 by ulnar nerve
|
|
|
Why is it that if NCS show a non-localizing median neuropathy you are limited by saying EMG shows the lesion is at or proximal to the most proximal muscle innervated?
|
The reason is because some proximal lesions spare some of the more distally innervated muscles while affecting others
|
|
|
What is the innervation of flexor pollicis brevis?
|
both median and ulnar n.; C8-T1
|
|
|
What is the innervation of adductor magnus?
|
both obturator n. and sciatic n. L2-3-4
|
|
|
How does relaxation occur after muscle contration?
|
Ca++reuptake in SR by calsequestrin
|
|
|
What are the roots for the ilioinguinal n?
|
L1-2
|
|
|
What are the roots for iliohypogastric n. ?
|
L1
|
|
|
What are the roots for posterior cutaneous n. of thigh?
|
S2-3-4
|
|
|
What are the roots for pudendal n?
|
S1-2-3
|
|
|
What are the 3 types of MGA?
|
All median to ulnar cross-over in forearm. 1) ADM 2) FDI *most common 3) thenar muscles
|
|
|
How are the 2 muscle fiber types different?
|
Type 1 slow oxidative
Type 2 fast glycolytic 2a fatigue resistant 2b fast-fatiguing |
|
|
What are the muscles innervated by the distal deep palmar motor branch?
|
4 dorsal interossei (away from middle finger)
3 palmar interossei (adduct to middle finger) adductor pollicis flexor pollicis brevis deep head |
|
|
What are the different (4) types of lesions of UNW (ulnar neuropathy at the wrist)?
|
1. distal deep palmar motor branch no sensory
2. proximal deep palmar motor branch- all muscles of distal + hypothenar no sensory 3. superficial sensory 4. proximal guyon's canal (deep palmar+ superficial sensory) |
|
|
What nerve conduction studies prove UNW?
|
conduciton block between wrist and palmar stimulation for FDI & ADM
inching techniques conduciton velocity slowing across the wrist DML FDI >6 msec or 130% normal |
|
|
What studes are consistent with UNW?
|
1. 2nd lumbrical-interossei comparison >0.4 msec difference
2. DML FDI > 4.5 msec 3. comarison DML FDI to ADM >2 msec difference |
|
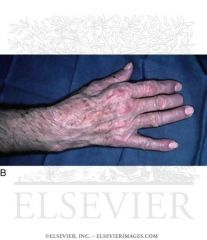
What nerve is involved and why?
|
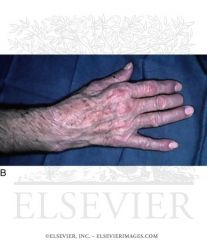
Wartenberg's sign
Ulnar neuropathy Weakness of the 3rd palmar interossei leading to abduction of the fifth digit |
|

This patient was asked to extend fingers (DIP/PIP). Name the nerve involved.
|
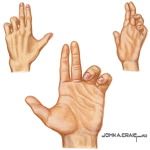
Benediction hand. Ulnar nerve. Weakness of teh 3rd & 4th lumbrical cannot extend DIP/PIP. Abduction of the thumb and 2nd digit due to weakness of adductor pollicis and FDI
|
|
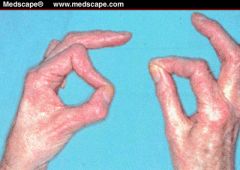
This patient was asked to hold a piece of paper between the thumb and index finger. Name the nerve involved.
|
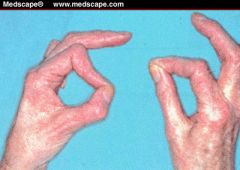
Froment's sign. Ulnar nerve lesion due to weakness of adductor pollicis which is compensated by the FPL and FDP 2,3
|

