![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
7 Cards in this Set
- Front
- Back
|
Aims for payment systems
|
1) Efficiency (static and dynamic)
2) Equity/Access 3) Cost-effectiveness 4) Quality 5) Robustness |
|
|
What is a P4P system?
|
A system which providers are paid by performance indicators.
|
|
|
What is a fee-for-service system?
|
A system in which providers are paid by volume measures
|
|
|
Why is a fee-for-services system more dominant?
|
P4P is harder to measure (health is hard to measure), and fee-for-service is more efficient. When there is a high correlation between input and output, FFS is better.
|
|
|
What are the complications of a variable payment system (ie FFS)?
|
1) Supplier induced demand
2) Over-provision of services |
|
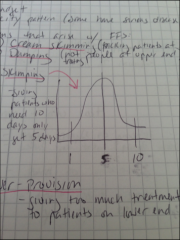
What are some complications of a prospective system (costs not reimbursed, ie DRG)?
|
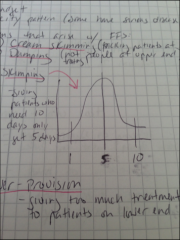
1) Cream skimming - Over provision of services to low severity patients
2) Skimping - Under-provision of services to high severity patients 3) Dumping - Avoidance of high severity patients 4) Over-provision - Giving too much treatment to patients at lower end |
|
|
Special characteristics of the health care market?
|
1) Asymmetric info - imperfect info
2) Uncertainty - Imperfect information, most important factor influencing physician behavior (Wennburg, 1985) 3) Non-repeat business 4) Non-tradeability of goods - goods and services that cannot be re-sold. They are rival goods. |

