![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
33 Cards in this Set
- Front
- Back
|
Risk factors for PE from PIPOED II Study |
Surgery within the last 3 months
|
|
|
Vichows Triad |
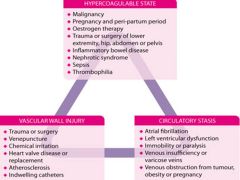
|
|
|
Inherited Risk Factors for PE |
Factor V Leiden mutation |
|
|
Deep Venous System of Lower Extremity |
Calf (distal DVT) -Anterior tibial -Posterior tibial -Peroneal
Thigh (proximal DVT) - Polpiteal vein - Superificial/deep femoral vein - External Illiac Vein |
|
|
Superficial venous system of lower extremity |
Greater/Lesser saphenous veins Perforating veins |
|
|
Differential Diagnosis of DVT |
Muscle strain, hematoma |
|
|
Wells Score for DVT |
- Active cancer (treatment ongoing or within previous 6 months or palliative) |
|
|
Mnemonic for Wells DVT Rule |
C3POR2D2
C3 Cancer Collateral superficial veins Calf Swelling
3PO Pitting oedema Odema of whole lege Previous DVT
+ Tenderness along deep venous sytem
R2 Recent immoblization/surgery Recent paralysis/paresis/plaster
D2 Diagnosis other than DVT as/more likely
|
|
|
Risk categories and probability of DVT in validation study |
Low (-2 to 0) = 3% Moderate (1 to 2) = 17% High (3 or more) = 75% |
|
|
DVT WORK-UP ALGORITHIM INCORPORATING WELLS SCORE |
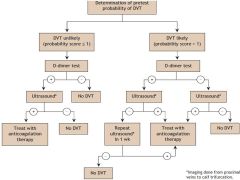
|
|
|
Long term Anti-coagulation |
- 3 months OAC for identified transient risk factor - 6 months OAC for 1st idiopathic/selected thrombophilia - Long term LMWH for Cancer associated - Recurrent at least 6 months (asses with thrombo)
|
|
|
Superficial thrombophlebitis |
Conservative management: NSAIDs/heat/compression stockings
Repeat U/S and if extending above knee then consider anticoagulation |
|
|
Phlegmasia alba dolens |
Massive DVT of deep illiofemoral system but with sparing of superifical collaterals
Milky white leg but no venous congestions |
|
|
phlegmasia cerulea dolens |
Painful inflamed blue leg with thrombosis of both deep and superficial that can progress to venous gangrene if capillaries thrombose |
|
|
Complications of DVT |
Venous insufficiency PE |
|
|
PERC Mnemonic |
H – Hormone (estrogen) use A – Age > 50 D – DVT or PE history (have they HAD CLOTS?) C – Coughing blood L – Leg swelling disparity O – O2 sats < 95% T – Tachycardia (>100bpm) S – Surgery or Trauma (recent) |
|
|
PERC Exclusion criteria |
|
|
|
Hampton hump |
Pleural based wedge shaped opacification that can indication pulmonary infarction secondary to PE |
|
|
Westermark sign |
Proximal pulmonary artery dilitation with regional oligemia secondary to PE |
|
|
ECG findings suggesting PE |
Sinus tachycardia S1Q3T3 new RBBB/RAD Anterior (V1-V4) T wave Inversions |
|
|
Age Adjusted D-Dimer Score |
If age >50:
Age in years X 10ug/L |
|
|
Wells Criteria for PE |
Hemoptysis 1.0 Malignancy (Tx within the last 6 mo/palliative) 1.0 Previous DVT/PE 1.5 Heart rate >100 beats/min 1.5 Immobilization or surgery (within 4 wk) 1.5 Suspected DVT 3.0 An alternative diagnosis is less likely than PE 3.0 |
|
|
Mnemonic for Wells Critiera for PE
|
SS PERCC
Suspicious for PE (3) Signs of DVT now (3) Pulse >100 (1.5) Extremity: Past DVT/PE (1.5) Recent surgery/immob (<4wk/>3d respectively) (1.5) Coughing up blood (1) Cancer (1) |
|
|
Wells Score Cutoffs |
Low (<2) 7% Moderate (2-6) 27% High (>6) 58%
Unlikely (0-4) 13% Likely (>4) 39% |
|
|
Rosens Algorithim to W/U Suspected PE |
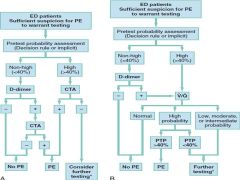
|
|
|
VQ Scan results and presence of PE |
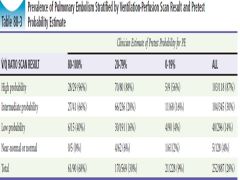
|
|
|
Factors that may impact accuracy of D-Dimer for PE
FALSE POSITIVE FALSE NEGATIVE |
False-negative D-dimer
|
|
|
Comparison of the Advantages and Disadvantages of CTPA vs VQ Scan |
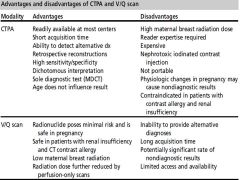
|
|
|
ROSENS APPROACH TO PE RISK STRATIFICATION AND TREATMENT |

|
|
|
Indications for IVC Filter placement |
Contraindication to anitcoagulation DVT/PE in a patient with a complication of anti-coagulant therapy Free floating illiofemoral/caval thombosis Possible prophylaxis for high risk of PE |
|
|
Risk Categories for PE from JAMA Thrombolysis meta-analysis |
Low risk (HD stable and no evidence of RV dysfunction)
Intermediate risk (HD stable and objective evidence of RV dysfunction)
High Risk (HD unstable and/or SPP <90)
RV Dysfunction = Cardiac biomarkers or echocardiographic evidence |
|
|
PULMONARY EMBOLISM SEVERITY INDEX (PESI) |
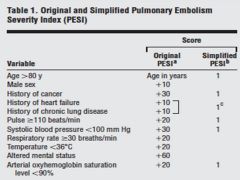
|
|
|
SIMPLIFIED PESI RISK STRATIFICATION |
0 = Low risk (1% mortality) 1 and more = High risk (10% mortality) |

