![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
22 Cards in this Set
- Front
- Back

Diagnosis?
A) Sunburn B) Allergic contact dermatitis C) Irritant contact dermatitis D) Thermal burn E) Dermatomyositis |

B) Allergic contact dermatitis to unknown plant
|
|
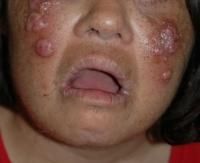
Correctly match disease and type of infiltrate.
A) Atypical mycobacterial infection - granulomatous B) Sweet's syndrome - neutrophils C) Atypical fibroxanthoma - histiocyte-like spindle cells D) Tuberous xanthoma - foam cells |
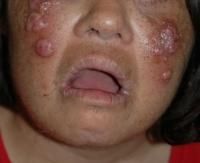
B) Sweet's syndrome
|
|
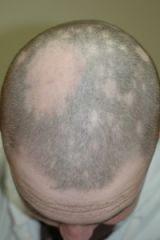
Diagnosis and clinical sign?
A) Trichotillomania - varying lengths of hair in segments with alopecia B) Tinea capitis - fine scale and post-auricular lymphadenopathy C) Alopecia areata - exclamation point hairs D) Non-scarring alopecia - normal ostia E) Two of the above |
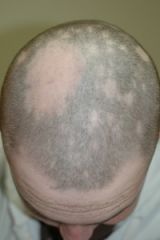
E) Two of the above - alopecia areata is a non-scarring alopecia with exclamation point hairs and nail pitting. Check for thyroid disease.
|
|
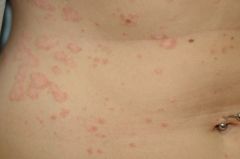
Diagnosis?
A) Disseminated granuloma annulare B) Tinea corporis C) Guttate psoriasis D) Subacute cutaneous lupus E) Mycosis fungoides |
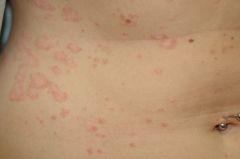
C) Guttate psoriasis - classically develops post streptococcal infection. Elevated anti-DNAse, ASOT or streptozyme. Often remits in children, but persists or develops into plaque psoriasis in adults.
|
|
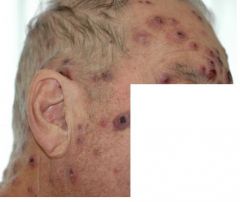
Morphology?
A) Dermal plaques wtih edema, pseudovesiculation and pustules B) Wheals that last longer than 24 hours and resolve with scarring C) Violaceous exophytic nodules that can ulcerate D) Papules to plaques that ulcerate; gun metal gray rolled border. |
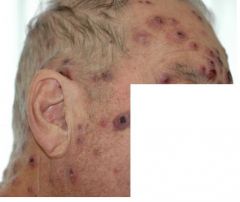
A) Dermal plaques wtih edema, pseudovesiculation and pustules - bullae may be rarely present as well.
Sweet's syndrome. |
|
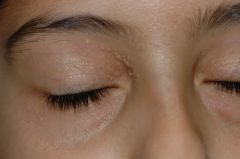
Diagnosis?
A) Sebaceous hyperplasia B) Trichoepithelioma C) Milia D) Molluscum contagiosum |
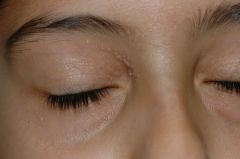
C) Milia. Preceding EMLA cream with electrodessication may be of benefit in conjunction with a comedone extractor.
|
|
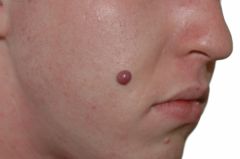
Diagnosis?
A) Spitz nevus B) Pyogenic granuloma C) Kaposi sarcoma D) Bacillary angiomatosis E) Blue nevus |
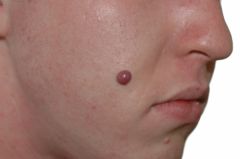
B) Pyogenic granuloma - abnormal response to tissue injury with aberrant proliferation of blood vessels (lobular capillary hemangioma)
|
|
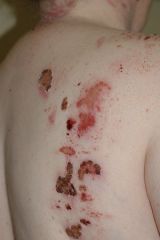
Diagnosis?
A) Bullous pemphigoid B) Pemphigus vulgaris C) HSV in an immuno-compromised host D) Factitial ulcer (self-induced) |
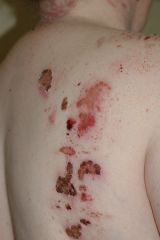
D) Factitial ulcer (self-induced) - this is a diagnosis of exclusion.
|
|
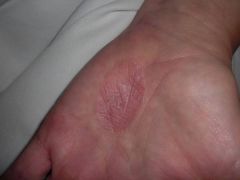
Diagnosis
A) hand eczema B) dishidrotic eczema C) Pompholyx D) palmar psoriasis E) tinea manum |
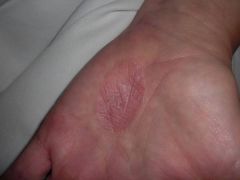
D) Palmar psoriasis - extremely well defined scaly palmar plaque. Hand eczema and psoriasis can be difficult to distinguish clinically and histologically. Treatment for both are the same (topicals - topical PUVA - systemic MTX or retinoid such as acitretin / isotretinoin / alitretinoin)
|
|
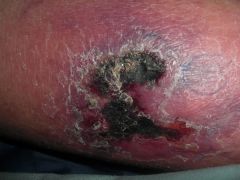
Morphology and diagnosis?
A) Necrotic plaque - vasculitis B) Ulcer with hemorrhagic crust, gun-metal gray scalloped border - pyoderma gangrenosum C) Painful punched out ulcer - arterial ulcer D) Angulated, retiform ulcer with background inflammation - calciphylaxis |
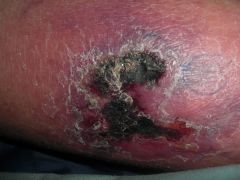
D) Angulated, retiform ulcer with background inflammation - calciphylaxis. Renal dialysis patient who presented extremely painful ulceration over the shins. Deep incisional biopsy showed intravascular calcium deposition with von Kossa stain.
|
|
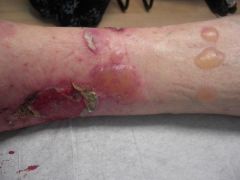
Diagnosis?
A) Porphyria cutaneous tarda B) Bullous pemphigoid C) Pemphigus vulgaris D) Epidermolysis bullosa acquisita E) Bullous diabeticorum |
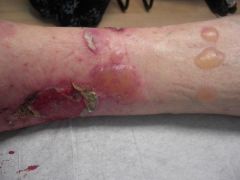
B) Bullous pemphigoid - tense, serous to hemorrhagic bullae; various stages of evolution (bullae to deroofed,crusted, healing areas with serosanguinous crust); Targets are hemidesmosomal proteins BPAg1 and BPAg2 in the dermo-epidermal junction.
|
|
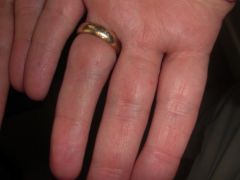
What are findings of this genodermatoses?
A) Multiple fibrofolliculomas / trichodiscomas wtih renal disease B) Mucosal lentigines with GI malignancy C) Basal cell carcinomas, falx cerebri calcification, odontogenic keratocysts, bifid ribs, facial dysmorphism (frontal bossing, hypertelorism, coarse facies) D) Basal cell carcinomas, follicular atrophoderma, hypertrichosis, and hypohidrosis of the face and the head |
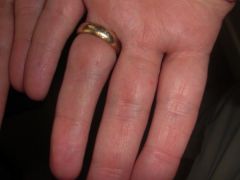
C) Basal cell carcinomas, falx cerebri calcification, odontogenic keratocysts, bifid ribs, facial dysmorphism (frontal bossing, hypertelorism, coarse facies)
Basal cell nevus syndrome (nevoid basal cell carcinoma syndrome / Gorlin's syndrome) |
|
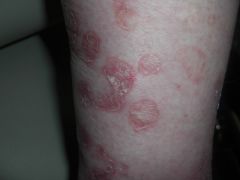
What are the histiologic features?
A) Cornoid lamellae B) Psoriasiform hyperplasia with hyperkeratosis, neutrophilic microabscesses, vascular dilation and parakeratosis C) PAS positive stain D) Keratinocyte atypia E) |
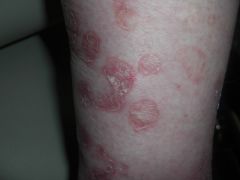
A) Cornoid lamella; diagnosis is superficial actinic porokeratosis; note depressed nature of lesions
|
|
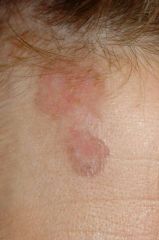
Diagnosis?
A) Superficial basal cell carcinoma B) Invasive squamous cell carcinoma C) Squamous cell carcinoma in situ (Bowen's disease) D) Amelanotic superficial spreading melanoma E) Pigmented basal cell carcinoma |
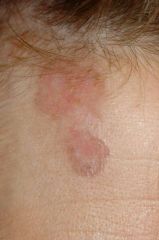
A) Superficial basal cell carcinoma - atrophic, pearly appearance to inferior portion of lesion
|
|
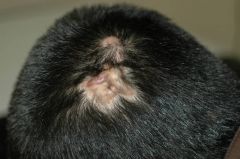
Diagnosis?
A) Acne keloidalis B) Keloid scar C) Cutaneous metastases D) Dissecting folliculitis of scalp E) Kerion |
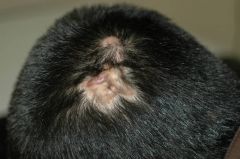
D) Dissecting folliculitis of scalp
|
|
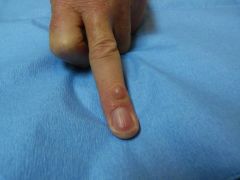
Diagnosis?
A) Epidermoid cyst B) Acquired digital fibrokeratoma C) Digital mucous cyst D) Heberden node E) Tophaceous gout |
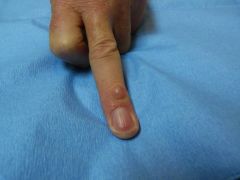
C) Digital mucous cyst - aspiration reveals gelatinous mucinous material. Histopathology shows a pseudocyst with fibrous capsule and myxoid stroma; Gelatinous material stains for acid mucopolysaccharides with Alcian blue / colloidal iron
|
|
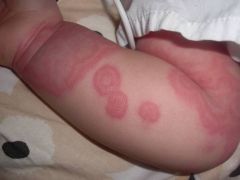
Diagnosis?
A) Erythema multiforme B) Urticaria C) Erythema gyratum repens D) Steven's Johnson Syndrome E) Toxic epidermal necrlysis |
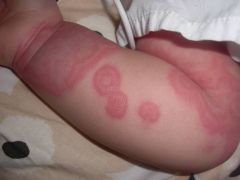
B) Urticaria - migratory, pruritic violaceous, edematous targetoid plaques with dusky centres; involvement of face, trunk, legs and abdomen (not shown). Consider "urticaria multiforme" or atypical urticaria
|
|
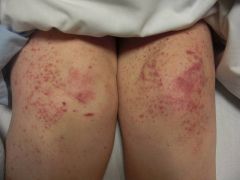
Diagnosis?
A) Small-vessel vasculitis B) Viral exanthem C) Embolic phenomenon D) Lichen planus E) Leukemia cutis |
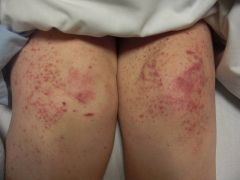
A) Small-vessel vascultis with palpable violaceous purpura, often in dependent, peripheral areas. Causes: idiopathic, drug, post-infectious, malignancy, small-to-medium vessel vasculitides, autoimmune connective tissue disease
|
|
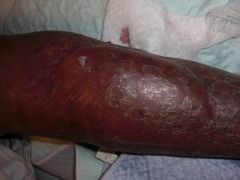
Diagnosis?
A) Bullous pemphigoid B) Coma bullae C) Epidermolysis bullosa acquisita D) Friction blister E) Bullous disease of diabetes |
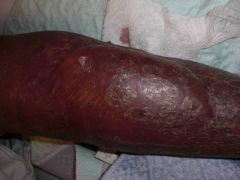
E) Bullous disease of diabetes - easily induced by trauma or occur spontaneously; generally asymptomatic and heal over weeks; recurrence frequent
|
|
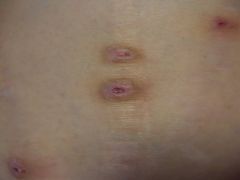
Which category best describes the following lesions?
A) Infectious B) Granulomatous C) Papulosquamous D) Eczematous E) Infiltrate malignancy |
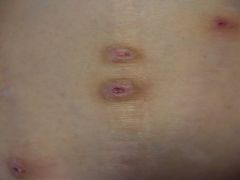
D) Eczematous - biopsy proven prurigo nodularis in a liver transplant candidate; note central excoriated erosions in lesions
|
|
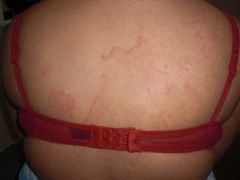
What is the diagnosis?
1) Psoriasis 2) Subacute lupus erythematosus 3) Tinea incognito 4) Tinea corporis 5) Two of the above |
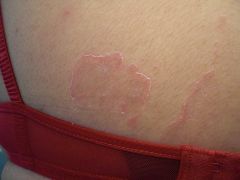
Biopsy showed changes of psoriasis & lupus. Patient was started on hydroxychloroquine.
|
|
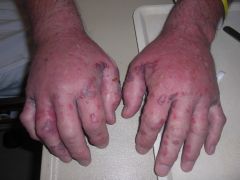
What is the diagnosis?
1) Papular urticaria 2) Arthropod assault 3) Bullous pemphigoid 4) Vasculitis 5) Well's syndrome |
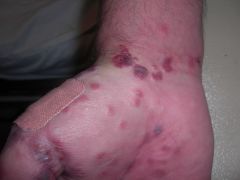
Well's syndrome - biopsy proven! Painful, edematous extremities with vesicles on a violaceous base. Healthy otherwise. Lab work showed peripheral eosinophilia. Biopsy showed "flame figures." Started on tapering course of prednisone with significant improvement.
|

