![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
189 Cards in this Set
- Front
- Back
|
The “master” gland_________: controls function of other endocrine glands
|
Pituitary Gland
A pea behind optic chiasm |
|
|
Hormones Produced by Pituitary Anterior Lobe
|
a. Growth Hormone
b. Prolactin c. ACTH (adrenocorticotropic) d. TSH (thyroid stimulating hormone) e. FSH (follicle stimulating hormone) f. LH (luteinizing hormone) |
|
|
Hormones Produced by Pituitary Intermediate Lobe
|
a. MSH (melanocyte stimulating hormone)
|
|
|
Hormones Produced by Pituitary Posterior Lobe
|
a. Oxytocin (pregnancy/delivery)
b. ADH (aka vasopressin) |
|
|
T/F Pituitary tumors are mostly FUNCTIONAL, where the pitutary still produces hormone
|
T
|
|
|
Galactorrhea (milk flowing from breast), and amenorrhea (cessation of menstruating) indicate a problem with what hormone?
|
Prolactin
|
|
|
a problem with the production of ACTH can lead to what condition
|
Cushing’s syndrome
|
|
|
Most common pituitary tumor leads to
|
Hyperprolactinemia
|
|
|
The hormone prolactin is downregulated by ___________ and is upregulated by _________
|
dopamine
estrogen |
|
|
Prolactin secretion in the pituitary is normally suppressed by the brain chemical _____. Drugs that block the effects of _________ at the pituitary or deplete dopamine stores in the brain may cause the pituitary to secrete prolactin.
|
dopamine
|
|
|
__________ is used to treat PRL secreting tumors
|
Bromocriptine
|
|
|
___________ is secreted by neurons in hypothalamus/posterior pituitary
Its function: acts on distal renal tubule to retain water in dehydration/reabsorb H2O from kidneys |
Anti-Diuretic Hormone
|
|
|
Too little ADH leads to
|
Diabetes Insipidus, no H2O gets reabsorbed
|
|
|
_______________ – most common form of thyroiditis, iodine levels are not sufficient, characterized by gradual thyroid failure because of autoimmune mediated destruction of gland.
|
b. Hashimoto’s thyroiditis
|
|
|
A patient who comes in with these symptoms probably has:
a. Reduced basal metabolic rate: weight gain b. Cold intolerance c. Fatigue, weakness, lethargy d. Slow pulse e. Decreased reflexes, somnolence f. Constipation g. Myxedema: puffiness of face, hands, feet h. Dry skin, coarse hair, thinning of eyebrows |
HYPOthyroidism
|
|
|
__________ can occur during severe hypothyroidism; it is often triggered by stress, Infections, alcohol, drugs
|
Myxedema Coma
c. Respiratory failure, hypothermia, hypoglycemia d. Sluggish cerebral perfusion, coma e. Death. |
|
|
____________ has the classic triad: diffuse goiter, ophthalmopathy and dermopathy.
|
HYPERthyroidism
|
|
|
if patient has an increase in TSH, decrease in Free T3 & T4 they probably have
|
hypothyroidsm
|
|
|
If patient has an increased Free T3 & T4 and decrease in TSH they probably have
|
HYPERthyroidism
|
|
|
Thyroid Storm is:
|
Thyroid Storm
d. Sudden exacerbation of hyperthyroidism e. Fever, agitation f. Fast heart rate g. Low blood pressure h. Coma, death |
|
|
Parathyroid Glands-imp for blood __________ levels
|
calcium
|
|
|
Hyperparathyroidism – hallmark sign:
|
hypercalcemia
1. Excess PTH is produced |
|
|
If a patient has these symptoms, he probably has:
a. Tetany, muscle twitching b. Laryngeal spasm c. Seizures d. Blurry vision e. Early PSC f. Alopecia g. Trousseau’s sign |
2. Hypocalcaemia
Trousseau sign of latent tetany is a medical sign observed in patients with low calcium.[1] This sign may become positive before other gross manifestations of hypocalcemia such as hyperreflexia and tetany, but is generally believed to be more sensitive than the Chvostek sign for hypocalcemia. To elicit the sign, a blood pressure cuff is placed around the arm and inflated to a pressure greater than the systolic blood pressure and held in place for 3 minutes. This will occlude the brachial artery. In the absence of blood flow, the patient's hypocalcemia and subsequent neuromuscular irritability will induce spasm of the muscles of the hand and forearm. The wrist and metacarpophalangeal joints flex, the DIP and PIP joints extend, and the fingers adduct. |
|
|
The VI. Adrenal Glands are responsible for what hormones?
|
(adrenal cortex--> aldosterone, cortisol and androgens;
adrenal medulla--> NE and NE |
|
|
What is Cushing’s Disease?
|
high levels of ACTH from pituitary lead to adrenal hyperplasia and high levels of cortisol; not an adrenal problem but pituitary problem
|
|
|
T/F Cushing's Disease is a problem in the adrenal glands
|
FALSE
it is a porblem of the pituitary! high levels of ACTH from pituitary |
|
|
T/F Cushing's Syndrome is a problem in the pituitary glands
|
F!!
Its due to ADRENAL problems cortisol production by adrenal adenoma or carcinoma, or exogenous steroids. will have low levels of ACTH, high cortisol |
|
|
3. Clinical Features of _______________ include:
a. Facial Plethora (Moon Faces) b. Central Obesity c. Buffalo Hump d. Supraclavicular fat pads e. Purple Striae f. Mild hypertension g. Impaired glucose tolerance (20% DM) h. Androgen excess |
Cushing's
|
|
|
Adrenal Insufficiency – primary Addison's Disease is due to
|
adrenal suppression *imp; no ACTH secretion so no cortisol
|
|
|
A cortisol Deficiency leads to–
|
secondary Addison disease, rapid decrease or withdraw of glucocorticoids.
|
|
|
Pheochromocytoma:
|
1. Catecholamine producing adrenal tumor
a. Epinephrine and norepinephrine involvement |
|
|
One of the most common cause of amenorrhea
|
a. Turner Syndrome
i. iii. Do not have ovaries iv. No estrogen - no secondary sexual characteristics v. Short stature vi. Diagnosis usually around 14 y/o |
|
|
T/F In Testicular Feminiziation syndrome, the body does not make testosterone
|
FALSE
i. 46XY genotype ii. No androgen receptor in peripheral tissues; body making testosterone just not recognizing it |
|
|
b. Hypothalamic Amenorrhea occurs due to
|
. Decreased production of GnRH
ii. Physiologic stress iii. Psychologic stress iv. Physical stress |
|
|
80% of blood traveling to the eye goes to the
|
CHORIOD
cools down retina and supplies it with neutreints. SYMPATHETIC control |
|
|
an example of sympathetic control in terms of blood travelling to the eye involves
|
blood flow to choriod
|
|
|
15% of blood traveling to the eye goes to
|
the iris and ciliary body to make aqueous --> AUTOREGULATION
|
|
|
The retina functions in _________ mode and therefore must extract every amount of oxygen possible in the 5% of blood that travels to the eye
|
starvation
|
|
|
T/F Optic nerve and choiriod circulatio nare BOTH under SYMPATHETIC control
|
T
|
|
|
T/F The retina blood supply is controlled by SYMPATHETIC control
|
FALSE
AUTOREGULATION |
|
|
Outer blood barrier is the
|
tight junctions between RPE cells
|
|
|
Inner blood barrer is the
|
tight junctiosn between endothelial cells surrounding branches of CRA
|
|
|
A pre-hypertensive patient would have a blood presure of
|
120-139 mm Hg
80-89 mmHg |
|
|
HTN Stage 1 blood pressure:
|
140-159 mm Hg
90-99 mm Hg |
|
|
HTN Stage 2 blood pressure:
|
>160 mm Hg
>100 mm Hg |
|
|
If you have a pre-HTN patient what MYST you do?
|
Refer to PCP!
|
|
|
Grade 1 HTN retinopathy
|
Retinal vessel narrowing
>.90 and <110 distolic BP |
|
|
Grade 2 HTN retinopathy
|
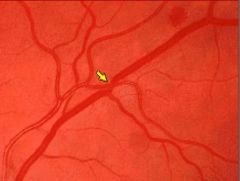
Nicking of vessles
>90 and < 110 diastolic BP |
|
|
Grade 3 HTN retinopathy
|
CWS, hemes, lipid exudeates
>110-115 diastolic BP |
|
|
Grade 4 HTN retioapthy
|
CWS, hemes, lipid exdues, AND optic disc sweeling
>130 diastolic BP |
|
|
AS 3
|
copper wiring
|
|
|
AS 4
|
silver wiring
|
|
|
A hemmorrage with a white center is known as a
|

Roth spot
|
|
|
3 ways that HTN presents in the eye
|
autoregulation is altered --> HTN retinopathy
sympathetics are altered leading to ischemia --> HTN choroidopathy HTN neuropathy |
|
|
When HTN effects sympathetics and causs ischemia of choriocapiris, RPE dies and changes shape, which leads to
|
Seigrist streaks (sleroised vessles) or Elshnig spots (RPE scar)
|
|
|
T/F Vision loss depends on how long BP has been elevated
|
T
elevation is chronic, photoreceptors can die and result in scotoma |
|
|
T/F Macular edema due to HTN is treated with focal grid laser
|
FALSE
only therapy is to decrease BP!! |
|
|
HTN that occurs during pregnancy is known as
|
pre-eclampsia
|
|
|
Malignant Hypertension occurs when BP is
|
> 210/110
It differs from other complications of hypertension in that it is accompanied by papilledema. |
|
|
T/F You must decrease BP SLOWLY or you can cause a stroke of te choriod and optic nerve
|
T
|
|
|
S HTN urgency occurs when there is a large increase in BP with a diastolic elevation greater tha
|
120-130 mmHg
|
|
|
________ has been associated with malignant arterial hypertension
|
HLA-B15
|
|
|
Elevated BP leads to what three prevelant diseases?
|
coronary heart disease, stroek, and renal disease
|
|
|
Most common cause of HTN
|
ESSENTIAL/no known cause
|
|
|
T/F In elderly patients, HTN is more common in females
|
T
|
|
|
If you see grade 3/4 HTN in patient you must think
|
secondary problems exists
|
|
|
Retinal Arterial Macroanuerysm
|

vessel wall is weak troughout life, when bP increases, it ballons out and may bleed, which can cause exudates
|
|
|
The optic nerve swells by the _________ rule
|
ISNT
inferior (thickest) swells first |
|
|
HTN is a risk factor for
|
Carotid artery disease
CRVO RVO NAION Retinal Arterial MAcroaneurysm Glaucoma worsen diabetic retinopathy AMD |
|
|
In DM, BP gial is to be under
|
130/75
|
|
|
First line of treatment for high blood pressure
|
diuretics
Especially beneficial for african americans, and people who have HEART failure |
|
|
The site of Central Retinal Vein occlusion is the
|
lamina crbrosa
|
|
|
The site of Branch Retinal Vein occlusion is in
|
the retina at A/V crossings
|
|
|
T/F Ischemic CRVO is morelikely to develop neo of the iris
|
T
BRVO neo is more likely to occur in retina |
|
|
In ischemic _____, the VA is 20/200 or worse, APD is present and blood blocks ability to see choroid
|
CRVO
|
|
|
Accroding to the BRVO study, if macula edema is present after 4 months and VA is worse than 20/40 ___ will improve edema and VA
|
focal grid therapy
|
|
|
Perfusion pressure is
|
the mean blood pressure in the OHTHALMIC artery- IOP
BLood pressure of ophthalmic artery is usually around 65 |
|
|
BLood pressure of ophthalmic artery is usually around
|
65 mm Hg
|
|
|
T/F an IOP of 70 can cause atery or vin occlusion
|
T
|
|
|
What can result from Pheochromocytoma?
|
Hypertensive choroidpathy
|
|
|
What test do you order to check kidney function?
|
Creatinine, BUN, urinalysis
|
|
|
What tests for polycythemia?
|
cbc
|
|
|
If patient has HTN grade 3 or 4, what has been overcome?
|
The inner BRB and autoregulation
|
|
|
What grade of HR is a medical emergency?
|
4
|
|
|
What does AS correlate to?
KNOW |
age and HTN
|
|
|
What is diastolic bp seen in grade 3?
|
110-115 mm Hg
|
|
|
What diastolic bp is seen in HTN grade 4?
|
> 130 mm Hg
|
|
|
T/F You do not tend to get AS of 3 or 4 in essential HTN, but you do see it in malignant
|
T
|
|
|
____- blockage of carotid artery is required to cause effects in the eye, but may occur at 70% of patient has carotid artery disease
|
90%
|
|
|
Cause of HIV/Aids
|
retro virus that depletes CD4 population of T lymphocytes
|
|
|
AIDS occurs when CD4 counts is less than ________ in a person who is HIV positive
|
200 ul
|
|
|
Normal CD4 ratio is around
|
800-1400 mm
|
|
|
3 transmission routes of HIV
|
1. SExual contact
2. Percutaneous inolcuation of blodo or other infected materials 3. Exposure to infected blood and tissues during birth or infected breast milk |
|
|
______% of AIDS cases globally are heterosexual
|
60%
|
|
|
Initial Stage of HIV
|
become HIV + during this phase
Mild influenza like illness, 4-12 eeks after becoming infected may not have a positive test for the inital 6 weeks |
|
|
Chronic stage of IV
|
latent period, may last ov average for 10 years
|
|
|
THe most common systemic opportunistic infection of AIDS patients, aka the "marker" disease is
|

Pneumocystitis carinii pneumonia PCP
Choroidal pneumocytosis appears as MULTIFOFCAL, yellow, round deep choroidal lesions on-half to two disc diametser in size located in posterior ole. |
|

What is this a picture of?
|
Choroidal pneumocytosis
seen in HIV/AIDs patients most common systemic infection |
|
|
Bacterial diseases that are common in HIV/AIDS
|
Staph, strep
Tuberculosis Pulmonary Tuberculosis (>80%) Extrapulmonary TB |
|
|
Ocular manifestations of TB include
|
Tubercules (granulomas)
Phylcyenulosis, smal unilateral or ilateral white nodules in bulbar conj (Treatment: topical steriod) Uvetitis Scleritis Optic neuropathy |
|
|
In order to diagnosis TB patient must get
|
a PPD and chest x ray
|
|
|
First line treatment of TB
|
Rifampin, isoniazid. Therapy is a minimum of 6 motnhs for standard, 9 motnhs for those with HIV and AIDS,
|
|
|
_______________- is common in immunocompetant self limited infection and causes unremitting diarrhea in AIDS
|
cryptosporidium
|
|
|
prevalance of in HIV patients is higher than in general population. It is known as the GREAT MAQUERADER
|
Syphilis
due to a spirochete infection passes through many stages |
|
|
Primary stage of sphyilis
|
skin leasions, painless papule, heals in 2-6 weeks
see bilateral lymphadenopathy |
|
|
secondary stage of Sphyllis
|
see conjunctivitis, interstitial keratitis, ANTERIOR uveitis (most common), posterior uveitits, optic nerve head involvement
BRVO, CRVO CRAO |
|
|
Treatment for sphyilis includes
|
Benzathine PCN
Doxycycline or tetracline |
|
|
Most cmmon fungal infection is located
|
oral, esophageal
|
|
|
Most common neuroplasm in AIDS
|
Karposi sarcoma, caused by papiloma virus
lesions interfere with eyelids, tear film, cornea, mitility |
|
|
This infection found commonly in HIV has a lag between infection and developing antibody 6 weeks to 6 months
|
Non-hogkin's lymphoma
|
|
|
________ is used to track the progression of HIV
|
Viral Load testing
two types of viral load tests measure HIV RNA in a sample. THESE ARE NOT DIAGNOSTIC tests, just used in adjuct to CD4 count. VIRAL load test ONE measure RNA INDIRECTLY Viral load test TWO measure RNA DIRECTLY |
|
|
VIRAL load test ONE measure _________-
|
RNA INDIRECTLY
|
|
|
Viral load test TWO measure _________
|
RNA DIRECTLY
|
|
|
The low baseline viral load HIV RNA test is __________
The high baseline viral laod is any number hier than |
500 or fewer
40,000 to 100,000 copies Testing should include 2 viral load tests taken 2-4 weeks apart |
|
|
______% of AIDS patients have eye signs
|
75
|
|
|
Most common ocular opportunistic infection that effects approximately 30% of patients and is the LEADING cause of AIDS related blindess is
|
Cytomeglaovirius Retinitis
usually seen when CD4 is below 100 cheese and ketchup fundus |
|
|
Indolent form of CMV is
|
peripheral granular opacities with hemorrhages
|
|
|
Fulminant form of CMV is
|
confluent area of necrosis with associated hemorrages along vascular arades
|
|
|
Retinal detachmesn occur in ______ of pateitns with CMV retinitis
|
1/3
|
|
|
What treatment is used with CMV
|
Valgemcclovir
Gancyclovir |
|
|
The most common form of retinoschoroiditis in AIDS patient
|
CMV
|
|
|
The second most common form of retinochoroiditis in aids is
|
Toxoplasmosis
|
|
|
How does Toxoplasmosis appear in AIDS patient differently than the rest of the population
|

see BILATERAL multiple large retinal lesions
Genera pop. only have it unilaterally |
|
|
t/f systemic steriods are contrainidcated for AIDS patients
|
T
|
|
|
What is PORN?
|

Progressive Outer REtinal Necrosis
diffuse uvetitis characterized by posterior pole and peripheral necrotizing retinitis and vasculitis in AIDS patients HZV is a major cause of PORN See it bilaterally and more progressive than CMV retinitis in aIDS patients They are multifocal deep yellow/white, retinal infiltrates with minimal vitritis leading to rapid confluence and full thickness retinal necrosis Treat with gancyclovir with foscarnet |
|
|
How do you treat PORN?
|
Progressive Outer REtinal Necrosis
treat with gancyclovir and foscarnet |
|
|
Where is Histoplasmosis most prevalent?
|
Ohio/Mississippi river valleys
See granulomatous reaction, caseating necrosis, or calcification. Looks like TB Triad inclues: Exudative maculopathy, atophic peripheral chioretinal lesions, peripaillary scars |
|
|
What is the Triad of pathology for ocular histoplasmosis syndrome?
|
Triad inclues: Exudative maculopathy, atophic peripheral chioretinal lesions, peripaillary scars
MAY see neovascular membrane from breaks in BRUCH's membrane |
|
|
How is Histoplasmos treated?
|
Amphotericin B, primary antifungal drug IV
Ketoconazole, oral Pred Forte can be used with stromal involvement |
|
|
What do we typically see with patients who have Molluscum contagiosum?
|
Raised vesicular lsion with chronic filicular conjunctivitis
Tend to be multiple and bilateral in AIDS patients. Usually need to be lanced |
|
|
If you see Herpes Zoster Varicella in a patient younger than 40 what must you think?
|
Immunocompromised patient, possible AIDS
See Hutchinson sign Treated with Acyclovir Valacyclovir Bacitracin or erythromycin topically |
|
|
If your pt has a CD4 count of 200-500 when should you see them?
IF pt has less than 200? |
every 6-12 months
Every 2-6 months |
|
|
How is AIDS treated?
|
HAART, highly active antiretroviral therapy
|
|
|
Adverse side effects with HAART?
|
Lactic acidosis/hepatic steatosis
Hepatotoxicity Hyperglycemia ROIL3H Fat maldistribution Hyperlipidemia Increased bleeding in hemophiliacs Osteonecrosis Rash |
|
|
___________: period of ventricular contraction
____________: period of ventricular relaxation |
Systole
Diastole |
|
|
Cardiac output: amount of blood pumped by the heart every ________
|
minute
|
|
|
_______ volume: amount of blood pumped by the heart each systole
|
Stroke
|
|
|
Dyspnea =
|
short of breath (at rest; on exertion)
|
|
|
Paroxysmal nocturnal dyspnea =
|
sudden dyspnea(Shortness of breath) in the middle of the night
|
|
|
_______ = dyspnea when lying flat
|
Orthopnea
|
|
|
________________ = Systolic - Diastolic
|
Pulse pressure
|
|
|
Hypertension: systolic BP >=_______- mm Hg AND/OR diastolic BP >=_______ mm Hg
|
140
90 |
|
|
T/F In persons>50 years, a SBP>140 is a more important CVD risk factor than the diastolic BP
|
T!
|
|
|
HTN first line drug?
|
Diuretic is the First-line treatment, first choice
Act in the kidney by increasing salt wasting through the urine |
|
|
Examples of ________ are: lasix, HCTZ, aldactone, bumex
|
diuretics
|
|
|
______________:Decrease the strength of heart’s contraction
Decrease the heart rate Examples: atenolol, metoprolol, carvedilol |
Beta-blockers –
|
|
|
Ca++ blocker examples
|
Examples: nifedipine, diltiazem, amlodipine
|
|
|
_____________- –
Increase sodium wasting in the urine and relax blood vessels Examples: captopril, enalapril, lisinopril, ramipril, fosinopril |
ACE inhibitors/ARBs
|
|
|
Diabetics and pts with renal failure with protein in the urine who suffer from Hypertension would do best on what drug?
|
ACE inhibitors
|
|
|
Symptoms of the metabolic syndrome include
|
Abdominal obesity (men>40 in; women>35 in)
Atherogenic dyslipidemia (high LDL, low HDL (<40 in men, <50 in women, high tryglicerides (>150 mg/dL) - Foster plaque buildups in arterial walls) Glucose intolerance High blood pressure (>130/85 mmHg) Elevated markers of inflammation |
|
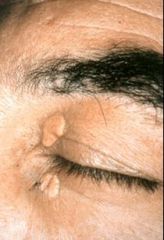
What is this a picture of?
|
Xanthelasma
|
|
|
What are statins useful for?
|
Statins – Very well studied; safe; first-line
Inhibit cholesterol formation by your body. Reduce LDL by up to 60% Examples: simvastatin, pravastatin, atorvastatin, rosuvastatin |
|
|
________–
Increase trygliceride degradation and uptake by the liver. Decrease triglycerides by up to 30-50% |
Fibrates
gemfibrozil, fenofibrate |
|
|
________ – It is vitamin B3
Increases HDL by 30% |
Niacin
|
|
|
What are Resins?
|
Resins –
Bind to dietary cholesterol and inhibit its absorption. Decrease LDL by 20% Examples: colestipol, colestyramine |
|
|
________–
Inhibits cholesterol absorption without binding to it. Decreases LDL by 25% |
Ezetimibe
|
|
|
CAD pathogenisis
|
Initial step : “fatty streak” - subendothelial accumulation of lipids and lipid-laden macrophages (“foam cells’)
LDL cholesterol is the major atherogenic lipid - oxidation of LDL particle is the rate-limiting step HDL cholesterol is protective Plaque progression - smooth muscle cells migrate into lesion - fibrous cap forms - calcified - vessel lumen becomes narrowed Most plaques remain stable or progress gradually Plaque rupture or hemorrhage - extrusion of lipids and tissue factors - cascade of events leading to intravascular thrombosis (unstable angina or MI) Factors producing enhanced plaque vulnerability : 1. soft lipid core 2. higher concentration of macrophages 3. thin fibrous cap |
|
|
________
Most useful noninvasive procedure for evaluating a patient with angina |
Stress test
|
|
|
Treatment for CAD
|
Nitrates: dilate coronary vessels (increase oxygen supply). Relieve the pain
Beta-blockers Calcium-channel blockers |
|
|
The Most Severe Heart Attack:
|
ST Elevation Myocardial Infarction (STEMI)
The most severe type of heart attack is caused by complete blockage of a coronary artery. Within several minutes irreversible damage occurs to heart muscle |
|
|
If the ECG shows no STEMI and the cardiac enzymes are normal, but angina is still suspected, the diagnosis may be _______________. It’s “unstable” because the blood flow through a coronary is no longer sufficient to supply the heart muscle, which is now starving.
|
unstable angina
|
|
|
MI treatment drugs are useful for
1Beta-blockers: 2Nitrates: _______ 3ACE-I: _________- 4Statins: ______________- |
1. (keep HR<60)
2.for symptomatic relief 3.especially if heart muscle is weak 4.for cholesterol management |
|
|
_________is the strongest predictive factor of mortality in CHF
|
Ejection factor
he fraction of blood pumped out of a ventricle with each heart beat |
|
|
Angiotensin II Receptor Blockers (ARB) are used when
|
When pt intolerant to ACEI
Proven reduction in morbidity and mortality In combination with an ACEI, may provide additional benefits Examples: valsartan, candersartan, losartan, irbesartan, telmisartan Do not cause cough and angioedema is much less common |
|
|
_______-- – Very well studied
From being contraindicated, they went on to being first-line treatment for CHF |
Beta-blockers
|
|
|
Transient loss of consciousness, due to decrease cerebral blood flow
|
Snycope
|
|
|
Causes of Syncope
|
Cardiac (18%): palpitations (arrhythmias), during exertion (HOCM, AS, MS, pulmonary HTN, atrial myxoma). Usually, no preceding symptoms
Neurologic (10%): seizures (different diagnosis) Orthostasis (8%): due to dehydration, medications (especially BP medications), diabetes, alcohol |
|
|
Grave's triad consists of
|
triad:
1. Hyperthyroidism with diffuse hyperplasia of the thyroid gland (goiter) 2. Infiltrative dermatopathy 3. Infiltrative ophthalmopathy (invading orbit) |
|
|
Cause of Grave's
|
Autoimmune disease
Hypersensitivity reaction with thyroid stimulation by the circulation of Abnormal thyroid stimulating immunoglobulins (TSI) |
|
|
T/F When pt has Grave's, inflammatory infiltrate of the orbital contents exclusive of the globe!
|
T
|
|
|
What tests should you order for someone who you think has Grave's?
|
. Laboratory testing:
1. Serum T4 (Thyroxine)* (KNOW) 2. Serum T3 (Triiodithyronine)* (KNOW) 3. Sensitive serum TSH test* (Thyroid stimulating hormone) (KNOW) |
|
|
How do you treat someone with Graves?
|
First line of treatment.
a. Tapazole, methimazol b. Propylthiouracil (PTU) c. Inderal, Propranolol (controls sympathetic over-activity; nervousness, eyelid twitching) 2. Surgery is last resort* |
|
|
_________ is the single most common cause of all bilateral and unilateral proptosis.
|
Grave's
|
|
|
Unilateral or bilateral proptosis (Hertel or Lute Results)
a. Minimal: ______ b. Moderate: __________ c. Marked: ______ d. ___difference between the eyes is clinically significant. |
a. 21mm – 23 mm
b.24 mm – 27 mm c. 28mm or more d. 2mm |
|
|
Grave's Eyelid retraction. Possible mechanisms include: (KNOW)
|
a. Direct inflammatory involvement of the levator muscle
b. Hyperactivity of the sympathetic nervous system with activation of Mueller’s muscle. c. Secondary over-action of the levator/ superior rectus complex in response to involvement and tethering of the inferior rectus muscle. |
|
|
Why would someone with Grave's show decreased VA?
|
Compressive optic neuropathy due to the thickened extraocular muscles at the orbital apex. Look for an APD when testing pupils.
|
|
|
T/F Grave's Disease can show a APD
|
T
Compressive optic neuropathy due to the thickened extraocular muscles at the orbital apex. Look for an APD when testing pupils |
|
|
How can you tell if Grave's disease is responsible for APD and decreased VA?
|
A CT scan will reveal why the patient has optic nerve compression.
Thick, enlarged muscle will be seen especially at the orbital apex. Usually the EOM’s are barely visible on CT. |
|
|
How do you treat GRave's disease proptosis
|
a. Prednisone 100 mg PO QD x 1-2 days with taper
b. Consider orbital decompression surgery |
|
|
How do you treat the optic neuropathy present in some pt's with Graves?
|
a. Prednisone 60-100mg PO QD with taper
b. Super voltage orbital radiation therapy c. Orbital decompression: Sight threatening infiltrative disease may need surgical compression including i. Removal of orbital floor and medial wall of the orbital cavity. ii. Once the floor of the orbit is removed the pt has an increased chance of developing orbital cellulitis with sinus problems |
|
|
What are the six classes of Grave's disease?
|
1 Class 0: No signs or symptoms
2 Class 1: Only signs – Upper lid retraction 3 Class 2: Soft Tissue involvement with symptoms 4 Class 3: Proptosis 5 Class 4: EOM involvement 6 Class 5: Corneal Involvement 7 Class 6: Sight Loss due to ONH |
|
|
All of the followingg diseases are commonly found in patients with AIDS except:
a. Xerosis b. Oral Candidiasis c. Vasculitis d. Seborrheic dermatitis |
C
|
|
|
A pt with hyperthyroidism may exhibit all of these physical signs except:
a. nervousness b. bulging eyes c. sweating d. weight gain e.lid lag |
D
|
|
|
a pt complains of always being tired and lethargic. Pt is obese, and has a puffy face and sparse hair.
Does this pt have? a. hyperthyroidism b. myasthenia gravis c. hypoparathyroidism d/ hypothyroidism |
D
|
|
|
Best test for screening Thyroid function is
a. T4 RIA b. free T4 c. T3 resin uptake d. TRH stimulation |
B
|
|
|
Pt with hypertensin with normal to high renin levels will respond best to
a. diuretics b. beta blockers c. calciium antagonists d. none of the above |
B
ACE inhibitors will also work |
|
|
The class of drugs that most pts with HTN would show a favorable response to if used alone would be
a. beta blockers b. ACE inhibitors c. calcium blockers d. diuretics |
D
|
|
|
Grave's disease is not accompanied by:
a. a decrease in thyroid stimulating hormone level b. a decrease in thyroid stimulating immunoglobin c. an increase in thyroid homrones levels d. an increased basal metabolic rate e. exessive sweating |
B
|
|
|
If your pt presents with a diffuse goiter and yperthyroidism. What are the expected values of TSH and thyroid hormones?
|
LOW TSH and HIGH thyroid hormones
|

