![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
51 Cards in this Set
- Front
- Back
|
is the conscious or subconscious awareness of changes in the external or internal environment.
|
sensation |
|
|
is the interpretation of sensations performed by the cerebral cortex.
|
perception |
|
|
Each type of sensation is called a
|
sensory modality
|
|
|
Sensory modalities are grouped into either general senses or
|
special senses |
|
|
tactile (touch, pressure, vibrations, itch, tickle) thermal, pain, proprioceptive (perception of moving and nonmoving body parts and positions).
|
somatic |
|
|
pressure, chemicals, stretch, nausea, hunger, temperature in internal organs
|
visceral |
|
|
possess bare dendrites. The are used to detect somatic pain, temperature, tickle, itch and some touch.
|
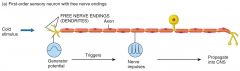
Free nerve endings
|
|
|
have dendrites enclosed in a connective tissue capsule. They are used to detect somatic and visceral pressure, vibration and some touch.
|
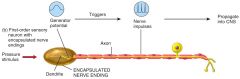
Encapsulated nerve endings
|
|
|
Sensory receptors cells for some special senses include gustatory receptor cells in taste buds, photoreceptors in the retina of the eye and hair cells in the inner ear for hearing.
|
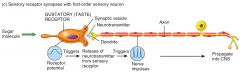
separate cell |
|
|
in or near external surface of the body; monitor external environment through hearing, vision, smell, taste, touch, pressure, vibration and pain.
|
Exteroreceptors
|
|
|
monitor the body’s internal environment with receptors in blood vessels, visceral organs, and nervous system
|
Interoreceptors
|
|
|
located in muscles, tendons, joints, and inner ear; provide info about body position, muscle length/tension and the position and movement of joints. See Fig. 16.4 (p. 554) for two examples: 1) muscle spindles – changes in muscle length 2) tendon organs – monitor force of contraction
|
Proprioceptors
|
|
|
detect sensations of touch, pressure, vibration, proprioception, hearing and equilibrium as a result of stretching, bending, or changing the shape of a cell
|
Mechanoreceptors
|
|
|
detect changes in temperature
|
Thermoreceptors
|
|
|
detect painful stimuli resulting from tissue damage
|
Nociceptors
|
|
|
detect light that hits the retina of the eye
|
Photoreceptors
|
|
|
detect chemicals in the mouth, nose and body fluids
|
Chemoreceptors
|
|
|
detect the osmotic pressure of body fluid
|
Osmoreceptors
|
|
|
that arise from stimulating the skin are called cutaneous sensations.
|
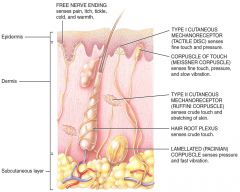
Somatic sensations
|
|
|
Pain serves a protective function by indicating tissue damage and/or helping to pinpoint the underlying cause of disease/disorder. Receptors for pain are called ________ and are located in almost every tissue in the body.
|
nociceptors
|
|
|
acute, sharp or prickling; perceived within 0.1 second.
|
Fast pain
|
|
|
chronic, burning, aching or throbbing pain; perceived a second or more after the stimulus. It may grow in intensity over time.
|
Slow pain
|
|
|
arising from skin receptors.
|
Superficial somatic pain
|
|
|
arising from skeletal muscles, joints, tendons and fascia.
|
Deep somatic pain
|
|
|
usually present in or just deep to the skin that overlies the stimulated organ.
|
Visceral pain
|
|
|
block the formation of prostaglandins, which stimulate nociceptors. Ex. Aspirin and ibuprofen
|
Analgesic drugs
|
|
|
short term pain relief by blocking conduction of nerve impulses. Ex. Novocaine
|
Local anesthetics
|
|
|
alter the perception of pain coming from the brain. Ex. Morphine
|
Opiate drugs
|
|
|
If an organ and a different part of the body are served by the same segment of the spinal cord, the pain may be felt beyond the stimulated organ. This is called
|
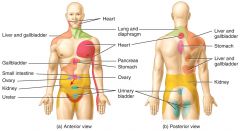
referred pain.
|
|
|
pathways carry information from somatic sensory receptors to the primary somatosensory area in the cerebral cortex and to the cerebellum.
|
Somatic sensory
|
|
|
carry impulses from somatic receptors to the spinal cord and/or brain stem
|
First-order neurons
|
|
|
carry impulses from the brain stem to the thalamus. These axons decussate before ascending to the thalamus.
|
Second-order neurons
|
|
|
carry impulses from the thalamus to the primary somatosensory area of the cerebral cortex.
|
Third-order neurons
|
|
|
located on both parietal lobes of the brain are the sites for the primary somatosensory area.
|
Postcentral gyri
|
|
|
The posterior ___________ tract and the anterior ___________ tract carry proprioceptive impulses from the spine to the cerebellum. These impulses help maintain posture, balance, and coordination of skilled movements.
|
spinocerebellar
|
|
|
nerves that extend out of the brain stem through cranial nerves or out of the spinal cord through spinal nerves to control all voluntary and involuntary movements
|
Lower motor neurons (LMNs)
|
|
|
provide input to LMNs from the cerebral cortex and motor centers in the brain stem to carry out voluntary movements. They also help maintain balance, muscle tone, and posture
|
Upper motor neurons (UMNs)
|
|
|
Monitoring intentions for movementMonitoring actual movementComparing command signals with sensory informationSending out corrective feedback when there’s a discrepancy between intended and actual movement
|
cerebellum
|
|
|
the processing of sensory info by analyzing and storing it and using it to make decisions for various responses; includes : Sleep and wakefulness Learning and memory Emotional responses
|
Integration
|
|
|
difficulty falling asleep or staying asleep caused by stress, caffeine*, depression, disruption of circadian rhythm, etc.
|
Insomnia
|
|
|
breathing repeatedly stops while sleeping due to loss of pharyngeal muscle tone
|
Sleep Apnea
|
|
|
involuntary periods of sleep that last about 15 minutes that occur throughout the day due to a deficiency of orexin, a chemical released from the hypothalamus which promotes wakefulness
|
Narcolepsy
|
|
|
the process by which info acquired through learning is stored and retrieved
|
Memory
|
|
|
the ability to acquire new info or skills through instruction or experience
|
learning |
|
|
severed endings of sensory axons still present in severed limbs can be activated to produce severe pain that is perceived to be coming from the nonexistent limb. It can be treated with electrical nerve stimulation, acupuncture, and biofeedback.
|
Phantom Limb Sensation
|
|
|
a degenerative disease that attacks motor areas of the cerebral cortex, causing progressive muscle weakness and atrophy. Death typically occurs in 2-5 years. The drug riluzole reduces damage to motor neurons, but is not a cure.
|
Amyotrophic lateral sclerosis (ALS)
|
|
|
due to an inherited loss of neurons that release GABA and ACh, resulting in rapid, jerky movements and progressive mental deterioration. Symptoms often do not appear until age 30-40 and death typically occurs 10-20 years later.
|
Huntington Disease
|
|
|
characterized by involuntary body movements and use of inappropriate sounds or words
|
Tourette syndrome
|
|
|
excess dopamine activity in the brain causes delusions, paranoia, and hallucinations
|
Schizophrenia
|
|
|
repetitive thoughts cause repetitive actions
|
Obsessive-compulsive disorder (OCD)
|
|
|
due to too little dopamine and too much ACh; typically affects victims around the age of 60. Symptoms are progressive and include tremors (especially hands), muscle rigidity, slowness of movement and decreased range of motion. Taking dopamine orally is ineffective because it cannot cross the BBB. Anticholinergic drugs can block the build-up of ACh to reduce some symptoms. Surgical treatments show some promise, including implanting electrodes that release electrical currents to reduce some of the symptoms.
|
Parkinson’s Disease (Basal Nuclei Disorder)
|

