![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
48 Cards in this Set
- Front
- Back
|
What is cardiac output (CO)?
|
Volume of blood ejected by the heart in one minute (HRxSV)
|
|
|
What is stroke volume (SV)?
|
The amount of blood ejected by the heart in one contraction; influenced by preload, afterload, and contractility
|
|
|
What is preload?
|
Volume of blood returning to the heart (circulating blood volume). As the amount of blood delivered to the heart increases, then myocardial fibers lengthen and a greater amount of blood is pumped out of the heart. Measured by CVP
|
|
|
What is afterload?
|
Resistance against wich the ventricles pump when ejecting blood; severe HTN, systemic and vascular resistance. Measured by BP
|
|
|
What is contractility?
|
Efficiency of myocardial fiber shornetig or the ability of the cardiac muscle to act as an efficient pump; assessment of tisue perfusion (pulses, warmth, cap refill)
|
|
|
What is function of foramen ovale?
|
Located between two atria, closes d/t pressure changes, in fetus allows oxygenated blood to go from LV out to systemic circulation
|
|
|
What is the function of ductus arteriosis?
|
Shunts blod from pulmonary artery up to aorta
|
|
|
What is the function of ductus venosus?
|
It shunts blood from placenta to right ventricle and the to the aorta through foramen ovale
|
|
|
What are indications of pedatric cardiac dysfunction?
|
Poor feeding
tachypnea (60) tachycarda (160) failure to trhive poor weight gain activity intolerance developmental delays prenatal hx (premie, IDM, IUGR) family hx (frequent fetal loss, sudden infant deaths, sudden adult deaths r/t heart disease, congenital heart defects) |
|
|
What is a murmur?
|
Heart sounds that reflect flow of blood within the heart; produced by vibrations witin the heart chambers or in the major arteries from the back-and-forth flow of blood.
|
|
|
When do innocent murmurs occur and how many children get them?
|
During times of increased cardiac output (fevers, anemia, rapid growth); 50% of children have innocent heart murmurs at some time
|
|
|
What is a thrill?
|
the sound of a thrill is a soft vibration over the heart that refects the transmitted sound of a heart murmur
|
|
|
What does preprocedual care includes for pediatric patient before cardiac catheterization?
|
accurate measure of height to determine cath length
weight history of allergies/family history severe diaper rash may cancel the procedure if femoral access is necessary assess and mark pedal pulse locations Prepare child for what they may feel—pressure at insertion site and vasospasm of small vessels with entry, warmth, N/V, HA with infusion of contrast material Sedation |
|
|
What does postprocedal care includes for pediatric patient after cardiac catheterization?
|
PULSES for equality and symmetry (especially on cath side)
Temp and color of cath extremity VS q 15 minutes at first—emphasis on HR (one full minute if no monitor) BP (especially for hypotension—hemmorrhage) Dressing—hemmorrhage or hematoma formation—occlusive waterproof pressure dressing Fluid intake—IV and oral—need adequate intake because blood loss in the cath lab, NPO status prior to procedure, and the contrast material used all put patient at risk for dehydration.—infants need dextrose fluids! Bedrest with extremitiy straight for 4-6 hours (venous) or 6-8 hours (arterial) |
|
|
What are the two types of cardiac defects?
|
1. Congenital - anatomic, abormal function
2. Acquired - disease process (infection, autoimmune response, enviromental factors, familial tendencies |
|
|
What are the causes of congenital heart disease?
|
1. Maternal (drug use, rubella, CMV, toxoplasmosis, viral illneses, IDMs) or envirometal (1-2%)
2. Chromosomal/genetic (10-12%) 3. Multifactorial (85%) |
|
|
How are congenital heart defects classified?
|
1. Increased pulmonary blood flow (CHF)
2. Decreased pulmonary blood flow (cyanosis) 3. Obtruction of blood flow out of ventricles a. Obstructed left heart - CHF b. Obstructed rt heart - cyanosis 4. Mixed blood flow (depends on degree of mixing) |
|
|
What can be the cause of increased pulmonary blood flow defects?
|
- Abnormal connection between two sides of the heart
- Increased blood volume in the right side of the heart - increased pulmonary blood flow - Decreased systemic blood flow |
|
|
What are examples of increased pulmonary presure defects?
|
- Atrial septal defect
- Ventricular septal defect - Patent ductus arteriosis |
|
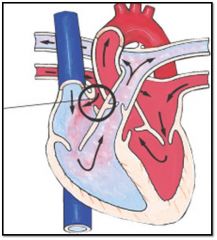
What is the name of this cardiac defect?
|
Atrial septal defect
|
|
|
What is diagnostic sign for atrial septal defect?
|
Fixed split S2 sound
|
|
|
What is the treatment for atrial septal defect?
|
It may be closed in cardiac cath procedure; surgical repair with patch (ususally before age 6)
|
|
|
What symptoms can atrial septal defect cause?
|
minimal symptoms of vascular changes; risk for dysrhythmias and emboli formation later in life if unrepaired
|
|
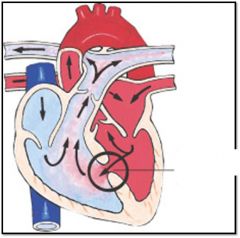
What cardiac defect is this?
|
Ventriclar septal defect
|
|
|
What are the risks with VSD?
|
Bacterial endocarditis, pulmonary vascular obstructive disease, reversal of blood flow through ventricles (severe)
|
|
|
What are the symptoms of VSD?
|
Depends on the size of opening; murmur, CHF
|
|
|
How VSD can be repaired?
|
Cath repairs in clinical trials
Surgical repair w/ bypass; Pulmonary artery banding (if not too large) or patch |
|
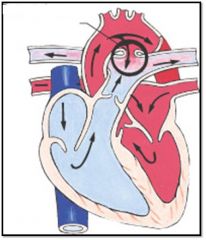
What is the name of this heart defect?
|
Patent ductus arteriosus
|
|
|
Why does ductus arteriosus closes?
|
B/c of change in arterial oxygen concentration that follows initiation of pulmonary function
|
|
|
What aids in PDA closure?
|
Prostaglandin E
|
|
|
What direction does PDA allow blood to flow in?
|
From aorta into pulmonary arteries
|
|
|
What are manifestations of PDA?
|
Large PDA - CHF with tachypnea, dyspnea, hoarse cry
Bounding peripheral pulses Widened pulse pressure (>25) Machinery murmur at upper left sternal border; murmur audible throughout cardiac cycle |
|
|
What test provides difinitive diagnosis of PDA
|
Echocardiogram
|
|
|
What is tx for PDA?
|
Preterm kids= INDOMETHACIN to close PDAs
Surgical ligation if meds fail Prophylactic antibx to prevent bacterial endocarditis Surgery>> between age 1-2 yrs |
|
|
Name obstructive defects
|
1. Coarctation of the aorta
2. Aortic stenosis 3. Pulmonic stenosis |
|
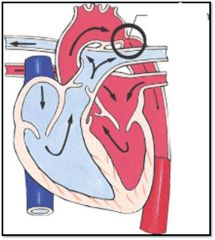
What is the name of this cardiac defect?
|
Coarctation of the Aorta
|
|
|
In what location does aorta narrows in coarctation of the aorta?
|
Aorta is narrowed near the insertion of ductus arteriosus and causes increased pressure proximal to the defect
|
|
|
What is the treatment for coarctation of the aorta?
|
Nonsurgical - balloon angioplasty
Surgical - HTN is postop complication; risk of recurrence; done before 2yo |
|
|
What risks does a person with coarctation of aorta has?
|
Risk for raptured aorta
Aortic aneurism Stroke |
|
|
What are the symptoms of coarctation of aorta?
|
In infants - CHF, quickly deteriorate
In older kids - dizziness, HA, fainting and epistaxis from HTN General - HTN, bounding pulses in arms, weak or absent femoral pulses, cool lower extremities |
|

Name this defect
|
Aortic stenosis
|
|
|
What is aortic stenosis?
|
Narrowing of aortic valve that causes increased resistance in te left ventricle, decreased CO, L ventricular hypertrophy, pulmonary congestion
|
|
|
What is the treatment for aortic stenosis?
|
Balloon angioplasty to dilate the valve
OR Kono procedure - valve replacement; may need repeat procedures |
|
|
What are s/sx?
|
Faint pulses
Hypotension Poor feeding Tachycardia Murmur Excersise intlerance Chest pain Dizziness with standing |
|
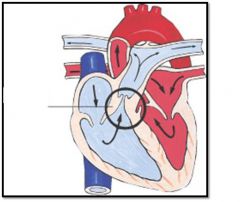
What is this heart defect?
|
Pulmonic stenosis
|
|
|
What does pulmonic stenosis cause?
|
Rt ventricular hypertrophy, decreased pulmonary blood flow, may reopen foramen ovale
|
|
|
What are s/sx of pulmonic stenosis?
|
Systemic cynosis
Maybe CHF Often accompnied by PDA |
|
|
What is the treatent for pulmonic stenosis?
|
Balloon angioplasty to dilate the valve
Brock procedure (bypass to do valvotomy) Usually can repair with cath |

