![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
43 Cards in this Set
- Front
- Back
|
What are the functions of the vascular system?
|
Transport O2 and nutrients and waste products (e.g. lactic acid and CO2)
Transport defence cells, hormones, growth factors Regulate distribution of blood Blood pressure and temperature Wound healing |
|
|
What are the 3 layers of blood vessels?
|
Tunica intima
Tunica media Tunica adventitia |
|
|
What is the tunica intima composed of?
|
Endothelium (simple squamous epithelium on basement membrane)
|
|
|
What is the tunica media composed of?
|
Smooth muscle and connective tissue
|
|
|
What is the tunica adventitia composed of?
|
Connective tissue - collagen and elastin
Sometimes vaso vasorum - blood vessels supplying vessel wall (lymphatics and nerves too) |
|
|
Give examples of elastic arteries
|
Aorta
Pulmonary artery |
|
|
Give examples of muscular arteries
|
Most arteries, size variation
|
|
|
Describe the structure of elastic arteries
|
Tunica intima - thin, endothelium with layer of collagenous tissue rich in elastin, myointimal cells (atherosclerosis) and fibroblasts
Tunica media - broad, elastin, collagen and smooth muscle fibres Tunica adventitia - relatively thin, vasa vasorum - lymphatics, nerves, elastin and type 1 collagen |
|
|
What is the function of elastic arteries?
|
Shock absorption in response to high pulse pressure - distension during systole, recoil during diastole
Maintains smooth blood flow and blood pressure |
|
|
Describe the structure of muscular arteries
|
Two well defined elastic sheets - internal elastic lamina between tunica intima and media, external elastic lamina between tunica media and adventitia
Tunica media usually equal to or smaller then tunica adventitia Tunica adventitia - collagen and elastin, broad |
|
|
What is the function of muscular arteries?
|
Control or adjust blood flow distribution and blood pessure by nervous control and vasodilation/constriction respectively
|
|
|
Describe the structure of arterioles
|
Lumen diameter usually <0.3mm and fewer than 6 layers of smooth muscle
Tunica intima and adventitia layers quite insignificant |
|
|
What is the function of arterioles?
|
Regulate blood pressure and blood flow to capillary beds
|
|
|
What does increased vasoconstriction in arterioles cause?
|
Increased peripheral resistance -> increased blood pressure
|
|
|
How do arteries protected by the skull differ?
|
Thin t. media (no need for protection, already protected)
Thick inner elastic lamina |
|
|
How are arteries in the penis specialised?
|
Helicine arteries
Extensively branched and coiled Smooth muscle cushions - valves for erection |
|
|
How do umbilical arteries differ?
|
No inner elastic lamina
Inner longitudinal and outer circular smooth muscle layer |
|
|
How are arteries in the lung specialised?
|
Less elastin and muscle due to lower pressure in pulmonary circulation
|
|
|
Describe the structure of capillaries
|
Endothelium, basement membrane and CT
Diameter of 3-10µm Flattened cells pericytes present - progenitor CT cells: fibroblasts, macrophages, smooth muscle - contractile or regulatory |
|
|
What does the density of capillaries in a tissue represent?
|
How metabolically active a tissue is
|
|
|
What are the 3 different types of capillaries?
|
Continuous
Fenestrated Sinusoidal |
|
|
Describe where continuous capillaries are found and how exchange occurs
|
Lungs, muscle, skin, exocrine glands, nervous tissue
Passive diffusion - gases, ions and small molecules Pinocytic vesicles - proteins and some lipids Intercellular passage - via intercellular space between endothelial cells |
|
|
Describe where fenestrated capillaries are found and how exchange occurs
|
Kidneys, intestines, endocrine glands
Pores - much greater permeability, macromolecules smaller than plasma proteins Fewer, if any, pericytes |
|
|
Describe where sinusoidal capillaries are found and how exchange occurs
|
Spleen and liver
Large spaces between endothelial cells allowing large particles like RBCs and proteins to pass through |
|
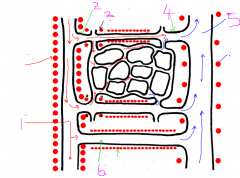
Name numbers
|
1 - arteriole
2 - metarteriole 3 - precapillary sphincters 4 - thoroughfare channel 5 - venule 6 - arteriovenous shunt |
|
|
What is a metarteriole?
|
Connects a terminal arteriole and venule
Capillary bed branches off arteriole end and reemerge into thoroughfare channel |
|
|
What happens if the precapillary sphincters close?
|
Blood bypasses capillary bed through arteriovenous shunts
|
|
|
What happens if the arteriovenous shunt smooth muscle or metarteriole smooth muscle contracts?
|
Blood flows into capillary network
|
|
|
Why is the arteriovenous shunt contraction/precapillary sphincter shutting an important mechanism?
|
For tissue with intermittent blood flow e.g. digestive system
Temperature regulation |
|
|
Describe the 3 types of venules
|
Postcapillary venules - drain several capillaries, wider diameter, blood almost stagnant but inflammation, allergies, temperature
Collecting venules - larger diameter and greater number of pericytes Muscular venules - 3 layer structure, 1-2 muscle layers |
|
|
What are valves in veins made up of?
|
Fibroelastic infolding of tunica intima
|
|
|
Why are veins considered blood reservoirs?
|
Up to 65% of body's blood in veins
|
|
|
Describe small/medium and large veins
|
Small/medium - t. media 2-3 layers of smooth muscle and t. adventitia contains longitudinal collagen fibres
Large - NO VALVES, t. intima some elastic fibres, t. media poorly developed with circular muscle except vena cava where it is longitudinal, t. adventitia very thick with vaso vasorum, lymphatics, collagen, elastin |
|
|
How are veins that have to cope with high hydrostatic pressure specialised?
|
Thick tunica media
e.g. teat veins, limb veins |
|
|
How are veins specialised in protected regions?
|
No tunica media
e.g. bones, penile erectile tissue |
|
|
Do endothelial cells retain their ability to repair and divide throughout life?
|
Yes
|
|
|
How do endothelial cells respond to injury?
|
Produce Vascular Endothelial Growth Factor (VEGF) which acts on VEGF receptor
- manipulated by tumours |
|
|
How do veins respond to age?
|
Loss of elasticity, thickening, fragmentation, atherosclerotic plaques, calcification of t. media
|
|
|
What are the 3 forms of control of blood vessels?
|
Neural control - sympathetic postganglionic fibres - noradrenaline - α-1 adrenergic receptors = vasoconstriction - β-2 adrenergic receptors (blood vessels in skeletal muscle) - vasodilation
Endocrine - catecholamines from adrenal medulla - vasoconstriction (except skeletal muscle) Autoregulation - local control in response to local O2/lactic acid concentrations |
|
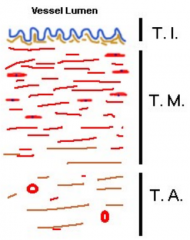
Which vessel?
|
Elastic artery
|
|

Which vessel?
|
Muscular artery
|
|
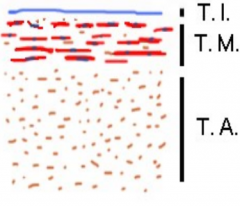
Which vessel?
|
Small and medium veins
|
|
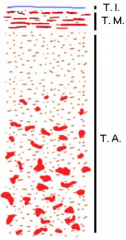
Which vessel?
|
Large vein
|

