![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
59 Cards in this Set
- Front
- Back
|
Define Heart failure
|
The heart is unable to supply the needs of tissues or is able to do so only at high filling pressures.
|
|
|
4 General categories of things that can malfunction and cause HF
|
Valves
Pericardium Myocardium Vessels/Blood |
|
|
CO is a product of
|
HR and SV
|
|
|
4 things that influence CO
|
Preload
Afterload (BP) Wall stress Contractility |
|
|
In patients with a ___1___ CM, ___2___ function is impaired meaning that contractility is poor and the body responds by increasing BP (afterload) by secreting ___3____. This is ca improve perfusion, but worsens the HF.
|
1) Dilated
2) systolic 3) Catecholamines (NE) |
|
|
1) 3 Hormones the body secretes to increase arterial BP (Afterload) when the heart is failing.
2) In practice, how do we counteract this pharmacologically to reduce the afterload stress on the heart? |
1)NE
AII Endothelin 2) ACE inhibitors |
|
|
1) The heart (Laplace's law) compensates for increased ___1___ by increasing wall thickness in order to preserve ___2___.
|
1) radius
2) wall stress |
|
|
Name the three GENERAL mechanisms that the heart uses to maintain CO in failure.
|
Frank-Starling
Neurohumoral system Cardiac Remodeling |
|
|
Starling compensation for ___1____ heart dysfunction worsens the problems because it increases already pathologically high ___2____. This can cause ___3_____ in the lungs.
|
1) Systolic
2) P and V in the ventricle 3) Pulmonary edema. |
|
|
Neurohumoral response to heart failure:
Name as many mediators that are increased in systemic circulation by HF. |
NE (low in heart)
Renin AII Aldosterone ADH/AVP TNF IL6 IL1 Endothelin ANP (in heart too) BNP (in heart too) CNP (not in hear, just systemically) |
|
|
1) Name 4 effects of NE which is elevated in HF.
2) These things can predispose to what complication? |
1) Systemic vasoconstriction
Increase HR Stimulates myocardial contractility Renin Release (myocyte death) 2) Arrythmia |
|
|
1) In HF, what is the level of NE in the heart? Why?
2) BEta1 receptors? Why? 3) How does (2) affect response to an inotrope like dobutamine? 4) How can we counteract this effect? |
1) It is low because of exhaustion due to prolonged adrenergic stimulation
2) Low, due to increased stimulation 3) Blunted, this is not good because we use dobutamine to support HF. 4) Beta-blocker increases the receptor level. |
|
|
HF causes renin release, which leads to AII, which ehances release of __1___ and directly causes release of __2__.
3) __2___ worsens HF by two mechanisms. Name them. |
1) NE
2) Aldosterone 3) Na+/volume retention Cardiac myocyte remodeling |
|
|
1) AVP is increased or decreased in HF?
2) besides water retention, how else does it worsen HF? |
1) increased
2) Vasoconstriction |
|
|
1) Elevation of systemic or myocardial levels of these two compensatory, and adaptive proetins are a good marker for HF and Volume overload.
2) What is their direct effect? 3) what other actors do they supress? |
1) ANP
BNP 2) natriuresis in in response to stretch 3)AII, ADH/AVP, aldo, renin (all the ones in the renal axis) |
|
|
Cytokines of HF- What do they do in general?
(TNF, IL1B, IL6) 2) What is a specific action of TNF? |
1) Regulate myocyte growth--> hypertrophy
2) Immediate myocyte dysfunction |
|
|
What are the negative sequelae directly on the heart of myocardial hypertrophy.
|
Mismatch of blood supply (low capp. density)
This can lead to ischemia or necrosis. |
|
|
1) Dilated CM causes ___1__ dysfunction. Extra sound?
2) Hypertrophic CM causes ___2__ dysfunction. extra sound? 3) Restrictive CM causes ___3__ dysfunction |
1) systolic- S3
2) diastolic- S4 3) Diastolic |
|
|
Ischemia causes diastolic or systolic dysfunction or both? Explain the pathophysiology.
|
both
Diastolic- fibrous scar, diastole is active process Systolic- myocardium loss |
|
|
Random extra two cardiomyopathies
1) Important in kids 2) Catchall |
1) Arrythmogenic RV Cardiomyopathy- ARVD
(FIbro-fatty change in RV) 2) Unclassafied |
|
|
Forward failure is caused by LV ______ dysfunction
(forward or backward) |
Forward
|
|
|
Hypertensive CM is a type of ___1___ CM.
|
Hypertrophic
|
|
|
Hypertrophic CM is caused by RV or LV ________ failure.
(forward of backward) |
backward
|
|
|
Rx of choice for a pure diastolic dysfunction (pure hypertrophic)
|
Diuretic
|
|
|
Describe the changes in P-V loop in systolic and diastolic dysfunctional HF.
|
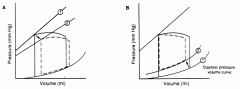
1) systolic dysfunction is due to down-right shift of the end systolic P-V relation (straight line at the top). This is reduced conrtactility
2)Diastolic dysfunction is due to the up -left movement of the end-diastolic passive P-V relation. This means increased stiffness or decreased compliance. |
|
|
1)__1___ is the biggest cause of both systolic and diastolic HF.
2) HTN, DM, and AS are a bigger cause of systolic or diastolic dysfunction 3) alcohol are a bigger cause of systolic or diastolic dysfunction |
1) CAD
2) Diastolic (Hypertophy) 3) Systolic (Dilated) |
|
|
1) Dyspnea, Orthopnea, and PND are symptoms of ___-sided, ___ward HF.
2) RUQ tenderness, Reduced appetite, Edema are symptoms of ___sided, ___ward HF. 3) Weakness and fatigue are symptoms of ___sided, ___ward HF. 4) What are the symptoms of Left sided Backward HF? 5) What are the symptoms of backward Right sided HF? 6) Forward HF? |
1) Left sided, backward
2) RIght sided backward 3) Left sided forward 4) Tachypnea, Lung crackles 5) JVD, Hepatomegaly, Edema 6) Decreased mentation Cool extremeities Pulsus alternans Cheyne-stokes respirations |
|
|
What is indicated by a loud pulmonary valve closure? What might cause this?
|
Pulmomary HTN
(maybe due to backward left sided HF) |
|
|
Three possible causes of idiopathic DCM?
|
familial
viral myocarditis Immunological abnormalities |
|
|
DCM natural history
25% die in __1____ year(s) 50% dies in ____2__ year(s) |
1) 1
2) 5 |
|
|
Thigns that predict poor prognosis in DCM?
|
degree of ventricular enlargement
limited exercise capacity rduced maximal O2 uptake |
|
|
Two causes of DCM that we might be able to fix without heart transplant?
|
alcohol
CAD |
|
|
__1____ should be performed in any patient with suspected HF
2) Once the diagnosis of DCm has been made, what two test should be give to look for CAD? 3) what will be the finding on CXR? 4) ECG findings that may be present,(but needn't be). |
1) echo
2) stress test or cardiac cath 3) enlarged heart with or without fluid in the lungs 4) poor R wave progression, LBBB |
|
|
1) Two three- letter acronyms that characterize bad HCM?
2) the second one is caused by the ____effect |
2) ASH- assymetrical septal hypertrophy
SAM- systolic anterior movement of the anterior leaflet of the mitral valve. 2) venturi |
|
|
in HCM with LVOT, the LV pressure is much __1___ than the aortic pressure.
This can be quantified by using ___2___. |
1) higher
2) Doppler |
|
|
1) SAM caused by HTM can cause ___2___. If this is severe, what symptom may be felt.
3) describe the heart sound that would be heard (in total) |
1) MR
2) Dyspnea. 3) Late systolic myrmur (MR) maybe a holosystolic murmur from the LVOT Probably an S4 |
|
|
How does HCM lead to myocardial ischemia (4 ways)
|
Hypertrophy of coronary vessels leading to imparment in dilation
inadequate capp. density for the muscle. Increased demand Compression of coronaries during strong contraction |
|
|
1) Inheritance pattern of HCM
2) most common |
1) AD
2) Beta myosin heavy chain |
|
|
histology of HCM
|
disorganized muscle bundles leading to a whorled appearance
fibrosis and necrosis Thickening of coronary arteries |
|
|
1) Most Common symptom of HCM
2) other common ones |
1) dyspnea
2) angina, fatigue, syncope, palpitations, sudden death |
|
|
Two physical (no tools) findings in HCM?
|
strong apical impulse
Strong carotid pulse |
|
|
1) Describe how the holosystolic ejection murmur from LVOT can change with postion?
2) Where is it best heard? |
1) Increases with valsalva, standing (anything that makes ventricle smaller)
Decreases with squatting or raising the legs (anything that increases ventricular size) 2) between apex and Left sternal border |
|
|
HCM findings on
1) ECG 2) Echo 3) Doppler |
1) increased voltage, ST and T-wave changes, maybe Q-waves
2) LV thickness maybe with ASK 3) Gradient of P across the aortic valve (low on aorta side) |
|
|
1) Prognosis of HCM in general population (% death yearly)
2) Predictors of poor prognosis |
1) 1% death yearly
2) abnormal BP response to exercise, syncope, marked hypertrophy |
|
|
Management of HCM
1) to relieve pulmonary congestion 2) to cause decreased contractility 3) to caused increased diastolic filling 4) to depress LV contractility |
1) Diuretics to reduce pulmonary congestion
2) Beta blockers to relieve LVOT bly blocking contractility 3) Calcium channel blockers (Verapamil specifically) to improve diastolic filling except in people with HF 4) Disopyramide (1-A) to depress LV contractility. |
|
|
5 invasive options for HCM
|
Dual chamber pacer
ICD Alcohol septal ablation Myomyectomy MVR (to relieve SAM) |
|
|
Important causes of Restrictive CM
|
Amyloid
Sarcoid Gauchers Fatty infiltration Hemochromatosis Fabry Glycogen storage diseases Carcinoid Radiation Familial Scleroderma Diabetic CM |
|
|
1) Initial presentation of RCM
2) After progression, presentation |
1) dyspnea on exertion, weakness
2) Ascites, Hepatomegaly, edema (anasarca) |
|
|
Findings in RCM:
1) Echo 2) doppler 3) ECG |
1) normal systolic function
2) diastolic dysfunction 3) Diffusely diminished voltage |
|
|
1) Characteristic sign of RCM and pericardial constriction on a time-pressure tracing.
2) explain why this sign happens |
1) Square root sign
2) early diastolic filling abruptly halts as the volume in the ventricles quickly reaches its limits imposed by the constrcited pericardium. |
|
|
Three diagnostic tests we use to search for an etiology for RCM
|
fat pad aspirate for amyloid
iron studies fo hemochromatosis Endomyocardial biopsy |
|
|
Tx of RCM
1) in general 2) if amyloid 3) if hemochromatosis |
1) diuretics
2) DNA alklating agents 3) Desferroximine and phlebotomy |
|
|
Important causes of constrictive pericarditis
|
idiopathic
infection post surgical trauma radiation neoplastic uremia Connective tissue disorders Procainamide hydralazine |
|
|
Constrictive pericarditis presents like ____ failure even though they have not failed
|
ventricular
|
|
|
Diagnostic sign seen on exam of constrictive pericarditis (proably in RCM too)
|
Kussmauls sign (inspiratory increase in JVD)
|
|
|
Constrictive pericarditis CXR appearance
|
can sometimes see calcification of pericardium in lateral view
|
|
|
Findings in constrictive pericarditis
1) Echo 2) Ct or MRI 3) management? |
1) normal systolic function, dilated atria. cannot see pericardium
2) thick pericardium on either 3) Diuretics or Pericardial stripping |
|
|
Given a sign, tell whether is is present in RCM, constrictive pericarditis, or both. (some answers are "maybe present")
1) S3 2) pericardial knock 3) Kussmaul's sign 4) HF 5) Thick ventricles 6) Valvular Regurg 7)Atrial enlargement 8) Atrial pressures 9) Ventricular pressure (Square root) 10) Pulmonary pressure (numerical) 11)Pericardial thickening (CT or MRI) 12) Biopsy |
1) absent in PC
Present in RCM 2) Present in PC absent in RCM 3) present in PC may be present in RCM 4) present in both 5) absent in PC may be present in RCM 6) absent in PC Present in RCM 7) present in both 8) elevated in both 9) square root in both 10) 35-40 mmHg in PC >50 mmHg in RCM 11) thick in CP normal in RCM 12) normal in CP infiltrativ process in RCM |
|
|
5 steps in evaluating a pt. with HF
|
H & P
ECG CXR Echo CT or MRI if indicated |

