![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
70 Cards in this Set
- Front
- Back
|
Bacteria causing community acquired pneumonia
|
S. pneumoniae
H. influenza b M. catarrhalis Legionella spp Mycobacteria pneumoniae Chlamydophila pneumoniae others |
|
|
Bacteria causing hopital-acquired pneumonia
|
Pseudomonas aeruginosa
Klebsiella pneumoniae Legionella spp Acinetobacter Staph. aureus |
|
|
What type of pneumonia is this?
Presentation often acute with shaking chills, productive cough, CXR showing consolidation, no extra-pulmonary symptoms |
typical
note- this classification system is not reliable, although you may still encounter it |
|
|
What type of pneumonia is this?
Slower onset, non-productive cough, frequent extra-pulmonary symptoms |
atypical
|
|
|
pathogens causing typical pneumonia
|
S. pneumo, H. influenzae, M. catarrhalis
|
|
|
pathogens causing atypical pneumonia
|
Legionella sp, Mycoplasma pneumoniae, Chlamydophila pneumoniae
|
|
|
Immune Compromised pts get pneumonia from the previously listed bugs plus what viruses?
|
CMV, HSV, VZV, measles, others
|
|
|
CF pts get pneumonia with what uncommon bug?
|
Pseudomonas-
|
|
|
alcoholics get pneumonia with what uncommon bug?
|
Klebsiella-
|
|
|
AIDS pts get pneumonia with what uncommon bug?
|
Pneumocystis-
|
|
|
outpatient treatment of pneumonia (pt has had no previous antibiotitics)
|
Macrolide or doxycyclin
Previous antibiotics Respiratory fluoroquniolone Advanced macrolide |
|
|
In-patient treatment of pneumonia
|
Respiratory fluoroquniolone
Advanced macrolide plus b-lactam |
|
|
Most common cause of CAP requiring hospitalization
|
Streptococcus pneumoniae
|
|
|
Classic symptoms of Pneumococcal Pneumonia
|
High fever
Tachycardia Hypoxia Respiratory distress CRX often shows consolidation |
|
|
What immune cells account for the consolidation in pneumonia?
|
PMNs
|
|
|
__?-valent vaccine
Recommended for 65 and older or >2yr with chronic disease, lack of functional spleen, institutionalized, immune suppressed |
23
|
|
|
__? valent congugate vaccine
Recommended for Infants and toddlers |
7
|
|
|
Where do legionella pneumophilia live?
|
Grow in amoebae in the water
|
|
|
Are legionella pneumophilia resistant to chlorine?
|
yes
|
|
|
Legionella sp.- Associated Diseases
_____ Fever- mild self-limiting febrile illness Fever, chills, myalgia, malaise |
Pontiac
|
|
|
Legionella pneumonia
Virulence factors- |
1) Facultative intracellular pathogen
replicates in alveolar macrophages and monocytes 2) Endotoxin |
|
|
Legionellosis has two forms: Pontiac fever, a mild respiratory infection, and ________' disease, a serious and potentially fatal form of pneumonia
|
Legionnaires
|
|
|
Symptoms of legionnaires disease
|
Abrupt onset of fever, chills, non-productive cough, headache
Involves more than lung- multisystem disease involving GI tract (diarrhea), liver, kidneys, CNS |
|
|
Clues that you might have legionnaires disease
|
Non-pulmonary symptoms
Negative sputum gram stain (small very faintly staining, gm – bacilli, hard to see) |
|
|
Legionnella:
Culture sample from bronchoalveolar lavage on _________ agar |
BCYE-buffered charcoal yeast extract
|
|
|
Other ways to diagnose legionnaires disease
|
1) DFA (fluoro) of sputum
2) Urine antigen test 3) PCR 4) Serology |
|
|
DOC for legionnaires disease
|
is newer macrolides- azithromycin- or respiratory fluoroquinolones (levofloxacin, others)
|
|
|
DOC for pontiac fever
|
no treatment (don't need it)
|
|
|
How do you treat the source of legionnella? (eg, wet A/C unit)
|
Superheating of water to 70-80C
Install copper-silver ionization units Produce metallic ions that kill microbes |
|
|
Why can't you use B-lactam antibiotics or vancomycin to treat mycoplasma pneumoniae?
|
no cell wall
membrane made of sterols |
|
|
Symptoms of walking pneumonia
|
Slow onset (weeks) beginning with URT symptoms, flu-like illness
Body aches, sore throat, headache, chills, malaise Fever Non-productive cough Rales and rhonchi, +/- wheezing on auscultation |
|
|
WBC count in walking pneumonia
|
WNL
w/i normal limits |
|
|
CXR of walking pneumonia
|
CXR: Diffuse unilateral or bilateral infiltrates usually involving lower lung; rarely shows consolidation
|
|
|
Pathogenesis of M. pneumoniae:
P1 adhesion protein mediates attachment to ____ on epithelial cells |
cilia
Cilia stop moving and epithelial cells die |
|
|
Mycoplasma pneumoniae culture
|
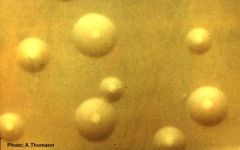
What's this?
|
|
|
Treatment of M. pneumoniae
|
Most often empiric
macrolides or respiratory fluoroquinolones sensitivity testing not necessary |
|
|
Culture of Chlamydophila penumoniae, Chlamydia trachomatis, Chlamydia psittaci
|
no culture
(Obligate intracellular pathogens) |
|
|
Chlamydophila Exist as elementary and ______ bodies
|
reticulate
|
|
|
Which are infectious, elementary or reticulate bodies?
|
elementary (metabolically inactive)
(reticulate bodies are opposite) |
|
|
Which Chlamydia?
STD and perinatal infection Can cause pneumonia in perinatally infected infants |
Chlamydia trachomatis
|
|
|
Which Chlamydia ?
Exposure to organism shed from psittacine birds (parrots, parakeets) Causes pneumonia or FUO |
Chlamydia psittaci
|
|
|
Which Chlamyda(-ophila)
Causes mild pneumonia, bronchitis, sinusitis 3-10% of CAP 300,000 pneumonia cases/yr Usually affects adolescents and young adults |
Chlamydophila pneumoniae
|
|
|
How does Chlamydophila pneumoniae survive in a cell?
|
Prevents fusion of phagosome with lysosomes
|
|
|
Most of Chlamydophila pneumoniae disease's manifestations are due to inflammatory response to ____
|
LPS
|
|
|
Diagnosis of C. pneumoniae- associated pneumonia
|
Diagnosis difficult
Organism is hard to culture, must be grown in cells; identifiied by immunoassay or immunofluorescence Serology requires acute and convalescent antibody titers; PCR is rapid and sensitive, |
|
|
Hospital-Acquired Pneumonias
Most frequently in ______ patients (VAP) |
ventilated
|
|
|
Hospital-Acquired Pneumonias
some pathogens |
Pseudomonas aeruginosa
Acinetobacter baumannii MRSA Klebsiella pneumoniae Enterobacteriaceae |
|
|
Pseudomonas aeruginosa
Aerobic, catalase-positive, Gm ____ rod |
neg
|
|
|
Pseudomonas aeruginosa is resistant to some ______ disinfectants
|
common
|
|
|
What kind of person gets infected with Pseudomonas aeruginosa
|
Swimmers- otitis externa
CF- pneumonia Catheterized patients- UTI, septisemia Burn patients- wound infections, septisemia Intubated patients- pneumonia, septicemia |
|
|
P. aeruginosa:
Found in soil and water Frequently isolated from water sources in hospitals- sinks, faucets, ______ solutions |
disinfectant
|
|
|
Virulence Factors in Pathogenesis of Pseudomonas:
Bacterial attachment and colonization |
Pili (attachment)
|
|
|
Virulence Factors in Pathogenesis of Pseudomonas:
Obstruction of host defenses |
Pyocyanin (blue-green pigment, impairs cilia)
Capsule (antiphagocytic) Exotoxins A and S are suppressive Cytotoxin |
|
|
Virulence Factors in Pathogenesis of Pseudomonas:
Induce inflammation |
LPS, pyocyanin, phosphlipase C
|
|
|
Virulence Factors in Pathogenesis of Pseudomonas:
Tissue destruction, local invasion and dissemination |
Elastase, toxins, pyocyanin, other secreted enzymes
|
|
|
Diagnosis of Pseudomonas
|
Gram stain, culture and sensitivity of:
Biopsied lung tissue is best sample Most common sample is bronchoscopic or BAL Sputum cultures not reliable Growth on blood agar or MacConkey agar Produce fruity odor |
|
|
Treatment of Pseudomonas pneumonia
|
Anti-pseudomonal penicillins along with an aminoglycoside
Ie, ticarcillin-clavulanate or piperacillin-tazobactam with tobramycin Other drug choices- imipenem-cilastatin, aztreonam, quinolones, ceftazidime, cefepime, |
|
|
Klebsiella pneumoniae
Gram ____. rods, , |
neg
|
|
|
Klebsiella pneumoniae
catalase ________ |
positive
|
|
|
Klebsiella pneumoniae
oxidase negative, ferments _____ |
lactose
|
|
|
Klebsiella pneumoniae
Colonizes _______ |
mucosal surfaces (especially gut) and skin
|
|
|
Who are at greatest risk for pneumonia due to K. pneumoniae
|
Intubated patients and alcoholics
|
|
|
Klebsiella pneumoniae:
Causes inflammation, necrosis and _______ in lung |
hemorrhage
|
|
|
Klebsiella pneumoniae:
May produce thick, bloody, mucoid sputum "_______ sputum” |
“currant jelly
|
|
|
Klebsiella pneumoniae:
Many hospital strains produce extended spectrum ______ (ESBL) |
b-lactamses
|
|
|
Extended spectrum cephalosporins, such as the third generation cephalosporins, were originally thought to be resistant to hydrolysis by ________!
|
beta-lactamases
|
|
|
mid 1980's it became evident that a new type of beta-lactamase was being produced by Klebsiella & E coli that could hydrolyze the ______ ______ cephalosporins.
|
extended spectrum
These are collectively termed the •'extended spectrum beta-lactamases'(ESBL's) |
|
|
Diagnosis of Klebsiella pneumoniae:
Growth on _____ Agar and Blood agar |
MacConkey
|
|
|
Why the slimey appearance of Klebsiella on agar?
|
due to capsule
|
|
|
Treatment of Klebsiella pneumonia
|
Non-ESBL strains
Third generation cephalosporins with or without aminoglycosides Susceptible to wide range of b-lactams, aminoglycosides, quinolones, aztreonam ESBL strains imipenem |

