![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
55 Cards in this Set
- Front
- Back
|
pasteurisation |
lowers microbial numbers for preventing spoilage |
|
|
sterilisation |
kills all microbes |
|
|
decontamination |
cleans an area for future use (detergents) |
|
|
disinfection |
lowers microbial numbers for preventing infection (disinfectants or antiseptics) |
|
|
treatment |
lowers microbial numbers for preventing/curing disease |
|
|
bacteriocidal |
kills bacteria |
|
|
bacteriostatic |
inhibits bacterial growth |
|
|
what organisms are most resistant |
bacterial spores |
|
|
what organisms are least resistant |
lipid enveloped viruses |
|
|
high heat kills bacteria including what |
thermophiles |
|
|
the standard temperature protocol for sterilising items involves what |
heating 121 degrees celsius for 15 min at high pressure (100 kPa) |
|
|
what does sterilisation kill |
both vegetative bacteria and spores |
|
|
what times can sterilisation be prolonged to if necessary |
30, 45 or 60 min |
|
|
what needs longer sterilisation time than water |
oils as well as large volumes (>2L) |
|
|
what piece of equipment can be used for sterilisation |
autoclave |
|
|
exposure of items to UV light for 10-15 min can lead to what |
their sterilisation |
|
|
UV light is often used in laminar flow cabinets for ensuring what |
an aseptic environment for microbiological work |
|
|
UV light is also used for sterilising what |
surgical tools or other instruments |
|
|
how does UV light kill bacteria |
causes numerous DNA mutations |
|
|
gamma radiation : |
disposable medical equipment, usually cobalt-60 or caesium-137 |
|
|
gamma radiation easily reaches all parts of the object to be |
sterilised |
|
|
gamma radiation permits sterilisation of |
heat sensitive materials |
|
|
gamma radiation has relatively low |
chemical reactivity |
|
|
gamma radiation has an instantaneous and simultaneous |
sterilising effect |
|
|
gamma radiation is |
very dangerous |
|
|
only well trained and experienced staff should decide upon the use and monitoring of |
gamma radiation |
|
|
specially designed and purpose built installations and equipment must be used for |
working with gamma radiation |
|
|
samples are often sterilised by passage through a sterile filter with a pore diameter of |
0.22 μm |
|
|
hundreds of tiny holes are present on each what |
sterile filter |
|
|
the holes in sterile filters detain what |
all bacteria (cell size ~1 μm) and fungi or parasites (> 1 μm) |
|
|
membrane filters composed of high tensile strength polymers (cellulose, acetate, cellulose nitrate or polysulfone) are what |
commonly used and are often used in microbiology labs |
|
|
it is important to not do what to the filter when placting it in the filtrate collection tube |
contaminate it |
|
|
pasteurisation was invented by who and when |
louis pasteur in 1864 |
|
|
what did louis pasteur discover |
that heating beer and wine was enough to kill most of the bacteria that caused spoilage, preventing these beverages from turning sour |
|
|
pasteurisation is a process that does what |
kills microbes (mainly bacteria) in food and drink, such as milk, juice, canned food, and others, without inactivating beneficial enzymes and nutrients |
|
|
unlike sterilisation, pasteurisation is not intended to do what |
kill ALL microorganisms in the food, instead aims to reduce the number of viable pathogens so they are unlikely to cause disease (assuming the pasteurised product is stored as indicated and consumed before expiration date) |
|
|
pasteurisation temperature is usually what |
72 degrees celsius for 15 min (continuous flow) or 63 degrees celsius for 30 min (batch) then immediately cooled to 5 degrees celsius |
|
|
what can modify the protocols of pasteurisation |
changes in composition, processing and use of a product the heat treatment efficiency is continuously monitored in the dairy industry |
|
|
why does cream need a treatment at 75 degrees celsius for 15 min |
because of its high fat content |
|
|
graphs of cell number vs time can be plotted for each what |
heat treatment (killing curves) |
|
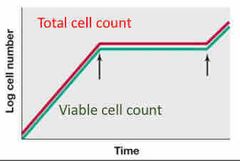
Front (Term) |
bacteriostatic |
|
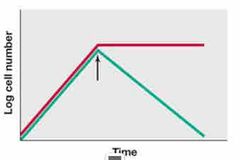
Front (Term) |
bacteriocidal |
|
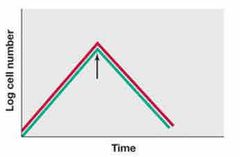
Front (Term) |
bacteriolytic |
|
|
what is an antibiotic |
antimicrobial compounds produced by microorganisms |
|
|
antibiotics are produced by what |
bacteria and fungi for killing or inhibiting the growth of their neighbours (bacteria only) |
|
|
about 70% of antibiotics are produced by what |
streptomyces other important antibiotic producing fungi are penicillium and acremonium |
|
|
only 1% of known antibiotics are used clinically because of |
their toxicity or lack of uptake by host cells |
|
|
some antibiotics can be artificially modified for improving their |
efficacy (semi-synthetic antibiotics) |
|
|
what can ergosterol inhibitor anti fungals do |
bind to ergosterol destabilising fungal cell membranes and leading to cell death - polyenes inhibit ergosterol synthesis |
|
|
what can echinocandins do |
inhibit 1,3-β-glucan synthase stopping fungal cell wall synthesis |
|
|
who invented aseptic methods |
sir joseph lister |
|
|
sterilisant |
destroy all microorganisms, including endospores use in hospital when the use of heat or radiation is impractical (catheters, thermometers) ethylene oxide (gas) |
|
|
disinfectants |
kill microorgansims but not necessarily endospores used on surfaces (phenolic compounds, cationic detergent) |
|
|
sanitisers |
less harsh than disinfectants reduce microbial numbers but do not sterilise (food industry) most used are chloride compound (sodium hypochlorite devro - collagene from cowhide) |
|
|
antiseptics (germicides) |
kill or inhibit microorganisms growth but non toxic can be applied to living tissues / surface wounds (alcohol 60-85%) |

