![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
22 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
What are the 3 main elements of blood? And what is it all suspended in? |
1. RBC (erythrocytes) 2. Platelets 3.WBC (Leukocytes)
|
|
|
|
What are the types of leukocytes or white blood cells? |
1. Granulocytes (3): eosinophil, basophil, neutrophil 2. Agranulocytes (2): monocytes & lymphocytes (small and large) |
|
|
|
Erythrocytes (RBC) Characteristics (4)? Size? Function?amount in normal adult blood? lifespan? |
1.Anucleated 2.no granules 3.Eosinophillic cell (it’ll stain pink since no nucleus) 4. Bi-concave Size: 7-7.3 microns Function: cytoplasm filled with hemoglobin which Irreversibly binds oxygen and CO2. Hemoglobin is responsible for transport and delivery of oxygen and transport of CO2 away from tissues Lifespan:120 days Accounts for about 45% of total blood volume Extras: “hematocrit” in blood panel, normally negatively charged, have antigens (A,B,O) which determines blood type. |
|
|
|
Name three cells that extrude their the nucleus to fill their cytoplasm with a class of protein in the mature state? Also list the protein. |
1.RBC, hemoglobin 2.Keratinocytes, keratin 3.lens fibers, crystallins |
|
|
|
What are reticulocytes? What is the prevalence in blood? How do they stain? An increase in reticulocytes usually means? |
I precursors are red blood cells. That is they are immature RBCs that are released from bone marrow. They mature after 1 to 2 days in the peripheral blood 1 Reticulocyte/ 100 RBCs These cells stain strands and dots of blue because they still have RNA containing organelles like free ribosomes Increase in reticulocytes due to anemia or hypoxia |
|
|
|
Platelets Whats are 2 main characteristics (2)? Go in depth if applicable Size? Prevalence in blood? Lifespan? |
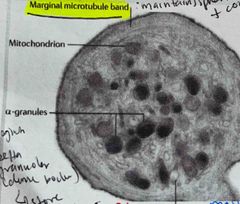
No nucleus The marginal region of the cell contains a microtubule band which maintains sphericity and produces contraction when activated. It also contains different types of granules which perform different functions 33 types of granules: 1.alpha granules which are the most common and contain proteoglycans, hemostasis factors/cofactors 2. Gamma granules Which store calcium 2+, serotonin and ATP/ADP 3. Lysosomes are membrane-bound organelles with roles in processes involved in degrading and recycling cellular waste, cellular signalling and energy metabolism Size:2-3 microns Lifespan: 5-11 days Prevalence:150k-450k /ml |
|
|
|
Steps for a blood spear (3)? |
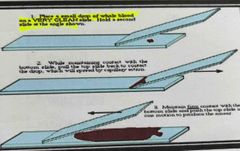
1. Place a small drop of a hole blood on a very clean slide. Hold a second slide at the angle shown 2. While maintaining contact with the bottom slide pull the top slide back to contact the drop which will spread by capillary action 3. Maintain firm contact with the bottom slide and push the top slide in one motion to produce the smear |
|
|
|
What are stains for blood smears? (2) And when is appropriate to use each? |
1. Wright stain: routine blood smears -Eosin: stains cytoplasm pink -Methylene Blue: stains nuclear material/nucleic acids Blue 2. Glemsa stain: preferred when systemic microbial disease suspected -Eosin: stains cytoplasm pink -Methylene Blue: stains nuclear material/nucleic acids Blue (lymphocytes, monocytes) -Azure B: Especially good at identifying reticulocytes and bugs |
|
|
|
What stain was used for this blood smear? |
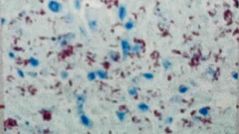
Back (Definition) |
Glemsa stain |
|
|
What stain was used for this blood smear? |
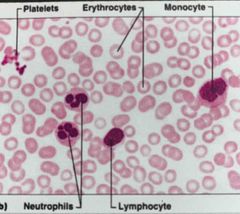
Back (Definition) |
Wrights stain |
|
|
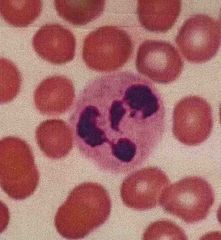
Neutrophil Characteristics (2) Functions prevalence |
Granulocytes that has very tiny light staining granules that are difficult to see because they are neutrophilic and don’t stain with blood smears. nucleus is multi lobed with the lobes connecting by strands of nuclear material phagocytosis foreign cells, bacteria, toxins and viruses Most numerous 50 to 70% of all leukocytes |
|
|
|
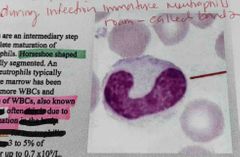
What are Bands? Main characteristic? What does an increase in bands mean? Prevalence? |
Band neutrophils are an intermediate step prior to the complete maturation of segmented neutrophils Have a Horseshoe shape nucleus not yet fully segmented like a neutrophil An increase in band of neutrophils means that the bone marrow has been singled to release more WBCs. This is called “left shift” which is often due to infection or inflammation 3-5% of WBC |
|
|
|
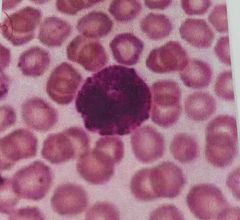
Basophil. Characteristics (2) Function? Prevalence? Leave blood? |
Basophilic granules are large and so numerous they mask the bilobed nucleus. Stain deep blue-purple. Function in inflammation mediation similar to mast cell function. Contain histamines which cause vasodilation and heparin which is a anticoagulant Less than 1% of all leukocytes Basophils do not leave blood vessels |
|
|
|
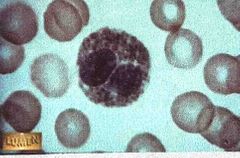
Eosinophil. Characteristics(2), function (2), prevalence, what does a high blood content mean? |
Has large granules that are pink or red and they stay in preparation Bilobed nucleus Contain digestive enzymes that are particularly effective against parasitic worms in their larval form. They also phagocytize antigen antibody complexes Less than 5% of WBC A high eosinophil content in blood usually is indicative of systemic disease |
|
|
|
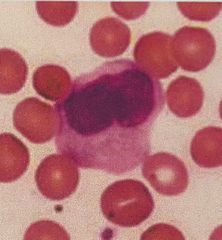
Monocytes. Characteristics (5), Function, prevalence |
Largest of all leukocytes Agranular nucleus that is often “U” shaped or kidney bean shaped Cytoplasm is abundant and light blue The cells leave the bloodstream to become macrophages as a monocyte or macrophage the cells are phagocytic and defend the body against viruses and bacteria 3 to 9% of all leukocytes Side Note: histiocyte is a form of macrophage derived from extravascular monocytes |
|
|
|
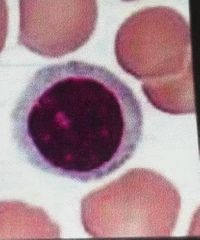
Lymphocytes. Characteristics, Function & Prevalence |
Agranular large nucleus smaller than the 3 Granulocytes T lymphocytes act against virus infected cells and tumor cells the cells B lymphocytes LEAVE the bloodstream to become plasma cells that produce antibodies second most numerous leukocyte 25 to 35% of cells |
|
|
|
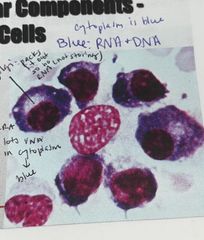
The plasma cell is derived from? |
B lymphocytes. Plasma cells then produce antibodies these have a lot of RNA in cytoplasm so they will stain blue |
|
|
|
A histiocyte is a |
A form of macrophage derived from extravascular monocytes |
|
|
|
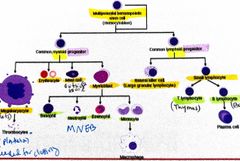
Hematopoesis is the formation of blood cellular components. During embryogenesis this process occurs ________ Postpartum this process begins in the______ Maturation of certain cells occurs in peripheral lymphoid organs-where? Differentiation ultimately occurs under tight regulations via interleukins, colony stimulating factors, TNF-alpha, TGF-beta |
Embryogenesis: Islands of cells in the yolk sac Post partum: begins in the bone marrow Maturation: T cells in thymus B cells (bursa of fabricius) in bone marrow |
|
|
|
Haematopoiesis |
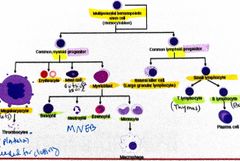
Back (Definition) |
|
|
|
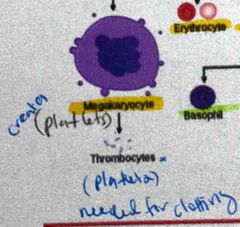
Development of platelets |
They are formed by pinching off a portion of the cell membrane and cytoplasm from the surface of a megakaryocyte |
|
|
|
What is a Erythropoeitin (EPO)? |
It is a glycoprotein hormone produced mostly by the kidneys (interstitial fibroblast) and some by the liver (peri-sinusoidal cells) Functions as cytokine acting on red blood precursers it’s production and release is stimulated by hypoxia or anemia Recombinant forms of EPO are available for treatment of anemia as following blood loss in inflammatory bowel disease or after chemo or renal dialysis |
|

