![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
35 Cards in this Set
- Front
- Back
|
What's the way that RBC are prepared?
|
1. Get blood from person
2. Spin down the blood 3. Take off the plasma 4. Save the concentrate |
|
|
How long can RBCs be stored?
|
45 days
|
|
|
How long can plasma be stored?
|
At -20, 1 year
|
|
|
What is found in cryoprecipitate?
|
High MW VWF
Fibrinogen Factor VIII |
|
|
How is cryoprecipitate formed?
|
Thaw plasma in the cold
|
|
|
How do you manufacture platelets?
|
1. Centrifuge the platelet rich plasma
2. Take off the supernatant, you've got platelets There's not enough here for 1 person, so you need to combine 4-5 units to get enough for it to be useful |
|
|
What are some different diseases that are tested for in blood?
|
HepB
HepC Trypanosoma HIV HCV West nile virus |
|
|
What are the adverse effects of blood donation?
|
Iron deficiency
Hematoma Pain at phlebotomy site Syncope |
|
|
How long is it between times that you can donate blood?
|
52 days
|
|
|
What are the componenets derived from whole blood?
|
RBCs
Platelet concentrate FFP Cryoprecipitate |
|
|
What are the storage changes in RBCs?
|
Hemolysis
K+ leakage Decreased DPG |
|
|
How long can you keep thawed plasma in the fridge?
|
5 days
|
|
|
Where do you store platelets?
|
Room temperature
|
|
|
What's the problem with platelet storage?
|
Activation
-P-selectin expression -CD40L release Granule release -B-thromboglobulin -CCL5, CXCL4, CXCL7 Lectin mediated clearance |
|
|
What kinds of red cell antibodies are there?
|
Naturally occurring
Secondary to exposure Autoantibodies |
|
|
What are the different kinds of leukocyte antibodies?
|
HLA
HNA Autoantibodies |
|
|
How do you detect red cell antibodies?
|
Direct agglutination
Indirect antiglobulin test Direct antiglobulin test |
|
|
What are you testing for with red cell direct agglutionation?
|
IgM antibodies
|
|
|
What are you testing for with red cell indirect antiglobulin test?
|
IgG antibodies
|
|
|
What are you testing for with red cell direct antiglobulin test?
|
IgG or C3 coated cells
|
|
|
How do you do an indirect antiglobulin test? What are you looking for?
|
1. Patient serum with Ab
2. Mix serum with RBCs of known phenotype 3. Wash 4. Apply anti-IgG to serum If you get a reaction, there are patient IgG antibodies against that kind of cell |
|
|
How do you do a direct antibody antiglobulin test?
|
1. Take patients cells with the stuff already on it
2. Use anticomplement, anti IgG Reaction, there are already the complement/IgG on the body |
|
|
What are the applications of the direct antiglobulin test?
|
Autoimmune hemolytic anemias
Transfusion reactions Drug-induced hemolysis Cold agglutinin disease Autoimmune diseases |
|
|
What are tests that you do before transfusing?
|
ABO typing:
-A and b antigen tests -Anti-A and Anti-B antibody test Rh(D) typing Red cell antibody screen |
|
|
What are causes of blood typing discrepancies?
|
Transplantation
Bone marrow problems/cancers Neonates (<4 months) Infections We just need to know that there are different reasons that blood can't work! |
|
|
How do you go about selecting compatible blood?
|
ABO type
Rh type Cross match |
|
|
What population do you really want to give Rh negatve blood to?
|
Women of child bearing potential
|
|
|
What are indications for a RBC transfusion?
|
Symptomatic anemia
Bleeding more than 1L Chronic hypoproliferative anemia Hemolytic anemia (sickle cell in particular) Uremic bleeding |
|
|
Based on the FOCUS and TRICC study, what are the differences between transfusing and not transfusing?
|
There's really not a difference
There is evidence that the restricted transfusion strategy is better!!! |
|
|
What level of hematocrit indicates transfusion?
|
24%
Patient usually has other symptoms |
|
|
What are indications for platelet transfusion?
|
Hemorrhage due to thrombocytopenia
Hemorrhage due to platelet dysfunction Hypoproliferative thrombocytopenia with risk of hemorrhage (<10,000/uL) Thrombocytopenia (<50,000/uL) with bleeding or invasive procedure |
|
|
What are contraindications to platelet transfusion?
|
Immune thrombocytopenic purpura
Thrombotic thrombocytopenic purpura Heparin-associated thrombocytopenia |
|
|
What are indications for plasma transfusion?
|
Multifactor coagulation factor deficiency
DIC Reversal of warfarin anticoagulation Massive transfusion Hemorrhage in liver disease Thrombotic thrombocytopenic purpura |
|
|
If a trauma comes in and they're bleeding out, how do you manage blood componenets?
|
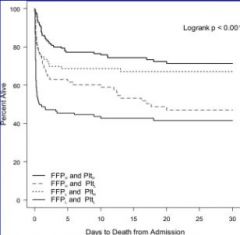
Aggressively.
Better outcomes if you transfuse platelets and plasma aggressively. |
|
|
What are indications for cryoprecipitate transfusion?
|
Factor VIII deficiency
von Willebrand's disease Hypofibrinogenemia Factor VIII deficiency Uremic bleeding |

