![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
133 Cards in this Set
- Front
- Back
|
Anatomical Position
|
Subject stands erect facing the observer with the head level and the eyes facing directly forward. The feet are flat on the floor and directed forward, the upper limbs are at the sides with the palms turned forward.
|
|
|
levels of body organization
|
1.) chemical
2.) cellular 3.) tissue 4.) organ 5.) system 6.) organism |
|
|
differentiation
|
the development of a cell from an unspecialized state to a specialized state
|
|
|
responsiveness
|
the body's ability to detect and respond to changes internally and externally
|
|
|
homeostasis
|
the condition of equilibrium in the body's internal environment
|
|
|
negative feedback system
|
reverses a change in a controlled condition
[e.g. blood pressure] |
|
|
positive feedback system
|
strengthens/reinforces a change in one of the body's controlled conditions
[e.g. childbirth] |
|
|
intracellular fluid
|
ICF
fluid within the cells |
|
|
extracellular fluid
|
ECF
fluid outside body cells differs depending on where it occurs in the body |
|
|
pH
|
A solution's acidity or alkalinity is expressed on this scale [0-14]
pH <7 acidic pH =7 neutral pH >7 basic |
|
|
Phospholipids
|
hydrophilic heads and hydrophobic tails
|
|
|
three main parts of an animal cell
|
plasma membrane
cytoplasm nucleus |
|
|
plasma membrane
|
Made up of a phospholipid layer, forms the cell's outer boundary and separates the cell's internal environment from the outside environment
5% glycolipids 20% cholesterol (contributes to fluidity) Amphipathic: polar heads and nonpolar tails Selectively permeable More concentrated inside than outside the cell More positive inside and more negative outside |
|
|
integral proteins
|
Extend into or through the lipid bilayer among the fatty acid tails and are firmly embedded
|
|
|
transmembrane proteins
|
Span the entire lipid bilayer and protrude into both the cytosol and the extracellular fluid
|
|
|
vesicular transportation
|
endocytosis
exocytosis transcytosis |
|
|
endocytosis
|
A highly selective type of endocytosis by which cells take up specific ligands,
a vesicle forms after a receptor protein in the plasma membrane recognizes and binds to a particular particle in the extracellular fluid |
|
|
exocytosis
|
Releases materials from a cell
|
|
|
transcytosis
|
vesicles undergo endocytosis on one side of a cell, move across the cell, and then undergo exocytosis on the opposed side
|
|
|
active transport
|
movement of substances against the concentration gradient
requires cellular energy (ATP) |
|
|
passive transport
|
movement of substances down a concentration gradient until equilibrium is reached
no energy required |
|
|
factors that influence diffusion
|
steepness of the concentration gradient
temperature mass of the diffusing substance surface area diffusion distance |
|
|
transcription
|
Occurs in the nucleus, the DNA is used as a template to make an RNA strand
|
|
|
translation
|
Occurs in the cytoplasm, the mRNA is used as a template by amino acids to produce a protein strand
|
|
|
DNA nucleotides
|
cytosine
guanine thymine adenine |
|
|
RNA nucleotides
|
cytosine
guanine thymine uracil |
|
|
Mitosis
|
The distribution of two sets of chromosomes into two separate nuclei [PMAT]
|
|
|
prophase
|
The chromatin condenses into chromosomes, the mitotic spindle begins to form, and the nuclear envelope disappears
|
|
|
metaphase
|
The microtubules of the mitotic spindle align the centromeres of the chromatid pairs at the metaphase plate
|
|
|
anaphase
|
The centromeres split, separating the two members of each chromatid pair and pulling them towards opposite poles of the cell
|
|
|
telophase
|
After chromosomal movement stops, the chromosomes uncoil and revert to chromatin. A nuclear envelope forms around each mass and the mitotic spindle breaks up
|
|
|
tight junctions
|
Fuse together the outer surfaces of adjacent plasma membranes to seal off passageways between adjacent cells
|
|
|
adherens juntions
|
attach both to membrane proteins and to microfiliments of the cytoskeleton to join two cells
|
|
|
desmosomes
|
Extend into the intercellular space between adjacent cell membranes and attach cells to one another
|
|
|
hemidesmosomes
|
Attach to intermediate filaments made of the protein keratin and anchor cells to the basement membrane
|
|
|
gap junctions
|
Connect neighbouring cells and allow the cells in tissue to communicate with one another and enable nerve or muscle impulses to spread rapidly among cells
|
|
|
epithelial tissue
|
tightly packed with little or no extracellular matrix
|
|
|
connective tissue
|
large amount of extracellular matrix that separates the cells which are usually widely scattered
|
|
|
types of epithelial tissue
|
-simple squamous epithelium (lines heart & blood vessels)
-simple cuboidal epithelium (kidney) -simple columnar epithelium (& ciliated) (bronchioles) -pseudostratified columnar epithelium (lines airways) -stratified squamous epithelium (skin) -stratified cuboidal epithelium (sweat glands) -stratified columnar epithelium (esophageal glands) -transitional epithelium (urinary bladder) |
|
|
exocrine gland secretion
|
granular epithelium
produce substances (sweat) to help lower body temperature, oil, earwax, saliva or digestive enzymes |
|
|
types of connective tissue
|
-areolar (in & around nearly every body structure)
-adipose (fat tissue) -reticular (supporting frameworks) -dense regular (tendons, ligaments, & aponeuroses) -dense irregular (beneath skin & around muscles) -elastic (lungs, arteries, trachea, bronchial tubes) |
|
|
stroma
|
New cells originate by cell division from this supporting connective tissue
|
|
|
stem cells
|
immature, undifferentiated cells that divide to replace lost or damaged cells
|
|
|
layers of the skin
|
epidermis
dermis |
|
|
epidermal layer
|
The superficial, thinner portion which covers the deeper layers of skin
(bottom to top): stratum basale, stratum spinosum, status granulosum, stratum lucidum, stratum corneum |
|
|
keratinization
|
keratinocytes produce the protein keratin which helps protect the skin and underlying tissues from abrasions, heat, microbes, and chemicals. They also produce lamellar granules, which release a water-repellant sealant that decreases water entry and loss and inhibits the entry of foreign materials
|
|
|
skin colour
|
the amount of melanin causes the skin's colour to vary from pale yellow to reddish-brown to black
pheomelanin (yellow to red) eumelanin (brown to black) |
|
|
deep wound healing
|
inflammatory phase - formation of blood clot
migratory phase - clot becomes a scab, wound is filled with granulation tissue proliferative phase - growth of epithelial cells beneath the scab maturation phase - scab sloughs off once the epidermis has been restored |
|
|
fibrosis
|
process of scar tissue formation
|
|
|
types of scars
|
hypertrophic - remains within the boundaries of the original wound
keloid/cheloid - extends beyond the original boundaries of the wound |
|
|
burn classification system
|
first degree burn - epidermis
second degree burn - epidermis and dermis third degree burn - epidermis, dermis, and subcutaneous layers |
|
|
types of bone cells
|
Osteogenic, osteoblasts, osteocytes, and osteoclasts
|
|
|
osteogenic cells
|
Precursor cells that develop into an osteoblast by cell division
|
|
|
osteoblasts
|
For the bone extracellular matrix, and develop into osteocytes
|
|
|
osteocytes
|
Maintain bone tissue, mature bone cells
|
|
|
osteoclasts
|
Take away components of bone derived from monocytes (resorption)
|
|
|
hormones involved in bone formation
|
parathyroid hormone (PTH)
calcitriol calcitonin (CT) |
|
|
osteon
|
![Central canal [blood and lymphatic vessels found here]
concentric lamellae
lacunae [small spaces between the lamallae, house osteocytes]
canaliculi [small channels filled with extracellular fluid connecting the lacunae]
interstitial lamallae
...](https://images.cram.com/images/upload-flashcards/43/33/78/3433378_m.png)
Central canal [blood and lymphatic vessels found here]
concentric lamellae lacunae [small spaces between the lamallae, house osteocytes] canaliculi [small channels filled with extracellular fluid connecting the lacunae] interstitial lamallae Volkmann's canals (perforating) [allow transit of these vessels to the outer cortex of the bone] circumferential lamallae [outer encircles the bone beneath the periosteum, inner encircles the medullary cavity] perforating sharpey's fibres |
|
|
types of fractures
|
open (compound) - simple fracture, no broken skin
comminuted - bone is splintered, crushed, or broken into pieces greenstick - partial fracture impacted - one end of the fractured bone is forcefully driven into the other Pott - fracture to the distal end of the fibula Colles' - fracture to the distal end of the radius |
|
|
function of the skeletal system
|
support
protection movement mineral homeostasis blood cell production triglyceride storage |
|
|
anatomy of a long bone
|
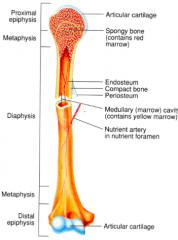
diaphysis
epiphyses metaphyses articular cartilage periosteum medullary cavity endosteum |
|
|
types of bones
|
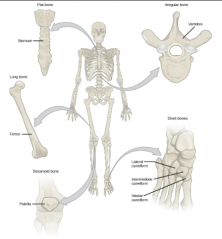
long
flat irregular short sesamoid |
|
|
fetal v. adult vertebral column
|
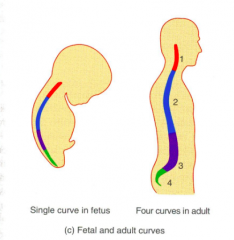
fetal: Single concave curve
adult: Four curves, two concave and two convex Primary: Thoracic and Sacral curves that retain the concave shape Secondary: Cervical and Lumbar curves that grow to be convex |
|
|
scoliosis
|
Lateral bending of the vertebral column in the thoracic region
|
|
|
kyphosis
|
Hunchback
Increase in the thoracic curve |
|
|
lordosis
|
Increase in the lumbar curve
"hollow back" |
|
|
sequence of regions of the vertebral column
|
![cervical (7)
thoracic (12)
lumbar (5)
sacral (2)
[26 in all]](https://images.cram.com/images/upload-flashcards/43/37/23/3433723_m.png)
cervical (7)
thoracic (12) lumbar (5) sacral (2) [26 in all] |
|
|
male pelvis
|
Heavy
Rough Large Vertical Narrow true pelvis Tilted forward Pelvic inlet is heart shaped <90 degree pubic arch angle |
|
|
female pelvis
|
Small
Light Large true pelvis Tilted forward Flared Pelvic inlet is round or oval >90 degree pubic arch angle Wide sciatic notch |
|
|
directional terms
|
Posterior
Anterior Lateral Medial Superior Inferior Distal Proximal Contralateral Ipsilateral superficial deep |
|
|
joints of the pectoral shoulder girdle
|
sternoclavicular joint (sternum and clavicle)
acromioclavicular joint (scapula and clavicle) glenohumeral joint (scapula and humerus) |
|
|
functional classification of joints
|
Relates to the degree of movement the joint permits
Synarthrosis Amphiarthrosis Diarthrosis |
|
|
synarthrosis joints
|
immovable joints
|
|
|
amphiarthrosis joints
|
slightly movable joints
|
|
|
diathrosis joints
|
freely movable joints
all are synovial joints |
|
|
lower limb bones
|
femur (1)
patella (1) tibia (1) fibula (1) tarsals (7) metatarsals (5) phalanges (14) [30 in all] |
|
|
joint diseases
|
Rheumatoid Arthritis
Osteoarthritis Gouty Arthritis |
|
|
rheumatoid arthritis
|
Joints are swollen, stiff and painful
Body attacks its own tissues Inflammation of the joints Loss of function Occurs bilaterally |
|
|
osteoarthritis
|
Due to wear and tear of the body
degenerative joint disorder joint cartilage is gradually lost ends of the bones are exposed bones grow more and create spurs, which add to the discomfort first the hips and the knees effected mainly the articular cartilage |
|
|
gouty arthritis
|
build up of uric acid in the blood
reacts with sodium and creates crystals that accumulate in the tissues of joints kidneys and feet effected associated with a lot of alcohol and red meat intake |
|
|
connective tissue layers
|
epimysium
perimysium endomysium |
|
|
epimesium
|
The outermost layer of dense, irregular connective tissue, encircling the entire muscle
|
|
|
perimysium
|
A layer of dense, irregular connective tissue
Surrounds groups of 10-100 or more muscle fibres, separating them into bundles called fascicles |
|
|
endomysium
|
Penetrates the interior of each fascicle and separates individual muscle fibre from one another
Reticular fibres |
|
|
sarcolemma
|
The plasma membrane of a muscle cell
|
|
|
sarcoplasm
|
The cytoplasm of a muscle fibre
|
|
|
T-tubles
|
Tiny invaginations of the sarcolemma that tunnel in from the surface toward the centre of each muscle fibre
|
|
|
myofilaments
|
Protein structures within myofibrils
Thin filaments: composed mostly of protein actin Thick filaments: composed mostly of the protein myosin Both are directly involved in the contractile process 2 thin filaments for ever thick filament |
|
|
sarcomere
|
The basic functional units of a myofibril
The filaments inside a myofibril are arranged in these compartments |
|
|
motor unit
|
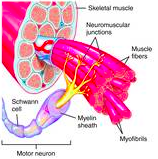
Consists of a somatic motor neuron plus all the skeletal muscle fibres it stimulates
A single one makes contact with an average of 150 skeletal muscle fibres All of the muscle fibres in one unit contract in unison |
|
|
sarcomere regions
|
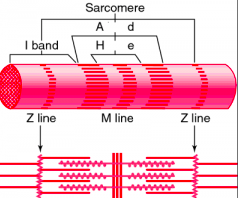
Z disc - separates one sarcomere from the next
M line - hold the thick filaments together at the centre I band - thin filaments A band - extends the length of the thick filaments H zone - thick filaments |
|
|
role of calcium in contraction
|
An increase in Ca ion concentration in the sarcoplasm starts muscle contraction, and a decrease stops it
Stored inside the sarcoplasmic reticulum Binds with troponin |
|
|
sliding filament theory
|
1.) ATP hydrolysis: myosin heads hydrolyze ATP and become reoriented and energized
2.) Attachment of myosin to actin to form cross-bridges 3.) Power stroke: Myosin cross-bridges rotate towards the centre of sarcomere 4.) Detachment of myosin from actin: as myosin heads bind to ATP, the cross-bridges detach from actin |
|
|
Acetylcholinesterase
|
Breaks down ACh after a short period of time (enzyme)
|
|
|
neuromuscular junction
|
NMJ
synapse between a somatic motor neuron and a skeletal muscle fibre |
|
|
blood types
|
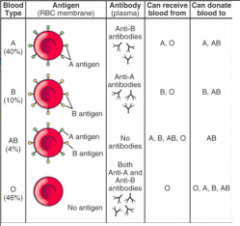
A, B, AB, O
|
|
|
why is type O the 'universal donor'?
|
type O blood has no antigens on it, so the antibodies of any other blood type would not attack it
|
|
|
erythropoiesis
|
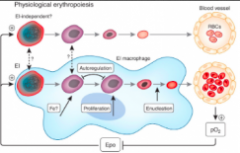
Production of RBCs
Increased in low levels of O2 life span: 120 days |
|
|
polycythemia
|
The percentage of RBCs is abnormally high
The hematocrit may be 65% or higher |
|
|
thrombocyte formation
|
platelets
pluripotent stem cells - myeloid stem cells - megakaryoblasts - megakaryocytes - thrombocytes (platelets) lifespan: 5-9 days |
|
|
function of plasma proteins
|
antibodies or immunoglobulins
produced during immune responses to fight foreign substances |
|
|
function of hemoglobin
|
transports oxygen through the blood and releases it into the interstitial fluid and then into the cells
transports 23% of CO2 out of the body regulation of blood flow and blood pressure |
|
|
electrocardiogram (ECG)
|
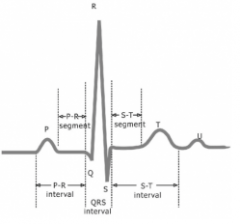
Recording of the electrical current as APs pass through the heart
P wave - atrial depolarization (atrial contraction) QRS Complex - ventricular depolarization and atrial repolarization (ventricular contraction & atrial relaxation) T wave - ventricular repolarization (right ventricular relaxation) P-Q interval - conduction time from the beginning of atrial excitation to the beginning of ventricular excitation S-T segment - ventricular fibres are depolarized during the plateau phase of the action potential Q-T interval - time from the beginning of ventricular depolarization to the end of ventricular repolarization |
|
|
heart sounds
|
'lubb' - closure of AV valves
'dupp' - closure of SL valves |
|
|
the path of blood through the pulmonary and systemic circulations
|
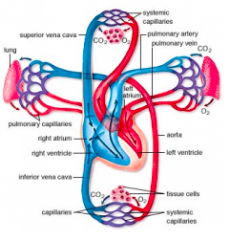
Right atrium
Tricuspid valve Right Ventricle Pulmonary Valve Pulmonary Trunk Pulmonary Arteries Pulmonary Capillaries Pulmonary Veins Left Atrium Bicuspid Valve Left Ventricle Aortic Valve Aorta Systematic Arteries Systematic Capillaries Systematic Veins Superior and Inferior Vena Cava Coronary Sinus Right atrium |
|
|
atrioventricular valves
|
bicuspid and tricuspid
|
|
|
semilunar valves
|
aortic and pulmonary
|
|
|
action potential through the heart
|
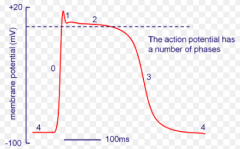
step 1: Depolarization - threshold is reached and AP starts, opens Na+ gated channels (fast) and inflow into muscle fibre produced rapid depolarization
step 2: Plateau - maintains depolarization, Ca+2 gated channels (slow) open and inflow into cytosol through the sarcolemma into the cardiac fibre step 3: Repolarization: Recovery of Resting Membrane Potential, K+ gated channels are opened and outflow closes Ca+2 and Na+ channels |
|
|
hypovolemic shock
|
caused by decreased blood volume
|
|
|
function of baroreceptors
|
send impulses to the cardiovascular centre to help regulate blood pressure
|
|
|
location of the cardiovascular centre
|
the middle of the medulla oblongata
|
|
|
signs and symptoms of shock
|
systolic blood pressure lower than 90 mmHg
resting heart rate is rapid weak pulse cool, pale, and clammy skin altered mental state reduced urine formation the person is thirsty pH of blood is low nausea |
|
|
response of the cardiovascular system to a decreased frequency of action potentials from the baroreceptors
|
the cardiovascular centre decreases parasympathetic stimulation of the heart and increases sympathetic stimulation of the heart
|
|
|
tunic layers of arteries
|
tunica interna: endothelium, basement membrane, internal elastic lamina
tunica media: smooth muscle, external elastic lamina tunica externa (elastic and collagen fibres) |
|
|
tunic layers of veins
|
tunica interna: endothelium, basement membrane
tunica media: smooth muscle tunica externa (elastic and collagen fibres) |
|
|
tunic layers of capillaries
|
endothelium
basement membrane |
|
|
elastic arteries vs. muscular arteries
|
elastic: largest, thin vessel walls, internal and external elastic laminae, "conducting arteries", help propel blood onward while the ventricles are relaxing
muscular: "distributing arteries", more smooth muscle and fewer elastic fibres, maintain proper vascular tone |
|
|
filtration
|
the movement of fluid through the walls of the capillary into the interstitial fluid
|
|
|
reabsorption
|
the movement of fluid from the interstitial fluid back into the capillary
|
|
|
epinephrine
|
Adrenalin
Released from the adrenal medulla as an endocrine auto regulatory response to sympathetic stimulation Increase cardiac output by increasing rate and force of heart contractions |
|
|
antidiuretic hormone (ADH)
|
Released from the posterior pituitary gland in response to dehydration or decreased blood volume
Causes vasoconstriction, increases BP |
|
|
atrial naturetic peptide (ANP)
|
A natural diuretic polypeptide hormone released by cells of the cardiac atria
Participates in auto regulation by lowering blood pressure (vasodilation) and reducing blood volume (promoting loss of salt and water as urine) |
|
|
fate of lipids
|
may be oxidized to produce ATP
structural molecules or molecules to synthesize other essential substances if there is no immediate need for them, they are stored in adipose tissue |
|
|
lipid profile test
|
LDL = Total cholesterol + HDL + Triglycerides
|
|
|
ATP breakdown into ADP and phosphate
|
ATP = ADP + P + energy
|
|
|
glucose movement across the plasma membrane
|
secondary active transport or facilitated diffusion
|
|
|
catabolism
|
chemical reactions that break down complex organic molecules into smaller ones
|
|
|
anabolism
|
chemical reactions that combine simple molecules and monomers to form the body's complex structural and functional components
|
|
|
oxidation
|
the removal of electrons from an atom or molecule
decrease in potential energy |
|
|
reduction
|
addition of electrons to a molecule
increase in potential energy |
|
|
chylomicrons
|
transportation of dietary lipids
|
|
|
examples of elastic arteries
|
aortic
pulmonary brachiocephalic subclavian common carotid common iliac |
|
|
cardiac output
|
stroke volume x heart rate
total blood flow |

