![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
19 Cards in this Set
- Front
- Back
|
What does innate mean?
|
inborn, not acquired
|
|
|
What are some examples of innate immunity?
|
-barriers such as skin, mucus on mucous membranes
-cells including neutrophils, macrophages, and natural killer cells |
|
|
What are 3 attributes of innate immunity?
|
-Rapid (hours) response
-not specific -no memory |
|
|
What triggers an innate immunity?
|
-Receptors for opsonins - CR1, CR3, FcyRI, receptor for C1q
-Pattern Recognition Receptors (PRRs) on host cells recognize broad structural motifs highly conserved in microbial species ---toll-like receptor family, scavenger receptors -Pathogen-associated molecular patterns (PAMPs) ---Lipopolysaccharide (LPS - powerful stimulus of innate immunity), N-formyl-methionyl peptides (f-met leu phe), DNA sequence CpG - unmethylated cytosine linked to guanine which is abundant in microbial DNA |
|
|
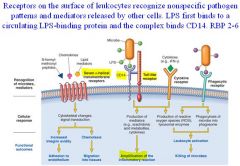
Receptors on the surface of leukocytes recognize nonspecific pathogen patterns and mediators released by other cells. LPS first binds to a circulating LPS-binding protein and the complex binds CD14.
|
|
|
|
What are the 2 TLR (toll-like receptors) that we need to know for innate immunity and what microbes they react to?
|
-TLR6 - gram-positive bacteria and fungi
-a dimer of TLR4 - gram-neg bacteria (TIR, Toll/IL-1 receptor is the intracellular domain) |
|
|
What are the 4 outcomes of acute inflammation?
|
-Resolution - clearance of stimulus, inflammatory cells and mediators; return to normal
-Chronic inflammation - persistent injury, inability to clear infection -Abscess formation - a walled off purulent infiltrate; certain bacterial infections are likely to result in abscesses -Healing can occur agter acute inflammation, chronic inflammation, or abscess and may involve - regeneration and or scarring |
|
|
What are the 3 processes occurring in chronic inflammation?
|
-Active inflammation
-Tissue destruction -Attempts at repair - regeneration, fibrosis, angiogenesis |
|
|
What are some common causes of chronic inflammation?
|
-persistent infections - mycobacteria, fungi, T. pallidum, viral e.g. hepB
-prolonged exposure to toxic agents - e.g. silicosis -autoimmunity - e.g. rheumatoid arthritis (may result from acute inflammation or develop insidiously) |
|
|
Who is the key player in chronic inflammation?
|
the MACROPHAGE
-monocyte to macrophage --extravasate and become larger ---capable of phagocytosis |
|
|
What activates the macrophage and what does the macrophage activate?
|
-transformation by chemical mediators or cytokines
-larger, more lysosomal enzymes -secrete many products - systemic affects, activate other cells such as fibroblasts and lymphocytes |
|
|
What are the products of a Macrophage?
|
-enzymes that cause tissue destruction - collagenase, proteases, elastase, etc
-Reactive oxygen metabolites -Cytokines (IL-1, TNFalpha, IL-8) -Growth factors (PDGF, EGF, FGF, TGFalpha, TGFbeta) -Nitric oxide -arachidonic acid metabolites |
|
|
What macrophages to accumulate?
|
-continued recruitment from circulation - primary source for additional macrophages
-local proliferation - mitosis -immobilization - cytokine MIF (migration inhibitory factor) |
|
|
What are some histilogic features of chronic inflammation?
|
-Infiltration of "mononuclear" leukocyts: lymphocytes, plasma cells, and macrophages are "mononuclear" b/c nucleus in not multilobed
---sometimes mast cells and eosinophils are present ---neutrophils may still be present -Tissue destruction -Attempts at healing - collagen deposition and angiogenesis |
|
|
What is Granulomatous inflammation?
|
a distinctive pattern of chronic inflammation
-predominant cell is the activated macrophage - epithelial like appearance = epithelioid macrophage -Often multinucleate giant cells are present - from the fusion of many macrophages +/- granulomas - focal area of granulomatous tissue - epithelioid macrophages surrounded by mononuclear cells and often some fibroblasts ---central area may or may not be necrotic material |
|
|
What are the causes or types of Granulomas?
|
-Foreign body - irritating substance such as talc, suture
-Immune - persistent infection e.g. tuberculosis -enknown etiology - sarcoidosis (granulomas are not static - cell and cytokine interactions maintain them) |
|
|
What are the 2 types of tissue repair?
|
Regeneration - replacement of injured tissue by cells of same type
-regeneration of epithelium requires an INTACT BASEMENT MEMBRANE Fibrosis - replacement by connective tissue -results in a scar -if the ECM has been destroyed, tissue can only heal by fibrosis (both processes usually occur at same time) |
|
|
What are some requirements for regeneration to be viable?
|
-Cells must have proliferative potential in order to regenerate
---either labile or stable cells can regenerate ---cells such as cardiac myocytes and motor neurons cannot regenerate -Normally, the population of cells inn a tissue remains the same after reaching adult size ---the increase by proliferation = the decrease due to apoptosis and differentiation |
|
|
What are labile, stabile, and permanent cells?
|
Labile - continuously cycling/dividing, renewing cells (slow or rapid)
Stable - faculative dividers, quiescent Permanent - terminally differentiatied, static cells |

