![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
71 Cards in this Set
- Front
- Back
|
sagittal plane
(and alternative name) |
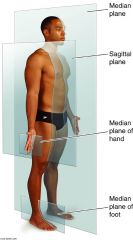
anteroposterior
|
|
|
Frontal plane
(alternative name?) |

coronal plane
|
|
|
transverse plane
(alternative name?) |
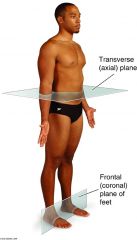
horizontal plane
|
|
|
internal-external
|
nearer to -or- farther from the center
|
|
|
Rostral
|
used in describing the brain
nearer anterior part of head |
|
|
caudal- cranial
|
toward tail region -or- toward the head
|
|
|
unilateral- bilateral
|
occuring on one side -or- having right and left members
|
|
|
circumduction
|
distal end circular movement
|
|
|
rotation
|
revolving around longitudinal axis
|
|
|
medial/ internal rotation
|
brings anterior surface closer to median plane
|
|
|
eversion- inversion
|
movement of sole away from median plane -or- movement of sole toward median plane
|
|
|
reposition
|
movement from opposition back to anatomical position
|
|
|
retrusion
|
opposite of protrusion
movement backward of chin/lips/tongue |
|
|
integumentary functions
|
protection
excretion regulate body temp produce vitamin D storage lipids in adipocytes extend range of nervous system |
|
|
layers of integumentary
|
Epidermis, Dermis, subcutaneous tissue (superficial fascia-- not really part of skin)
|
|
|
Epidermis
|
-keratinized epithelium
-tough, protective outer layer over regenerative, pigmented basal layer -no blood vessels or lymphatics |
|
|
keratin cells in epidermis
|
are horny like substances made of proteins
|
|
|
stratum germinativum (aka stratum basale)
|
-single row of rapidly dividing stem cells
-hemidesmosomes attach it to underlying dermis -epidermal ridges increase surface connection with dermis -basal cell carcinoma originates in stem cells of this layer. |
|
|
hemidesmosomes
|
attach one cell to the extracellular matrix
attach stratum germinativum to underlying dermis. |
|
|
integumentary functions
|
protection
excretion regulate body temp produce vitamin D storage lipids in adipocytes extend range of nervous system |
|
|
layers of integumentary
|
Epidermis, Dermis, subcutaneous tissue (superficial fascia-- not really part of skin)
|
|
|
Epidermis
|
-keratinized epithelium
-tough, protective outer layer over regenerative, pigmented basal layer -no blood vessels or lymphatics |
|
|
keratin cells in epidermis
|
are horny like substances made of proteins
|
|
|
stratum germinativum (stratum basale)
|
-single row of rapidly dividing stem cells
-hemidesmosomes attach it to underlying dermis -epidermal ridges increase surface connection with dermis -basal cell carcinoma originates in stem cells of this layer |
|
|
5 epidermal layers- starting superficial
|
1. stratum corneum
2. stratum lucidum 3. stratum granulosum 4. stratum spinosum 5. stratum germinativum |
|
|
basal cell carcinoma
|
-type of non-melonoma skin cancer
-most common cancer in US -accounds for 75% of skin cancer -rarely metastasizes -occurs on skin regularly exposed to sun/ UV radiation -appears as flat lesions |
|
|
hemidesmosomes
|
attach one cell to the extracellular matrix
attach stratum germinativum to underlying dermis |
|
|
stratum spinosum
|
-8-10 cells thick
-langerhans' cells -keratinocytes continue to divide -squamous cell carcinoma originates in keratinocytes here |
|
|
Langerhans' cells
|
take up and process microbial antigens during skin infections
|
|
|
squamous cell carcinoma
|
-2nd most common
-appears crusted/ scaly patches w/ red, inflamed base or growing tumor -slow-growing malignant tumor -frequently found in lungs and skin (also occuring in anus, cervix, larynx, nose, and bladder) |
|
|
Melanoma
|
-malignant tumor of melanocytes (cells that produce pigment melanin)
-predominantly in skin -less common--more deadly (75% deaths related to skin cancer) |
|
|
stratum granulosum
|
-3-5 cells thick
-cells become flattened -cells produce toughening keratin and keratohyaline granules |
|
|
stratum lucidum
|
-very thin layer
-found only in thick skin -densely packed with keratin |
|
|
stratum corneum
|
-15-30 cells thick
-cells dead -accounts for 3/4 of epidermal thickness -cells very tough and water resistant |
|
|
dermis
|
-vascularized/contains nerve endings
-dense, interlacing collagen and elastic fibers -provides skin tone/ strength and toughness -fiber direction provides tension lines (langer lines) |
|
|
langer lines
|
tension lines in skin
in cuts, if you cut along a langer line the wound will close up nice. if you cut across, the would will gap |
|
|
dermal layers
|
papillary layer
reticular layer |
|
|
papillary layer
|
-areolar connective tissue
-collagen/elastin fibers form loose mat -abundant blood vessels, nerve fibers, lymphatic vessels -superior surface forms dermal papillae |
|
|
areolar connective tissue
|
connective tissue, loosely organized
|
|
|
reticular layer
|
-80% dermal thickness
-primarily dense irregular connective tissue -collagen/elastin fibers extend up into papillary layer and down into subcutaneous layer |
|
|
dermal papillae
|
form fingerprints
form superficial layer of dermis--protrude into epidermal layer |
|
|
erythema
|
unusually red
heat, inflammation, allergic reactions-- superficial capillary bedsengorged |
|
|
stretch marks
|
rapid changes stretch skin "too much" damaging collagen fibers in dermis
deep fascia is loosened due to protein breakdown--leading to reduced cohesion btw collagen fibers |
|
|
fascia
|
layer or boundar in body
fascia suround all our muscles, etc... |
|
|
1st degree burn
|
limited to epidermis
cells quickly replaced from basal layer |
|
|
2nd degree burn
|
epidermis and superficial dermis
-nerve endings damaged, hair follicle or sweat glands provide replacement cells for basal layer |
|
|
3rd degree burn
|
entire thickness and possible underlying muscle
marked edema--are numb because sensory endings destroyed |
|
|
topical medications/ ointments
|
drug administered to skin or mucous membrane
lipid-soluble more readily absorbed |
|
|
transdermal patches
|
attach to skin by adhesive layers
may be mixed with oily base to increase solubility provide slow, controlled release to ensure constant plasma level of drug |
|
|
functions of skeletal system
|
-support
-protection -leverage necessry for movement -mineral and lipid storage -blood cell production |
|
|
short bones
|
roughly cube shaped
|
|
|
sesamoid bones
|
form within tendons and frequently alter the direction of muscle pull. variable
ex patella |
|
|
sutural bones
|
(wormian bones)
small flattened bones in skull. variable |
|
|
bone composition
|
-calcium carbonate and calcium phosphate (60-70% dry weight; provides rigidity, compressive strength)
-collagen protein (provides flexibility, tensile strength) -water (25-30% weight, contributes to strength) |
|
|
compact bone (cortical bone)
|
external part of bone
looks smooth and solid to naked eye |
|
|
spongy bone (trabecular bone)
|
(cancellous bone)
-internal part of bone -honeycomb of osseous -tissue called trabeculae filled with bone marrow has vertical and horizontal columns that resist force |
|
|
diaphysis
|
-shaft of LONG bone
-compact bone externally -central medullary cavity contains bone marrow |
|
|
epiphyses
|
-end of LONG bone, larger diameter than diaphysis
-compact bone externally -spongy bone internally |
|
|
structure of flat bone
|
-layer of spongy bone btw compact bone (dipole)
-spongy bone contains bone marrow, althogh no marrow cavity is present |
|
|
periosteum
|
-covers outer surface of bone except joint surface
-outer layer dense irregular connective tissue -inner layer composed primarily of osteoprogenitor cells along with osteoblasts and osteoclasts -richly supplied with blood vessels, nerve fibers, lymphatic vessels -continuous with joint capsules, tendons, ligaments |
|
|
endosteum
|
-covers trabeculae of spongy bone and lines canals that pass through compact bone
-composed of osteoprogenitor cells with osteoblasts and osteoclasts -lacks dense irregular connective tissue present in periosteum |
|
|
osteoprogenitor cells
|
becomes osteoblast and osteoclast
|
|
|
osteogenesis (ossification)
|
process of bone tissue formation
-in embryos--leads to development of body skeleton -before adulthood--leads to growth of skeleton -in adulthood--leads to increase in thickness of bones--remodeling and repair of bones |
|
|
embryonic development of bone--two different tissue types bone develops from
|
1. fibrous CT
-intramembranous ossification (leads to formation of most bones in skull and miscellaneous other bone) 2. hyaline cartilage -endochondral ossification (bones of skeleton from base of skull down (some exceptions) |
|
|
osteoclasts
|
of endosteum and spongy bone/ compact bone interface remove internal bone (keeps bones light)
|
|
|
bone growth in length
|
extension of endochondral ossification (i.e. cartilage forms and is replaced by bone)
|
|
|
adult bone
|
increasing loss of collagen
age-related decline in density trabecular bone affected |
|
|
Type 1 osteoporosis
|
post menopausal osteoporosis
40% women over 50 |
|
|
Type II osteoporosis
|
age associated osteoporosis
-affects most women -men after age 70 -90% of all fractures after age 60 related to osteoporosis |
|
|
dowager's hump-- cause
|
crush fractures of trabecular bone in vertebrae
|
|
|
fibrous joints
|
connected by fibrous tissue
1. syndemosis type-- partially moveable- connected by sheet of ligament of fibrous membrane 2. gomphosis type- peg-like process and socket |

