![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
29 Cards in this Set
- Front
- Back
|
What are the FUNCTIONS of the skeletal system? |
-Support -Blood Formation -Protection -Storage of Minerals -Shape -Movement |
|
|
What are the 4 types of BONE cells? |
1. Osteogenic 2. Osteoblast 3. Osteocyte 4. Osteoclast
REMEMBER! oste- : bone -genic : "produced or reproduced" -blast : immature, precursor cell -cyte : cell -clast : "something that breaks" |
|
|
Define OSTEOGENIC CELL |
"osteo-" meaning bone "-genic" meaning produced or reproduced
osteogenic cells are undifferentiated cells under the peri- and endosteum, able to divide, or differentiate into OSTEOBLASTS |
|
|
Define OSTEOBLAST |
"osteo-" meaning bone "-blast" meaning immature precursor cell
osteoblasts are immature precursor cells that produce matrix and collagen fibers - they CANNOT divide. once surrounded by matrix, they differentiate into OSTEOCYTES |
|
|
Define OSTEOCYTE |
"osteo-" meaning bone "-cyte" meaning cell
osteocytes are mature bone cells. They are enclosed in LACUNAE, and surrounded by calcified bone matrix. Responsible for tissue maintenance. Connect with other osteocytes through CANALICULI |
|
|
Define OSTEOCLAST |
"osteo-" meaning bone "-clast" meaning "something that breaks"
osteoblasts are cells formed from fused white blood cells. They are located beneath the periosteum and endosteum, and secrete an enzyme that dissolves bone matrix. |
|
|
What is the composition of BONE MATRIX? |
15% water (lacunae and ICF) 30% organic matrix (collagen fibers -> strength, flexibility) 55% inorganic matrix (mineral salts -> hardness) |
|
|
What is MINERALIZATION? |
MINERALIZATION (or calcification) is the hardening of tissue when mineral crystals deposit around collagen fibers |
|
|
Define the organization and components of COMPACT BONE |
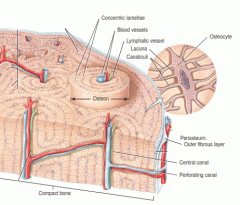
Osteon : repeating structural units Haversian Canal Volkmann's Canal Concentric Lamellae |
|
|
Define the organization and components of SPONGY BONE |
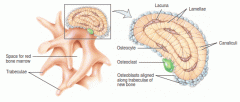
Trabeculae |
|
|
Name the bones of the body that contain RED MARROW |
Flat bones: cranial bones, pelvis, ribs, sternum Proximal femur, proximal humerus |
|
|
What are the two types of BONE FORMATION? |
Intramembranous bone formation (from mesenchymal cells) Endochondral bone formation (from cartilage model) |
|
|
Step 1 : Intramembranous Ossification |
At ossification center (future bone site), mesenchymal cells differentiate into osteogenic cells, then osteoblasts (as needed) and secrete bone matrix until surrounded |
|
|
Step 2 : Intramembranous Ossification |
Osteoblasts surrounded by matrix differentiate into osteocytes. Osteocytes within lacunae extend cytoplasmic processes into canaliculi. Extracellular matrix hardens (or calcifies). |
|
|
Step 3 : Intramembranous Ossification |
Trabeculae is formed from calcified matrix; forms spongy tissue. Blood vessels grow into spaces between trabeculae. Mesenchyme condenses at surface. |
|
|
Step 4 : Intramembranous Ossification |
Condensed mesenchyme cells become periosteum. Superficial layers of spongy bone are replaced by compact bone. |
|
|
Step 1 : Endochondral Ossification |
At bone site, mesenchymal cells crowd to form shape of future bone, differentiate into chondroblasts.
REMEMBER! "chondro-" means cartilage "osteo-" means bone |
|
|
Step 2 : Endochondral Ossification |
Chondroblasts secrete cartilage extracellular matrix. INTERSTITIAL (from within - length) and APPOSITIONAL (at surface - width) growth takes place. Matrix beings to ossify, and chondroblasts/chondrocytes begin to die from lack of nutrients. |
|
|
Step 3 : Endochondral Ossification |
Primary ossification center (POC) develops. Nutrient artery penetrates perichondrium, which stimulates cells in perichondrium to differentiate into OSTEOBLASTS instead of chondroblasts. Perichondrium becomes PERIOSTEUM with introduction of bone cells. |
|
|
Step 4 : Endochondral Ossification |
As bone grows outwards of the POC, osteoclasts break down newly made spongy bone to create MEDULLARY CAVITY. |
|
|
Step 5 : Endochondral Ossification |
Epiphyseal artery enters epishyses, creating the secondary ossification center (SOC). Bone formation is similar to that of POC, with the exception of NO medullary cavity. |
|
|
Step 6 : Endochondral Ossification |
Hyaline cartilage covering the epiphyses becomes articular cartilage. Hyaline cartilage between diaphysis and epiphyses remains and becomes the EPIPHYSEAL PLATE, which is responsible for growth (lengthwise) of bones. |
|
|
What are the zones of the EPIPHYSEAL PLATE? |
Zone of resting cartilage Zone of proliferating cartilage Zone of hypertrophic cartilage Zone of calcified cartilage |
|
|
Define the zones of the epiphyseal plate |
Zone of resting cartilage: anchors growth plate to bone Zone of proliferating cartilage: rapid cell division, chondrocytes secrete matrix Zone of hypertrophic cartilage: cells enlarged, remain in columns Zone of calcified cartilage: thin zone, mostly dead cells. Osteoclasts removing matrix, and osteoblasts and capilaries move in, create bone over calcified cartilage. |
|
|
What are the 5 types of bone SHAPES? |
Long Short Flat Irregular Sesamoid
|
|
|
What are the bones of the AXIAL skeleton? |
Skull Hyoid Bone Thoracic Cage (sternum, ribs, thoracic vertebrae, costal cartilage) Spinal Column (includes sacrum and coccyx!) |
|
|
What are the bones of the APPENDICULAR skeleton? |
Shoulder Girdle: scapula and clavicle Upper Limbs Pelvic Girdle: os coxa (ilium, ischium, pubis) Lower Limbs |
|
|
What are the 5 vertebral regions, and how many vertebrae are in each? |
Cervical (7 - C1 is called Atlas, C2 is called Axis) Thoracic (12 - one for each rib!) Lumbar (5) Sacrum (5 fused) Coccyx (4 fused) |
|
|
Define the SPINAL CURVATURES (how many, when formed) |
There are FOUR spinal curvatures: PRIMARY: Thoracic and Sacral (formed as fetus) SECONDARY: Cervical (formed ~ 4 months) and Lumbar (formed ~1 year) |

