![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
37 Cards in this Set
- Front
- Back
|
Functions of the Urinary System |
Excretion (removal of metabolic wastes) Urea: primary nitrogenous end product (also excrete some ammonium, uric acid and creatinine Kidneys maintain homeostasis |
|
|
How does the kidneys maintain homeostasis? |
Preservation of water-salt balance (blood osmolarity) Maintenance of blood pressure and acid-base balance |
|
|
Urinary System (overview) |
Urine produced by pair of kidneys (mostly water) Ureters transport urine from kidneys to bladder When full then released through the urethra |
|
|
Structure of kidneys |
Held in place by connective tissue called renal fascia Bean shaped, reddish brown colour Covered by tough connective tissue called the renal capsule Concave side: has a depression called the hilum- renal artery enters, and a renal artery and ureter exit the kidney |
|
|
Blood supply and pathway of kidneys |
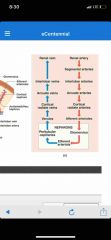
1200 ml of blood flows through the kidney every minute Receives from renal artery then branches off to abdominal aorta |
|
|
Nephrons |
Microscopic structures that are the functional units of the kidneys Millions found in the kidneys |
|
|
Renal Corpuscle |
Formed by the Bowman’s capsule which contains a capillary network (glomerulus) which work together to form the renal corpuscle |
|
|
Renal Corpuscle |
Formed by the Bowman’s capsule which contains a capillary network (glomerulus) which work together to form the renal corpuscle |
|
|
Urine formation: Glomerular Filtration |
Non selective process (cause useful materials get filtered) Materials filtered from blood become the filtrate (inside nephron) |
|
|
Urine formation: Tubular Reabsorption |
Selectively takes back useful materials Might take back unusefull materials Takes materials from the filtrate back into the blood |
|
|
Urine Formation: Tubular Secretion |
Selectively take materials from blood back into the filtrate |
|
|
Renal Corpuscle (filtration) |
Glomerular filtration occurs when whole blood enters the afferent arteriole and the glamerulus Due to the blood pressure only water and small molecules pass by (large molecules and blood cells cant so they continue to travel to the efferent arteriole) FILTERED (goes to Bowman’s capsule): water, nitrogenous wastes, salts, uric acid, creatinine, small molecules NON FILTERED: RBC, WBC, platelets, large plasma proteins |
|
|
Proximal Tubule (Reabsorption) |
Filtrates produced by Bowman’s capsule has many nutrients Reabsorption must happen after through active or passive transport Every substance requires a carrier transport and when all carriers are working at max speed a threshold is reached Blood pH controlled by secretion of H ions and absorption of bicarbonate ions |
|
|
Loop of Henle |
Descending and ascending limb Water is absorbed by osmosis As filtrates move down the descending limb, osmolarity of the filtrates increase Na and Cl absorbed my active transport As filtrates move up ascending limb, the osmolarity of the filtrates decrease |
|
|
Loop of henle |
U shaped, peritubular capillary (vasa recta) minimizes loss of solutes Vasa recta collects salts and water forming the plasma which is transported out of the kidneys back to circulation |
|
|
Distal tubule and collecting duct |
80-85% of water and solutes have been absorbed Final adjustments of urine made here by af |
|
|
Regulating blood pressure (RAAS) |
Aldosterone acts on nephrons to increase Na absorption @ distal tubule and collecting duct Hormone produced in the vortex of the adrenal glands (above kidneys) NaCl Reabsorption increases, osmotic gradient increases and water moves out of nephron back to the blood (by osmosis) |
|
|
Action of Aldosterone |
Carried in the blood to the kidneys where it acts on the cells of the distal tubule and collecting duct to: Increase Na transport Water absorption Blood volume increases Blood pressure increases |
|
|
Regulating blood pressure (RAAS) |
Aldosterone acts on nephrons to increase Na absorption @ distal tubule and collecting duct Hormone produced in the vortex of the adrenal glands (above kidneys) NaCl Reabsorption increases, osmotic gradient increases and water moves out of nephron back to the blood (by osmosis) |
|
|
Action of Aldosterone |
Carried in the blood to the kidneys where it acts on the cells of the distal tubule and collecting duct to: Increase Na transport Water absorption Blood volume increases Blood pressure increases |
|
|
Juxtaglomerular apparatus |
Blood pressure receptors Found near glomerulus Detect low blood pressure |
|
|
Renin |
Specialized cells release this Enzyme that converts angiotensinogen (plasma protein produced by liver) into angiotensin I then into angiotensin II @ the lungs All done by ACE (angiotensin-converting enzyme) |
|
|
Functions of Angiotensin II |
Causes constriction of blood vessels (blood pressure increases when diameter of blood vessel is reduced) Stimulates the release of aldosterone from the adrenal gland Can be interrupted by a drug called ACE inhibitor (controls high blood pressure) |
|
|
Atrial Natriuretic Hormone (ANH) |
Hormone secreted by the Syria of the heart when cells stretch due to increased blood volume Inhibits the secretion of renin by juxtaglomular apparatus and of adolsterone by the adrenal gland To promote the excretion of Na which comes with water which therefore blood volume and pressure decreases |
|
|
Antidiuretic Hormone (ADH) |
Water absorbed at distal tubule and collecting duct is regulated by this Made by hypothalamus in posterior pituitary gland Regulates blood osmolarity by promoting water absorption Is released when person is dehydrated (blood osmolarity increases, hypothalamus shrinks signalling the gland) |
|
|
Regulating blood pressure (RAAS) |
Aldosterone acts on nephrons to increase Na absorption @ distal tubule and collecting duct Hormone produced in the vortex of the adrenal glands (above kidneys) NaCl Reabsorption increases, osmotic gradient increases and water moves out of nephron back to the blood (by osmosis) |
|
|
Alkalosis |
When blood pH is too high |
|
|
Maintaining pH |
Buffer system- removes H ions, must be restored to protect body by the kidneys |
|
|
Action of Aldosterone |
Carried in the blood to the kidneys where it acts on the cells of the distal tubule and collecting duct to: Increase Na transport Water absorption Blood volume increases Blood pressure increases |
|
|
Juxtaglomerular apparatus |
Blood pressure receptors Found near glomerulus Detect low blood pressure |
|
|
Renin |
Specialized cells release this Enzyme that converts angiotensinogen (plasma protein produced by liver) into angiotensin I then into angiotensin II @ the lungs All done by ACE (angiotensin-converting enzyme) |
|
|
Functions of Angiotensin II |
Causes constriction of blood vessels (blood pressure increases when diameter of blood vessel is reduced) Stimulates the release of aldosterone from the adrenal gland Can be interrupted by a drug called ACE inhibitor (controls high blood pressure) |
|
|
Atrial Natriuretic Hormone (ANH) |
Hormone secreted by the Syria of the heart when cells stretch due to increased blood volume Inhibits the secretion of renin by juxtaglomular apparatus and of adolsterone by the adrenal gland To promote the excretion of Na which comes with water which therefore blood volume and pressure decreases |
|
|
Buffers |
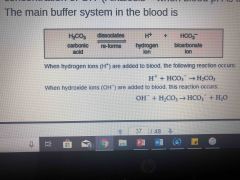
Combo of acid/base that works together to resist small changes in pH Acid- low pH (<7) caused by high concentration of H ions Base- high pH (>7) cause by high concentrations of OH ions |
|
|
Diabetes Insipidus |
Destruction of ADH producing cells of the hypothalamus causes this Without ADH to regulate water absorption, having to urine increases (may become very thirsty) Just drink bare water to replace decrease of Reabsorption |
|
|
Buffers |
Combo of acid/base that works together to resist small changes in pH Acid- low pH (<7) caused by high concentration of H ions Base- high pH (>7) cause by high concentrations of OH ions |
|
|
Acidosis |
When blood pH is too low |

