![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
95 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
How does appendicitis begin in a patient?
|
The accumulation of material, usually feces within the appendix.
|
|
|
|
How does appendicitis develop?
|
Once obstructed pressure builds up decreasing the flow of blood and lymph. This reduces the body's ability to fight infection.
|
|
|
|
Should appendicitis remain untreated what can result?
|
The appendix may eventually rupture causing peritonitis, sepsis and death.
|
|
|
|
What symptoms does the patient with appendicitis present with?
|
Periumbilical visceral pain which eventually migrates to the RLQ.
|
|
|
|
What can suggest possible perforation of the appendix?
|
Rebound tenderness
|
|
|
|
What other signs and symptoms of appendicitis can present?
|
Anorexia, nausea and fever.
|
|
|
|
How should suspected appendicitis be managed in the pre-hospital environment?
|
Remain vigilant for signs of perforation or septic shock. Volume resuscitation may not be sufficient to restore blood pressure.
|
|
|
|
What is Pancreatitis?
|
The pancreatic duct is blocked leading to enzymes becoming activated within the pancreas and breaking down its protein and fat.
|
|
|
|
What is this process called?
|
Autodigestion of the pancreas.
|
|
|
|
What can cause pancreatitis?
|
Alcohol, Gallstones, medication reactions, trauma, cancer and very high triglyceride levels.
|
|
|
|
How does pancreatitis develop?
|
Can occur suddenly or persist over many months. Can be singular or recurrent.
|
|
|
|
What section of the population is pancreatitis more prevalent in?
|
African Canadians aged 35-64 yrs.
|
|
|
|
What is the presentation of a patient with suspected pancreatitis?
|
Pain located in the epigastric area or RUQ. Can be sharp pain and can be severe.
|
|
|
|
Is there any radiation of pain?
|
Radiation of pain to the back is very common.
|
|
|
|
What additions symptoms can present?
|
Nausea, Vomiting, fever, tachycardia, hypotension, and muscle spasms in the extremities due to hypocalcemia. The inflammatory condition as well as erosion of nearby blood vessels can cause hemodynamic instability. Bruising in the flanks and umbilicus indicated reteroperitoneal bleeding.
|
|
|
|
How is pancreatitis managed in the pre-hospital setting?
|
Assess patient for signs of severe hemorrhage or shock. If present begin fluid resuscitation.
|
|
|
|
What is Ulcerative Colitis?
|
Generalized inflammation of the colon.
|
|
|
|
What causes Ulcerative Colitis?
|
Causes are unclear, thought that genetics, stress and autoimmunity contribute to etiology.
|
|
|
|
What are the effects of UC?
|
Inflammation causes thinning of the intestinal wall resulting in weakened dilated colon. The damaged lining is prone to bacterial infection and bleeding.
|
|
|
|
Who is most often affected by the disease.
|
The young, 15-30 yrs. 20% of patients have a family member with the disease.
|
|
|
|
What symptoms to patients present with?
|
Bloody diarrhea (hematochezia) and abdominal pain ranging from mild to severe.
|
|
|
|
What are other symptoms of UC?
|
Can have fever, fatigue, and loss of appetite. Joint pain and Skin lesions.
|
|
|
|
Why can UC present with joint pain and skin lesions?
|
Due to the systemic nature of the autoimmune response thought to be responsible.
|
|
|
|
How is the UC patient managed in the pre-hospital setting?
|
Determine the degree of hemodynamic instability. Look for signs of shock. If diarrhea and bleeding have caused sufficient volume loss to make the patient unstable administer fluids. otherwise provide supportive care.
|
|
|
|
What is Diverticulitis?
|
Pouches in the colon wall where fecal matter can become trapped leading to localized inflammation and infection.
|
|
|
|
How does the disease occur?
|
Low fibre diets producing more solid stools and increased intraaluminal pressures in the colon. Small defects in the colon wall where arteries enter result in bulges which eventually turn into pockets where fecal matter can accumulate.
|
|
|
|
What can occur as a result?
|
Scaring can occur along with adhesions and fistulas.
|
|
|
|
How does the patient with Diverticulitis present?
|
Abdominal pain tends to be localized to the left side of the abdomen.
|
|
|
|
What are the Classic signs?
|
Fever, malaise, body aches, chills, nausea and vomiting. Can be a source of lower GI bleeding often without pain.
|
|
|
|
What can develop as a result?
|
Adhesions, narrowing the diameter of the colon resulting in constipation and bowel obstruction.
|
|
|
|
What in the management for this condition in the pre-hospital setting?
|
Make patient comfortable. Examine closely for severe infection as sepsis can occur. Can develop complications such as fistulas to the bladder. May need fluids to maintain blood pressure.
|
|
|
|
What is Cholecystitis?
|
The obstruction of the cystic duct leading from the gall bladder to the duodenum (usually gallstones).
|
|
|
|
Symptoms?
|
If a blockage patient may experience severe, extreme RUQ pain radiating to right shoulder.
|
|
|
|
Murphy's sign?
|
Ask patient to inhale deeply while pressing on the RUQ near the costal margin. If patient stops inhaling due to pain the sign is positive.
|
|
|
|
Billiary Colic or Cholecystitis?
|
Pain alone suggest billiary colic. Pain with fever, jaundice and tachycardia suggests cholecystitis.
|
|
|
|
How does the patient present?
|
Patients with billiary colic typically develop severe RUQ pain after eating large or fatty meals. The development of fever and tachycardia is suggestive of inflammation of the gall bladder wall occuring with cholecystitis.
|
|
|
|
How is cholecystitis managed?
|
Make patient comfortable and treat hypovolemia if a fever and any indications of septic shock.
|
|
|
|
What are Esophageal Varices?
|
Bleeding in the distal esophagus due to increased venous pressures. Usually as a result of liver damage or cirrhosis.
|
|
|
|
Liver Damage?
|
Chronic alcohol consumption damages and scars the interior of the liver leading to slower blood flow and higher venous pressures. The higher pressure causes and increased risk of bleeding.
|
|
|
|
How does the patient with EV present?
|
Initially asymptomatic. Patient may show other subtle signs of liver disease, fatigue, weight loss, jaundice, anorexia, edema in abdomen and puritis.
|
|
|
|
How does EV develop?
|
Once there is a variceal bleed presentation is dramatic. The patient may complain of discomfort in the throat. Often copious vomiting of bright red blood, hypotension and signs of shock.
|
|
|
|
What if bleeding is less severe?
|
Hematemesis and melena predominate.
|
|
|
|
How is EV managed in the pre-hospital enviroment?
|
Assess blood loss as acurately as possible. Volume resuscitation and agressive suctioning. May need airway support.
|
|
|
|
What is Acute Hepatitis?
|
The result of damage to the liver by one of several viruses. Usually in Canada this is A, B or C.
|
|
|
|
What routes are these aquired?
|
Hep A is usually fecal-oral. B and C are person to person contact (sexual or blood).
|
|
|
|
How can Hepatitis develop?
|
Can range from 14-180 days with acute hepatitis.
|
|
|
|
What are signs and symptons of hepatitis?
|
Acute H can cause abdominal pain, vomiting, fever and jaundice. Chronic infection or complications of acute infections can lead to cirrhosis.
|
|
|
|
What are 1st phase signs and symptoms?
|
Suggest mild viral illness. Joint pain, weakness, fatigue, fever, nausea, abdominal pain (often mild) vomiting and anorexia.
|
|
|
|
What are Late phase symptoms?
|
Can be days to years after the initial infection. Acholic stools, darkening or urine and sclerae of jaundice. Abdominal pain is RUQ and enlarged liver becomes apparent. Total liver failure may be days away.
|
|
|
|
How is this managed in the pre-hosptal setting?
|
Supportive care, infection control, BSI precautions. Hep B can remain infectious in the blood for up to a week.
|
|
|
|
What is Mallory-Weiss Syndrome?
|
Where the esophageal lining tears during severe vomiting.
|
|
|
|
What can happen in extreme cases?
|
A frank rupture of the esophagus can rarely occur leading to spillage of gastric contents into the mediastinum. This can result in Pneumothorax and overwhelming sepsis.
|
|
|
|
Who does this affect?
|
Men and Women equally but more in older adults and older children.
|
|
|
|
How does Mallory-Weiss Syndrome develop?
|
Repeated severe vomiting. In women this can be with hyperemesis gravidarum.
|
|
|
|
How can bleeding vary?
|
From very minor with little blood loss to severe bleeding and extreme hypovolemia.
|
|
|
|
What are symptoms in extreme cases?
|
Signs of shock, epigastric abdominal pain, hematemesis and melena.
|
|
|
|
How is Mallory-Weiss Syndrome managed in the pre-hospital environment?
|
Determine the extent of blood loss, may need fluid resuscitation and suctioning. Support airway as required.
|
|
|
|
What are symptoms in extreme cases?
|
Signs of shock, epigastric abdominal pain, hematemesis and melena.
|
|
|
|
How is Mallory-Weiss managed in the pre-hospital environment?
|
Determine the extent of blood loss. May need fluid resuscitation. Suction as needed along with airway support if required.
|
|
|

What is this?
|
Melena (Blood in stool)
|
|
|
|
What are hemorrhoids?
|
Caused by swelling and inflammation of the blood vessels surounding the rectum.
|
|
|
|
What causes hemorrhoids?
|
Can result from conditions that increase pressure on the rectum or irritation of rectum. Pregnancy, straining at stool and chronic constipation cause increased pressure. Anal intercourse and diarrhea cause irritation.
|
|
|
|
How do hemorrhoids present?
|
Bright red rectal bleeding. The hematochezia tends to be minimal and easily controlled. Blood loss can appear dramatic to the patient.
|
|
|
|
What symptoms can the patient experience?
|
Pain, itching and a small mass on the rectum. Typically the mass is a clot formed in response to the mild bleeding.
|
|
|
|
How are hemorrhoids managed in the pre-hospital environment?
|
Largely supportive. In isolation they are more an inconvenience than a life threatening condition.
|
|
|
|
What can happen in rare cases?
|
Can result rarely in severe GI bleeding. Hemorroidal source may not be apparant. Ensure patient is hemodynamically stable with fluid resuscitation if necessary.
|
|
|
|
What is Acute Gastroenteritis?
|
A family of infectious conditions presenting with nausea, vomiting and diarrhea.
|
|
|
|
What causes Acute Gastroenteritis?
|
Bacterial, viral and parasitic organisms typically entering the body through contaminated food, water or via fecal oral contact with ill patients.
|
|
|
|
What can some organisms do?
|
Secrete toxins destroying the mucosa leading to bloody diarrhea.
|
|
|
|
Who are more at risk of AG?
|
Immune compromised patients.
|
|
|
|
How does AG present?
|
Vomiting and diarrhea. Some organisms cause inflammation of the intestines resulting in blood, mucous or pus in the stool.
|
|
|
|
What are the symptoms?
|
Abdominal cramping is frequent. Nausea and anorexia are often present.
|
|
|
|
What can happen if the vomiting and diarrhea continue?
|
Dehydration and hemodynamic instability will result. As volume of fluid lost increases there is greater chance of sodium and pottasium imbalance.
|
|
|
|
What should you look for?
|
Changes in heart rate, blood pressure, LOC and other signs of shock.
|
|
|
|
How is AG managed in the pre-hospital environment?
|
Determine the degree of fluid deficit, determine the need for fluid resuscitation from vitals.
|
|
|
|
What is Crohns Disease?
|
Similar to Ulcerative Colitis but may affect the entire GI tract. The immune system attacks the GI tract and the activity of white blood cells damages all layers of the GI tract involved.
|
|
|
|
Where is the most likely site of this attack and what is the result?
|
The most likely site is the ileum and the result is a scarred narrowed, stiff and weakened portion of bowel.
|
|
|
|
What age are most patients?
|
20-30 years.
|
|
|
|
How do patients present?
|
Recurrent flares of abdominal pain. rectal bleeding, weight loss, diarrhea, arthritis and fever.
|
|
|
|
Describe typical bleeding?
|
Tends to be small amounts over long period of time acute severe bleeding is rare but chronic bleeding resulting in anemia can occur. Patients may experience repeated episodes of mild to severe signs and symptoms.
|
|
|
|
What is the management for Crohns in the pre-hospital setting?
|
Volume resuscitation may be required due to diarrhea and chronic hemorrhage.
|
|
|
|
What is Peptic Ulcer Disease?
|
The protective layer in the stomach is eroded and stomach acid is allowed to eat into the mucosal lining of the stomach.
|
|
|
|
What are the etiologies of PUD?
|
Many, Heliobacter Pylori infection, Use of NSAID's.
|
|
|
|
What can exacerbate PUD?
|
Alcohol and Tabacco.
|
|
|
|
What section of the population does PUD occur in more frequently?
|
Older adults due to increased prevalence of H pylori and use of NSAID's.
|
|
|
|
How do patients with PUD present?
|
Burning or gnawing pain in the abdomen subsiding after eating and re-emerging 2-3 hours later. Nausea, vomiting, belching and heartburn are common as well.
|
|
|
|
What if the erosion is severe?
|
Gastric bleeding can occur resulting in hematemesis and melena. Any perforation of the stomach or intestine will result in signs of peritoniotis.
|
|
|
|
What is the management for PUD in the pre-hospital setting?
|
Assess the extent of blood loss and manage any hypotension present. Orthostatic vital signs critical.
|
|
|

What is this condition?
|
Jaundice
|
|
|

What is this?
|
Melena.
|
|
|
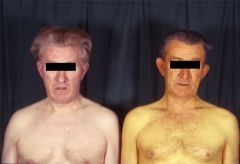
What is this?
|
Jaundice.
|
|
|
|
What are the signs of Hyponatremia (low sodium)?
|
Muscle weakness, cramping, coma, convulsions.
|
Causes the swelling of cells!
|
|
|
What are the signs of Hypernatremia (low sodium)?
|
Coma, convulsions.
|
Shrinking of cells due to excessive water loss
|
|
|
What are the signs of Hypokalemia (low potassium)?
|
Muscle cramps, weakness, paralysis, heart failure, dysrhythmia
|
More stimulation needed to fire nerve/muscle cells.
|
|
|
What are the signs of Hyperkalemia (high potassium)?
|
Muscle weakness and cramps, bradycardia, asystole
|
Less stimulation need to fire nerve/muscle cells
|

