![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
88 Cards in this Set
- Front
- Back
|
Life spam of an erythrocyte?
|
120 days
|
|
|
4 functions of erythrocytes?
|
1. Gas Exchange
2. Acid-base balance 3. Clear immune complexus 4. clear nitric oxide |
|
|
2 problems with methemoglobin?
|
1. not functional
2. can be damaging |
|
|
what serves as a protective mechanism for oxidative damage in erythrocytes?
|
glutathione
|
|
|
How many oxygen molecules can 1 hemoglobin chain carry?
|
4
|
|
|
Most common componets of adult hemoglobin?
|
2 alphas and 2 betas
|
|
|
A high A2 count can be diagnostic of?
|
Thalassemias
|
|
|
Max value of A2?
|
7-8%
|
|
|
How man aloha genes do we have? beta? gamma?
|
4 Alpha
2 Beta 4 gamma |
|
|
P50?
|
Partial pressure at which hemoglobin is 50% saturated with oxygen
|
|
|
Amount of oxygen usually unloaded at the tissue?
|
20-25%
|
|
|
Normal P50?
|
26 mm Hg
|
|
|
Higher affinity causes the O2 curve to shift which direction?
|
Left
|
|
|
Function of 2,3 DPG?
|
stabilizes the deoxy form of hemoglobin and thus decreases the affinity for oxygen
|
|
|
One signal that increases the synthesis of 2,3 DPG?
|
high deoxy hemoglobin
|
|
|
3 factors that will decrease o2 affinity?
|
1. 2,3 DPG
2. Acidosis 3. High tempurature |
|
|
Bohr effect?
|
acidosis is associated with stress, shock ect which signals a need for more O2 and decreases it's affinity for hemoglobin.
|
|
|
Iron is usually in which state?
|
Fe2+
|
|
|
Heme synthesis requires what as a cofactor?
|
B6
|
|
|
Rate limiting step in heme sythesis?
|
ALA synthase
|
|
|
the gene for RBC ALA synthetase is located?
|
X chromoasome
|
|
|
Iron is found in which state in methemoglobin?
|
FE3+
|
|
|
How does methemoglobin damage RBCs?
|
They tend to degrade and cause oxidative damage to the cell leading to premature distruction
|
|
|
What are the steps to methemoglobin's conversion to hemoglobin?
|
1. methemoglobin is converted to hemoglobin by methemoglobin reductase using NADH and producing superoxide
2. The superoxide is converted to hydrogen peroxide by superoxide dismutase 3. Hydrogen peroxide is reduced by glutathione 4. Glutathion is reduced back by glutathione reductase suing NADPH |
|
|
How does a RBC generate energy?
|
Glycolysis
|
|
|
How does the RBC generate NADPH?
|
Hexose monophosphate shunt
|
|
|
First enzyme in hexose monophosphate shunt?
|
glucose-6-phosphate dehygrogenase
|
|
|
G6PD gene is located?
|
X chromosome
|
|
|
How is 2,3 DPG generated?
|
Glycolysis
|
|
|
Where are RBC cells destroyed?
|
reticuloendothelial system 90% in the spleen and 10% in circulation
|
|
|
Where do the parts of RBC end up after degredation?
|
Iron goes back to the liver
Heme-biliverdin-bilirubin-congugated bilirubin whe is either eabsorbed or secreted |
|
|
Haproglobin?
|
complexes with alph and beta dimers in circulation
|
|
|
Reticulocyte?
|
immature RBC that still contains RNA
|
|
|
Normal Reticulocte count?
|
.5-2.5%
|
|
|
Normal hematocrite for men? women?
|
45% and 40%
|
|
|
What is used to gauge size in RBCs?
|
Nucleous of a lymphocyte
|
|
|
Normal RBC count?
|
4.7-6.1 in men
4.2-5.4 in women |
|
|
Normal Hemoglobin?
|
14-18 in men
12-16 in women |
|
|
Normal Heatocrit?
|
42-52 in Men
37-47 in Women |
|
|
Normal MCV?
|
80-94 in Men
81-99 in Women |
|
|
Why do men have higher hemoglobin?
|
Testosterone stimulates RBC production
|
|
|
Appearance of neutrophils under microscope?
|
Nucleous is segmented or banded. small weakly stained granules
|
|
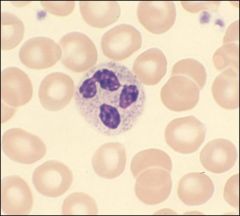
What is this?
|
Nutrophile
|
|
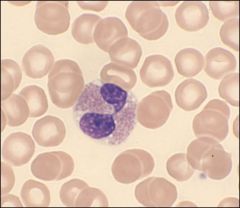
What is this?
|
eosinophile
|
|
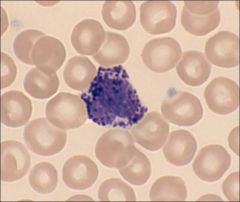
What is this?
|
Basophile
|
|
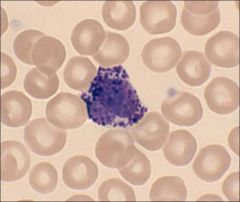
What is this?
Function? |
Large granular lymphocyte
natural killer function |
|
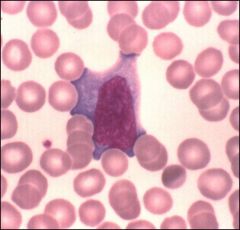
What is this?
When do you see them? |
Reactive atypical lymphocyte
characteristic of infectious monomucleosis. |
|
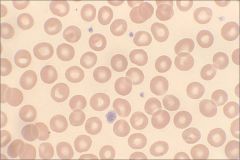
What are these?
|
Platets
|
|
|
Normal platlet count?
|
140-440
|
|
|
How many are necessary for clotting?
For surgery? At risk for spontaneous hemorrhage? |
20,000
50,000-100,000 under 10,000 |
|
|
Normal MCV range?
|
80-100
|
|
|
Normal WBC count?
|
4-11
|
|
|
Normal Hgb count?
|
13-18 in men
15-16 in Women |
|
|
Normal Hct count?
|
39-52 in men
34-46 in women |
|
|
how are stem cell identified?
|
Growth on a plate
|
|
|
stem cell differentiate into 2 different types of progenitor cells?
|
common myloid progenitor (CMP)
common lymphoid progenitor (CLP) |
|
|
Hematopoieses occures where?
1st trimester? 2nd trimester? 3rd Trimester? Post natal? |
Yolk sac and aorta=gonaldal-mesoderm (AGM)
Liver and some spleen Bone marrow becomes dominant Only bone marrow |
|
|
Where does hematopoisis occure in adults?
|
Axial skeliton and proximal bones
|
|
|
Red vs Yellow marrow?
|
Red = hematopoisis
Yellow is mostly fat but can become red if there is need |
|
|
Most hematopoisis recptors are what kind?
|
Tyrosine kinases, Jak Stat
|
|
|
Erythropoietin is produced where?
|
Kidneys and a little liver
|
|
|
Thrombopoietine is produced where?
|
Liver and a little spleen
|
|
|
4 clinicaly available stimulating factors?
|
G-CSF
GM-CSF Erythropoitin Thrombopoitin |
|
|
G-CSF? Where is it produced? stimulates? Uses?
|
Produced in bone marrow
Stimulates production of granulocytes Is used for granulocytopenia and transplantation |
|
|
GM-CSF. Where is it produced? Stimulates? Uses?
|
Priduced in bone marrow
Stimulates production of granulocytes and monocytes Used for granulocytopenia and transplantation. |
|
|
Erythropoietin? Stimulates? used for?
|
Stimulates RBC production
Used for Anemia |
|
|
Thrombopoietin? Stimulates? uses?
|
Stimulates megakaryocyte differentiation and platlet production
Used for thrombocytopenia and transplantation |
|
|
Neupogen and Neulasta?
|
G-CSF
|
|
|
Romiplostim (Nplate) and Eltrombopag (Promacta)?
|
Thrombopoietin mimetics
|
|
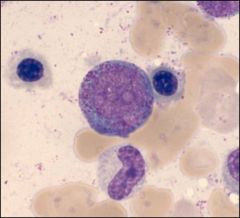
What is this?
Defining characteristics? |
Promyelocyte
Presence of primary granules, nucleus is large and uncondenced, presence of nucleolus |
|
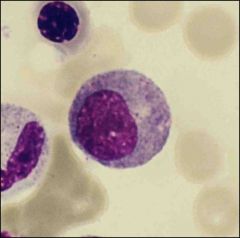
What is this?
Defining charactersitics? |
Neutrophilic myelocyte
Secondary granules, nucleous is still round, chromatin condensation, nucleolus is gone |
|
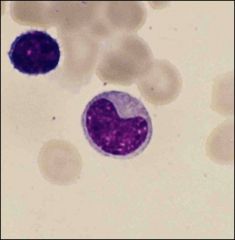
what is this?
Defining characteristics? |
Metamyelocyte
Necleus becomes bean shaped, chromatin more condensed |
|
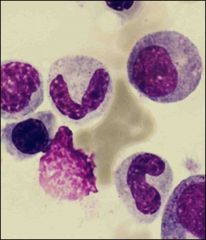
What is this?
charactersitics? |
Band neutrophile
hourse shoe shaped nucleous |
|
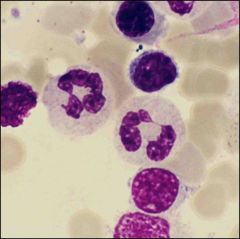
What is this?
Characteristics? |
neutrophile
segmented nucleous |
|
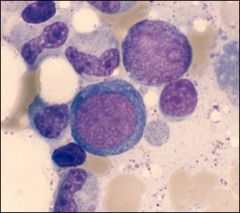
What is this?
characteristics? |
Proerythroblast
large round nucleus with fine chromatin. nucleolus is present and deeply basophilic cytoplasm |
|
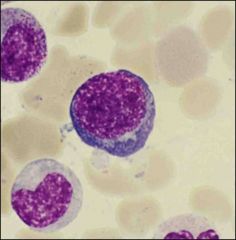
What is this?
characteristics? |
Basophilic erythroblast
deeply basophilic cytoplasm, nuclear chromatic starts to condence, nucleolus is lost |
|
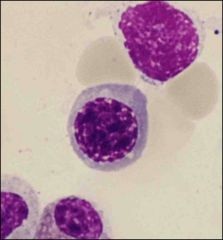
What is this?
characteristics? |
Polychromatophilic erythroblast
Hemoglobinization begins and cytoplasm becomes grey to orange as chromatic condenses more |
|
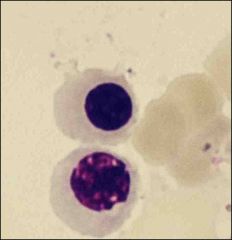
What is this?
characteristics? |
Orthochromic erythroblast
normal color, fully hemoglobinized, nucleus is totally condenced |
|
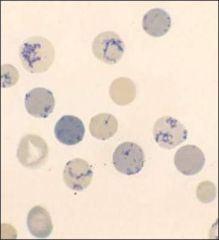
What are these?
|
Reticulocytes
|
|
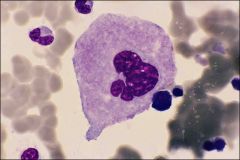
What is this?
|
Megakaryocyte
|
|
|
schitocytes suggest?
|
mechanical or intravascular trauma
|
|
|
Paroxysmal nocturnal hemoglobinuria is caused by?
|
loss of complement fixation protection
|
|
|
PNH is inhereted how?
|
X linked
|
|
|
3 major symptoms of PNH?
|
intravascular hemolysis
thrombhillis bone marrow failure |
|
|
What gene is lost in PNH?
|
glycosylphosophatidylinositol (GPI) anchored protiens
|
|
|
Why do you get smoth muscle symptoms in PNH?
|
free hemoglobin scavenges for nitric oxide
|
|
|
How do you diagnose PNH?
|
Flow cell
|
|
|
Some treatments for PNH?
|
transfusion, iron and follate supplimentation, anticoagulation and Eculizumab
|

