![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
37 Cards in this Set
- Front
- Back
|
What is the causative agent of Leprosy?
|
Mycobacterium leprae, acid-fast bacillus
|
|
|
How is Mycobacterium leprae transmitted?
|
respiratory droplets
|
|
|
What is the transmission pathway for leprosy?
|
Respiratory droplets from an infected person get inhaled by uninfected person. alveolar macrophages phagocytose Mycobacterium leprae and disseminate in the bloodstream.
|
|
|
What temperature does Mycobacterium leprae prefer to grow in and how does that reflect the cell type in which it grows?
|
cooler temperatures
skin cells and peripheral nerves |
|
|
What is the difference between tuberculoid leprosy and lepromatous leprosy?
|
tuberculoid leprosy (paucibacillary) is the milder form of leprosy resulting from a strong cellular response. bacteria are not found in the tuberculoid leprosy-like lesions.
lepromatous leprosy (multibacillary) results from a trivial immune response and it shows up as a much more striking destruction of peripheral tissue. |
|
|
How long does it take for Mycobacterium leprae to show symptoms of infection?
|
can take years
|
|
|
What is the causative agent of Anthrax?
|
Bacillus anthracis, Gram(+), endospore-forming bacillus
|
|
|
What two ways can anthrax be transferred?
|
breathe in spores
spores get into skin lesions |
|
|
What is the transmission pathway for anthrax?
|
spores are inhaled
alveolar macrpohages engulf anthrax is moved to lymph nodes spores germinate and replicate bacteremia |
|
|
What are the two stages of anthrax infection?
|
first stage: fever, shortness of breath, cough, headache, vomiting, chills, chest/abdominal pain
second stage: worsening fever, edema, massively enlarged mediastinal lymph nodes, meningitis |
|
|
If untreated what is the mortality rate for anthrax infection?
|
95% within three days of symptoms
|
|
|
What is the difference between acute and chronic sinusitis?
|
acute = < 12 wks
chronic = < 12 wks |
|
|
What organisms cause acute sinusitis?
|
Streptococcus pneumoniae, nonencapsulated Haemophilus influenzae and Moraxella catarrhalis
which all happen to be causative agents of typical pneumonia |
|
|
What organisms cause chronic sinusitis?
|
Staphylococcus aureus, coagulase-negative Staphylococcus, anaerobic bacteria and gram-negative bacteria are commonly isolated from the sinuses of patients with chronic sinusitis. The bacteria which cause chronic sinusitis are normal inhabitants of skin, anterior nares or oral cavity.
|
|
|
What are complications of sinusitis?
|
otitis media
osteomyelitis orbital problems brain abscesses bacteremia induced organ seeding |
|
|
What is the antibiotic of choice for sinusitis?
|
Amoxicillin/clavulanate = Augmentin
|
|
|
What are the 4 concerning issues with infections from normal oral flora?
|
1) actinomycosis
2) meningococcal disease 3) aspiration pneumonia 4) abscesses |
|
|
What is the causative agent for Actinomycosis?
|
Actinomyces israelii and other microbes, so polymicrobial
|
|
|
What is the most common form of actinomycosis?
|
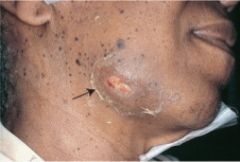
cervicofacial that involves a swelling of the soft tissue at the angle of the jaw
(pic) |
|
|
What is the cause of cervicofacial actinomycosis?
|
oral surgery
poor dental hygiene |
|
|
What causes thoracic actinomycosis?
|
oropharyngeal secretions are aspirated into the lungs.
these can form abscesses that drain through the chest wall |
|
|
What is the causative agent of meningococcal disease?
|
Neisseria meningitidis
|
|
|
How is meningococcal disease spread?
|
a non-resident strain of Neisseria meningitidis is transferred between people by respiratory droplets
|
|
|
What is it called when meningococcal disease is spread to the blood?
|
septiciemia called meningococcemia which can lead to meningitis
|
|
|
How does meningococcemia present clinically?
|
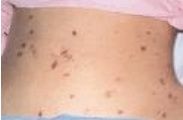
petechiae (rash all over body), upper respiratory tract infection before the onset of fever, chill, headache, nausea, vomiting
|
|
|
What is fulminant meningococcemia?
|
Full on, bad news bears meningococcemia. pts suffer high fever, shock, petechiae coalesce into large lesions and disseminated intravascular coagulation occurs.
|
|
|
What is the mortality rate for fulminant meningococcemia even in spite of proper antibiotic tx?
|
50%
|
|
|
What is aspiration pneumonia?
|
aspirating gastric secretions into the lungs as well as oropharynx normal flora
|
|
|
What are the two conditions that can increase risk for aspiration pneumonia?
|
periodontal disease and conditions that alter consciousness (alcoholism, seizures, anesthesia)
|
|
|
What normal flora are involved with aspiration pneumonia?
|
Bacteroides, Fusobacterium and Peptostreptococcus which are all normal oral flora
|
|
|
What other bacteria are present besides the normal flora that will be found in aspiration pneumonia?
|
Staphylococcus aureus and Escherichia coli
|
|
|
What is the most common abscess of the head and neck?
|
peritonsillar
|
|
|
What are symptoms common to peritonsillar abscesses?
|
sore throat that is resistant to antibiotics, fever, drooling, ear pain
|
|
|
What bacteria are common with peritonsillar abscesses?
|
polymicrobial and including Staphylococcus aureus, Streptococcus pyogenes, Prevotella, Porphyromonas and Bacteroides.
|
|
|
What is special about antibiotic treatment regarding abscesses?
|
antibiotics must be supplemented with surgical draining
|
|
|
What are the three bacteria that cause complications of cystic fibrosis in the end stage lung disease?
|
Pseudomonas aeruginosa, Burkholderia cepacia (formerly Pseudomonas cepacia),
and Staphylococcus aureus. |
|
|
How do you treat cystic fibrosis complicated with bacteria infected end-stage lung disease?
|
biofilm and antibiotic resistance prevents effective treatment
|

