![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
74 Cards in this Set
- Front
- Back
|
metabolic bone disease
- aka - caused by |
Osteodystrophy
Nutritional or hormonal imbalances |
|
|
Metabolic bone disease
4 main types |
Osteoporosis (osteopenia)
Fibrous osteodystrophy Rickets Osteomalacia |
|
|
Hormones affecting bone growth
|
Corticosteroids
GH & IGF-I Thryoid hormone Sex steroids |
|
|
Increased corticosteroids
- affect on bone |
Osteoporosis dt decr rate of bone formation
|
|
|
Decreased GH & IGF-I
- affect on bone |
Proportional dwarfism
- progenitor cell differentiation - chondrocyte proliferation |
|
|
Hyopothyroidism
- affect on bone |
Neonatal mortality
Postnatal exposure: retarded growth |
|
|
Hyperthyroidism
- affect on bone |
Osteoporosis prob dt negative metabolic balance
|
|
|
Sex steroids
- affect on bone |
Osteoblasts have both estrogen & progesterone receptors
Hypoestrogenism > osteoporosis (menopause) |
|
|
Define osteoporosis & osteopenia
|
Osteopenia: reduced mass of normal quality bone tissue (can be clinically silent)
Osteoporosis: reduced mass of normal bone quality OF CLINICAL SEVERITY |
|
|
5 general causes of osteoporosis
|
1. Starvation - protein/calorie malnutrition
2. Gastrointestinal parasitism 3. Specific deficiency 4. Disuse atrophy 5. Endocrine associated osteoporosis |
|
|
4 specific deficiencies that can lead to osteoporosis
|
- calcium
- phosphorus - copper - vitamin C |
|
|
Osteoporosis from most causes is due to impaired deposition of bone
- except for which two causes? |
Disuse atrophy and calcium deficiency lead to ACCELERATED RESORPTION of bone and thus osteoporosis
|
|
|
Histology of osteoporotic bone
- what feature indicates whether dt increased resorption or decreased production of bone? |
Less trabeculae if increased resorption
Normal no. of thin trabeculae if decreased production |
|
|
2 main consequences of osteoporosis
|
Pathological fractures & epiphyseal separation
Hypocalcaemic crises - weaned lambs - lactating ewes |
|
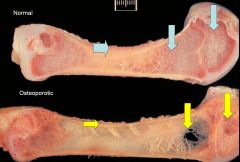
What are you seeing
|
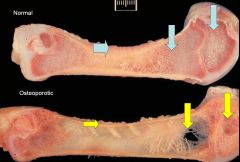
Osteoporotic bone with thinned and porous cortices
|
|
|
What might you see in an osteopenic bone during starvation or specific mineral deficiencies?
|
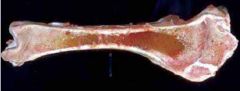
Serous atrophy of marrow
Metaphyseal growth arrest lines Widely spaced trabeculae |
|
|
Why, in some circumstances, doesn't osteoporotic bone return to normal when nutrients balance resumes?
|
Trabeculae surfaces are required for the formation of new bone by apposition
|
|
|
What are common sites of epiphyseal separation (4)
|
Femoral head
Humeral head Ischial tuberosity Vertebrae |
|
|
How does copper deficiency lead to osteoporosis?
|
Copper is required for adequate production of matrix collagen
|
|
|
What causes fibrous osteodystrophy
|
Prolonged and excessive exposure to PTH
|
|
|
What is the aetiology of fibrous osteodystrophy
|
Prolonged & excessive PTH ->
Increased osteoclastic resorption (>porosity), AND Proliferation of osteoprogenitor cells to produce excess fibrous and fibro-osseus tissue |
|
|
List the 4 sources of increased PTH secretion
|
Tumours of the PTH gland (rare)
Paraneoplastic secretion of PTH-like hormone by malignancies (lymphoma, anal gland tumour) Secondary nutritional hyperparathyroidism Secondary renal hyperparathyroidism |
|
|
How can secondary nutritional hyperparathyroidism occur?
|
Occurs in response to relative Ca deficiencies (ratio Ca:P = 1:1)
- diet low in Ca, high in P (ratio imbalance) - bran is high in P (horses) - carnivores on offal (high P) |
|
|
How does secondary renal hyperparathyroidism occur?
|
Renal failure leads to
- failure to excrete P (thus depression of Ca) - reduced synthesis of active VitD |
|

This horse was fed a diet in bran. What is this disease and cause?
|

Nutritional fibrous osteodystrophy ("Bighead" or "bran disease")
Bran high in P, Ca:P imbalance, PTH oversecretion, increased deposition of fibrous material in bone |
|
|
Some tropical grasses can lead to fibrous osteodystrophy. How?
|
High in oxalates which band Ca++ in the gut and prevent absorption leading to hyperparathyroidism
|
|
|
Osteomalacia
|
Softening of bone (can be cut with a knife) dt deficiency of phosphrous or of vitamin D -> failure of bone matrix to mineralise
|
|
|
Rickets
|
Deficiency of phosphrous or of vitamin D -> failure of cartilage AND bone matrix to mineralise
|
|
|
How are osteomalacia and rickets similar and different
|
Both are dt vit D or P deficiency
- Osteomalacia: bone affected - Rickets: cartilage AND bone fail to mineralise Osteomalacia is aka adult rickets |
|
|
What are the two main causes of osteomalacia in cattle & sheep?
|
VitD deficiency in pastured animals where winter sun is low on the horizon (sheep more susceptible)
Phosphorous deficiency dt grazing deficient pastures (uncommon: cattle more susceptible) |
|
|
List 4 sequential changes in rickets
|
1. Failure of mineralisation & vascular invasion of the hypertropic zone
2. Failure of replacement of the growing cartilage with woven bone 3. Formation of osteoid (not bone) on persistent cartilage with irregular osteochondral junctions 4. Metaphyseal compression fractures with fibrosis & deformities of the shape & structure of bone |
|
|
What is the simplest and earliest anatomic manifestation of rickets
|
Widening of the physis
|
|
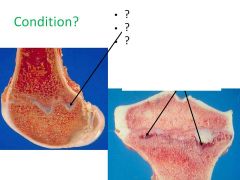
What condition is this most likely to be? What processes can be seen?
|
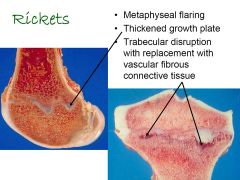
|
|

What's this? Why?
|

Rachitic rosary
Enlarged joints at the costo-chondral junctions. |
|
|
What are the causes of rickets in calves, sheep, pigs, puppies & kittens and Alpaca crias?
|
Calves: P-deficient pastures, sunlight deficiency
Young sheep: sunlight deficiency, green feed low in VitD Pigs: sunlight deficiency, VitD deficiency (feed errors), insufficient activation of VitD in kidney Puppies & kittens: same as pigs Crias: common bouts of severe GI disease -> electrolyte loss (Ca & P) |
|
|
What is florid rickets?
What is it commonly seen in pigs? |
"Florid" = quick, flamboyant
Occurs in pigs as they are frequently weaned early and the grow rapidly |
|
|
What animal species is mostly affected by osteomalacia?
|
?
|
|
|
What is scurvy?
|
Vitamin C deficiency in animals requiring an exogenous source (guinea pigs, primates)
|
|
|
What is the aetiology of scurvy?
|
Vit C required for collagen formation
Thus failure of osteoid formation Cartilage calcification is unaffected leading to a distinctive line of calcified cartilage spicules without newly formed osteoid "SCORBUTIC LATTICE" |
|
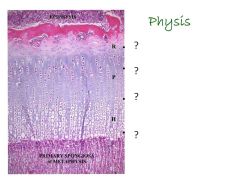
Review physis biology
|
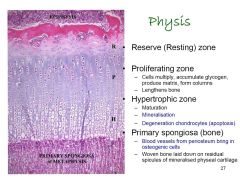
|
|
|
Causes of toxic osteodystrophies (3)
|
Fluorosis
VitD toxicity VitA toxicity |
|
|
Fluorosis
- how? - who's affected? - What's affected? - CS? |
Chronic exposure to excess fluoride leading to lack of mineralisation of teeth and bones
Herbivores Teeth (toxic to odontoblasts) & bones (toxic to osteoblasts) Teeth: mottling enamel, rapid wear, chipping Bones: compensatory periosteal bone formation -> shifting lameness. Also spontaneous fractures |
|
|
VitD toxicity
- 3 sources - increased by? |
Dietary supplementation
Plants Rodenticides VitD toxicity increased with high dietary levels of calcium |
|
|
VitD toxicity
- acute responses |
Hypercalcaemia & hyperphosphatemia (dt incr osteoclast activity initially)
Metastatic mineralisation of soft tissue Renal failure |
|
|
VitD toxicity
- chronic responses |
Early: incr. osteoclast activity -> removal of primary spongiosa
Then: incr. osteoblast activity and incr mineralisation -> osteosclerosis ("hardening") |
|
|
VitA
- role in bone |
Stimulate osteoclast activity
|
|
|
VitA deficiency
- causes in LA & SA |
Cattle, pigs: unsupplemented rations or old hay
Carnivores: lean meat (no liver) |
|
|
VitA deficiency
- main effects |
Defective remodelling of membranous bone in skull & spine -> cerebellar herniation into foramen magnum
Also blindness, deafness, CNS signs |
|
|
VitA toxicity
- how? |
Esp cats fed almost exclusive diet of raw liver
|
|
|
VitA toxicity
- effect on growing animals & adults |
Growing animals:
- degeneration & necrosis of chondrocytes & osteoblasts - premature closure of growth plates, deformity, OSTEOPOROSIS Adults - paradoxical stimulation of osteoblasts -> OSTEOSCLEROSIS, periosteal bone formation, exostoses, spondylosis |
|

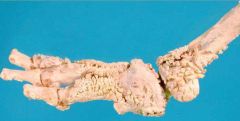
Fused cervical vertebrae, cat: Name and likely cause
|
Deforming cervical spondylosis: VitA toxicity
|
|
|
From here on, have given a definition of each term.
|
May expand later
|
|
|
Osteonecrosis
- 6 causes - 1 potential consequence of importance |
1. Inflammatory diseases
2. Infiltration neoplasma 3. Peripheral vasoconstriction 4. Emboli (gas or fat) 5. Impaired lipid metabolism Bone infarction can lead to OSTEOSARCOMA |
|
|
Aseptic necrosis of bone
- aka ? -cause? |
Osteonecrosis
- bone death dt ischaemia (infarction) |
|
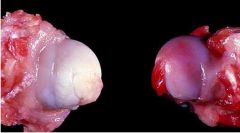
Legg-Calve-Perthes disease
Which is the affected side? |
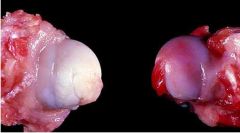
Left (avascular)
|
|
|
Legg-Calve-Perthe disease
- what is it? - who's most affected |
Avascular necrosis of the femoral head
Poodles, Westies, Yorkies |
|
|
Canine hypertrophic osteodystrophy (HOD)
- aka - what is it? - who's affected? |
Metaphyseal Osteopathy
Initial lesion - neutrophilic osteomyelitis of metaphysis Young, fast-growing large breeds Most resolve spontaneously |
|
|
Consequence of metaphyseal osteopathy?
|
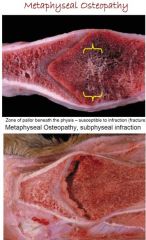
Subphyseal infraction
|
|
|
Craniomandibular osteopathy
- aka - who? - what? |
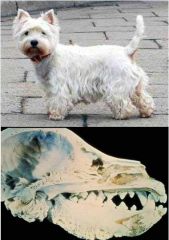
Lion jaw
- terriers (4-7mo) - endosteal & periosteal proliferation of woven bone in mandible, occipital & temporal bones |
|
|
Canine panosteitis
- who? - what? - effect? |
Young, fast growing, large breed dogs (esp male GSD)
Inflammatory process, unknown cause Waxes 7 wanes -> mild-severe lameness |
|
|
Marie's disease
- aka - commonly associated with? - effects? why? |
Hypertrophic osteopathy
Commonly assoc with a space occupying lesion of thorax (lung or chest wall) esp Spirocerca in dogs Primarily a vascular disease leading to deposition of periosteal bone |
|
|
Osteochondritis dissecans
- who? - aetiology |
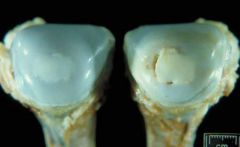
Young, fast growing animals
Multifactorial (genetic, trauma, nutrition, excess dietary ca, cu def, hormones) but underlying pathogenesis is ISCHAEMIC DAMAGE TO GROWING CARTILAGE |
|
|
Main histological features of osteochondrosis
|
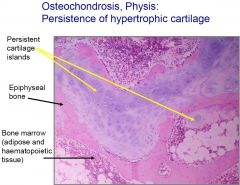
Persistence of hypertrophic cartilage at physis
|
|
|
Name different types of bone tumours
|
Osteoma
Ossifying fibroma Osteosarcoma Fibroblastic osteosarcoma Giant cell osteosarcoma Chondroma Osteochondroma Chondrosarcoma Fibrosarcoma Haemangiosarcoma Plasma cell myeloma Lymphosarcoma Enzootic bovine leukosis |
|
|
What cells type can lead to primary neoplasms of bone
|
Bone
Cartilage Fibrous Adipose Vascular Myeloid cell lineages Lymphoid cell lineages |
|
|
Osteoma
|
?
|
|
|
Ossifying fibrtoma
|
?
|
|
|
Osteosarcoma
- frequency? - progression |
Most common pirmary neoplasm of dogs & cats
Rapidly progressive - 14-22w survival |
|
|
Osteosarcoma
- classification |
6 histological categories
- poorly differentiated (agressive) - osteoblastic - chondroblastic - fibrobalstic (last aggressive) - telangiectatic (most aggressive) - giant cell |
|
|
Ostesarcoma
- common sites in dogs |
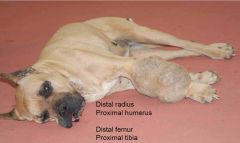
Away from the elbow, towards the knee
|
|
|
Name 2 cartilage forming tumours
|
Chondroma
Chondrosarcoma |
|
|
Chondroma
- what? - where? |
Benign tumour of cartilage
Mainly flat bones (scapula, ribs) From articular cartilage? |
|
|
Chondrosarcoma
- what? - where? |
Malignant tumour of cartilage
Arise from existing growth plate cartilage or metaplastic cartilage NOT articular cartilage |
|
|
Some more to do briefly
|
Some more to do briefly
|

