![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
17 Cards in this Set
- Front
- Back
|
When comparing pulmonary and systemic circulations:
Which one has a higher driving pressure? |
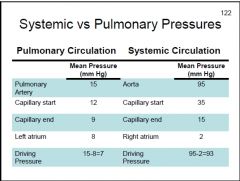
Systemic circulation
|
|
|
When comparing pulmonary and systemic circulations:
Which one has a higher risistance to blood flow? |
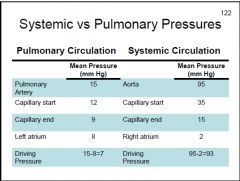
5L/min = 83 ml/s
R(systemic)=93 mmHg/83 ml/s R(systemic)=1.1 R(pulmonary)=7 mmHg/83 ml/s R(pulmonary)=0.08 |
|
|
What is the systemic and pulmonary responses to hypoxia?
|
Systemic hypoxia causes vasodilation.
Pulmonary hypoxia causes vasoconstriction. |
|
|
With respect to alveolar pressure P(A), pulmonary arterial pressure P(Pa) & pulmonary venous pressure P(PV)...describe Zone 1 perfusion?
|
Zone 1:
P(A) > P(Pa) > P(PV) -P(A) exceeds both arterial & venous pressure, therefore flow stops (ie. hemorrhage drops P(Pa) or P(A) is strongely positive such as in pos. pressure ventilation) |
|
|
With respect to alveolar pressure P(A), pulmonary arterial pressure P(Pa) & pulmonary venous pressure P(PV)...describe Zone 2 perfusion?
|
Zone 2:
P(Pa) > P(A) > P(PV) -50:50 Distention to Recruitment -flow driven by P(Pa) --> P(A) gradient -capillary pinching occurs at venous end of capillary since P(A) is larger than P(PV)...this increases resistance to flow and reduced flow to this zone |
|
|
With respect to alveolar pressure P(A), pulmonary arterial pressure P(Pa) & pulmonary venous pressure P(PV)...describe Zone 3 perfusion?
|
Zone 3:
P(Pa) > P(PV) > P(A) -70:30 Distention to Recruitment -flow driven by P(Pa) --> P(PV) gradient...capillaries dilated and flow is high |
|
|
With respect to alveolar pressure P(A), pulmonary arterial pressure P(Pa) & pulmonary venous pressure P(PV)...describe Zone 4 perfusion?
|
Zone 4:
P(Pa) > P(PV) > P(A) -extra-alveolar vessels more closed b/c transpulmonary pressure is lowest here -flow is reduced |
|
|
How does alveolar & extra-alveolar vessels affect pulmonary vascular resistance (PVR) at total lung capacity (TLC) & residual volume (RV)?
|
Alveolar vessels ↑PVR at TLC & ↓resistance at RV
Extra-alveolar vessels ↓PVR at TLC & ↑PVR at RV |
|
|
Serotonin, histamine and NE would affect PVR how?
Isoproteranol, nitric oxide and Ach would affect PVR how? |
Serotinin, histamine and NE cause smooth muscle contraction and thus ↑PVR
Isoproternal, nitric oxide and Ach cause smooth muscle relaxation and thus ↓PVR |
|
|
What is the consequence of hypoxic pulmonary vasoconstriction on blood flow?
|
Lung hypoxia causes vasoconstriction of poorly oxygenated areas, a local increase in PVR & diverts blood toward higher functioning areas.
Thus, ↑pumonary vascular pressure leads to ↓PVR due to distention and recruitment. |
|
|
How does 'general hypoxia' differ from 'regional hypoxia'?
|
Regional hypoxia of the lung will divert blood away from the area to another higher functioning area.
General hypoxia causes pulmonary hypertension which leads to pulmonary edema. |
|
|
Why would COPD, high altitudes and mitral stenosis cause pulmonary edema?
|
↑Hydrostatic pressure:
-COPD causes pulmonary hypertension -High altitudes causes hypoxic vasoconstriction -Mitral stenosis causes ↑central venous pressures |
|
|
Why would overtransfusion of saline cause pulmonary edema?
|
↓Oncotic pressure
Overtransfusion of saline dilutes blood, ↓oncotic pressures and absorption of fluid is reduced |
|
|
Why would lymphangitis or a tumor of the lymphatics cause pulmonary edema?
|
↓Lymphatic drainage
Obstruction of lymphatics cause reduced drainage |
|
|
Why would a newborn or premature infant be susceptible to pulmonary edema?
|
↑Surface tension
Respiratory distress of a newborn or premature infant which has ↓surfactant, therefore ↑surface tension and draws H2O into the alveoli & extracellular space |
|
|
Why would toxic inhalants such as chlorine, high O2, inflammation or even positive pressure ventilation cause pulmonary edema?
|
Capillary permeability after capillary damage
Toxic inhalants such as chlorine, high O2, inflammation or positive pressure ventilation can damage capillaries, which become leaky and result in fluid movement to interstitial space and the alveolus. |
|
|
What is the significance of the bronchial circulation? (shunt)
|
The bronchial circulation supplies the conducting airways w/ blood and then directly draining into the pulmonary vein. Thus 2-5% of the CO is shunted, which lowers arterial O2 content. This is called an "anatomical right-to-left shunt".
|

