![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
93 Cards in this Set
- Front
- Back
|
Which is not a typical finding on ECG for Hypertrophic cardiomyopathy (HOCM). |
A. Left atrial enlargement = broad, bifid P waves . |
|
|
Which of the 3 Sgarbossa Criteria has the most specificity associated with it ? |
Concordant ST Elevation > 1mm in leads with a positive QRS complex. |
|
|
List the Ischaemic STEMI equivalents that are found on ECG that are not of the classical variety ( 5).
|
1. Posterior MI |
|
|
List the causes of ST Elevation on the ECG that are non-ischaemic.
|
1. Benign Early Repolarisation (BER) |
|
|
What are the ECG criteria for reperfusion in AMI ? |
1. ST segment elevation > 1mm in 2/more contiguous LIMB LEADS |
|
|
What are the ECG features for Hypokalemia with K+ < 2.7 mmol / L ?
|
1. P wave - peaking |
|
|
What are the ECG features of Hyperkalaemia with K+ > 5.5 mmol / L ?
|
1. P wave - loss of |
|
|
In regards to the QT nomogram, at what uncorrected QT interval of 500 msec does the heart rate have to be to have an increased likelihood of arrhythmia ? |
less than 60 bpm. |
|
|
What is Bazett's Formula for the corrected QT interval ? |
QT (milliSeconds) / Square root RR interval (seconds ) Square root of 1 = 1 therefore QT at rate of 60 (R-R = 1) is uncorrected |
|
|
What is the length of 1 small square on the ECG ?
|
40 msec ( 0.04 sec)
|
|
|
What is the length of 1 large square on the ECG ?
|
200 msec ( 0.2 sec)
|
|
|
What is the normal speed of the paper for the 12 lead ECG ?
|
25 mm/sec.
|
|
|
List the ECG features of Hypothermia .
|
1. Tremor artefact |
|
|
Which is incorrect regarding Osborn J waves in Hypothermia? |
B. Temperature < 32 degrees.
|
|
|
What are the ECG features that increase the likelihood of a rapid wide complex tachycardia being VT rather than SVT with aberrancy ? ( 9 )
|
1. Wide complex tachycardia
- > 160 msec - HR 140-200 bpm 2. Extreme axis deviation ( "Northwest axis " ; + QRS in aVR and negative in I and aVF) 3. AV dissociation (25%) 4. Capture beats 5. Fusion beats "hybrid complex" 6. Concordance ( + or - in precordial leads ) 7. Brugada's sign ( > 100msec distance from QRS onset to nadir of S wave ) 8. Josephson's Sign ( notching near nadir if S wave in V1V2 ) 9. RSR complex has taller left R wave ( Rsr) |
|
|
Which of the 4 ECG stages of pericarditis has the most prominently recognised ECG findings?
|
Stage I : |
|
|
Best place to look at p wave? What conditions cause prominent P wave changes ? P waves all look different? |
Lead II & V1
Hypokalaemia : peaked P wave
Multifocal Atrial Tachycardia |
|
|
What of the following conditions does not cause PR interval lengthening ? |
B. Hypocalcaemia |
|
|
Which Environmental / Electrolyte / drug-induced conditions does not cause QRS widening ?
A. Hypothermia B. Hyperkalaemia C. Hypomagnesaemia D. Hypercalcaemia |
D.
|
|
|
Which Conditions / drugs / electrolytes does not cause QT interval shortening ?
A. Hyperkalaemia B. Hypokalaemia C. Hypercalcaemia D. Digoxin effect |
B.
|
|
|
Which conditions / drugs / electrolytes does not cause QT interval prolongation ?
A. Hypocalcaemia B. Hyperkalaemia C. Hypokalaemia D. Hypothermia and Hyperthermia |
B.
|
|
|
What are the differentials for ST elevation in aVR ? (5)
|
1. Left main coronary occlusion
2. Ventricular tachycardia (VT) 3. Hyperkalaemia 4. Na+ channel blockade 5. Lead placement ** |
|
|
What are the ECG features of Hypercalcaemia ?
|
ST segment depression |
|
|
List the 7 main categories of causation of a Prolonged QT interval.
|
1. Electrolytes
2. Endocrine 3. Environmental 4. Drugs / Toxins 5. Cardiovascular disease 6. Cerebrovascular disease 7. Hereditary |
|
|
List the electrolyte causes of a Prolonged QT interval.
|
1. Hypokalaemia
2. Hypomagnesaemia 3. Hypocalcaemia |
|
|
List the Endocrine and Environmental causes of a Prolonged QT interval .
|
Endocrine
1. Hypothyroidism Environmental 1. Hypothermia |
|
|
List the 6 drug / toxin categories that cause a prolonged QT interval. |
1. Antiarrhythmics ( Ia ; Ic ; III ) |
|
|
LVH criteria |
V5 or V6 >25mm S in V1 + R V5/6 >35mm R in lead I + S lead 3 >25mm R avL >11mm |
|
|
RVH criteria |
RAD R in V1 >7mm (or R:S >1 i.e. dominant) R in V1 + S V5/6 >11mm
(QRS < 120mm i.e. changes not due to RBBB) |
|
|
Causes dominant R wave in V1 |
Posterior MI WPW type A RVH R heart strain = Lung disease RBBB |
|
|
Changes in pericarditis |
Widespread STE PR segment depression |
|
|
Pericardial effusion |
Electrical alternans - axis changes with each beat i.e. different QRS complexes |
|
|
ANTERIOR ISCHAEMIA: 'Extensive' - anterolateral Septal Anterior Lateral (apical)
|
Extensive - V1-6; I; avL - Proximal LAD Septum - V1-3 - Septal perforaters of LAD Anterior - V4-6 (I; avL) Diagonal (supplies ant LV wall) Lateral - V5,6; I; avL - Distal LAD or circumflex
|
|
|
INFERIOR ISCHAMIA: Inferior (localised) Inferior (extended): Infero-lateral Inferio-posterior RV |
Localised - II, III; avF - RCA or circumflex Extended - as above, plus: Inf-lat - I; avL; V5-6 - RCA or dominant Cx Inf-post - V1-2 - PDA or RCA RV - V1-3R; V4R - Prox RCA |
|
|
V1/2 prominent R wave + ST depression + TWI |
Consider posterior leads |
|
|
Prolonged QT - values |
Normal = 435msec Prolonged = >50% of R-R interval F = 460; M = 450 QTc = QT / (sq r) of RR |
|
|
Causes long QT - Congenital |
Romano-ward syndrome - autosomal dominant Juville Lane syndrome - autosomal recessive (+ sensorineural deafness) |
|
|
Causes Long QT - Acquired |
Cardiac - ischaemia; myocarditis; CM SAH Electrolytes - Dec Ca/Mg Drugs: Antiemetics - droperidol; metoclo; ondans ABs - erythromycin Antipsycho - halop Antidepressants - TCA Anti-arrhyth - amiodarone; procainamide Prokinetics - cisapride |
|
|
Digoxin changes |
AF ST dep & TWI lateral chest leads |
|
|
U wave |
Extra wave after T wave: - Bradycardia (most common cause) Dec K (characteristic of severe) - Dec Mg - Dec Ca - CM |
|
|
Hypercalcemia |
Shorted QT Wide T J/osborn waves U wave |
|
|
Hyperkalaemia |
Tented p; Prolonged PR (5.5-6.5) Loss of p (6.5-7.5) Long QRS (7.5-8.5) Sine wave (>8.5) VT
|
|
|
Hypokalaemia |
Enlarged P Prolonged PR TWI ST dep U waves Long QT Arrhythmia |
|
|
LAD |
Left anterior hemiblock L BBB WPW type B Inferior MI |
|
|
RAD |
L posterior hemiblock RVH / strain RBBB WPW type A Posterior MI |
|
|
VT criteria |
Broad complex: >120 = VT 100-120 = accelerated idioventricular rhythm <100 = idioventricular rhythm |
|
|
Differentiating VT from SVT with aberrant conduction = Brugada criteria |
Absence of R-S complexes in each chest lead = VT RS interval > 100ms (2.5 small squares) = VT Independent atrial actvity (fusion beat, capture beat) = VT Typical bundle branch pattern = SVT |
|
|
LBBB - how do you tell if there is ischaemia? |
Appropriate disconcordance = normal Inappropriate concordance = ischaemia |
|
|
cc |
LVH |
|
|
cc |
RVH |
|
|
ccc |
Pericarditis |
|
|
cc |
Pericardial effusion Electrical alternans |
|
|
cc |
Long QT |
|
|
cc |
Digoxin changes: AF + STD + TWI lateral leads |
|
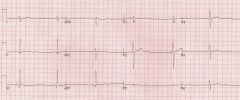
|
Sinus bradycardia & U waves Anorexia nervosa pt |
|
|
ST depression Morphology |
Myocardial ischamie: - Horizontal or downsloping ST depression >0.5mm at the J point in 2 or more contiguous leads - > 1mm - more specific & worse prognosis - >2mm in >3 leads - high chance of NSTEMI & high mortality (35% at 30 days)
Upsloping - non-specific for ischaemia |
|
|
Left Main occlusion |
Pattern of widespread ST depression, with STE in avR |
|
|
Right Heart strain |
ST depression / T wave inversion in the right precordial (V1-4) and inferior (II, III, aVF) leads |
|
|
ECG Changes in PE |
Sinus tachy most common SI Q III T II Complete or incomplete RBBB RV strain pattern RAD P pulmonale - peaked p wave in lead II>2mm Simultaneous TWI inferior & R praecordial leads (V1-3) |
|
|
What is Wellens Syndrome |
ECG abnormality strongly associated with significant left anterior descending coronary artery stenosis Two types - most common being deep TWI in leads V2-3 |
|
|
In Left Atrial Enlargement, the P wave: A. Increases in amplitude B. Increases in duration C. Increases in both amplitude & duration D. Shows terminal P negativity in lead I E. All of the above |
B |
|
|
When interpreting an ECG, right ventricular hypertrophy (RVH) can mimic which of the following conditions? A. LBBB B. AV Block C. True posterior MI D. LAFB E. LPFB |
C
The prominent anterior forces seen in RVH are also seen in a number of other conditions including a true posterior MI. Thus, RVH is sometimes referred to as a pseudoinfarct. |
|
|
Sign of Right atrial enlargement? |
RAE is recognized by the tall (> 2.5mm) P waves in leads II, III, aVF. |
|
|
Signs of Left Atrial Enlargement? |
The P-wave is notched, wider than 0.12s, and has a prominent negative (posterior) component in V1. These are all criteria for left atrial enlargement (LAE). |
|
|
Pacemaker Code VOO |
Asynchronous No sensing circuitry Discharges continuous regardless of pt's rhythm
|
|
|
PM Code VVI |
Demand Pacing Paces when it doesn't sense R waves from V electrode Doesn't interfere with intrinsic rhythm above a certain rate |
|
|
PM Code DDD |
Sequential/Dual Pacing Maintains AV contraction sequence Pace & sense A & V sequentially |
|
|
What is Wellen's Syndrome? |
ECG abnormality strongly assoc w significant LAD stenosis 2 Types: - Symmetric deeply inverted T waves in V2 & V3 - Biphasic T waves in V2 & V3 (less common) Plus Hx of CP, no Q waves, No STE |
|
|
Measuring PR interval |
From beginning of p to beginning of QRS Normal <200ms |
|
|
Normal QT interval |
Measure from beginning of QRS to end of T wave At HR = 70, upper limit of QT is 400ms Add or subtract 20msec for every 10 beats above or below 70 |
|
|
Pathological Q wave |
Either wide >0.04ms Or deep >30% of QRS height |
|
|
MI - LCx - Region & leads |
LCx * Posterior MI* Dominant R & Tall T V1-2 * STE V7-9 (STD V1-2)
Seek & exclude LCx + LAD = Posterolateral LCx + RCA = Inferoposterior |
|
|
MI - Lesion LAD - Type of MI & leads |
LAD - Combination of following: * Septal (STE V1-2)* Anterior (STE V3-4) * Lateral (STE V5-6; I; aVL) |
|
|
RCA 'Type' MIs - Region & Leads |
RCA - Occlusion distal to RV: * Inferior MI - 58% of MI (STE II, III, aVF; STD aVL)* Inferior & RV MI (as above + STE V1, V4R) * Increased mortality * LAD & LCx occlusion in L dominant system |
|
|
What does concordance mean? |
Throughout chest leads - leads V1-6 show entirely positive (R) or entirely negative (QS) complexes, with no RS complexes seen
Increases likelihood of VT > SVT w aberrant conduction |
|
|
VT vs SVT with aberrant conduction - relative frequencies |
VT: - 80% of all broad complex tachycardias (BCT) - 95% in pts w structural heart disease
So if in doubt - Rx as VT |
|
|
Left Main Occlusion Features |
STE >1mm in aVR - 95% for LMCA occlusion when there is evidence of ischaemia in other leads (typically widespread STD)
STE in aVR >1.5mm - 75% mortality Need urgent cath lab |
|
|
WPW Diagnostic criteria (WHO) |
PR interval <0.12s Delta wave QRS >0.12s Normal p-wave axis
Orthodromic - down AV & back up accessory (most common) Antidromic - down accessory & back up AV node - ominous as can drive at rapid vent rates (p is after QRS) |
|
|
What is a fusion beat? |
When a VE occurs just after a sinus beat has started to propagate into the His-Purkinje system - combines morphology of normal sinus beat to the extrasystole |
|
|
What is a capture beat? |
During VT - when a normal sinus beat sneaks through - normal-shaped QRS & T wave |
|
|
Trifascicular Block |
Trifascicular block - disease in all 3 fascicles i.e. CHB: * Right bundle* Left bundle = Left anterior & Left Posterior * Bifascicular + 1st (most common) or second degree AV block * RBBB + LAFB or LPFB |
|
|
LBBB Diagnostic Criteria |
* QRS duration >120ms
* Dominant S wave in V1 * Broad mono phasic R wave in lateral leads * Absence of q waves in lateral leads (still allowed in aVL) * Prolonged R wave peak time >60ms in left praecordial leads Associated: - Appropriate DISconcordance - ST & TW in opposite direction to main vector of QRS - Poor R wave progression |
|
|
Risk of Asystole if Bradycardic |
* Mobitz II AV block
* Recent asystole * Ventricular pauses > 3sec * CHB with broad complex QRS |
|
|
Signs of Digoxin Effect |
Downsloping ST depression - characteristic "sagging" appearance (most evident in lateral leads) Flattened, inverted, or biphasic T waves (most common) Shortened QT
Also - Mild PR prolonged (increased PNS tone); U waves |
|
|
Digoxin Toxicity |
Clinical Features: * Nausea; Vomiting; Anorexia |
|
|
Causes of LVH |
* HTN
* AS * AR * MR * Coarctation of aorta * HOCM |
|
|
LV & RV Strain |
Strain = repolarisation abnormality due to hypertrophy or dilation LV: * TWI in lateral leads (V5-6, I & aVL)* TWI & STD in right praecordial leads (V1-3 & inferior leads - i.e. RV is anterior & inferior) |
|
|
Post-Op Visual Loss - Causes |
1. Central retinal artery occlusion (external orbital compression)
2. Ischaemic optic neuropathy (anterior or posterior) 3. Compression optic nerve or chasm by pituitary tumour (check cortisol & TSH) 4. Cortical visual loss 5. Functional visual loss |
|
|
Examination post-op visual loss |
* Visual acuity (doesn't help with Dx as variable findings)
* Pupillary testing * Visual fields * External examination * Ocular motility * Fundoscopy (dilated) |
|
|
Findings Orbital compression (CRAO) |
* Usually monocular
* Ocular motility abnormalities * External oedema * Chemosis * Fundus findings of CRAO |
|
|
ION Findings |
* Afferent pupillary defect if unilateral
* If bilateral -> poorly reactive pupils (although meds can confuse findings) * Optic nerve: * Acuity - range normal to 'no light perception' |
|
|
Post-op Visual Loss from intracranial compression - O/E findings |
Can be unilateral or bilateral. Afferent pupillary defect if unilateral, or bilateral & asymmetric. Visual acuity - variable. Chiasm compression -> Visual fields are the key Cortical visual loss - 2 patterns: 1. Unilateral -> homonymous hemianopic visual defect w normal acuity2. Bilateral -> bilat homnomous hemianopic visual field defects w variable loss of visual acuity In cortical blindness - even is pt completely blind pupils will be normal reactive w normal fundo. MRI is critical |
|
|
Post-op Visual Loss - Treatment |
* Controversial w poor evidence
* Transfuse to Hb 10 * Normal BP & supplementary O2 (unproven but likely harmless) * No evidence for steroids, IOP-lowering agents or anti-plts |

