![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
101 Cards in this Set
- Front
- Back
|
Brunner’s Glands:
Function Location |
Located in duodenum.
Secrete alkaline mucous into ducts that track upward through the muscularis mucosae and into the crypts of Liberkühn for release into lumen. |
|
|
Crypts of Liberkühn:
Function Location |
Located in duodenum and colon.
Release the alkaline mucous produced by Brunner’s glands in duodenum Release mucus produced by goblet cells in colon |
|
|
Peyer’s Patches:
Location |
Ileum
|
|
|
Glomerulonephritis
Photosensitivity Rash Arthralgias |
SLE
|
|
|
VRDL in SLE:
Lab values Effects |
Lab values show increased antiphospholipid antibody (APLA) against Lupus anticoagulant
Effects: 1) Venous thromboembolism 2) Arterial thromboembolism 3) Increased fetal loss*** |
|
|
Lupus anticoagulant:
Diagnostics Effects |
Can detect with positive VRDL (*false positive*), prolonged PTT***
Inc’d anticoagulant→hypercoagulable state (uncertain mechanism)→thromboembolism and/or repeated miscarriages |
|
|
Anaplastic cells:
Define anaplasia Histologic features |
Anaplasia = neoplastic cells with a complete lack of differentiation
Histologic features: -Lose cell polarity/tissue architecture—cells coalesce into sheets/islands in disorganized fashion -Cellular pleomorphism—sig variation in shape/size of cells -Larger nuclei than those in normal cells (high nucleus-to-cytoplasm ratio) -Numerous, often abnl mitoses -GIANT, MULTINUCLEATED TUMOR CELLS |
|
|
Under 1 year-old
Repeated lower respiratory infections Candida extract injection results in indurated nodule |
Bruton’s agammaglobulinemia
Positive reaction to candida indicates intact T cell response Recurrent resp infections due to very low number of mature B cells |
|
|
Bruton’s agammaglobulinemia:
Pathophys |
X-linked immunodeficiency
Absence of immunoglobulin and B cells due to defect in B cell maturation (remember: B cells produce Ig) |
|
|
No LN germinal centers
|
Bruton’s agammaglobulinemia
|
|
|
Paracortical zone of LN:
Contents |
T cells
APCs |
|
|
Cystic Fibrosis:
Molecular pathophys |
Mutation in CFTR gene (deltaF508) results in defective post-translational folding and glycosylation
Results in degradation of CFTR membrane protein before it reaches cell surface |
|
|
ANOVA;
Utility |
Compare means of three or more variables
|
|
|
Chi-square test:
Utility |
Compare proportions of a categorized outcome (“high”, “normal”, “low”, etc)
|
|
|
A study compares drug outcome via fibrinogen levels categorized as high and normal.
What statistical test would be appropriate for this study? |
Chi-square
|
|
|
Patent Urachus:
Presentation Embryologic pathophys |
Patent urachus presents with urine discharge from umbilicus.
Urachus is remnant of allantois, which connects bladder with yolk sac during fetal development. Failure of urachus to obliterate = patent urachus. |
|
|
Persistent yolk sac:
Presentation |
Persistent yolk sac (vitelline duct) connects small bowel with skin at umbilicus. Presents w/meconium discharge from umbilicus.
|
|
|
Cyanide poisoning:
Pathophys Presentation Treatment and MOA |
Cyanide binds cytochrome a-a3 complex (…)—critical for electron transport during ox-phos. This results in inhibition of aerobic metabolism and death
Presentation: Rapidly-developing cutaneous flushing Tachypnea HA Tachycardia N/V Confusion Weakness Tx: Nitrites (Fe2+→Fe3+)—form methemoglobin, which can’t bind oxygen, but can avidly bind CN-; thus, sequestering it in blood (keeps poison out of mitochondria) ALTERNATE TREATMENT: Na+ Thiosulfate—combines w/CN- to form less-toxic thiocyanate, which is excreted in urine. |
|
|
How does methemoglobin differ from hemoglobin?
|
Methemoglobin contains ferric rather than ferrous iron. CN- binds ferric iron more avidly than mitochondrial cytochrome enzymes.
|
|
|
This nerve exits through the obturator foramen.
Function? |
Obturator nerve: adductor compartment of thigh
Damaged during pelvic surgery, especially during LN dissection |
|
|
Adduction of thigh:
Nerve |
Obturator nerve
|
|
|
Abduction of thigh:
Nerve |
Superior gluteal nerve
Femoral nerve |
|
|
Extension of thigh:
Nerve |
Inferior gluteal nerve
|
|
|
Flexion of thigh:
Nerve |
Lumbar plexus
Femoral nerve |
|
|
Extension of leg:
Nerve |
Femoral
|
|
|
Glossopharyngeal nerve:
CN Number Result of injury |
CN IX
Lose gag reflex, sensation in upper pharynx, POSTERIOR tongue, tonsils, middle ear, loss of taste in POSTERIOR third of tongue |
|
|
Taste sensation in anterior two-thirds of tongue:
Cranial Nerve |
Facial
|
|
|
General sensation of tonsillar lining:
Cranial Nerve |
Glossopharyngeal
|
|
|
Salivary secretion from submandibular and sublingual gland:
Cranial Nerve |
Facial
|
|
|
Protrusion of tongue:
Cranial Nerve |
Hypoglossal Nerve
|
|
|
Minute ventilation:
Formula |
Tidal volume x Respiratory Rate
INCLUDES DEAD SPACE |
|
|
Urea formation:
Critical step Effect of defect in this step Treatment |
Ornithine transport from cytosol to mitochondria, where it then combines with carbamoyl phosphate to form citrulline.
Defect in this step would lead to inc’d levels of ammonia!-->CNS dysfn Tx: Protein restriction |
|
|
Nicotinic acid:
MOA Use AEs |
Nicotinic acid aka vit B3/niacin, inhibits VLDL production.
Used to increase HDL levels. AEs: Flushing Hepatotoxicity in high doses Cholesterol gallstones if acts as bile acid-binding resin (research this) |
|
|
Hypertension
Low plasma renin Weakness Paresthesia |
HTN & low renin→elevated aldosterone
Weakness & parasthesia→hypokalemia (expected in aldosterone excess) Thus, primary mineralocorticoid excess |
|
|
Excess aldosterone:
Effects |
Sodium retention
K+ loss Inc’d urinary H+ excretion (metabolic alkalosis) |
|
|
Why is hypernatremia not seen in hyperaldosteronism?
|
Aldosterone escape—inc’d sodium and Cl- absorption in hyperaldosteronism leads to intravascular hypervolemia.
This promotes releas of atrial natriuretic peptide→diuresis and eventual compensatory sodium loss Thus, no edema |
|
|
Describe the following lab values for primary aldosterone excess:
Bicarbonate Potassium Sodium |
Bicarb will be elevated—this is a state of metabolic alkalosis
K+ will be decreased—aldosterone promotes K+ excretion Sodium will be normal—despite retention of Na+, ANP keeps Na+ levels normal |
|
|
Digoxin:
Effects Use |
Use for a. fib w/rapid ventricular response (AD w/RVR—HR>100) bc slows conduction through AV node (USED AS SECOND LINE TX)
Slows conduction through inc’d parasympathetic tone via VAGUS STIMULATION Summary--Digoxin has 2 physiologic effects: 1) Blocks Na-K-ATPase in cardiac myocytes→inc’d intracellular Ca2+ 2) Dec’d AV nodal conduction by inc’d Psymp tone |
|
|
Obstructive lung disease:
Effect on lung volumes Examples of such diseases Effect on TLC/RV |
Ex: Asthma, chronic bronchitis, emphysema, bronchiectasis
Obstructive lung dz→air trapping and hyperinflation of lungs: Inc’d TLC, RV, and RV/TLC Dec’d FEV1, FEV1/FVC While TLC will be increased, RV will be decreased by a much greater factor; thus TLC/RV will increase. |
|
|
Pulsus paradoxus is a sign of __________.
|
Cardiac tamponade
|
|
|
2 weeks post-mild respiratory illness
Severe weakness, dizziness Fluid accumulation in pericardial cavity |
Cardiac tamponade; likely secondary to inflammn caused by virus (possibly same virus that caused upper resp tract infection)
|
|
|
What is pulsus paradoxus?
|
Drop in arterial BP during inspiration of over 10 mmHg (decrease of less than 10 mmHg is physiologic)
Clinically: palpate radial pulse and noting it disappears on inspiration |
|
|
When does cardiac tamponade become symptomatic?
Pathophys? Effects on pre/afterload |
When pericardial pressure exceeds 10 mmHg, force is sufficient to cause collapse of atria→inc’d systemic venous pressure, reduced ventricular preload, and eventually dec’d cardiac output.
Death results from cardiogenic shock, when Q is insufficient to provide O2 for tissue. |
|
|
Pulsus alternans is a sign of_________.
|
LV dysfn
|
|
|
What is pulsus alternans?
|
Beat to beat variation in magnitude of pulse pressure in presence of regular cardiac rhythm.
|
|
|
Pulsus parvus et tardus is a sign of _______.
|
Aortic stenosis
|
|
|
What is pulsus parvus et tardus?
|
Pulse of low magnitude and delayed peak
|
|
|
Multiple sclerosis:
Molecular pathophys Diagnosis Presentation |
Lesions of white matter than result in:
-demyelination (denudation) of axons -Depletion of oligodendrocytes (produce myelin in CNS) -Lipid-laden macrophages (they phagocytize myelin breakdown products) -Astrocytosis (astrocyte proliferation is a reaction to inury) Dx: Brain MRI Presentation: -Dysfnl lateral conjugate gaze (slow adduction of one eye while looking laterally)—due to denudation of MLF (medial longitudinal fasciulus) -Optic neuritis—dec’d or blurred vision, monocular blindness, central scotoma (whatever that is) -Sensory loss, arm of leg weakness -Cerebellar syx (clumsiness, ataxia) |
|
|
Intenuclear ophthalmoplegia:
What is it? Cause? |
Dysnl lateral conjugate gaze—have trouble adducting one eye upon lateral gaze
Due to lesion of MLF (as in MS) |
|
|
Pyridoxine:
Role |
AKA vitamin B6—cofactor for transamination and decarboxylation of amino acids, for gluconeogenesis, etc.
Transamination = amino acid + alpha-keto acid→transfer amino group to alpha-keto acid for it to become amino acid Ex: oxaloacetate + glutamate→aspartate Transaminases (aminotransferases) = enzyme, pyridoxine (B6) = cofactor |
|
|
Lecithinase:
Associated bug MOA |
Main toxin of C. perfringens
Lecithinase AKA phospholipase C AKA alpha-toxin; splits phospholipid molecules |
|
|
This bug cannot grow on 5% sheep blood agar.
Why not? How can this be changed? |
Sheep blood agar plates lack nutrients to support growth of H. flu; also have Factor V inactivating enzymes.
Growth of H flu can be achieved by streaking medium w/Staph aureus. Staph. Aureus lyses RBCs in medium and releases Factor X (hematin) is released. Factor V (NAD+) is also released by staph. |
|
|
Factor V and X AKA
|
Factor V = NAD+
Factor X = Hematin |
|
|
Lactose fermentation:
Associated bug Gene required |
E. coli
Lac-operon (inducible and repressible in absence of glucose)—activated by glucose deficit, repressed when glucose available |
|
|
Recurrent infections with Pseudomonas
Chronic diarrhea Weight loss |
Cystic fibrosis
|
|
|
How does cystic fibrosis result in diarrhea and weight loss?
Treatment? |
Obstructive fibrosis and progressive exocrine pancreas insufficiency→malabsorption→diarrhea
Tx with pancreatic lipase |
|
|
Sulfasalazine:
MOA Use |
Inhibit PG and LK synthesis during inflammn
Use in Crohn’s, UC |
|
|
Octreotide:
MOA Use |
SMS analogue that decreases gut motility, blood flow, pancreatic secretion
Use in VIPoma |
|
|
This nerve is most commonly affected in leg injuries.
|
Common peroneal (fibular) nerve—superficial and courses laterally around neck of fibula
|
|
|
Fibular nerve:
Location Functions Effect of lesion Examples of trauma |
Located at neck of fibula
Eversion of foot Dorsiflexion of feet and toes Sensation of feet Lesion→foot drop and foot inversion Ex: Lateral blow to knee and tightly applied plaster casts/devices |
|
|
Foot drop
|
Fibular nerve (common peroneal)
|
|
|
Unopposed inversion of foot
|
Lesion to fibular nerve (Common peroneal)
|
|
|
Unopposed eversion of foot
|
Injury to tibial nerve
|
|
|
Dorsiflexion of foot
|
Injury to tibial nerve
|
|
|
Tibial Nerve:
Function |
Inversion and plantarflexion of feet
|
|
|
Long-term hemodynamic compensatory response to aortic regurgitation.
|
Inc’d LV preload (end-diastolic volume)
ECCENTRIC LV hypertrophy |
|
|
When is concentric hypertrophy seen in the LV?
|
In times of pressure overload, such as aortic stenosis and systemic HTN.
|
|
|
When is eccentric hypertrophy seen in the LV?
|
In times of volume overload, such as in aortic regurgitation.
|
|
|
Patient undergoing elective surgery:
Drug to prevent venous thrombosis MOA |
Heparin—increases effect of Anti-Thrombin III (by binding it)
|
|
|
Argatroban:
MOA Use |
Directly bind thrombin active site and inhibit its activity
Use in HIT |
|
|
Ticlopidine:
MOA Use |
Inhibit ADP mediated platelet aggregation; useful in tx of unstable angina and non-Q wave MI (…)
|
|
|
This drug inhibits arachidonate product formation.
|
ASA
Arachidonate = arachidonic acid |
|
|
Pelvic inflammatory disease:
Presentation Causes Effect on pregnancy |
Fever
Rebound abdominal tenderness Vaginal discharge N. gonorrhoeae or Chlamydia 50% of patients with PID have ectopic pregnancy |
|
|
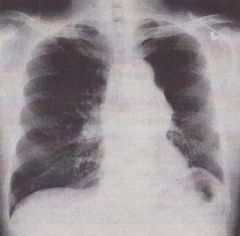
COPD:
Low, flattened diaphragm Hyperinflated lungs |
|
|
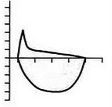
Severe obsructive dz—COPD (inc’d RV at end-expiration, dec’d tidal volume)
|
|
|
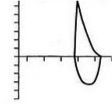
Pulmonary fibrosis—dec’d lung volume and compliance (RESTRICTIVE PATTERN)—dec’d tidal volume and residual volume
|
|
|
Slow growing mass
Oral trauma Yellow pus |
actinomyces israeli
|
|
|
Actinomyces:
Gram -/+ Location Effects Treatment |
Gram +
Oral flora Chronic (slow growing) face and neck abscesses Tx: Parenteral PCN, surgical debridement |
|
|
Ectopic pregnancy:
Treatment MOA |
Methotrexate (<6 weeks gestation of ectopic pregnancy)
MTX competitively inhibits dihydrofolate reductase (DHF), which catalyzes reduction of folic acid to DHF and subsquently reduces DHF to tetrahydrofolate (THF). MTX inhibition of THF inhibits purine and thymidylate synthesis and results in accumulation of dihydrofolic acid polyglutamate. |
|
|
This drug is structurally similar to folic acid.
|
Methotrexate
|
|
|
Why is hydroxyurea used in HbS?
Under what circumstances is it used? |
Increases Hb F synthesis thus conferring protection against polymerization of sickle cells
Reserved for sickle patients with pain crises |
|
|
Why are Gardos channel blockers used in HbS?
|
Hinder efflux of K+ and H2O from cell, preventing dehydration of RBCs and reducing polymerization of HbS
|
|
|
Left supraclavicular LAD
|
Occult gastric cancer (Virchow's node)
|
|
|
Subcutaneous mass in periumbilical region
|
Occult gastric cancer
(Sister Mary Joseph Nodule) |
|
|
Poorly differentiated cells in ovary heavily loaded with mucus
|
Krukenberg tumor due to gastric cancer mets
|
|
|
Severe chest pain not relieved by rest of nitroglycerin
Diaphoresis Dyspnea Lightheadedness |
Acute transmural MI
|
|
|
What are the EKG signs of acute transmural MI? Provide a chronological progression.
|
Peaked T waves = first sign
ST elevation in minutes to hours Q-waves in involved leads within hours to days |
|
|
Transmural infarction:
Cause |
Plaque rupture producing a superimposed thrombus that COMPLETELY occludes involved coronary artery
|
|
|
When do symptoms of unstable angina become apparent?
|
Upon 75% of coronary artery lumen occlusion
|
|
|
What is Prinzmetal's angina?
How does it differ from acute MI? |
Episodic angina that occurs at rest
Duet o coronary artery vasospasm Responds promptly to vasodilators such as nitroglycerin |
|
|
Describe the steps of glycolysis in both aerobic and anaerobic conditions.
|
Glucose-->Fructose 1,6-bisphosphate
-->Glyceraldehyde-3-phosphate-->1,3-BPG via glyceraldehyde-3-phosphate dehydrogenase REQUIRES NAD+ -->Pyruvate -->Acetyl Coa-->TCA Aerobic: NAD+ regenerated (from NADH) via TCA In exercising muscle, cell has limited stored of NAD+; instead of pyruvate forming, lactate is made. |
|
|
P50:
What is it? Effect of left/right shifts? When do left/right shifts occur? Physiologic responses to these shifts? |
P50 = Po2 where Hgb is 50% sat'd
A decreased in P50 means Hgb has increased O2 affinity--this causes less O2 to be released into tissues, and results in hypoxia, then reflex POLYCYTHEMIA KNown as a LEFT shift (inc'd pH, dec'd 2,3-DPG, dec'd Temp)--THINK LUNGS for LEFT Right shift: Inc'd p50 means lower affinity for O2 and will inc tissue delivery; Causes: Dec'd pH, inc'd 2,3-DPG, inc'd temp (THINK TISSUES) |
|
|
When is hypoxia-induced hemolysis seen?
|
Sickle cell
|
|
|
When is oxidant-induced hemolysis seen?
|
G6PD deficiency + oxidant stress (antimalarials, sulfonamides, fava beans)
|
|
|
Hereditary spherocytosis:
Associated mutations |
Mutations in spectrin and ankyrin
|
|
|
Marfan Syndrome:
Autosomal Dom/Rec? Gene defect Most likely cause of death Known anatomic abnormalities |
Autosomal dominant
Defect in fibrillin-1 gene-->lens dislocation, mitral valve prolapse, medial degeneration of the aorta (leading to aortic dilatation and ***dissection***) Most likely cause of death: aortic disease |
|
|
Hypertension
Low potassium Depressed renin Adrenal mass |
Aldosterone-secreting tumor (adenoma) leading to hyperaldosteronism (Conn's Syndrome)
|
|
|
Aldosterone secreting tumor:
Presentation What is the role of aldosterone? Treatment |
HTN, hypokalemia, metabolic alkalosis, depressed renin activity
Aldosterone induces resorption of Na, H2O, and wasting of K+ and H+, leading to hypokalemia and alkalosis. Inappropriately high aldosterone will inhibit renin activity. Tx: Aldosterone antagonists! Ex: spironolocatone, eplerenone |
|
|
Sprinolocatone:
Drug Class AE |
Aldosterone antagonist
AE: gynecomastia |
|
|
What drugs can be added to antibiotics to help overcome beta-lactamases?
|
Lactamase inhibitors such as tazobactam and clavulanic acid (and sulbactam)
|
|
|
Antibiotic for anaerobes
|
i.e., bacteroides!
Piperacillin |

