![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
74 Cards in this Set
- Front
- Back
|
What two components make up the LPS?
|
* Lipid A = hydrophobic lipid component
* Carbohydrate component |
|
|
What two components make up the hydrophilic carbohydrate portion of LPS?
|
* O-polysaccharide
* Core oligosaccharide |
|
|
Of the two components of the hydrophilic carbohydrate, which is utilized to differentiate between the serological diversity of gram bacteria?
|
O-polysaccharide
|
|
|
When during its development cycle will N. meningitidis shed endotoxin? By which method?
How does that compare to Enterobacteriacae? |
N. meningitidis sheds endotoxin while still growing via a process of BLEBBING.
Enterobacteriacae only release endotoxin at the death of the organism. |
|
|
Are all of the LPS components immunogenic?
Are they all useful for differentiating between strains or species? |
Yes
No |
|
|
Which of the two components of the LPS activate the complement pathways:
* Lipid A * Carbohydrate |
* Lipid A = classical
* Carbohydrate = alternative |
|
|
How are the major effects of Lipid A derived? Through which interaction?
|
Through its interaction with MACROPHAGES
|
|

Describe the major effects of Lipid A and its interaction between macrophages.
|
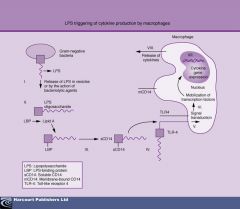
1. Lipid A enters the bloodstream, bound by LPS binding protein (LPS-BP)
2. LPS-BP + Lipid A = bound to soluble CD14 (sCD14) 3. LPS-BP + Lipid A + sCD14 are transferred to TLR4 on a MACROPHAGE 4. TLR4 (has signal transduction capabilities) when bound to Lipid A results in CYTOKINE gene activation 5. Production of TNF-α, IL-1, IL-6, and IL-8 |
|
|
Of the cytokines given here, which activate the "acute phase reaction" and which "recruit neutrophils"?
TNF-α, IL-1, IL-6, IL-8 |
acute phase reaction = TNF-α, IL-1, IL-6
neutrophil recruitment = IL-8 |
|
|
Of the known cytokines, which has systemic effects and is thought to cause extreme morbidity?
|
TNF-α
|
|
|
Clinically, what five effects are seen with the activation of TNF?
These effects will lead to what two events? |
1. High fever
2. Vasodilation 3. Capillary leakage 4. DIC 5. Cardiodepression *** These will all lead to SHOCK and ultimately MULTIPLE ORGAN FAILURE |
|
|
Describe N. meningitidis based on the following:
* Type of bacteria * Which two -ASEs? * Ferments what? Does not ferment what? * What is its only natural host? |
Type: encapsulated gram (-) diplococcus
ASEs: oxidase, catalase Ferments: glucose, maltose but NOT sucrose, lactose Host: humans |
|
|
What are the three (3) important virulence factors for N. meningitidis?
|
1. Polysaccharide capsule resisting phagocytosis
2. LPS that sheds by blebbing 3. IgA protease to cleave IgA |
|
|
Describe N. meningitidis in terms of transmission, attachment, and spread?
|
Transmitted: airborne droplets where infection is preceded by colonization of the nasopharynx
Attachment: to nasopharyngeal epithelial cells aided by fimbraiae Spread: by fimbriae allowing it to enter the bloodstream and spread to other sites |
|
|
The N. meningitidis organism is serologically divided into which groups?
|
A, B, C, W135, X, Y, Z
|
|
|
Which of the groups cause the most disease?
A vaccine is available against these groups? Which of the groups is NOT strongly immunogenic? |
Disease: A, B, C
Vaccine: A, C, Y, W135 NOT immunogenic: B |
|
|
What "drug" is recommend for those in close contact with patients with meningococcal disease?
|
Antimicrobial chemoprophylaxis
|
|
|
Patients with acute meningococcal infections can present with 1 of 3 syndromes. What are they?
|
1. Uncomplicated bacteremic process
2. Metastatic infection that involves the meninges 3. Overwhelming systemic infection with circulatory collapse and evidence of DIC |
|
|
Meningococcal septicemia is produced by four basic process.
What are they? |
1. Capillary leak
2. Coagulpathy 3. Metabolic derangement 4. Myocardial failure |
|
|
What is the associated with each of the four process of septicemia?
|
CAPILLARY LEAK
loss of albumin into urine & extravascular space -> hypovolemia & decreased venous return COAGULOPATHY severe bleeding tendency with severe thrombosis in (microvasculature of skin) -> amputation of digits or limbs METABOLIC DERANGEMENT Profound acidosis w/ severe metabolic abnormalities: Hypo-(kalemia, calcemia, magnesemia, phosphatemia) MYOCARDIAL FAILURE skin lesions often contain meningococci being phagocytosed by neutrophils skin rash is characteristic manifestation w/ widespread petechial eruption |
|
|
Fulminant meningococcemia has a mortalityrate that can exceed what percentage DESPITE appropriate antibiotic therapy?
|
50%
|
|
|
N. meningitidis is found to replicat where?
|
Upon entering the meninges, it multiples in the CSF and pia arachnoid
|
|
|
The neurological damage is a consequence of which three process?
|
* Direct bacterial toxicity
* Indirect inflammatory processes (cytokines, edema) * Systemic effects (shock, seizures, cerebral hypoperfusion) |
|
|
What are the major symptoms of N. meningitidis?
|
* Headache, stiff neck
* Lethary and drowsiness * Coma (ominous sign) * Kernig and Brudzinski sign NOTE: Children may exhibit projectile vomiting |
|
|
How is a diagnosis of N. meningitidis made?
|
CULTURES
blood (+ in 60-80% of untreated patients) CSF (+ in 70% of untreated patients) FINDINGS Incr. PMNs Incr. Thrombocytopenia Incr. CSF pressure Incr. proteins (breakdown of enzymes) Decr. glucose (bacteria utilize glucose) |
|
|
What immunity is there against N. meningitidis?
What about immunity for newborns? What about immunity for those in their teens or 20s? |
Immunity due to protective IgG antibody but it REQUIRES complement (classical) for protection
Newborns receive mother's IgG through milk The colonization of non-pathogenic strains may give protection against disease |
|
|
What are two important factors that predispose us to meningococcemia?
|
1. Inability to activate MAC
2. Patients with anatomic or functional asplenia |
|
|
What is the treatment for N. meningitidis?
|
Pencillin G is recommended therapy
Rifampin is recommended for chemoprophylaxis after contact with patient |
|
|
This bacteria is responsible for 80% of pus forming infections
|
S. aureus
|
|
|
Define the following words:
Suppuration (pyesis) Abscess |
Suppuration (pyesis): the formation of pus
Abscess: well circumscribed collection of pus associated with infection |
|
|
An abscess is relatively inaccessible to ____________ and _____________
It may have to be __________ to relive pressure or resolve infection |
antibodies, antibiotics
drained |
|
|
What is the most frequent cause of septicemia following surgical procedures?
|
S. aureus
|
|
|
Non-specific activation of macrophages and other cells of the innate immune system are brought about by which receptor?
|
TLR-2
|
|
|
Describe S. aureus based on the following:
* Type * ASEs * Motility * Spore forming capability * Resistance |
Type: gram + coccus (irregular grapelike clusters)
ASEs: catalase and caogulase positive Motility: none Spore-forming: none Resistance: 1. high temp 2. high salt concentrations 3. drying |
|
|
S. aureus when grown on a mannitol salt agar produces this type of a halo
|
yellow halo
|
|
|
Colonies of S. aureus are this color __________
S. aureus is known to be ____________________ on blood agar |
Golden
strongly hemolytic (beta hemolytic) |
|
|
Which groups of individuals have higher rates of S. aureus colonization?
|
Health care workers, diabetic patients, dialysis patients, alcoholics, and those that inject drugs (legal or illicit)
|
|
|
What are some of the major sites of colonization for S. aureus?
|
Anterior nares (major)
Axilla, rectum, perineum (minor) |
|
|
The colonization rate in this location (low then high) varies depending on blood loss.
When will this happen? |
Vagina
Higher colonization rate during menses |
|
|
TRUE or FALSE
S. aureus can escape from the abscess and can disseminate hematogenously |
TRUE
|
|
|
If S. aureus is able to spread beyond the local site, what conditions can a patient suffer?
|
* Pneumonia
* Bone and joint infection * Heart valve infection |
|
|
Untreated S. aureus septicemia has a mortality rate exceeding _________ %
Mortality rate for toxic shock syndrome is _______ % |
S. aureus: 80%
TSS: 3-5% |
|
|
Define the following words:
Folliculitis Furuncle Carbuncle |
Folliculitis: appearance of a tender pustule involve a hair follicle (ZIT)
Furuncle: an apparent small abscess that exudes purulent material from a single openin (BOIL) Carbuncle: an aggregate of furuncles with several openings |
|
|
What is impetigo?
|
Small area of erythema, then bullae (blister like lesions filled with cloudy fluid)
As it heals, a honey-colored crust develops |
|
|
Describe septic arthritis
|
* warmth, erythema, tenderness of joints
* infection is often unilateral |
|
|
Describe osteomyelitis
|
* bone infections indicated by fever, bony tenderness, and limp
|
|
|
Describe endocarditis
|
* highly variable as it involves multiple organs
* high fever, chills, sweats, and murmurs * Janeway lesions, Roth's spots |
|
|
Catherer associated infection are often due to ________________
UTIs in sexually active young girls are often due to ________________ |
Staph. epidermis
Staph. saprophyticus |
|
|
What are four virulence factors associated with S. aureus?
|
1. Capsule
2. Protein A 3. Coagulase and fibrinogen binding 4. Toxins |
|
|
What is the function of the capsule?
What is the function of Protein A? |
Capsule: inhibit phagocytosis
Protein A: binds to H chain of antibody and inhibits Ab opsonization -> inhibit phagocytosis |
|
|
What is the function of coagulase and fibrinogen binding?
|
coagulase allows S. aureus to coagulate plasma and form a fibrin barrier around infectious loci
staphylokinase aids the bacteria in breaking down fibrin and blood clots |
|
|
These four S. aureus toxins are know to by cytotoxic to blood cells
|
αβγδ-toxin
|
|
|
This toxin consists of two _______________ factors that act synergistically with α-toxin to kill leukocytes
Is this toxin an endotoxin or exotoxin? |
Leukocidin
Panton-Valentine (P-V) Exotoxin |
|
|
Exofoliatin consists of these two factors.
|
ETA, ETB
|
|
|
ETA and ETB result in this blister-like syndrome
|
SSSS (s. aureus scalded skin syndrome)
|
|
|
The initial features of SSSS are:
|
* Fever
* Erythema * Blisters -> rupture, leave red base * NIKOLSKY SIGN: + |
|
|
What is the Nikolsky sign?
In which other disease is Nikolsky sign (+) ? |
It is when you can push a blister up and down the skin without damaging the intact dermis
Pemphigus vulgaris |
|
|
This range of enterotoxins is responsible for different types of common food poisoning.
|
Enterotoxin A-E, G-I
|
|
|
Enterotoxins A-E, G-I stimulate T cell by binding to ____________
This causes the production of which cytokines? |
TCR Vβ chain
INF-γ and TNF-β |
|
|
What is the most common presentation of food poisoning?
|
* Acute onset of vomiting
* Watery diarrhea 2-6 hours AFTER INGESTION |
|
|
TSS is caused by _____________
It is most frequently associated with the use of ________________ during menstruation |
Tampons
|
|
|
TSS is mostly associated with S. aureus strains that produce _____________
However, strains that produce ________________ and ________________ can cause 50% of non-menstrual TSS |
Exotoxin TSST-1
Enterotoxin B, C |
|
|
TSS can be identified based on these symptoms:
|
* Fever
* Diffuse macular erythema -- sunburn rash, petichae * Hypotension |
|
|
Tampon use is associated with 50% of TSS cases. Which other situation is considered high risk for this condition?
|
Injuries to the nose
|
|
|
What is Bullous Impetigo?
|
* Localized form of SSSS
* Bullae are culture + * Nikolsk sign - * Occurs in infants and children HIGHLY COMMUNICABLE |
|
|
How do you diagnose S. aureus?
|
1. Obtain cultures WITH SUSCEPTIBILITIES appropriate for site of infection
2. Blood cultures (repeat if + as it could be contaminated) |
|
|
TRUE or FALSE
Most purulent infections are going to be caused by S. aureus |
True
|
|
|
The most important defense against S. aureus is ___________________
|
Neutrophils
|
|
|
_____________ patients are much more susceptibile to serious infections
|
Neutropenic
|
|
|
These two innate immunte system process are also involved in defense
|
* Opsonization by Ab
* Complement activation |
|
|
What part of the complement pathway is NOT involved in defense against S. aureus?
|
MAC
|
|
|
What is the most common Coagulase Negative Staphylococcus (CoNS) bacteria?
|
S. epidermis
|
|
|
Does S. epidermis have virulence factors?
|
No
|
|
|
S. epidermis can cause problems in _____________ and _____________
|
Heart valves, catheters
|

